Research Article
Retained Weapon Injuries: An Unusual Presentation with a Good Prognosis
Leire Zarain Obrador*, M Dolores Pérez Díaz, Marta Cuadrado Ayuso, Alejandro Sánchez Arteaga and Fernando Turégano Fuentes
Department of General Surgery, General of Hospital General Universitario Gregorio Marañon, Spain
*Corresponding author: Leire Zarain Obrador, Department of General Surgery, Hospital General, Universitario Gregorio Marañon, Madrid, Spain
Published: 07 Dec, 2016
Cite this article as: Obrador LZ, Dolores Pérez Díaz M,
Ayuso MC, Sánchez A. Retained
Weapon Injuries: An Unusual
Presentation with a Good Prognosis.
Clin Surg. 2016; 1: 1224.
Abstract
Introduction: Retained weapon injuries are unusual but present a diagnostic and therapeutic challenge. The aim of this study was to review our experience in the management of these patients.
Material and Methods: Retrospective review of patients with retained weapon injuries included in our Trauma Registry during a period of 21 years.
Results: Sixteen patients with retained weapon injuries were identified, 13 men and 3 women, with a median age of 45 years (25-88). Nine weapons were in the abdomen, three in the thorax, three in the head, and one in the neck. All patients were hemodynamically stable on admission, and the mean RTS and ISS were of 11.7 and 11, respectively. Surgical approaches included 8 laparotomies, 1 laparoscopy, 1 sternotomy, 1 VATS (video-assisted thoracic surgery), 2 craniotomies, 1 posterior neck exploration, and 2 simple extractions. There was one death, not directly related to the injury, in an 82 y.o. patient with a through-and-through cardiac wound.
Conclusions: Despite their spectacular presentation most patients will be hemodynamically stable, allowing for consideration of minimally invasive techniques in selected patients. Their overall prognosis is good.
Introduction
A retained weapon injury is that in which the weapon or a part of it is partially embedded in the body [1]. Retained weapon injuries are rare but they can pose a diagnostic and therapeutic challenge, and no established protocols exist for their management [2]. The manipulation or blind removal of the weapon before a careful evaluation can cause a significant bleeding, given a theoretical plugging effect of the weapon over adjacent vessels. Since these injuries are so infrequent, most centers have a very limited experience in their management [1,3]. Our aim was to review our experience in the management of these patients, with the hypothesis that, despite their spectacular presentation, the overall prognosis is good.
Materials and Methods
Retrospective study of patients with retained weapon injuries included in our Trauma Registry
from April 1994 to August 2014. We reviewed the demographics, anatomical location, diagnostic
studies, trauma scores, surgical approach, and outcome. The following trauma scores were used: ISS
(Injury Severity Score), RTS (Revised Trauma Score), and PATI (Penetrating Abdominal Trauma
Index).
X-rays were done in all hemodynamically stable patients in order to determine the position
of the weapon. When in doubt about a vital organ involvement, a CT scan or CT-angio was done.
Patients with a retained weapon injury in the precordial area had also a FAST ultrasound. All
patients had the weapons removed in the operating room..
Most patients were managed by the general surgeon on call. Those patients with retained
weapons in the head, thorax and heart were managed by the respective specialists.
A review of published series was carried out through a PubMed search.
Results
Sixteen patients with retained weapon injuries were identified from April 1994 to August 2014,
representing 4% of the stab wounds in our trauma registry. Demographic data and diagnostic tests
are described in Table 1. All retained weapons were visible except for
one patient. Only 5 patients had an ISS > 15. All patients but one was
operated on under general anesthesia.
Location of injuries, type of weapon, injury, surgical technique,
and trauma scores are described in Table 2. All patients but one could
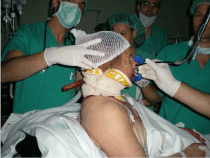
be placed in a supine position on the table; the remaining patient was
injured at the back of the neck and had to be intubated with fiberoptic
bronchoscopy in the sitting position (Figure 1); he was then lied
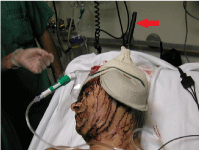
down in prone position. Two of the knives were embedded in bone
structures – one in the spine and, the other one in the skull (Figure 2).
Two patients developed surgical complications: a deep wound
infection (after gastric and transverse colon injury), and an early
postoperative bleeding after a pancreatic injury that needed surgery,
packing and laparotomy. Only one patient died; he was an 82 year old
male with dementia and a self-inflicted cardiac wound by means of a
skewer. The heart was sutured through a sternotomy and he recovered
well initially but ultimately died from a bilateral pneumonia 20 days
after surgery.
Eight patients were lost to follow up. Two patients had late
sequelae: the one with the neck wound had a suprascapular nerve
injury causing persistent weakness on abduction of the upper limb;
the patient injured in his brain and eye suffers from headaches and
slow speech.
Table 1
Discussion
Retained weapon injuries are not frequent and most centers have
a very limited experience in their management [3]. We only found two
published series, a very recent one with 102 cases [1] that proposes a
management algorithm, and another one with 33 patients [3], both
from South Africa; the rest of publications consist of case reports.
The evaluation of the patient must follow ATLS principles, and
the assessment of the location and depth of the weapon can make us
suspect possible visceral lesions [1]. The transfer of the patient by the
EMS must be careful, with immobilization of the weapon in order to
prevent further damage [4].
Around 90%-95% of patients were hemodynamically stable in the
two published series, and 100% in our series; this allows for imaging
techniques before the extraction of the weapon. A simple X-Ray
in two projections was performed in all our patients, and further
imaging was only done in doubtful cases. In some cases a CT scan can
be of help in establishing possible injuries and anticipating bleeding
upon extraction of the weapon [1,3,5].
Retained weapon injuries in the neck and thorax have a higher
risk of bleeding upon extraction of the weapon, in view of the possible
damage to the heart and blood vessels nearby [5]. An initial CT-angio
is advocated by some groups [3], whereas others prefer a simple
CT scan, leaving the CT-angio only for cases without “scattering”
and when it is considered that it can provide useful additional
information. They argue that the distortion effect caused by the
weapon is unpredictable, and that it would be convenient to avoid
the unnecessary administration of intravenous contrast, in case the
patient needs an interventional radiology procedure [1,6].
In the rare case of hemodynamic instability the patient should go
directly to the operating room. Nevertheless, hemodynamic stability
should not make us underestimate the possible presence of vascular
lesions due to the occasional “plugging” effect of the weapon [7];
this is why surgical extraction under direct vision is always required.
In our patient with a heart injury caused by a skewer there was no
cardiac tamponade, probably because of the small cross section of the
occluding weapon.
It is remarkable that in some series simple extraction of the
weapon was enough in 50% of cases [3], whereas in our series it was
only possible in 2 cases (12.5%). Some locations are very rare but
can be life-threatening or can seriously damage organs; transorbital
lesions could be an example, of which we only had one case [8-9].
The use of minimally invasive techniques in selected patients
can prevent unnecessary laparotomies or thoracotomies. The low
incidence of this approach in our series is partly due to the fact that
a majority of cases belong to a period prior to the introduction of
these techniques in the management of trauma. Our first laparoscopy
performed for a retained weapon injury was in 2012, although other
laparoscopic approaches had already been performed for penetrating
injuries in our centre; however, we believe there may be a concern,
at least theoretical, with the possible effects of the creation of
pneumoperitoneum in a patient with a retained weapon, in terms
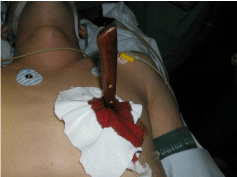
of distortion of the anatomy of the injuries. The only patient of our
series who underwent VATS had a knife which moved with the heart
beats (Figure 3). VATS allowed for the assessment of the integrity
of the pericardium and identification of a lung laceration which
was repaired with an endostapler. In experienced trauma centers
this surgical approach is considered a diagnostic and therapeutic
tool for the extraction of the weapon and the assessment of lung,
diaphragmatic and pericardic injuries. An endovascular approach
can be useful in some cranial lesions [3,10-12].
Retained weapons in the back can pose an anesthetic challenge
because of the impossibility of managing them in the supine position,
as shown in one of our cases; In some of these complex cases some
authors have described the “double table technique”, placing two
parallel operating room tables with a space between them, so that
the patient can be placed supine, and the object remains in the space
between the two tables [3,13,14].
Half of our patients had a history of psychiatric disorder, and
the injuries were self-inflicted; in seven there was an aggression, and
the other had an occupational accident [15]. This differs from the
literature, where most injuries are due to accidental falls over different
objects or to motor vehicle collisions, or also to aggressions [16,17].
The main limitation of this study is the small number of patients,
although be believe it is the third largest published.
Table 2
Figure 1
Figure 1
Intubation with fibrobronchoscopy in a patient with a posterior cervical retained weapon injury.
Figure 2
Figure 3
Conclusion
Penetrating injuries with a retained weapon are infrequent in our environment, they are usually self-inflicted, and have a mild-tomoderate severity; they mostly have a favorable outcome, despite their spectacular presentation. Most patients will be hemodynamically stable, allowing for consideration of minimally invasive techniques in selected patients.
References
- Kong V, Khan Z, Cacala S, Oosthizen G. Retained weapon injuries: experience from a civilian metropolitan trauma service in South Africa. Eur J Trauma Emerg Surg. 2015; 41: 161-166.
- Prasad BC, Vemula RC, Varaprasad G. Nonmissile. Penetrating Spinal Injury with an Impaled Knife: Case Report. Indian J Surg. 2013; 75: 237- 238.
- Sobnach S, Nicol A, Nathire H, Kahn D, Navsaria P. Management of the Retained Knife Blade. World J Surg. 2010; 34: 1648-1652.
- Thomson B, Knight S. Bilateral thoracoabdominal impalement: avoiding pitfalls in the management of impalement injuries. J Trauma. 2000; 49: 1135-1137.
- Frangos SG, Ben-Arie E, Bernstein MP, Miglietta MA. Thoracic stab wound with impaled knife. J Trauma. 2006; 60: 1379.
- Cho SH, Lee HC, Park CW. CT angiography with 3D reconstruction for the initial evaluation neck injury with retained knife. Otolaryngol Head Neck Surg. 2007; 136: 504-505.
- Quraishi A. Inferior vena caval injury following self-inflicted abdominal stab wound. Indian J Surg. 2008; 70: 35-36.
- Ballim S, Gundry B, Mahomed S, VisserL. Intra-orbital knife blade foreign body; a case series. S Afr J Surg. 2013; 51: 134-137.
- Rana MA, Alharty A, Aleterby WT, Kulshrestha A. Transorbital stab injury with retained knife: a narrow escape. Case Rep Crit Care. 2014; 1-4.
- Lunevicius R, O’Sullivan A. Unusual management of thoracoabdominal impalement injury to the right hemiliver and diaphragm. Chin J Traumato. 2014; 17: 41-43.
- Isenburg S, Jackson N, Karmy-Jones R. Removal of an impaled knife under thoracoscopic guidance. Can Respir J. 2008; 15: 39-40.
- Kodadek LM, Leeper WR, Caplan JM, Molina C, Stevens KA, Colby GP. Retained transcranial knife blade with ransaction of internal carotid artery treated by staged endovascular and surgical therapy. Operative Neurosurgery. 2015; E372-E375.
- Lipp M, Mihaljevic V, Jakob H, Mildenberger P, Rudig L, Dick W. Fiberoptic intubation in the prone position. Anesthesia in a thoracoabdominal knife stab wound. Anaesthesist. 1993; 42: 305-308.
- Kaur K, Singhai SK, Bhardwaj M, Kumar P. Anesthesia in a thoracoabdominal knife stab wound. Indian J Anaesth 2014; 58: 742-745.
- Nagar RC. Retained intra-abdominal knife in a self inflicted stab. Indian J Surg. 2013; 75: 414-415.
- Edwin F, Tettey M, Sereboe L, Aniteye E., Kotei D, Tamatey M et al. Impalemente injuries of the chest. Ghana Med J. 2009; 43: 86-89.
- Ruano RM, Pereira BM, Biazzoto G, Bortoto JB, Fraga GB. Management of severe thoracic impalement trauma against two-wheeled horse carriage: a case report and literature review. Indian J Surg. 2014; 76: 297-302.