Review Article
Transanal Surgery: New Therapeutic Tools
Carolina C. González-Gómez, Aurora Burgos García, Miguel León Arellano, Pedro de María Pallarés, Lidia Cristóbal Poch and Ramón Cantero Cid*
Department of General and Digestive Surgery, University Hospital La Paz, Spain
*Corresponding author: Ramón Cantero Cid, Department of General and Digestive Surgery, Colorectal unit, University Hospital La Paz, Madrid, Spain
Published: 05 Dec, 2016
Cite this article as: González-Gómez CC, García AB,
Arellano ML, de María Pallarés P, Poch
LC, Cid RC. Transanal Surgery: New
Therapeutic Tools. Clin Surg. 2016; 1:
1202.
Abstract
The standard care treatment for rectal cancer is radical surgery, including total mesorectal excision (TME). The management of early stage rectal cancer is based on finding the right balance between optimal oncologic outcomes and acceptable adverse effects for the patient. Trying to minimize the morbidity associated with radical surgery, alternative approaches have been created, including transanal endoscopic microsurgery (TEM) transanal endoscopic operation (TEO) and transanal minimally invasive surgery (TAMIS). Transanal minimally invasive surgery is a safe and effective technique for the resection of lesions located in the middle and upper third of the anus, so benign nature and neoplastic lesions T1N0 stage. The use of this technique in T2 lesions, today is controversial, and requires individual assessment of each case. The correct patient selection allows transanal resections having similar oncological long-term results versus conventional surgery, with a significant reduction in complications. In our experience, long-term oncologic results, and low morbidity and mortality let transanal minimally invasive surgery applicable for rectal lesions, also lower costs and shorter learning curve make a better option than TEM, due to the use of laparoscopic instruments in this field.
Introduction
Rectal cancer is the fifth most frequent worldwide, in the US there are around 40.000 patients
diagnosed each year. The screening programs have decreased the incidence of rectal cancer, in the
last decade, 1.5% in patients between 50 and 64 years and 4.3% over 65 years old, with a 5 years
survival rate around 66.5% [1,2]. Furthermore, routine colonoscopies have advanced the diagnosis
of adenocarcinoma earlier stages and facilitated the identification of premalignant lesions. Actually,
the rate of patients with an early stage diagnose of colorectal cancer (CRC) is around 40%, this
group is associated with a better survival rate [3]. Early stage of CRC includes lesions localized in
submucosa (T1) o muscularis mucosae (T2) or without lymphatic affection (N0).
Within this, new and different therapeutic options had emerged, allowing us a complete
resection or the tumor, with good survival rates and with less morbidity compared to conventional
surgery. In 1984, Dr. Buess [4] developed TEM “Transanal Endoscopic Microsurgery”, as an
alternative in patients with rectal cancer. This technique, was a real change in surgery, it could
achieve complete excision of rectal endoluminal lesions located between 4 and 20 cm from anus,
using a rigid sigmoidoscope. Despite all advantages, implementation of this technique was less than
expected, due to the important learning curve and the high cost of the materials.
The outcomes of new technology in the last decade, and the acquisition of skills in minimally
invasive surgery by colorectal surgeons, have developed a novel therapeutic approach, TAMIS
“Transanal Minimal Invasive Surgery”. It employs standard laparoscopic instruments, preserving
principles describes by Buess [4], through the creation of pneumorectum, across a transanal single
port and the same principles of TEM. This technique, first described in 2010, had allowed the
reduction of the learning curve in colorectal surgeons, and the decrease in instrumental costs.
On the other hand, over the last few years, some endoscopic techniques such as endoscopic
submucosal dissection (ESD) have shown to be effective in the management of early colorectal
neoplasms, particularly in Asian countries where these techniques were born. In Western world,
implementation of ESD is slow and laborious but can be an alternative to surgical treatment option
in selected cases [5].
TEM and TEO
Transanal Endoscopic Microsurgery (TEM) approach involves a technique for lesions located at upper and medium third of the rectum using a rigid sigmoidoscope designed by Wolf (Tuttlingen, Germany) [4], of 4 cm diameter and length between 12 and 20 cm, associated to a CO2 insufflation system. This equipment is connected to a binocular vision system that allows the surgeon a three-dimensional view with an optical magnification of up to 6, connected to a camcorder and three working channels. Before intervention, a rectoscopy is mandatory [6,7], so that the patient should be positioned such that the lesion to be removed will be at the bottom of the rectoscope. Rectal distension, complete excision of rectal wall thickness is achieved, usually using ultrasonic scalpel (Ultracision Harmonic Ethicon Endo-Surgery, Karl Storz, Germany) for a better hemostasis. Because the material used is rigid, this technique has limited application in patients with rectal stricture or those with higher-level concavity of the sacrum [8]. TEM and TEO “Transanal Endoscopic Operation” system uses the same equipment, differing only that TEO use a laparoscopic optic as a display system. Recent indications of TEM/TEO are benign lesions unresectable through endoscopy and early stages of malignant tumors T1 without lymphovascular invasion. Some groups have developed this as a palliative treatment in those patients dismissed for a regular surgery. The piece resection must be the full thickness of the wall, allowing a proper study of the surgical specimen.
The most frequent postoperative complications are urinary
retention and rectal bleeding. Despite the use of a rigid rectoscope
with a diameter of 4 cm, there is no fecal incontinence after TEM use
reported [9,10].
The tumor recurrence is between 5 and 7% for patients with stage
T1N0 complete tumor excision and resection margins free of disease
[11,12].
Figure 1 and 2
Figure 3 and 4
Figure 5
Figure 6
TAMIS
TAMIS “Transanal minimally invasive surgery” was developed
by Dr. Matthew Albert and Dr. Sam Atallah in Orlando, Florida,
and presented in 2010 in the American Society of Colon and Rectal
Surgeons Annual Meeting. Based on the principles proposed by Buess
[4], TAMIS use conventional laparoscopy materials. It allows local
excision of rectal tumors of middle and proximal third and those
benign lesions endoscopically unresectable. In the same way, it allows
excision node through the rectal defect.
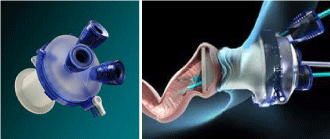
Today, several single-port devices are used for TAMIS [8,13].
- SILS (Single Incision Laparoscopic Surgery) of Covidien, Mansfield, MA. Among other advantages, the SILS device is elastic and soft so it facilitates the easy insertion and removal in the anus, and generates a minimum sphincter injury [14]. Given the proximity of the working ports, is less ergonomic than other devices, because it occur smaller triangulation movements. Figure 1 and 2.
- Gel Point Path® (Applied Medical Inc®, Rancho Santa Margarita, CA), was designed especially for TAMIS [8]. Given the position of the working ports, it allows greater triangulation of the movements, facilitating the operation. Figure 3 and 4.
- SSL Single-site laparoscopic® (Ethicon Endo-surgery®, Cincinnati, OH) available in 2 and 4 cm width. Figure 5.
- Triport (Olympus KeyMed®, Southend, UK). Figure 6.
- Gloveport®: It combines the application of a retractor Alexis® (ALEXIS Wound Protector/Retractor Medium, Applied Medical, Rancho Santa Margarita, CA) and a surgical glove.
- Triport (Olympus KeyMed®, Southend, UK).
- Mechanical preparation of the colon is done, after which the patient is always placed in lithotomy position. In contrast to TEM technique, the time of preparation of the operation field is considerably less (1.9 minutes), and surgical time is less than 1 hour in expert hands [8,15,16].
- After lubricating the working port, it is inserted through the anus and attached to perianal skin. CO2 is insufflated at 20 Lt/ minute with pressure of 15-20 mm Hg.
- The material we use are the same as conventional laparoscopy and the devices could be Ultracusion®, Ligasure ®, Thunderbeat ® or monopolar energy. Unlike TEM, which employs a rigid sigmoidoscope, this port leads to less anorectal injury; on the other hand, it achieves better adaptation in patients with fibrotic tissue [8].
- Indications are the same to TEM, used as a proven technique in benign lesions, patients with carcinoid, adenocarcinoma T1N0 stage, diameter of the lesion less than 3 cm or covering less than 40%, as well those in which there is no lymphovascular invasion [17-19].
- Depending on the size of the excised lesion and patient characteristics, this technique can be performed on an outpatient orinpatient.
Figure 7
Figure 7
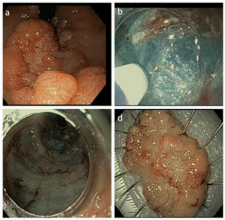
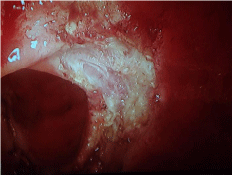
Rectal ESD procedure:
(a) Rectal 4 cm lesion Paris 0-IIa+IIc LSTGranular
type.
(b) Submucosal dissection.
(c) Resection bed. (d) Excised lesion.
Figure 8
Endoscopic Techniques: ESD
Endoscopic submucosal dissection (ESD) is a well-established
technique of endoscopic resection that allows en bloc removal of
gastrointestinal epithelial lesions. ESD differs from endoscopic
mucosal resection (EMR), another type of endoscopic resection. Both
techniques involve injection of a substance under the targeted lesion
to act as a cushion. With EMR, the lesion is then removed with a
snare or suctioned into a cap and snared. While ESD, submucosa is
instead dissected below the lesion with a specialized electrosurgical
knife (Figure 7). This enables the en bloc removal of large lesions
and even those showing shallow submucosal invasion with a curative
intent than can be accomplished with EMR [20].
ESD needs a specialized training to achieve competence and it
can be a lengthy procedure for non experts, especially in Western
countries. However, in expert hands, it has some advantages over
surgery: shorter procedure duration and hospital stay, low profile of
invasiveness and less need for general anaesthesia [5]. Furthermore,
TEM lacks a good view of the operative field near the dentate line
which is not an issue in ESD.
Indications for colorectal ESD are shown in the Table 1 [21,22].
ESD in colon and rectum has generally been used for laterally
spreading tumors (LST) larger than 2 cm in diameter have a higher
risk of submucosal invasion. By using image-enhanced endoscopy,
specific dyes and optical magnification, the endoscopist can evaluate
the lesion through its macro- and microscopic appearance (lesion
colour, surface unevenness, presence of depression, and fold
convergence) to assess the presence of signs of deep submucosal
invasion. Staging with either EUS and/or MRI can be considered for
rectal lesions showing the aforementioned signs [5].
The most frequent complications of ESD are bleeding and
perforation. Intraprocedural bleeding is a common and expected
event during ESD, and it can be typically managed endoscopically.
Delayed bleeding has been reported in 2% of patients in a metaanalysis
of colorectal ESD [23]. Perforation rate in this meta-analysis
of colorectal ESD was 4.8% [23] but in some studies reaches up to 18%
[24]. Fortunately, most perforations are recognized intraprocedurally
and are amenable to clip closure.
The 2010 guidelines from the Japanese Society for Cancer of the
Colon and Rectum define R0 resections as curative when none of the
following are present: depth of submucosal invasion greater than
1000 mm, lymphovascular invasion, poor differentiation, or higher
grade (2 or 3) tumor budding at the site of deepest invasion [25].
The efficacy of ESD in the colon and the rectum has been well
documented in many studies. A systematic review published in 2012
by Repici et al. [23] including 2841 lesions, reported a complete
resection rate of 96% (95%CI 91%-98%), R0 resection rate of 88%
(95 %CI 82 % – 92 %) and a negligible local recurrence rate (< 0.1%).
Another report by Lee et al. [26] that gathered 1000 cases showed
similar results. Nevertheless western endoscopists have also published
results that differ from those reported by more experienced centres,
like the multicenter study published by Rahmi et al. [24] that gathered
45 cases with an en bloc resection rate of 64%, R0 resection rate of
53% and a local recurrence rate of 7%.
Table 1
Table 2
Table 3
Discussion
Conventional treatment of rectal cancer involves the complete
mesorectal excision within a recurrence rates below 5%, a morbidity
rate around 30-68% and 2-7% mortality [8,27,28]. The Parks transanal
access technique is the choice for early lesions in the lower
rectum [29]. The difficulty comes within the middle and upper third
rectum lesions in which the transanal approach becomes limited by
the surgery field [8].
The TEM and TAMI’s transas anal surgery allow us the resection
of large benign lesions and early stages rectal adenocarcinoma. It
is used is mostly in T1N0 lesions. The indication in T2 lesions is
controversial. Although it is technically possible, the discussion
appears regarding cancer outcomes due to the lack of mesorectal
resection. We must consider that between 0-12% of T1 stage patient’s
present lymph node metastasis, and 10 to 22% of those with T2
injuries [30].
The accurate tumor staging and the lymphovascular invasion
are clue factors for transanal surgery indication. From our point of
view the adequate preoperative patient assessment by endoscopic
ultrasound, abdominopelvic MRI as well as CT scan and adequate
patient selection are crucial. We must know the lesion size and
location as well as the presence of lymphovascular invasion [27,30,31].
The endoscopic ultrasound and magnetic resonance imaging
(MRI) are the tests of choice. Sensitivity and specificity are superior
in MRI and there is no inter-observer bias [32]. Both tests can miss
the presence of distant metastases, so the preoperative study should
be completed with the completion of a CT scan.
In experienced centers oncological results are similar to
conventional surgery, within tumor recurrence between 5 and 7%
in T1N0 stage patients in which a complete tumor excision with
free resection margins was performed [11,12,27]. On the other
hand, important complications such as anastomotic dehiscence,
postoperative sepsis, surgical wound complications, sexual
dysfunction, and urinary or gastrointestinal complications arising
from the realization of a stoma are still present, with significant
reduction in quality of life [27]. The correct patient selection allows
transanal resections having similar oncological long-term results
versus conventional surgery [30], with a significant reduction in
complications. Regarding cancer follow up, current clinical guidelines
recommend performing colonoscopy every 6 months the first 5 years
after resection in T1 lesions patients and a CT chest-abdominal-pelvic
annually during the first three years [30,33]. In T2 or higher stage
patients we can perform the transanal surgery as a palliative option
in patients with comorbidities, disseminated stage or patient election.
The second place would be for those patients with higher lesions
than T2, which have undergone adjuvant treatment. According
to the series in the literature, about 20% of patients have complete
pathological response, and this is where the dilemma arises. Many
authors advocate complete mesorectal resection, despite tumor
response, others suggest the possibility of close monitoring without
surgical resection in cases with tumor regression with complete
clinical response [34], with similar long term survival rates. In this
field, the TEM or TAMI’s resection of tumor scar, in those patients
with good response to neoadjuvant therapy, would allow us to reduce
the local recurrence possibility and confirm complete pathological
response in the analysis of the tumor scar.
Unfortunately, nowadays, there is insufficient scientific evidence
around T2 patient. There are few studies in the literature that assess
the cancer outcomes of these patients in the short and med term.
The trial of the American College of Surgeons Oncology Group
(ACOSOG) Z6041 is a prospective and multicenter study of efficacy
and safety (Phase II) of chemo–radiotherapy and local resection of
patients with T2N0 lesions. It included 90 patients and observed
complete response in 44% of surgical specimens, and partial response
in 64% (ypT0/1) [35].
The long-term oncologic outcomes in patients with T2N0 lesions
are not yet known, which calls for the design of clinical trials and
the selection and close monitoring of these patients [35,36]. In this
line include the study of Lezoche compares local recurrence, distant
metastasis and survival of patients with rectal adenocarcinoma stage
T2N0. This study of two randomized groups compares patients with
total excision of mesorectum performed against those with a transanal
resection, in both cases after neoadjuvant therapy. After a follow up
of 84 months, it was observed that oncologic results were similar in
both groups [37]. Some authors suggest that TEM and TAMIS after
chemoradiotherapy increases the postoperative pain and surgical
wound dehiscence, so the patients should be carefully selected [38].
Regarding closure of the defect after resection, there is no
consensus in the literature. Closure can be performed by continuous
or interrupted suture, with intracorporeal or extracorporeal knotting.
The most important study of literature includes 75 operated patients,
of which 53% closure was performed. There are no statistically
significant differences in the postoperative period in both groups
concerning long-term continence. On the other hand, defect closure
is time consuming (an average of 38 minutes in the hands of expert
surgeons). What is undeniable is that in patients with an abdominal
inlet cavity, it is mandatory the rectal closure, either via transanal or
combined with laparoscopy [15].
In addition, we can say that both techniques are important tools
for other rectal diseases. It is useful for resection of rectal adenoma,
tumors of neuroendocrine line or anal warts [39]. It can also be used
to close the defect in rectal iatrogenic perforations. Also, it is a useful
tool in treating complex rectal fistulas, especially those with high
location, such as the urinary fistulas, with good outcomes and low
morbidity [40].
Finally, the data comparing ESD with surgical treatments for
colorectal neoplasia are retrospective and limited in the literature.
In a large systematic review published in 2014 by Arezzo [41], the
ESD procedure appears to be a safe technique, but TEM achieves a
higher R0 resection rate when performed in full-thickness fashion,
significantly reducing the need for further abdominal treatment. In
a single-centre South Korean retrospective study [42], both ESD and
TEM are effective and oncologically safe for treating non-polypoid
rectal high grade dysplasia and submucosa-invading cancers, and
ESD has the additional advantages of minimal invasiveness and
avoidance of anaesthesia. These results are shown in the Table 2 and 3.
Probably, in an ideal scenario, ESD might be a great option
for early colorectal neoplasia but frequently this is not the case in
most institutions in Western countries and surgical techniques are
commonly more accessible to physicians [43]. Recent European
guidelines for early rectal cancer do recommend either ESD or TEM,
both with optimal curative resection rate [44]. By last, we must not
forget that some techniques can be used in combination. Our group
has published [45] the utility of combining simultaneous flexible
endoscopy with TEM.
Conclusion
Transanal minimally invasive surgery is a safe and effective technique for the resection of lesions located in the middle and upper third of the anus, so benign nature as neoplasic lesions T1N0 stage. The use of this technique in T2 and T3 lesions, today is controversial, and requires individual assessment of each case. Long-term oncologic results and low morbidity and mortality make this technique applicable for rectal lesions, and lower costs and shorter learning curve in TAMIS make a better option than TEM (Transanal Endoscopic Microsurgery), due to the use of laparoscopic instruments. Endoscopic procedures such as ESD could be an alternative in selected cases. The application of this technique is developing in other rectal lesions.
References
- GLOBOCAN 2012: Estimated Cancer Incidence, Mortality and Prevalence Worldwide in 2012: International Agency for research on Cancer. WHO. 2014.
- Fazeli MS, Keramati MR. Rectal cancer: a review. Med J Islam Repub Iran. 2015; 29: 171.
- Colorectal Cancer Facts & Figures 2014-2016. Atlanta, GA: American Cancer Society. 2014.
- Buess G, Hutterer F, Theiss J, Böbel M, Isselhard W, Pichlmaier H. A system for a transanal endoscopic rectum operation. Chirurg. 1984; 55: 677-680.
- De María P, Burgos A, Pintor J, Cantero R. Colorectal Endoscopic Submucosal Dissection. SM Group. February 2016.
- Gavilanes Calvo C, Manuel Palazuelos JC, Alonso Martin J, Castillo Diego J, Martin Parra I, Gómez Ruiz M, et al. Cirugía endoscópica transanal en tumores rectales. Cirugía Española. 2014; 92: 38-43.
- Heras MA, Cantero R. Cirugía Transanal a través de Puerto Único (TAMIS). Revisión frente otras Técnicas de Escisión Endoscópica de Lesiones Rectales. Rev Arg Coloproct. 2013; 24: 55-60.
- Larach SW. Transanal endoscopic microsurgery (TEM) and transanal minimally invasive surgery (TAMIS). Cirugía Española. 2012; 90: 418-420.
- Mora López L, Serra Aracil X, Hermoso Bosch J, Rebasa P, Navarro Soto S. Study of anorectal function after transanal endoscopic surgery. Int J Surg. 2015; 13: 142-147.
- Valsdottir EB, Yarandi SS, Marks JH, Marks GJ. Quality of life and fecal incontinence after transanal endoscopic microsurgery for benign and malignant rectal lesions. Surg Endosc. 2014; 28: 193-202.
- Doornebosch PG, Ferenschild FT, de Wilt JH, Dawson I, Tetteroo GW, de Graaf EJ. Treatment of recurrence after transanal endoscopic microsurgery (TEM) for T1 rectal cancer. Dis Colon Rectum. 2010; 53: 1234-1239.
- McCloud JM, Waymont N, Pahwa N, Varghese P, Richards C, Jameson JS, et al. Factors predicting early recurrence after transanal endoscopic microsurgery excision for rectal adenoma. Colorectal Dis. 2006; 8: 581– 585.
- Burke JP, Albert M. Transanal minimally invasive surgery (TAMIS): Pros and cons of this evolving procedure. Semin Colon Rectal Surg. 2015; 26: 36–40.
- Cantero Cid R, García Pérez JC, González Elosua T, Lima Pinto F, Martínez Alegre J, Martín R, et al. Resección transanal a través de un trocar monopuerto. Una nueva aproximación al NOTES. Cirugía Española. 2011; 89: 20-23.
- Hahnloser D, Cantero R, Salgado G, Dindo D, Rega D, Delrio P. Transanal minimal invasive surgery for rectal lesions: should the defect be closed? Colorectal Dis. 2015; 17: 397-402.
- Lee TG, Lee SJ. Transanal single-port microsurgery for rectal tumors: minimal invasive surgery under spinal anesthesia. Surg Endosc. 2014; 28: 271-280.
- Maglio R, Muzi GM, Massimo MM, Masoni L. Transanal minimally invasive surgery (TAMIS): new treatment for early rectal cancer and large rectal polyps-experience of an Italian center. Am Surg. 2015; 81: 273-277.
- Albert MR, Atallah SB, deBeche-Adams TC, Izfar S, Larach SW. Transanal minimally invasive surgery (TAMIS) for local excision of benign neoplasms and early-stage rectal cancer: efficacy and outcomes in the first 50 patients. Dis Colon Rectum. 2013; 56: 301-307.
- Samalavicius N, Ambrazevicius M, Kilius A, Petrulis K. Transanal endoscopic microsurgery for early rectal cancer: single center experience. Wideochir Inne Tech Maloinwazyjne. 2014; 9: 603–607.
- ASGE Technology Committee, Maple JT, Abu Dayyeh BK, Chauhan SS, Hwang JH, Komanduri S, et al. Endoscopic submucosal dissection. Gastrointest Endosc. 2015; 81: 1311-1325.
- Pimentel-Nunes P, Dinis-Ribeiro M, Ponchon T, Repici A, Vieth M, De Ceglie A, et al. Endoscopic submucosal dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy. 2015; 47: 829- 854.
- Tanaka S, Kashida H, Saito Y, Yahagi N, Yamano H, Saito S, et al. (JGES Guideline) Colorectal endoscopic submucosal dissection / endoscopic mucosal resection guidelines. Dig Endosc. 2015; 27: 417- 434.
- Repici A, Hassan C, De Paula Pessoa D, Pagano N, Arezzo A, Zullo A, et al. Efficacy and safety of endoscopic submucosal dissection for colorectal neoplasia: a systematic review. Endoscopy. 2012; 44: 137-150.
- Rahmi G, Hotayt B, Chaussade S, Lepilliez V, Giovannini M, Coumaros D, et al. Endoscopic submucosal dissection for superficial rectal tumors: prospective evaluation in France. Endoscopy. 2014; 46: 670- 676.
- Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y, et al. Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol. 2012; 17: 1-29.
- Lee EJ, Lee JB, Lee SH, Kim DS, Lee DH, Lee DS, et al. Endoscopic submucosal dissection for colorectal tumors--1,000 colorectal ESD cases: one specialized institute's experiences. Surg Endosc. 2013; 27: 31-39.
- Althumairi AA, Gearhart SL. Local excision for early rectal cancer: transanal endoscopic microsurgery and beyond. J Gastrointest Oncol. 2015; 6: 296-306.
- Lazorthes F, Liagre A, Ghouti L. Surgery of rectal cancer: total exeresis of the mesorectum. Ann Chir. 1999; 53: 990-995.
- Parks AG. A technique for excising extensive villous papillomatous change in the lower rectum. Proc R Soc Med. 1968; 61: 441-442.
- Hompes R, Cunningham C. Extending the role of Transanal Endoscopic Microsurgery (TEM) in rectal cancer. Colorectal Dis. 2011; 13: 32-36.
- Serra-Aracil X, Mora-Lopez L, Alcantara-Moral M, Caro-Tarrago A, Gomez-Diaz CJ, Navarro-Soto S. Transanal endoscopic surgery in rectal cancer. World J Gastroenterol. 2014; 20: 11538-11545.
- Bipat S, Glas AS, Slors FJ, Zwinderman AH, Bossuyt PM, Stoker J. Rectal cancer: local staging and assessment of lymph node involvement with endoluminal US, CT, and MR imaging--a meta-analysis. Radiology. 2004; 232: 773-783.
- Engstrom PF, Arnoletti JP, Benson AB 3rd, Chen YJ, Choti MA, Cooper HS, et al. NCCN Clinical Practice Guidelines in Oncology: rectal cancer. J Natl Compr Canc Netw. 2009; 7: 838-881.
- Habr-Gama A, Gama-Rodrigues J, São Julião GP, Proscurshim L Sabbagh C, Lynn PB, et al. Local recurrence after complete clinical response and watch and wait in rectal cancer after neoadjuvant chemoradiation: impact of salvage therapy on local disease control. Int J Radiat Oncol Biol Phys. 2014; 88: 822-828.
- Garcia-Aguilar J, Shi Q, Thomas Jr. CR, Chan E, Cataldo P, Marcet J, et al. A phase II trial of neoadjuvant chemoradiation and local excision for T2N0 rectal cancer: preliminary results of the ACOSOG Z6041 trial. Ann Surg Oncol. 2012; 19: 384–391.
- Fichera A1, Allaix ME. Paradigm-shifting new evidence for treatment of rectal cancer. J Gastrointest Surg. 2014; 18: 391-397.
- Lezoche G, Baldarelli M, Guerrieri M, Paganini AM, De Sanctis A, Bartolacci S, et al. A prospective randomized study with a 5-year minimum follow-up evaluation of transanal endoscopic microsurgery versus laparoscopic total mesorectal excision after neoadjuvant therapy. Surg Endosc. 2008; 22: 352-358.
- Perez RO, Habr-Gama A, São Julião GP, Proscurshim I, Scanavini Neto A, Gama-Rodrigues J. Transanal endoscopic microsurgery for residual rectal cancer after neoadjuvant chemoradiation therapy is associated with significant immediate pain and hospital readmission rates. Dis Colon Rectum. 2011; 54: 545–551.
- Serra-Aracil X, Mora-Lopez L, Alcantara-Moral M, Corredera-Cantarin C, Gomez-Diaz C, Navarro-Soto S. Atypical indications for transanal endoscopic microsurgery to avoid major surgery. Tech Coloproctol. 2014; 18: 157-164.
- Kanehira E, Tanida T, Kamei A, Nakagi M, Iwasaki M, Shimizu H. Transanal endoscopic microsurgery for surgical repair of rectovesical fistula following radical prostatectomy. Surg Endosc. 2015; 29: 851-855.
- Arezzo A, Passera R, Saito Y, Sakamoto T, Kobayashi N, Sakamoto N, et al. Systematic review and meta-analysis of endoscopic submucosal dissection versus transanal endoscopic microsurgery for large noninvasive rectal lesions. Surg Endosc. 2014; 28: 427- 438.
- Park SU, Min YW, Shin JU, Choi JH, Kim YH, Kim JJ, et al. Endoscopic submucosal dissection or transanal endoscopic microsurgery for nonpolypoid rectal high grade dysplasia and submucosa-invading rectal cancer. Endoscopy. 2012; 44: 1031-6.
- Marín-Gabriel JC, Fernández-Esparrach G, Díaz-Tasende J, Herreros de Tejada A. Colorectal endoscopic submucosal dissection from a Western perspective: Today's promises and future challenges. World J Gastrointest Endosc. 2016; 8: 40-55.
- Morino M, Risio M, Bach S, Beets-Tan R, Bujko K, Panis Y, et al. Early rectal cancer: the European Association for Endoscopic Surgery (EAES) clinical consensus conference. Surg Endosc. 2015; 29: 755-773.
- Cantero R, Salgado G. Transanal access for rectal tumors: the simultaneous use of a flexible endoscope and SILS. Tech Coloproctol. 2014; 18: 301-302.