Research Article
Transverse Abdominal Incision for Encapsulated Peritoneal Sclerosis: A Surgical Secret
Meng-Hsing H1, An-Chieh F1, Hsiu-Lung F1, Shih-Hua L2, Teng-Wei C1, De-Chuan C1, Jyh-Cherng Y1 and Chung-Bao H1*
1Department of General Surgery, Tri-Service General Hospital, Taiwan
2Department of Nephrology, Tri-Service General Hospital, Taiwan
*Corresponding author: Chung-Bao Hsieh, Department of General Surgery, Tri-Service General Hospital, National Defense Medical Center, No. 325, Cheng-Kung Rd, Sec2, Neihu 11490, Taipei, Taiwan
Published: 06 Dec, 2016
Cite this article as: Meng-Hsing H, An-Chieh F, Hsiu-Lung
F, Shih-Hua L, Teng-Wei C, De-Chuan
C, et al. Transverse Abdominal Incision
for Encapsulated Peritoneal Sclerosis:
A Surgical Secret. Clin Surg. 2016; 1:
1216.
Abstract
Background: Encapsulating peritoneal sclerosis related to long-term peritoneal dialysis is a serious and complicated clinical dilemma and surgical treatment might be the final therapeutic option when bowel obstruction occurred. However, the operative therapy comprising peritonectomy and enterolysis is a complex and risky procedure, and the surgical mortality is mainly related to the iatrogenic intestinal perforation.
Methods: Between January 2010 and December 2012, there were 10 patients diagnosed with encapsulated peritoneal sclerosis who underwent surgical interventions in our hospital. Their medical records were reviewed and the general characteristics including operative time, blood loss, postoperative visual analogue scale score, surgical complications, and mortality were collected and analyzed.
Results: We introduce a transverse incision option to decrease the possibility of iatrogenic intestinal perforation and finally result in better clinical outcome.
Conclusions: Compared with traditional longitudinal incision, transverse incision can provide
a potential surgical plan from the pre-existing loculated ascites and avoid adhesive bowel loops
over the dangerous sector created by peritoneal dialysis catheter. However, further retrospective or
prospective cohort study with larger sample size is still required to confirm the exact benefit of this
new surgical technique.
Keywords: Encapsuled peritoneal sclerosis; Enterolysis; Intestinal obstruction; Peritoneal dialysis; Peritonectomy
Introduction
Encapsulated peritoneal sclerosis (EPS) is a rare condition related to long-term peritoneal
dialysis (PD) and characterized by extensive peritoneal fibrosis and encasement of bowel loops
resulting in various clinical symptoms, including chronic abdominal pain, intestinal obstruction,
and weight loss in the late stage [1]. Despite the high morbidity and mortality rate associated with this
condition, surgical treatment, composed mainly of peritonectomy and enterolysis (PEEL), might be
the final treatment option [2-4]. However, the surgical procedure is time-consuming and involves
an extremely high risk of morbidity and mortality because of preoperative malnutrition, a uremic
state, and, most importantly, iatrogenic intestinal perforation during the operation [5-9]. Therefore,
decreasing the mortality rate by improving the preoperative status, lowering the possibility of
iatrogenic intestinal perforation intraoperatively, and instituting aggressive postoperative care has
become the major issue in managing patients with late-stage EPS.
In this brief report, we introduce a transverse incision option to decrease the possibility
of iatrogenic intestinal perforation and provide a better operative field. We demonstrate the
intraoperative exposure, surgical time, and postoperative complications and mortality associated
with this technique.
Figure 1
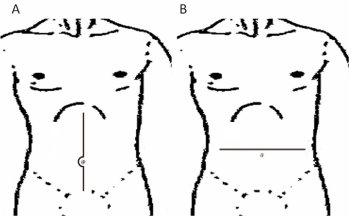
Figure 1
The traditional approach involving a longitudinal incision (A) and a modified approach involving a transverse incision (B).
Figure 2
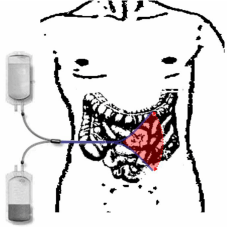
Figure 2
Dangerous fan-shape sector (red area) created by peritoneal dialysis catheter (blue lines) migration (dash-line arrow), which will cause inflammatory fibrosis of the nearby intestines and peritoneum.
Figure 3
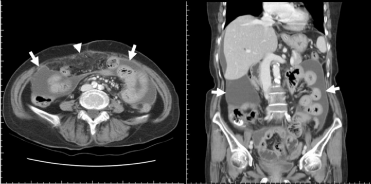
Figure 3
Loculated ascites (arrows) bilaterally and separated by adhesive peritoneum and omentum (arrow head), which provided a potential surgical plane to free the intestines from the abdominal wall at the umbilical level.
Figure 4
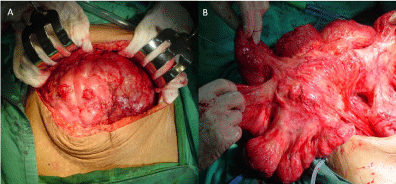
Figure 4
Complete exposure of the adhesive and encapsulated intestines by a transverse incision (A) and decortication of the firmly covered peritoneum (B).
Material and Methods
In the past 3 years, we have performed the PEEL procedure on 10 patients diagnosed with EPS
related to long-term PD. After institutional board reviewed (approval number), we retrospectively
reviewed their medical records and the treatment protocols which comprised the following steps.
Preoperative preparation
Total parental nutrition and human albumin were aggressively
administered to provide adequate energy and nutritional support.
Additionally, if the patient had no contraindications, corticosteroids
were administered to suppress the inflammation process and prevent
further ascites formation and fibrin deposition [10]. In recent years,
tamoxifen was considered if there were no potential thrombotic risks;
however, tamoxifen is still controversial with respect to the prevention
and treatment of EPS, and larger prospective studies are required
[10]. For regular hemodialysis (HD), a relatively dehydrated state
is favored to prevent intestinal edema and swelling preoperatively.
These preoperative measures should be continued for 1 to 2 weeks to
ensure that the patient is in an optimal condition for the operation.
Operation
The operation was comprised mainly of PEEL procedure. We
performed a longitudinal incision on the first and second patient;
however, this was not successful in the second patient because of
severe adhesion between the intestines and the abdominal wall [11].
After much consideration and reviewing of images, we attempted
a transverse approach for the second patient 4 days later. After this
experience with the second patient, the transverse incision approach
was applied to the remaining 8 patients. The transverse incision
provided an easier and safer way to approach the encapsulated
intestines compared with the traditional longitudinal incision (Figure
1). This unique surgical technique was based upon the hypothesis that
the PD catheter would create a sector around the umbilical region
and the intestines in this area would immerse in the dialysate directly
(Figure 2). On the other hand, the intestines in this area would be
more adhesive due to inflammatory fibrosis and firmly encased by the
peritoneum. Because of the sector created by the PD catheter in the
midline of the abdomen, the ascites accumulated bilaterally, forming
fluid pockets (Figure 3). As a result, it was safer and easier to separate
the abdominal wall and adhesive peritoneum, layer by layer, from left
to right, with a transverse incision through the potential space created
by the loculated ascites (Figure 4A). After completely exposing the
encapsulated intestines, repeated enterolysis and peritonectomy or
decortication were performed to restore bowel motility (Figure 4B).
Finally, all the bowel loops were relocated after adequate irrigation,
and the abdominal wall was closed, layer by layer.
Postoperative care
The postoperative care was composed mainly of adequate
nutritional support; control of infection, if present; early mobilization
with a proper pain control device; and the use of corticosteroids and
tamoxifen, if the patient had no contraindications. Additionally, a
relatively dehydrated state was still favored, similar to that during
preoperative conditioning, for the same reason-the intestines would
be less swollen and edematous, resulting in better motility.
Results
In the past 3 years, we performed the PEEL procedure on 10 patients diagnosed with EPS related to long-term PD. Table 1 lists the characteristics of these patients, including operative time, hospital stay, postoperative visual analogue scale (VAS) score, surgical complications, and mortality. There were 4 men and 6 women with a mean age of 52.7 (range, 31–69) years. All were diagnosed with EPS related to long-term PD. The first patient underwent the operation with a traditional longitudinal incision and experienced iatrogenic intestinal perforation with a total operative time of 11 hours and an intra-operative blood loss of 130 ml. The postoperative VAS score on the third day was 4 under the use of intravenous analgesic agents, and the patient died on the 15th postoperative day because of intraabdominal infection with severe sepsis. The second patient underwent surgery with a longitudinal approach at first; however, after 2 hours, we were unsuccessful in separating the adhesive intestines from the abdominal wall. Therefore, the abdominal wall was closed and the PEEL procedure was abandoned. After much consideration and reviewing the operative images of this patient, we decided to perform the PEEL procedure using a transverse incision as the initial step, because the patient had loculated ascites bilaterally, which might have provided a potential surgical plan to separate the adhesive intestines from the abdominal wall. The operation was successfully performed, and the patient recovered well without surgical mortality or complications. After our experience with the second patient, we decided to shift the original approach involving a longitudinal incision to a transverse incision. For the 9 patients (including the second patient) who underwent the PEEL procedure with a transverse incision, the mean operative time was 9.22 (range, 7-12) hours, and the mean intra-operative blood loss was 107.7 (range, 50- 170) ml. The mean VAS score on the third day postoperatively was 3.56 (range, 3-5), and the mean duration of hospital stay was 36.11 (range, 23-51) days. All of the following 8 patients underwent the PEEL procedure with a transverse incision, and the operations were successful without mortality or complications, such as surgical site infection, lung atelectasis, pneumonia, or incisional hernia; however, 2 patients exhibited recurrence 1 year later, and 1 patient underwent another operation subsequently. The other 6 patients recovered well and did not show any adverse findings at the follow-up observation.
Table 1
Table 1
† The first patient received a traditional longitudinal incision.
‡ The second patient received a longitudinal incision initially, but the incision was unsuccessful because of severe adhesion between the intestines and the abdominal wall.
Re-operation with a transverse incision was performed 4 days later with satisfying results, as listed in the table.
Table 1 Characteristics of 8 patients diagnosed with encapsulated peritoneal sclerosis -related bowel obstruction who received the peritonectomy and enterolysis procedure through a transverse incision
Discussion
EPS is a serious complication resulting from long-term
PD. Because of the intraperitoneal inflammation, adhesion and
encapsulation of the intestinal tract and the peritoneum will occur. In
late-stage EPS, patients will present with bowel obstruction, massive
ascites, and malnutrition. The present treatment choices include
total parental nutrition, corticosteroids, tamoxifen (although still
controversial), and surgery.
In EPS, patients generally have a poor nutritional status, and
the intestines are vulnerable because of severe adhesion, peritoneal
encasement, and degeneration. As a result, iatrogenic intestinal
perforation occurs frequently and leads to high surgical morbidity
and mortality. However, Kawanishi et al. [10] reported that the overall
mortality rate was 35.4%, and the 1-, 2-, 3-, and 5-year survival rates
were 93%, 83%, 78%, and 71%, respectively; these better results were
reportedly related to the change in disease severity, advancement and
modification of the surgical technique.
In our limited experience, the surgical mortality was highly related
to intestinal perforation intraoperatively, which might subsequently
lead to severe intra-abdominal infection. As a result, the prevention
of iatrogenic intestinal perforation became the most important issue
to our group. Traditionally, the longitudinal skin incision from the
xiphoid to the pubis has been the most acceptable way to approach
the firmly adhesive intestine covered with leather-like peritoneum
[9]. However, we found that the transverse incision will provide a
potential or initial surgical plane from the loculated ascites to separate
the abdominal wall and intestines through this naturally formed fluid
pocket. Additionally, by avoiding the dangerous sector related to PD
catheter migration, resulting in inflammation and a fibrotic change
of the adjacent peritoneum and intestines, the risk of iatrogenic
intestinal perforation the major cause of mortality could be lowered
remarkably.
However, one of the limitations of the technique is that this unique
incision involves the transaction of the bilateral rectus muscles, which
may cause more severe postoperative surgical wound pain. As a
result, adequate pain control is of great importance and can facilitate
early mobilization. In addition, the muscles of the abdominal wall are
relatively weak because of long-term malnutrition; therefore, there
will be less tension when closing the abdominal wall. On the other
hand, the intensity of postoperative surgical wound pain might be less
compared to other patients with different disease entities.
In managing patients with EPS, the preoperative conditioning
for 1 to 2 weeks requires maintenance of better nutritional support,
underlying disease control, and a relatively dehydrated status when
performing regular HD. After the operation, adequate nutritional
support, potential infection control, anti-inflammatory medication,
appropriate pain control with early mobilization, and mild
dehydration by regular HD should also be carefully considered.
For late-stage EPS complicated with intestinal obstruction,
surgical treatment is the curative treatment option. The operative
treatment involves complex procedures comprising peritonectomy
and intestinal enterolysis, and the transverse incision provides an
easier and safer way to approach the adhesive intestines with less
possibility of iatrogenic intestinal perforation, compared with the
traditional longitudinal incision. However, a large, randomized,
controlled study is still required to support our limited experience.
References
- Kawaguchi Y, Kawanishi H, Mujais S, Topley N, Oreopoulos DG. Encapsulating peritoneal sclerosis: definition, etiology, diagnosis, and treatment. International Society for Peritoneal Dialysis Ad Hoc Committee on Ultrafiltration Management in Peritoneal Dialysis. Perit Dial Int. 2000; 20: S43-S55.
- Braun N, Alscher MD, Kimmel M, Amann K, Büttner M. Encapsulating peritoneal sclerosis - an overview. Nephrol Ther. 2011; 7: 162-171.
- Gandhi VC, Humayun HM, Ing TS, Daugirdas JT, Jablokow VR, Iwatsuki S, et al. Sclerotic thickening of the peritoneal membrane in maintenance peritoneal dialysis patients. Arch Intern Med. 1980; 140: 1201-1203..
- Latus J, Ulmer C, Fritz P, Rettenmaier B, Biegger D, Lang T, et al. Encapsulating peritoneal sclerosis: a rare, serious but potentially curable complication of peritoneal dialysis-experience of a referral centre in Germany. Nephrol Dial Transplant. 2013; 28: 1021:1030.
- Brown MC, Simpson K, Kerssens JJ, Mactier RA. Scottish Renal Registry. Encapsulating peritoneal sclerosis in the new millennium: a national cohort study. Clin J Am Soc Nephrol. 2009; 4: 1222-1229.
- Johnson DW, Cho Y, Livingston BE, Hawley CM, McDonald SP, Brown FG, et al. Encapsulating peritoneal sclerosis: incidence, predictors, and outcomes. Kidney Int. 2010; 77: 904-912.
- Kawanishi H, Kawaguchi Y, Fukui H, Hara S, Imada A, Kubo H, et al. Encapsulating peritoneal sclerosis in Japan: a prospective, controlled, multicenter study. Am J Kidney Dis. 2004; 44: 729-737.
- "Rigby RJ, Hawley CM. Sclerosing peritonitis: the experience in Australia. Nephrol Dial Transplant. 1998; 13: 154-159.
- Summers AM, Clancy MJ, Syed F, Harwood N, Brenchley PE, Augustine T, et al. Single-center experience of encapsulating peritoneal sclerosis in patients on peritoneal dialysis for end-stage renal failure. Kidney Int. 2005; 68: 2381-2388.
- Kawanishi H. Surgical and medical treatments of encapsulation peritoneal sclerosis. Contrib Nephrol. 2012; 177: 38-47.
- Ulmer C, Braun N, Rieber F, Latus J, Hirschbuger S, Emmel J, et al. Efficacy and morbidity of surgical therapy in late-stage encapsulating peritoneal sclerosis. Surgery. 2013; 153: 219-224.