Research Article
Rectal Irrigation (RI) in the Treatment of Defecation Disorders – A Retrospective Evaluation of a Prospective Database
Srinivasaiah N1*, Marshall J2, Gardiner A3, J Monson RT4 and Duthie G3
1St. Mark’s Hospital, UK
2Hull & East Riding NHS trust, UK
3University of Hull, UK
4Florida Hospital, USA
*Corresponding author: Srinivasaiah N, St. Mark’s Hospital, Level 5, Watford Rd, Harrow HA1 3UJ, UK
Published: 06 Dec, 2016
Cite this article as: Srinivasaiah N, Marshall J, Gardiner
A, J Monson RT, Duthie G. Rectal
Irrigation (RI) in the Treatment of
Defecation Disorders – A Retrospective
Evaluation of a Prospective Database.
Clin Surg. 2016; 1: 1227.
Abstract
Background: Rectal Irrigation (RI) has been used in defecation disorders to relieve symptoms and
improve quality of life (QOL). We aimed to evaluate the efficacy and acceptability of RI using health
outcome measures.
Methods: The study was a retrospective review of a prospective database of patients who had rectal
irrigation between 2002 and 2005. The efficacy of rectal irrigation was determined by quantification
of symptoms using general standardized questionnaires (GSQ). The acceptability of rectal irrigation
was determined using the general health outcome measure SF-36 and the Fecal Incontinence
Quality of Life (FIQL) questionnaire.
Results: A total of 175 patients underwent rectal irrigation. There were 111 successful cases and
64 failures. Analysis was done only for the successful ones. Before rectal irrigation, the number of
patients who completed GSQ, SF-36 and FIQL were 72, 71 and 32 respectively. Of these only 43,
43 and 22 completed the GSQ, SF-36 and FIQL respectively after rectal irrigation. GSQ analysis
showed significant improvement in symptoms of straining, incomplete emptying, wind leakage and
urinary leak before and after RI. SF-36 demonstrated significant difference in physical functioning
(Z score -2.34; p< 0.05), social functioning (Z score -2.17; p< 0.05) and general health (Z score -1.97;
p< 0.05), before and after RI (95%CI). FIQL analysis showed no statistically significant difference
in the QOL after RI.
Conclusion: In patients with defecation disorders, RI can offer symptomatic improvement. Most
patients find the treatment acceptable.
Keywords: Incontinence; scoring systems; Outcomes; Constipation; Rectal irrigation
Introduction
Defecation disorders present with a wide spectrum of symptoms and etiologies [1]. A recent review [2] highlighted psycho-social distress along with impaired quality of life (QOL). The problem persists widely in the community and patients represent a diverse group. A systematic review reported a prevalence of 0.4-18% for fecal incontinence [3]. Among the institutionalized, prevalence is approximately 50%, with an annual incidence of 20% developing incontinence [4]. Most patients are managed by conservative and pharmacological methods. There exists an unfortunate group of patients who do not respond to either. An important measure of the severity of Defecation disorders is their effect on QOL. More than 50% of patients with major fecal incontinence report a significant negative impact on QOL [5]. Various therapies have been proposed to relieve the patients of their symptoms and improve their QOL. Rectal irrigation (RI) is one such therapeutic method [6]. The colorectal unit in Hull has been offering RI since 2002. The present study evaluates the efficacy and acceptability of RI in the treatment of Defecation disorders.
Materials and Methods
Between 2002 and 2005 patients initially deemed suitable were referred to the RI clinic. A
preliminary senior consultation was followed by a detailed history, examination and investigations
to assess each patient’s suitability for RI. The majority of the patients
had experienced either no improvement or minimal improvement
with pharmacological agents and conservative measures prior to
surgical intervention.
A colorectal nurse practitioner offered a detailed explanation of
the procedure and informed written consent was obtained. Patients
were given patient dairies and questionnaires to fill in at home. RI
was commenced three weeks later, with the return of pre-irrigation
questionnaires. Either a gravity-assisted or pump-assisted method
was offered. A further set of questionnaires were filled in six weeks
after RI. Patients quantified their symptoms (before and after RI) to
determine the efficacy of RI. The questionnaires used were the general
health outcome measure SF-36, the Fecal Incontinence Quality of
Life (FIQL) questionnaire and a general standardized questionnaire
(GSQ) exploring the symptomatology of Defecation disorders. The
efficacy of RI was evaluated by examining self-reported improvement
of symptoms in response to RI in terms of the GSQ and the visual
analogue scale (VAS). The general and specific health outcome
measures, namely SF-36 and FIQL, evaluated acceptability. For the
purposes of this study success was defined as improvement in the
symptomatology and continuation of RI. Failure was defined as lack
of benefit from RI. The questionnaires used are briefly described
below.
Short form 36
This is a general health outcome measure consisting of physical
and mental component scores. The eight health concepts captured
by the questionnaire are physical functioning (PF), physical health
(PH), emotional problems (EP), and energy fatigue (EF), emotional
well T being/mental health (EW), social functioning (SF), pain (P)
and general health (GH).
FIQL questionnaire
This is a validated QOL questionnaire specifically designed for
patients with fecal incontinence [7]. The four health concepts assessed
by the questionnaire are lifestyle, coping behavior, depression/selfperception
and embarrassment.
GSH questionnaire
The GSH questionnaire was developed in the academic surgical
unit in Hull and was internally validated. It assesses the common
symptoms associated with Defecation disorders. This tool was
used to compare the symptoms before and after RI. The symptoms
considered were frequency of bowel movement, consistency of stools,
mucous leakage, liquid leakage, solid leakage, wearing pad for bladder
symptoms, wearing pad for bowel symptoms, swollen area between
anus and vagina, feeling of bowel pushing forwards into vagina,
need to self-help to empty bowel, micturition urgency, frequency
of straining at stool, feeling of incomplete emptying, wind leakage,
pressure application on the area between the anus and vagina, leakage
of urine on coughing or sneezing, urgency to empty bowel and bowel
problems affecting life.
Data was gathered for presenting symptoms, previous therapies
and surgeries. Reminders were sent to non-responders. A review was
undertaken using the prospectively maintained database and case
notes.
The broad overlap in symptoms and aetiologies made analysis
particularly challenging. For the purposes of this article the
definitions for continence disorders have been deliberately kept
broad. Patients were divided into two categories depending on their
primary symptom of either incontinence or constipation. The term
incontinence was used to describe the involuntary escape of faeces
and includes those patients with primary sphincter problems, patients
with rectal compliance problems leading to urge incontinence and
patients who describe fecal soiling [8]. Constipation was defined
as the inability to evacuate the rectum when desired and included
normal transit constipation, slow transit constipation, obstructed
defecation and dyssynergic defecation [9].
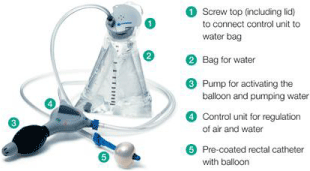
The techniques and apparatus of irrigation have undergone
changes with time. Dansac’s stomal irrigation set was used in the early
phase of the study for RI. This was later followed by the Coloplast
stoma irrigation set for gravity assisted RI and later the Qufora
irrigation system. A pump assisted irrigation set was also used,
the Irrimatic pump (B Braun, Sheffield, UK) (Figure 1). However,
subsequently, the Peristeen Anal Irrigation System (Coloplast
Limited, Peterborough) has been licensed for use and prescription
in the UK for trans-anal irrigation [10] and has now replaced the
majority of other irrigation systems (Figure 2).
Our early patients used the stomal irrigation sets for RI. Initially
patients undertook irrigation on a daily basis using 1.5 L of tap water
at body temperature. Irrigation was commenced sitting on the toilet
with the water bag hanging on a hook with the bottom of the water
bag just above head height. The cone was lubricated and inserted into
the anus holding it firmly, in order to give a good seal.
Between 300 and 500 mLs of water was instilled under gravity in
a gravity assisted method or the same amount using a pump. Patients
were informed that the irrigation process should be gentle and not
uncomfortable in any way. Once the water flow had stopped patients
waited for 1–2 minutes before removing the cone, resulting in an
immediate evacuation of water and stool. This irrigation process was
undertaken three times. Normally the first irrigation is followed by
a hard pellet-like/semisolid cleanse, the second is a brown fluid and
third one is near normal clear water.
Patients were told they should expect an urge to defecate for 10–
15 minutes after the third irrigation but should not experience the
urge to defecate again for 12–24 hours. Once proficient, patients were
encouraged to adopt the volume of water and frequency of irrigation
to suit their own needs.
Data collection was done methodically. Patients were given diaries
and questionnaires to fill in. The diaries consisted of incontinence
and bowel movement details. The questionnaires consisted of the
GSQ, the SF-36 and the FIQL. In addition, a linear scale was used
to quantify any reduction in the severity of the symptoms after RI to
produce a VAS. Lastly measures of satisfaction of medical care and
self-efficacy were also filled in. The SPSS and SF-36 analysis packages
were used for analysis.
Figure 1
Figure 2
Table 1
Table 2
Table 3
Table 4
Results
A total of 175 patients underwent RI. There were 111 successful
cases and 64 failures. Analysis was done only for the successful ones.
The failed cases consisted of people who did not attend, people
whose symptoms were resolved by medication and cases where RI
was not effective. The patient groups were predominantly female
(n=154, 88%) with similar proportions of female patients in both
the successful cases (n=97, 87.4%) and failed cases (n=57, 89.1%).
The mean age of our patient group was 52.6 years (±15.08 SD). The
median follow up was 20 months (IQR=10-30). The SF-36, FIQL and
general standardized questionnaires were analyzed before and after
RI.
SF-36
Seventy-one of the 111 patients completed the SF-36 questionnaire
before treatment, and 43 of these patients also completed the
questionnaire after treatment. Subscales were calculated on a score of
0 to 100, with 0 being the ‘worst’ score and 100 being the ‘best’. The
higher scores meant a better quality of life. Table 1 shows the median
(pre-RI) and median (post-RI) scores for each of the subscales of SFSF
36. There was an improvement in QOL after RI.
Comparison of various components of SF-36 before and after RI
using non-parametric tests showed a significant difference in PF, SF
and GH as shown in Table 2.
The Wilcoxon signed rank test demonstrated a significant
difference in PF, SF and GH between the pre- and post-treatment
status. Table 2 also shows that there were positive shifts in sub-scales
PH, EW and P. These differences were significant at the 90% CI but
not at the 95%CI.
FIQL questionnaire
Thirty-two of the 111 patients completed the FIQL questionnaire
before RI and 22 of these patients after RI. Table 3 shows the median
value (pre-RI) and median value (post-RI) for each of the subscales.
The post-RI median value is equal or higher than the pre-RI measure.
This suggests that there was a slight improvement in QOL measured
by the FIQL questionnaire post- RI. Non parametric tests are shown
in Table 4.
The Wilcoxon signed rank test did not demonstrate any
significant difference in any of the subscales of FIQL. This may be due
to the large amount of missing data and ‘not applicable’ answers to
the individual items on the questionnaire.
GSQ
Seventy-two of the 111 patients completed the GSQ questionnaire
before RI, and 43 completed it after RI. GSQ analysis (Table 5)
showed significant improvement (95%CI) in symptoms of straining,
incomplete emptying, wind leakage, perineal pressure and urinary
leakage before and after RI. At 90%CI there was improvement in
urgency and bowel problems affecting QOL.
There was no significant difference between pre- and post-RI
in frequency of bowel movements, consistency of stools, mucous
leakage, liquid leakage, solid leakage, wearing pad for bladder
symptoms, wearing pad for bowel symptoms, swollen area between
anus and vagina, feeling of bowel pushing forwards into vagina,
micturition urgency, need to self-help to empty the bowel or difficulty
reaching the nearest toilet on time to pass urine.
Visual analogue scale
Sixty-eight of the 111 patients completed the VAS questions
before RI and 42 after RI. Evaluation of the two visual analogue scores,
for bowel (Figure 3) and urinary function (Figure 4, Table 6) suggests
reduction in the severity of the problems affecting QOL. The median
values for severity of bowel function affecting QOL before and after RI
were 90 (IQR=80-100) and 65 (IQR=15-90) respectively. The median
values for urinary function before and after treatment were 12.5
(IQR=0-50) and 10 (IQR=0-28.75) respectively. These results suggest
improvement in symptom severity and in turn improved QOL. The
Wilcoxon signed rank test (Table 6) demonstrated a difference in preand
post-RI problem severity on the VAS, indicating that a greater
proportion of patients recorded an improvement following RI. The
various pathologies for which RI was undertaken were categorized
broadly into constipation, incontinence and miscellaneous.
Treatment success and failure are shown in Table 7.
Table 5
Table 6
Table 7
Discussion
The prevalence surveys suggest fecal incontinence affects more
than 1% of the population with 0.7% having symptoms which impact
on QOL [11] and 2.6% suffering from some form of anal incontinence.
Among those who reported some fecal incontinence, 10% experienced
the problem at least weekly, yet only 36% had consulted their general
practitioner [12]. Self-reported data on constipation in an English
population suggests that 10% of women and 2% of men experience
constipation, and 52% of women and 39% of men reported regular
straining to stool [13]. There do not appear to be any reliable figures
available to give an indication of the numbers of individuals affected
by incomplete evacuation. Such data are obtained from those who
have consulted a member of the health care team or who have been
approached and will admit to this problem. There may be many more
too embarrassed to report these symptoms [14].
Disorders of Defecation cover a spectrum of conditions including
fecal incontinence, idiopathic constipation, and dyssynergic
Defecation [8,9]. Patients can experience symptoms varying from
urgency of Defecation and incontinence, to difficulty initiating
Defecation and constipation. Sometimes the symptomatology can
be overlapping, and around 30% of patients presenting with fecal
incontinence also complain of difficulty evacuating their bowel [1,15].
RI has also been shown to be of benefit to patients with a whole
spectrum of pathologies from organic to functional by improving
symptoms and QOL [6]. A review by Tod and colleagues, evaluating
RI for functional bowel disorders, suggested this as a successful
treatment option for some people [16]. Moreover, other authors
confirmed that RI is a valuable tool for treating patients with
functional bowel disorders [17]. It has been shown to improve
symptoms of constipation, fecal incontinence, and the quality of
life in patients with spinal cord injuries [18]. Studies have also
evaluated long-term results of trans-anal irrigation for Defecation
disturbances and have concluded that trans-anal irrigation is simple
and safe for long-term treatment and is of most benefit to patients
with neurogenic bowel dysfunction [19]. RI now forms a part of the
conservative treatment algorithm in the Netherlands for management
of fecal soiling with normal ano-rectal function [20]. A prospective
study of colonic irrigation for the treatment of Defecation disorders,
by a group in Maastricht concluded that retrograde colonic irrigation
is an undervalued but effective alternative treatment for intractable
Defecation disorders [21].
The current study is a retrospective review of a prospective
database of patients who underwent RI for various evacuatory
disorders from 2002 to 2005. An attempt has been made to measure
both the generic as well as specific QOL using SF-36 and FIQL. Studies
examining the effect of biofeedback on fecal incontinence compared
to simple sphincter exercises alone suggest that biofeedback produces
better results but whether this is due to a placebo interaction with
the therapist rather than the treatment itself is debatable [15]. Initial
results suggest intensive nursing input plays an important role in the
treatment of these patients. However, the sustained improvement
in bowel control noted in our patients responding to RI suggests
the beneficial effect is more than just a placebo effect. If it were a
simple placebo effect one would expect to see the improvement in
symptomatology diminish over time as the input from the specialist
nurse decreased.
RI is a method of management that is time-consuming and
therefore requires commitment from the participants. It has no
apparent side-effects and can be discontinued or recommenced
at any time. The kits are economical and RI is easily supervised by
nursing staff, thus freeing precious time at otherwise busy colorectal
clinics. The Peristeen Anal Irrigation System (Coloplast Limited,
Peterborough) (Figure 2) is licensed for use and prescription in the
UK for trans-anal irrigation [10] and has replaced the majority of
other older irrigation systems. The approximate initial cost of the
irrigation system is around 100 GBP [22].
In summary, this study demonstrated significant QOL
improvement in the subscales of PF, SF and GH at the 95% CI and
in PH, EW and P at the 90%CI using the generic QOL measure.
FIQL revealed only a modest improvement in QOL which was
not statistically significant. Our GSQ demonstrated a significant
difference before and after RI in the following symptoms at the 95%CI:
frequency of straining at stools, feeling of incomplete emptying,
wind leakage, pressure application on the area between the anus and
vagina, leakage of urine on coughing, sneezing. At 90%CI there was
reduction in urgency and bowel problems affecting QOL. There was
no significant difference in pre and post-RI for frequency of bowel
movement, consistency of stools, mucous leakage, liquid leakage,
solid leakage, wearing pad for bladder symptoms, wearing pad for
bowel symptoms, swollen area between anus and vagina, feeling
of bowel pushing forwards into vagina, micturition urgency, need
to help yourself empty the bowel on reaching the nearest toilet on
time to pass urine. The VAS not only demonstrated a clear benefit in
terms of reduction of the severity of the symptoms in bowel function
but to a limited extent in bladder function also where there was an
associated bladder dysfunction.
In this study RI seemed to help both constipation and fecal
incontinence. In patients with incontinence it helped by washing
out the rectum and by giving them a window of respite for their
activities, thereby improving QOL. The varied pathologies for
which RI was undertaken and analysis of success and failures are
represented in this study. There are a few limitations to this study,
which need to be highlighted. The analysis was carried out only on
successful cases, meaning there is no information regarding the cases
that failed and the reasons for failure. The poor return of completed
questionnaires may reflect patient embarrassment due to the nature
of the problem. Though there was noticeable improvement in the
QOL according to the SF-36, the difference for the FIQL failed to
reach statistical significance, possibly due to small numbers and
too many ‘not applicable’ responses. There could be a bias in the
results to a more favorable outcome as patients who have had an
unfavorable experience or outcome from RI may be less likely to
respond to the questionnaire. Alternatively, those patients who are
still using the technique and anticipate a need for further input from
the Coloproctology clinic might be more motivated to respond. The
questionnaire was a ‘snap shot’ documenting the patient condition at
a single time point and asked them to recall their previous symptoms,
which in turn could bias these results. The median follow up was 20
months; there currently is no further long-term outcome data. The
complex symptomatology of this heterogeneous group evaluated
with the GSQ makes quantitative assessment difficult hence the VAS
being added to rate the reduction in the severity of the symptoms
after RI. Overall, RI produced an improvement in self-reported bowel
function in this non-selected group with multiple patho-physiologies.
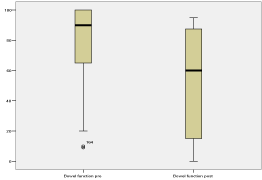
Figure 3
Figure 3
Visual analogue scale showing reduction in the severity of the bowel problems affecting quality of life.
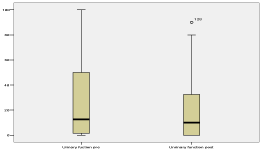
Figure 4
Figure 4
Visual analogue scale showing reduction in the severity of the bladder problems affecting quality of life.
Conclusion
RI can offer symptomatic improvement to patients with Defecation disorders where other conservative and pharmacotherapies have failed. Most patients find the treatment efficacious and acceptable. It should be considered an important tool in the armamentarium for the management of Defecation disorders.
References
- Whitehead WE, Wald A, Norton NJ. Treatment options for fecal incontinence. Dis Colon Rectum. 2001; 44: 131-142.
- Khaikin M, Wexner SD. Treatment strategies in obstructed defecation and fecal incontinence. World J Gastroenterol. 2006; 12: 3168-3173.
- Macmillan AK, Merrie AE, Marshall RJ, Parry BR. The prevalence of fecal incontinence in community-dwelling adults: a systematic review of the literature. Dis Colon Rectum. 2004; 47: 1341-1349.
- Chassagne P, Neveu C, Czernichow P, Bouaniche M, Doucet J, Denis P, et al. Fecal incontinence in the institutionalized elderly: incidence, risk factors, and prognosis. Am J Med. 1999; 106: 185-190.
- Donovan J, Bosch R, Gotoh M, Jackson S, Naughton M, Radley S. Symptom and quality of life assessment in incontinence. Health Publications Plymouth. 2005; 267-316.
- Crawshaw AP, Pigott L, Potter MA, Bartolo DC. A retrospective evaluation of rectal irrigation in the treatment of disorders of faecal continence. Colorectal Dis. 2004; 6: 185-190
- Rockwood TH, Church JM, Fleshman JW, Kane RL, Mavrantonis C, Thorson AG, et al. Fecal Incontinence Quality of Life Scale: quality of life instrument for patients with fecal incontinence. Dis Colon Rectum. 2000; 43: 9-16.
- Cheetham MJ, Malouf AJ, Kamm MA. Fecal incontinence. Gastroenterol Clin North Am. 2001; 30: 115-130.
- Rao SSC. Dyssynergic defecation. Gastroenterol Clin North Am. 2001; 30: 97–114.
- Alison Ebanks PM. The Peristeen Anal Irrigation System: a case study. Product REVIEW. 2011; 1: 68-69.
- Perry S, Shaw C, McGrother C, Matthews RJ, Assassa RP, Dallosso H, et al. Prevalence of faecal incontinence in adults aged 40 years or more living in the community. Gut. 2002; 50: 480-484.
- Nelson R, Norton N, Cautley E, Furner S. Community-based prevalence of anal incontinence. Jama. 1995; 274: 559-561.
- Heaton KW, Radvan J, Cripps H, Mountford RA, Braddon FE, Hughes AO. Defecation frequency and timing, and stool form in the general population: a prospective study. Gut. 1992; 33: 818-824.
- Blackley P. Practical stoma, wound and continence management. 1989.
- Norton C, Kamm MA. Outcome of biofeedback for faecal incontinence. Br J Surg. 1999; 86: 1159-1163.
- Tod AM, Stringer E, Levery C, Dean J, Brown J. Rectal irrigation in the management of functional bowel disorders: a review. Br J Nurs. 2007; 16: 858-864
- McWilliams D. Rectal irrigation for patients with functional bowel disorders. Nurs Stand. 2010; 24: 42-47.
- . Christensen P, Bazzocchi G, Coggrave M, Abel R, Hultling C, Krogh K, et al. A randomized, controlled trial of transanal irrigation versus conservative bowel management in spinal cord-injured patients. Gastroenterology. 2006; 131: 738-747.
- Christensen P, Krogh K, Buntzen S, Payandeh F, Laurberg S. Long-term outcome and safety of transanal irrigation for constipation and fecal incontinence. Dis Colon Rectum. 2009; 52: 286-292.
- Van der Hagen SJ, Soeters PB, Baeten CG, van Gemert WG. Conservative treatment of patients with faecal soiling. Tech Coloproctol. 2011; 15: 291- 295.
- Koch SM, Melenhorst J, van Gemert WG, Baeten CG. Prospective study of colonic irrigation for the treatment of defaecation disorders. Br J Surg. 2008; 95: 1273-1279.
- Peristeen Anal Irrigation System 29121. Available: Peristeen Anal Irrigation System 29121. 2013.