Case Report
Multiple Primary Malignant Neoplasms of the Kidney, Rectum and Pancreas: A Case Report
Shunda Wang, Ning Shi, Xiaoyan Chang, Menghua Dai* and Yupei Zhao
Department of General Surgery, Peking Union Medical College Hospital, China
*Corresponding author: Menghua Dai, Department of General Surgery, Peking Union Medical College Hospital, Chinese Academy of Medical Science and Peking Union Medical College, No. 1 Shuai Fu Yuan, Dongcheng District, Beijing 100730, People’s Republic of China, China
Published: 05 Dec, 2016
Cite this article as: Wang S, Shi N, Chang X, Dai M,
Zhao Y. Multiple Primary Malignant
Neoplasms of the Kidney, Rectum and
Pancreas: A Case Report. Clin Surg.
2016; 1: 1208.
Abstract
Patients with multiple malignant primary neoplasms (MPMN) are often described as synchronous
or metachronous tumors based on their chronology of presentation. Based on our literature search,
there has been no reported case of a patient with triple primary malignant neoplasms consisting a
combination of kidney, rectum and pancreas metachronously. Here we reported a patient diagnosed
with renal cell carcinoma in 2004, and the other two neoplasms were observed during follow-up in
2001 and 2015 respectively. He received surgical treatment for renal and rectum neoplasm and
chemotherapy was given for the pancreatic adenocarcinoma. Clinicians and scientists need to
emphasis on the importance of the regular physical examination and timely follow-up for older
cancer patients because of being at higher risk of second primaries.
Keywords: Multiple primary malignant neoplasms; Renal cancer; Rectal carcinoid; Pancreatic cancer
Introduction
Multiple primary malignant neoplasms (MPMN) refer to the same host that has two or more than two primary malignant neoplasms in single or multiple organs synchronously or metachronously. According to the number of tumors, it can be divided into double or triple cancers and triple cancers are very rare [1]. A patient has been diagnosed with the renal cell carcinoma, rectal carcinoid and pancreatic adenocarcinoma patients were admitted in Peking Union Medical College Hospital in recent year
Case Presentation
The 54-year-old male patient underwent the renal B-mode ultrasound examination in November
2004 and the result revealed that the left kidney had low, irregular echo with the abundant blood
flow. Then he received the renal blood flow chart which indicated the glomerular filtration rate
of the right kidney was 46.9 ml/min, while the left kidney 45.5 ml/min. Abdominal enhancement
computed tomography revealed the occupation at the middle of the left kidney with the diameter
of 4cm, enhanced significantly. The patient had denied the dysuria, hematuria since the onset
without the percussion pain of kidney during physical examination. In November 24, 2004, he
underwent the percutaneous double renal arteries angiography and left renal artery embolization.
Intraoperative blood flow in the left kidney was very rich, which indicated the great possibility of
malignant neoplasms, so the embolization of the renal artery with the gelatin sponge was given. The
next day he underwent the retroperitoneal laparoscopic radical resection of left renal carcinoma.
The tumor with the diameter of 3-4 cm, deep to renal collecting system, with the red brown profile
at the middle of the left renal was resected during the operation. Pathology findings were clear-cell
carcinoma, moderately differentiated (Figure 1A).
In October 2011, the patient found the tumor from the submucosa of the rectum by regular
physical examination. However, the chief complaint of him did not include the change of stool
character, pus and blood stool, and tenesmus. The he received the colonoscopy and the result
showed there was a soft protrusion from submucosa at the wall of rectum 3 cm from the anus
with the diameter of 3cm and the smooth surface. Rectal examination results were accord with
it. Then the patient received the transanal endoscopic microsurgery in December 1, 2011. During
operation, a 0.6cm tumor was removed 3 cm from the dentate line, with 1cm periphery totally
removed along it. The postoperative pathologic results indicated the neuroendocrine tumor, G1,
invaded the submucosal layer (Figure 1B). Immunohistochemical results were as follows: Syn (+),
CgA (-), CDX2 (-), CD20 (-), CK7 (-), CEA (-), SMA (-).
On 23 October 2015, he performed positron emission computed
tomography (PET-CT) to evaluate the whole body condition and
accidently found a low density occupation at pancreatic tail. It was
around 3.5x3.1x3.2 cm, out of contour with an increased uptake of
radioactive, SUV max 5.1, considering the primary pancreatic cancer.
Meanwhile there were also multiple liver low density lesions with
increased metabolism. Next the patient underwent the endoscopic
ultrasonography guided fine needle aspiration (EUS-FNA) for
further diagnosis in November 5, 2015. There was a 3.4x3cm nearlycircular
lesion at the tail of the pancreas with clear boundary. The
internal echo was uneven and the dilated-pancreatic-duct-like
structure was visible. Pathological smear indicated the ductal
adenocarcinoma, and a little heteromorphic glandular epithelium in
the pancreatic puncture tissue (Figure 2A). Because the origin of the
tumor could not identify clearly by this result, this case was discussed
in the consultation center of the pancreatic disease in Peking Union
Medical College Hospital in November 24. Specialist in our hospital
suggested him performing EUS-FNA liver biopsy, and the final
result indicated that the abnormal glands in the liver tissue with high
possibility of metastasis (Figure 2B). Then the immunohistochemical
results were as follows: CA9 (-), PAX8 (-), Vimentin (+), CK19 (+),
CK7 (+), hepotocyte (-). Combined with immunohistochemistry,
history and serum CA199 1645 U/ml, the diagnosis of pancreatic
adenocarcinoma with live metastasis was clear, T3N2M1, IV period.
The patient receives chemotherapy with combination of Gemcitabine
and Tegafur and has good control of his disease.
Figure 1
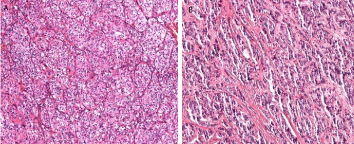
Figure 1
Histological examination of the clear-cell carcinoma of the kidney, moderately differentiated (A) and the neuroendocrine tumor of the rectum which invaded the submucosal layer (B) (H&E, ×200).
Figure 2
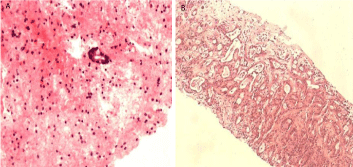
Figure 2
Histological examination of the biopsy of the pancreatic tissue, the ductal adenocarcinoma with a little heteromorphic glandular epithelium (A) and the liver lesion, abnormal glands with high possibility of metastasis (B) (H&E, ×400).
Discussion
According to the diagnostic standard of MPMN in 1932 revised
by Warren [2]: (1) every tumor was malignant identified by histology
(2) each tumor had its unique pathological morphology (3) tumor
occurred in different parts of the body without any connection (4)
excluded the metastasis of each other. According to the diagnostic
time, MPMN could be divided into the synchronized MPMN (the
interval time< 6 months) and the metachronized MPMN (the interval
time > 6 months). The interval times of the onset of three primary
malignant tumors were more than 6 months in our report and they
were independent of each other determined by immunohistochemical
stain, which meets Warren’s criteria and could be diagnosed as
MPMNs. And this kind of MPMN has not been reported in the
published literature before. This report perhaps was the first case with
the combination of the renal cancer, rectal carcinoid and pancreatic
adenocarcinoma in the world.
Most renal carcinomas were clear-cell carcinomas, and the blood
spread and lymph node metastasis were common. The diagnostic
accuracy of radiology was reliable and the 5-year survival rate was
relatively high. The renal cancer was diagnosed in 2004, and this
patient was diagnosed with rectal carcinoid 6 years after that, which
should be described as metachronous tumor. The pathological
diagnosis was neuroendocrine tumor, except for the metastasis of
the renal carcinoma definitely. The pathological type of pancreatic
cancer was adenocarcinoma usually. As for this patient, the PETCT
suggested the primary pancreatic cancer and multiple metastasis
lesions of the liver in 2015, but the biopsy of the pancreas failed to
identify the exact pathologic type. Finally the liver biopsy showed that
atypical glandular cells were arranged and the immunohistochemical
result was vimentin (+) and CK19 (+), CK7 (+), hepotocyte (-), so
it could be diagnosed accurately as primary pancreatic cancer with
liver invasion. By the way, the evaluated serum tumor marker CA199
further corroborated the diagnosis of primary pancreatic cancer.
The incidence of MPMN increased year by year. According
to literature report, the prevalence of MPMN reported varies from
0.7% to 11.7% of all patients with carcinomas in western countries
[3], however, in China it was about only 0.09% [4]. The pathogenesis
of MPMN was still unknown, which might be related to genetic
factors, the instability of the chromosome, the susceptibility of body,
environmental factors, the decline of the immunity and iatrogenic
factors (radiotherapy, chemotherapy and so on) [5].
There was no uniform standard for the treatment of MPMN, and
different measures should be given according to the personal situation
and the specificity of the different tumor. Surgery, radiotherapy and
chemotherapy were the main treatments for malignant tumors at
present. As for the patient in our report, the effect of the surgical
treatment was obvious for renal cell carcinoma and rectal carcinoid,
without any recurrence and metastasis. However, pancreatic
adenocarcinoma was at IV period with multiple hepatic metastatic
lesions. Considering the age of the patient, he lost the opportunity of
the surgery. The chemotherapy was given to the patient and now he
was still in good state. In general, although difficult to differentiate
with recurrent and metastatic carcinoma, the prognosis of MPN was
better than that of metastatic and recurrent cancer. Enough attention
should be paid to avoid missing the opportunity of surgical treatment.
For cancer patients, regular physical examination and timely followup
were very important to ensure early diagnosis, active treatment
and better prognosis.
References
- Fante R, Roncucci L, Di Gregorio C, Tamassia MG, Losi L, Benatti P, et al. Frequency and clinical features of multiple tumors of the large bowel in the general population and in patients with hereditary colorectal carcinoma. Cancer. 1996; 77: 2013-2021.
- Warren RF. Primary Malignant Tumours of the Small Bowel: (A Review of 26 Cases from the Toronto General Hospital). Can Med Assoc J. 1944; 51: 451-457.
- Demandante CG, Troyer DA, Miles TP. Multiple primary malignant neoplasms: case report and a comprehensive review of the literature. Am J Clin Oncol. 2003; 26: 79-83.
- Wang C, Zhao P, Wang J, Song D. [Multiple primary malignant neoplasms]. Zhonghua Wai Ke Za Zhi. 2002; 40: 902-904.
- Müller D, Tomasović-Loncarić C, Galeic-Iljubanović D, Heinzl R, Savić I, Marusić P. Renal cell carcinoma with concurrent urothelial carcinoma of urinary bladder and non-Hodgkin lymphoma. Coll Antropol. 2012; 36: 1049-1052.