Research Article
Peritoneal Cancer Indexes in Ovarian Carcinomatosis: Correlation between CT and Intraoperative Results and Survival. Is the CT a Good Tool for Correlation?
Lombardo Galera S, Espejo Herrera JJ, López Redondo C, Pérez Montilla ME, Muñoz Casares FC and Zurera Tendero LJ*
Interventional Radiology of Reina Sofia University Hospital, Spain
*Corresponding author: Zurera Tendero LJ, Interventional Radiology of Reina Sofia University Hospital, Córdoba, Av. Menedez Pidal s/n 14005, Spain
Published: 05 Dec, 2016
Cite this article as: Lombardo Galera S, Espejo Herrera JJ,
López Redondo C, Pérez Montilla ME,
Muñoz Casares FC, Zurera Tendero LJ.
Peritoneal Cancer Indexes in Ovarian
Carcinomatosis: Correlation between
CT and Intraoperative Results and
Survival. Is the CT a Good Tool for
Correlation?. Clin Surg. 2016; 1: 1209.
Abstract
Objectives: To value the performance of computed tomography (CT) for the detection of ovarian peritoneal carcinomatosis (PC). We review retrospectively abdominopelvic CT and compare them with surgical reports to value the correlation between surgical and radiological PC indexes and survey.
Methods: We compare the peritoneal tumor implants detected on CT performed before surgery with pathology results obtained after surgery. 48 patients with an average age of 58 years are investigated. Tumor localization and size are documented applying Sugarbaker´s Peritoneal Carcinomatosis Index (PCI) in both, radiological and surgical investigations, which divide the entire abdominal and intestinal regions into 13 spaces. In each one, the bigger visible lesion is measured and scored between 0 and 3.
Results: In our study, the correlation of Pearson shows there is a moderate correlation between the findings of the PCI obtained in the TC and surgical findings, appreciating a general low correlation in all regions, although the better results belong to regions 1,2,0 and 10. Also we observed a lower survival to greater PCI regarding carcinomatosis index in both TC and surgery. All patients received systemic chemotherapy before surgery, so its effect on the size of the peritoneal implants could explain the low correlation.
Conclusion: We can consider that TC is a useful tool for the planning of the surgery and the
preoperative treatments. The peritoneal cancer index is a significant index of survival in ovarian
cancer patients and by using PCI a detailed evaluation of the peritoneal spread is possible being
useful as a prognostic factor.
Keywords: Ovary; Carcinoma; Peritoneal cavity; Computed tomography; Surgery
Introduction
Ovarian cancer is the sixth most common cancer in the world if we consider the impact in
developed countries. It is also the most lethal of all gynecologic malignancies and the fifth cause of
the global dead from cancer in women [1-4]. The cause of this late diagnosis is the result of the low
symptomatology that produces and also that there are no effective screening methods that have
been adequately validated [5]. The 90% of neoplasm affect the surface of the ovary and this is the
reason because the most frequent pattern of dissemination is peritoneal carcinomatosis (PC) [6].
Some years ago PC was considered as a final stage of unresectable cancer, but now with the best
combination of treatment techniques (association of hypertermic intraoperative intraperitoneal
chemotherapy, surgical peritonectomy procedures and intravenous systemic chemotherapy) it can
be managed with curative intention [7]. When PC is diagnosed, disseminated metastatic disease
by other organs such as the liver or the lung is not usually found and it is still possible to get a
curative surgical resection [8], hence the importance of a correct as soon as possible diagnosis of
PC. The extent of carcinomatosis represents one of the most important prognostic factors for the
patients. Tumor implants of different sizes can occur anywhere from the diaphragm until the pelvis
[9]. Several methods of classifications for the PC have been used throughout the history. For all
methods to classify the degree of the carcinomatosis extension we commonly use the Peritoneal
Cancer Index (PCI), described by Jacquet and Sugarbaker [10]. PCI has been cataloged as a useful
quantitative prognostic tool [11]. Nowadays, we have several therapeutic procedures for the PC.
These treatments should be selected depending on the PC´s location
and the extension. Some of these therapies are surgery, systemic
chemotherapy, cytoreductive surgery. The peritonectomy procedure
related with a previous hyperthermic intraperitoneal chemotherapy
(HIPEC) has demonstrated to significantly improve survival in
patients with peritoneal metastases from abdominal primary cancers
[12-14].
The aim of this study is to assess the correlation between CT studies
performed on patients with peritoneal carcinomatosis secondary to
an ovarian neoplasm before surgery with the results obtained in this
surgery in order to evaluate if the CT is a good diagnostic method for
staging PC and studying the correlation between PCI and survival.
Purpose
To compare the findings obtained in the surgery and its
correlation with the preoperative CT in patients with malignant
ovarian peritoneal carcinomatosis. To determine the overall survival
and the disease-free survival in patients with malignant ovarian
peritoneal carcinomatosis treated by surgery and HIPEC in our
center according to the Score of Sugarbaker detected on CT and with
findings obtained in surgery.
Figure 1
Figure 2
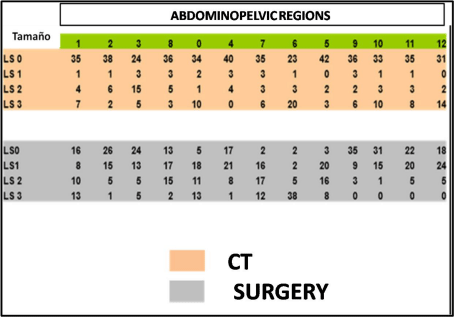
Figure 2
The score PCI obtained in both TC and surgery according to the size of the lesions (LS0-LS3), and areas abdominopélvicas where localized (0-12).
Graph 1
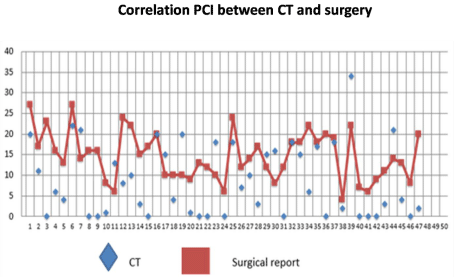
Graph 1
Correlation between the findings of the PCI obtained in the TC and surgical findings in each abdominal region following the score of Sugar Baker, using the statistician Pearson.
Methods
This is an observational and analytical study of prospective
cohorts. It is a unicentric study carried out in the Interventional
Radiology with the collaboration of the Service of General Surgery.
The inclusion criteria are women with malignant peritoneal
disease from ovarian cancer, diagnosed by clinical, radiological and
pathological characteristics between November 2008 to January 2012
with a prospective follow-up until August 2015 who were treated with
cytoreductive or radical peritonectomy associated with intraoperative
chemotherapy (HIPEC). No patients were excluded. We collected
dates including demographics, epidemiological, tomography findings
and other related to surgical treatment and follow-up of patients.
Informed consent was obtained from all individual participants
included in the study. All patients received systemic chemotherapy
before surgery, so its effect on the size of the peritoneal implants
could influence the findings in preoperative CT regarding to the
histopathological, so we assume that systemic chemotherapy could
be a confounding variable. All the CT scan of the abdomen and pelvis
were performed after the administration of ionated intravenous and
oral barium contrast, in a 16-row TC multidetector CT (different
machines) (Figure 1).
Peritonectomy surgery with intraoperative chemotherapy
(HIPEC) was performed by the same team of expert surgeons. For
clinical use, the CT was read by a staff radiologist. For the current
clinical research study, every CT images were read by a single expert
abdominal radiologist who knew that all patients included in the study
had clinical evidence of PC but without knowledge of the operative
findings. Once obtained radiological and surgical PCI-dates, a second
radiologist is responsible for entering the data in Excel format.
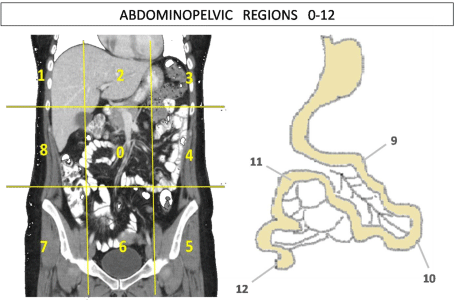
Tumor localization and size were documented applying
Sugarbaker´s PCI in both, radiological and surgical investigations,
which divide the entire abdominal and intestinal regions into 13
spaces. Two transverse planes and two sagittal planes divide the
abdomen into 9 regions. The upper transverse plane is located at the
lowest aspect of the costal margin and the lower transverse plane is
placed at the anterior superior iliac spine. The sagittal planes divide
the abdomen into three equal sectors. The lines define the nine regions
which are number in a clockwise direction with 0 at the umbilicus.
Regions 1, 2 and 3 are subdiaphragmatic from the right to the left
of the patient. Region 4 is left flank, region 5 is left iliac fosse, 6 is
pelvis, 7 is right iliac fosse, 8 is right flank and 0 is umbilicus (Figure
2). Regions 9-12 divide the small bowel considering regions 9 and 10
from jejunum proximal and distal respectively, and regions 11 and 12
from ileum proximal and distal (Graph 1).
In each of the 13 regions the maximum visible lesion size is
measured and assigned to a lesion size score between LS = 0 and LS
= 3. LS = 0 means no tumor visible, LS = 1 means a tumor lesion
size below 0.5 cm, LS = 2 means a tumor lesion size between 0.5 cm
and 5 cm, and LS = 3 means a tumor lesion size larger than 5 cm or
describes a confluent tumor. LS scores in the individual regions are
summed up to the PCI score which can assume a minimum score of
0 and maximum score of 39.
CT scans were analyzed before explorative laparotomy being the
CT results compared with intra-operative findings. The explorative
laparotomy and intra-operative data evaluations were conducted
by a surgical team of surgeon following a standard procedure and
protocol. Intra-operative results regarding PC existence, lesion size
and localization are considered the Gold Standard.
Prior to analyze the results regarding survival, we have artificially
grouped patients according to PCI values obtained in both CT and
surgery as follows:
Mild PCI (TC and surgery): It includes patients with a PCI score
obtained in TC between 0 and 12 points.
Moderated PCI (TC and surgery): It includes patients with a
PCI score obtained in TC between 13 and 26 points.
Histologic type: Nine groups are defined for the histological
descriptive statistical study. To perform the overall survival and
disease-free survival, we grouped these histologic types into
three groups with the most frequent types: Undifferentiated/
differentiated serous and the anaplastic tumors. For the statistical
study we use Windows 7 as operating system, Microsoft®Word 2010
,Microsoft®Excel 2010 and SPSS®22.0 Armonk, NY: IBM Corp.
The statistical analysis includes: For quantitative variables:
calculation of the average (m) as a measure of central tendency and
the standard deviation or standard (DS) as a measure of dispersion.
For qualitative variables calculation of percentages or proportions.
The magnitude of association between quantitative variables using the
Pearson-correlation-coefficient. The survival analysis was conducted
using the estimation method of Kaplan Meyer curves. The method
for the comparison of proportions of survival was performed using
the Mantel test-cox (Long rank test). In all the statistical tests are
considered "significant" with level of confidence was 95% (p< 0.05).
Table 1
Table 1
Correlation between the findings of the PCI obtained in the TC and surgical findings in each abdominal region following the score of Sugar Baker, using the statistician Pearson and Spearman bivariante correlation.
Graph 2
Results
The patients analyze were 47 women with an average age of 58
years. The most frequent histological types were (55.3%) of serous
and undifferentiated (14.9%). In 76 % of cases, radical peritonectomia
was carried out and in 23.4 patients a cytoreductive surgery was
performed. After calculate the Sugarbaker’s PCI in both radiological
and surgical investigations, we obtain respectively for TC and surgery
the following values according to localizations and size : space 1 (30
points on CT and 67 points on surgical procedure), space 2 (19,28),
space 3 (48,22), space 8 (22,53), space 0 (22,53), space 4 (11,40), space
7 (27,86), space 6 (67,126), space 5 (13,76), space 9 (25,15), space 10
(37,17), space 11 (31,30) and space 12 (46,34).
The score PCI obtained in both TC and surgery according to
the size of the lesions (LS0-LS3), and areas abdominopélvicas where
localized (0-12), is shown in Table 1, being the average score in TC
8.64 (0.34) and in surgery 14.66 (4-27). The correlation of Pearson
shows there is a moderate correlation between the findings of the
PCI obtained in the TC and surgical findings (0.379), being this
correlation statistically significant (P< 0.01). Then we analyze the
correlation between the PCI by TC and surgery in each abdominal
region following the score of Sugarbaker, using the statistician
Pearson and Spearman bivariante correlation (Graph 1).
ItWe can observe marked in yellow the significant correlations (p
0.05), appreciating a general low correlation in all regions, although
the better results belong to regions 1,2,0 and 10 (Graph 2).
Once classified the percentages according to
The Score (mild PCI 0-12 vs moderate 13-26) both in TC as
in surgery, Type of peritonectomía (cytoreductive vs radical),
Histopathology, performing three groups on the basis of its frequency:
serous carcinoma, Undifferentiated and differentiated.
The following results were obtained
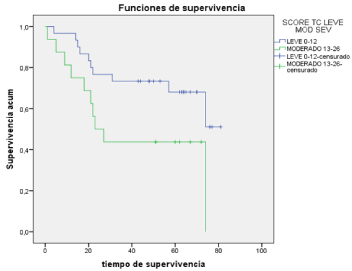
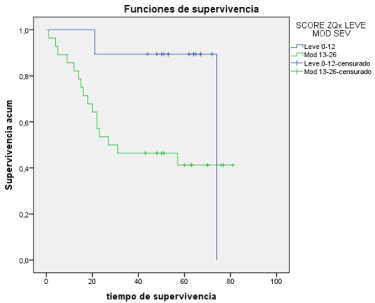
Survival according to PCI in TC: Median survival of 64 for mild
and an average of 41 months to the moderate, being observed a lower
survival to greater PCI, being statistically significant (p< 0.05) (Graph
2).
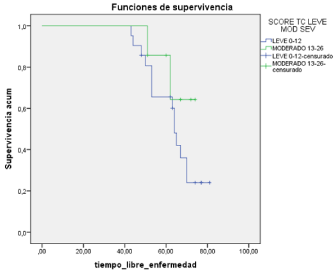
Disease-free survival according to PCI in TC: Average of
disease-free survival of 63 and 68 months respectively for mild
and moderate, showing a lower survival to greater PCI, not being
statistically significant (p< 0.05) (Graph 3).
Survival according to PCI in surgery: Average of disease-free
survival of 68 and 45 months respectively for mild and moderate,
showing a lower survival to greater PCI, being statistically significant
(p< 0.05) (Graph 4).
Survival according to histological type: We analyzed the
probability of survival of patients with peritoneal carcinomatosis
malignant according to the histological type grouping in serous,
differentiated and undifferentiated anaplastic, with an average of
disease-free survival of 49, 69 and 69 months respectively, not being
these differences were statistically significant (p< 0.05).
Graph 3
Graph 4
Discussion
In our study, the correlation of Pearson shows there is a moderate
correlation between the findings of the PCI obtained in the TC and
surgical findings, appreciating a general low correlation in all regions,
although the better results belong to regions 1,2,0 and 10. Also we
observed a lower survival to greater PCI regarding carcinomatosis
index in both TC and surgery. All patients received systemic
chemotherapy before surgery, so its effect on the size of the peritoneal
implants could explain the low correlation.
There are very few published studies about the correlation
between surgical and radiological results in ovarian PC. This may be
due to the extent of the peritoneal carcinomatosis has always been
considered difficult to evaluate preoperatively by CT and especially
before technological development of the image methods. Some years
ago, precise evaluation was necessary during the surgery because
there were not enough reliable imaging studies. Nowadays, with
multidetector CT, we can obtain images to assess for subcentimeter
implants and to create three-dimensional images. Multiplanar
images can be used as a problem-solving tool to confirm the presence
of implants and to assess areas that can be difficult to evaluate on
axial images [9]. That is the reason because although there are other
techniques that can also be used for the evaluation of peritoneal
carcinomatosis, as MR or PET-CT, the technique usually employed
is CT [15]. In our study results indicate better correlation between
surgical and radiological peritoneal carcinomatosis indexes in the
higher regions (especially on the right side and not so good on the
left). The lower values were obtained in both iliac fosses maybe
because in those spaces are difficult to distinguish from bowel loops.
The same findings have been demonstrated in the articles reviewed.
Duhr et al. [16] conclude that there is higher correlation in the upper
and middle abdominopelvic regions compared to the lower region
and the smaller bowel. In the smaller bowel they have obtained lower
levels of correlation (less than 0.6) and sensitivity below 70%. The best
evaluated regions were left flank (4) with 100% sensitivity, right lower
(7) and right flank (8) with 96% and left lower (5) with 93%. The lowest
sensitivity in this study is for smaller bowel (50%). The detection of
implants is as well influenced by the frequency of implants in each
of the spaces. In our study, spaces with most demonstrated lesions
were pelvis and subdiaphragmatic space. In Chandrashekhara et al.
[17] the most common sites of abdominal deposits were the right
subdiaphragmatic space, greater omentum and the pouch of Douglas.
The same results were obtained in the Buy et al. [18] study.
In our experience and also described in literature we have
noted that reformatted coronal and sagittal images can be so
helpful in anatomical regions such as the liver dome, right and left
hemidiaphragms, mesentery and the pelvis because here it could be
difficult to define lesions looking only at transverse images [19]. For
example, sagittal images allow assessment of the vaginal cuff, culde-
sac, peritoneal surface of the bladder and rectosigmoid. Axial
oblique and coronal images can be used to evaluate the region of
the uterosacral ligaments and pelvic side wall. The paracolic can also
be evaluated on coronal images for small implants near the bowel
surface.
Returning to the subject of the importance of lesion size for
detection, some the majority of investigators agree that CT is not
so useful for detecting a low-volume tumor. The sensitivity of CT
in detecting peritoneal metastases for tumoral implants of 1 cm in
diameter or greater is not significantly different from surgery results.
For lesions less than 1 cm the sensitivity of CT is significantly worse
[20].
It has further been shown that the usefulness of CT in the detection
of peritoneal carcinomatosis depends on the primary type of tumor.
It has been demonstrated better correlation in ovarian and colorectal
carcinoma but worse in mesenterium and small bowel among others.
The PCI is the most commonly used staging system for PC, and also
an independent prognostic indicator for long-term outcomes. The
French multi-institutional study confirmed the importance of PCI
in the prognosis of colorectal peritoneal metastases, being a 50%
survival with a PCI 1-6, 25% survival with a PCI of 7-12 and 13-19
and only 10% survival at 5 years with a PCI greater than 19 [21].
In the study of Tentes et al. [22], patients with a peritoneal cancer
index lower than 10 had a significantly better survival than those with
a PCI greater than 10.
In peritoneal carcinomatosis from gastrointestinal cancer,
Harmon and Sugarbaker observed some cases of low PCI score is
recorded in the presence of invasive cancer at a crucial anatomic
site. Even thought the PCI is low, a complete cytoreduction may not
be possible. In these cases, invasive cancer at a crucial anatomic site
places the patient into the same category as would systemic metastases
[23]. We must be careful in assessing the TC in case of low PCI in
ovarian peritoneal carcinomatosis to performed a correct staging of
the invasive cancer.
Related to histopathology, numerous studies show that
tumor-grades of more importance. It is believed that mucious
or endometrioid tumors have more favorable prognosis than
serous tumors that are more aggressive [24,25]. We can find some
limitations of our study that we must discuss. In the first place, the
type of study is retrospective, although all studies of TC were reevaluated
prospectively. The fundamental limitation to assess the
existing correlation between pre- and postsurgical PCI is the systemic
chemotherapy treatment given to the patients after the study of image
that influence the intraoperative findings.
Conclusion
The peritoneal metastases are the most common form of manifestation of ovarian cancer. It has always been considered difficult to assess findings by surgically pre image; however, the development of the TC has improved detection of these injuries. At present we can consider that it is a useful tool for the planning of the surgery and the preoperative treatments. Our findings indicate that there is a good correlation between the findings obtained in TC and surgery in a global way, although when we look at regions of PCI, the findings are not significant in the most regions. If is found abdominal regions in which the correlation is low, corresponding with the regions adjacent to the small intestine, probably due to the difficulty in differentiating between adjacent implant or located in the wall of the handle. On the other hand the score obtained in both TC as in surgery, is a good predictor of the overall survival and disease-free survival, both being lower than the highest score. In the future we will have to increase the sample of our study for best results of statistical significance. We should also consider the need to perform a second TC to the patients between the administration of systemic chemotherapy and surgery, provided by valuing the cost-benefit in terms of radiation dose, to improve the correlation between PCI TC and surgery. The peritoneal cancer index is a significant index of survival in ovarian cancer patients and by using PCI a detailed evaluation of the peritoneal spread is possible being useful as a prognostic factor.
References
- Modugno F, Edwards R. Ovarian Cancer: Prevention, Detection and Treatment of the Disease and Its Recurrence Molecular Mechanisms and Personalized Medicine Meeting Report. Int J Gynecol Cancer. 2012; 22: 45- 57.
- Archer AG, Sugarbaker PH, Jelinek JS. Radiology of peritoneal carcinomatosis. Cancer Treat Res. 1996; 82: 263-288.
- Chang-Yun L, Yonemura Y, Ishibashi H, Sako S, Tsukiyama G, Kitai T, et al. Evaluation of preoperative computed tomography in estimating peritoneal cancer index in peritoneal carcinomatosis. Gan To Kagaku Ryoho. 2011; 38: 2060-2064.
- Levy AD, Shaw JC, Sobin LH. From the Archives of the AFIP Secondary Tumors and Tumorlike Lesions of the Peritoneal Cavity: Imaging Features with Pathologic Correlation. RadioGraphics. 2009; 29: 347-373.
- Cragun JM. Screening for ovarian cancer. Cancer Control. 2011; 18: 16-21.
- Mazzei MA, Khader L, Cirigliano A, Cioffi Squitieri N, Guerrini S, Forzoni B, et al. Accuracy of MDCT in the preoperative definition of Peritoneal Cancer Index (PCI) in patients with advanced ovarian cancer who underwent peritonectomy and hyperthermic intraperitoneal chemotherapy (HIPEC). Abdom Imaging. 2013; 38: 1422-1430.
- Muñoz-Casares FC, Rufián S, Rubio MJ, Lizárraga E, Díaz-Iglesias C, Aranda E, et al. Treatment of peritoneal carcinomatosis from ovarian cancer. Present, future directions and proposals. Clin Transl Oncol. 2007; 9: 652-662.
- "Nougaret S, Addley HC, Colombo PE, Fujii S, Al Sharif SS, Tirumani SH, et al. Ovarian carcinomatosis: how the radiologist can help plan the surgical approach. Radiographics. 2012; 32: 1775-1800.
- Pannu HK, Bristow RE, Montz FJ, Fishman EK. Multidetector CT of Peritoneal Carcinomatosis from Ovarian Cancer. RadioGraphics. 2003; 23: 687-701.
- Jacquet P, Sugarbaker PH. Clinical research methodologies in diagnosis and staging of patients with peritoneal carcinomatosis. Cancer Treat Res. 1996; 82: 359–374.
- Cotte E, Passot G, Gilly FN, Glehen O. Selection of patients and staging of peritoneal surface malignancies. World J Gastrointest Oncol. 2010; 15: 31-35.
- Esquivel J, Sticca R, Sugarbaker P, Levine E, Yan TD, Alexander R, et al. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy in the management of peritoneal surface malignancies of colonic origin: a consensus statement. Society of Surgical Oncology. Ann Surg Oncol. 2007; 14: 128–133.
- Verwaal VJ, Kusamura S, Baratti D, Deraco M. The eligibility for localregional treatment of peritoneal surface malignancy. J Surg Oncol. 2008; 98: 220–222.
- Nelson RC, Chezmar JL, Hoel MJ, Buck DR, Sugarbaker PH. Peritoneal carcinomatosis preoperative CT with intraperitoneal contrast material. Radiology. 1992; 182: 33-38.
- Tempany CM, Zou KH, Silverman SG, Brown DL, Kurtz AB, McNeil BJ. Staging of advanced ovarian cancer: comparison of imaging modalities– report from the Radiological Diagnostic Oncology Group. Radiology. 2000; 215: 761-767.
- Duhr C, Kenn W, Kickuth R, Kerscher AG, Germer CT, Hahn D, et al. Optimizing of preoperative computed tomography for diagnosis in patients with peritoneal carcinomatosis. World Journal of Surgical Oncology. 2011; 9: 171.
- Chandrashekhara SH, Thulkar S, Srivastava DN, Kumar L, Hariprasad R, Kumar S, et al. Pre-operative evaluation of peritoneal deposits using multidetector computed tomography in ovarian cancer. Br J Radiol. 2011; 84: 38–43.
- Buy JN, Moss AA, Ghossain MA, Sciot C, Malbec L, Vadrot D, et al. Peritoneal implants from ovarian tumours: CT findings. Radiology 1988; 169: 691–694.
- Franiel T, Diederichs G, Engelken F, Elgeti T, Rost J, Rogalla P. Multidetector CT in peritoneal carcinomatosis: diagnostic role of thin slices and multiplanar reconstructions. Abdominal Imaging 2009; 34: 49- 54.
- Metser U, Jones C, Jacks LM, Bernardini MQ, Ferguson S. Identification and Quantification of Peritoneal Metastases in Patients With Ovarian Cancer With Multidetector Computed Tomography Correlation With Surgery and Surgical Outcome. Int J Gynecol Cancer. 2011; 21: 1391-1398.
- Spiliotis J, Halkia EE, Kalantzi N, Giassas S, Lianos E, Efstathiou E, et al. Mapping the location of peritoneal metastases using the peritoneal cancer index and the correlation with overall survival: a retrospective study. J BUON. 2015; 20: 64-70.
- Tentes AA, Tripsiannis G, Markakidis SK, Karanikiotis CN, Tzegas G, Georgiadis G, et al. Peritoneal cancer index: a prognostic indicator of survival in advanced ovarian cancer. Eur J Surg Oncol. 2003; 29: 69-73.
- Rhonda L Harmon, Paul H Sugarbaker. Prognostic indicators in peritoneal carcinomatosis from gastrointestinal cancer. International Seminars in Surgical Oncology. 2005; 2: 3.
- Ansell SM, Rapoport BL, Falkson G, Raats JI, Moeken CM. Survival determination in patients with advanced ovarian cancer. Gynecol Oncol. 1993; 30: 215-220.
- Swenerton KD, Hislop TG, Spinelli J, LeRiche JC, Yang N, Boyes DA. Ovarian carcinoma: a multivariante analysis of prognostic factors. Obstet Gynecol. 1985; 65: 264-269.