Case Report
Sporadic Mesenteric Fibromatosis Presenting as Intra- Abdominal Sepsis
Hunter Nolen1, Kulvinder S. Bajwa1, Sheilendra S. Mehta1, Peter A. Walker1, M. Elaine Kling2 and Shinil K. Shah1,3*
1Department of Surgery, McGovern Medical School, University of Texas Health Science Center at Houston, USA
2Department of Pathology and Laboratory Science, Memorial Hermann Hospital System, USA
3Michael E DeBakey Institute of Comparative Cardiovascular Science and Biomedical Devices, USA
*Corresponding author: Shinil K Shah, Department of Surgery, McGovern Medical School, University of Texas Health Science, Center at Houston, 6431 Fannin Street, Houston, TX 77030, USA
Published: 02 Dec, 2016
Cite this article as: Nolen H, Bajwa KS, Mehta SS, Walker
PA, Kling ME, Shah SK. Sporadic
Mesenteric Fibromatosis Presenting
as Intra-Abdominal Sepsis. Clin Surg.
2016; 1: 1188.
Abstract
We report an unusual case of mesenteric fibromatosis, a desmoid tumor, mimicking a left upper quadrant abscess, presenting as sepsis and colonic pseudo-obstruction. The authors review the presentation, workup and suggested treatment strategies for this rare tumor.
Case Presentation
A 26 year old woman with a past medical and surgical history remarkable for a cesarean section
one year prior presented to the emergency department for the third time in less than one week with
severe left upper quadrant abdominal and left lower chest pain associated with shortness of breath.
She had been discharged from a recent hospitalization with a diagnosis of constipation for similar
complaints two days earlier. On arrival to the emergency room, the patient was afebrile, hypotensive
(systolic blood pressure was 76 mmHg), and tachycardic (heart rate of 119). She reported having
severe left upper quadrant abdominal and left lower chest pain that began 1 week prior, associated
with nausea and vomiting. She had peritonitis on physical examination. Chest x-ray on admission
showed the patient to have bilateral pleural effusions, but no other abnormalities were noted. Labs
were unrevealing aside from leukopenia (white blood cell count 2.0 K/CMM, 75.1% neutrophils),
lactic acidosis (3.6mmol/L), and hypoalbuminemia (2.7 g/dL).
Review of previous imaging obtained including computed tomography (CT) of the chest,
abdomen and pelvis revealed an approximately 8 cm round intra-abdominal mass in the left upper
quadrant abutting the diaphragm, stomach, colon and spleen (Figure 1). Due to the patient’s
presenting symptoms and the corresponding findings seen on CT, the patient was emergently taken
to the operating room for a diagnostic laparoscopy with presumptive suspicion for a left upper
quadrant abscess versus mass of questionable etiology.
Upon entering the abdomen, ascites was noted in the right upper quadrant. The spleen
was visualized and noted to be well adherent to a left upper quadrant mass. The omentum was
subsequently dissected off of the mass. The capsule of the mass was noted to be very firm. A portion
of this tissue was resected and a frozen section was concerning for a possible spindle cell neoplasm.
Upon conversion to formal laparotomy, approximately 200-250 mL of purulent fluid was suctioned
from the pelvis. The mass was resected en bloc, requiring partial colectomy (splenic flexure) and
splenectomy (Figure 2). A primary colocolostomy was performed. The patient’s post-operative
course was prolonged secondary to delayed return of bowel function as well as poor pulmonary
toilet secondary to sympathetic left pleural effusion (requiring thoracentesis x 2). She had no
infectious complications.
Final pathology revealed a 10.3 x 8.8 x 7.0 cm mass consisting of bland spindle cell proliferation
without necrosis. Mitoses were noted to be 0 per 50 high power fields. The tumor cells were found
to be positive for vimentin, beta catenin, and CD10 and negative for pancytokeratin, S100, HMB45,
CD34, smooth muscle actin, desmin, GFAP, estrogen receptor, CD117, and DOG-1. Testing for
c-KIT and PDGFRmutations were performed, in order to completely exclude a gastrointestinal
stromal tumor, and was found to be negative. Three mesenteric lymph nodes were sampled and were
negative for any abnormality. These overall features were consistent with mesenteric fibromatosis.
Post-operatively, the patient has done well. Of significance, the patient has no significant family history of polyposis syndromes or colon/gastrointestinal cancer. Genetic testing for familial adenomatous polyposis (FAP) was negative.
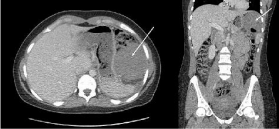
Figure 1
Figure 1
Computed tomography (CT) of the abdomen revealed a large mass (arrow) in the left upper quadrant abutting the spleen, splenic flexure, diaphragm and the stomach.
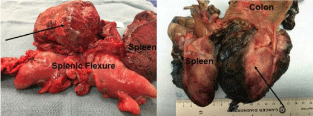
Figure 2
Figure 2
Photographs of the specimens revealed a large mass arising from the splenic flexure of the colon, consistent with mesenteric fibromatosis on final pathology. Demonstrated is the excised specimen as well as cross section demonstrating the pass to be arising from the splenic flexure of the colon.
Discussion
Mesenteric fibromatosis, also known as desmoid tumors, are
rare soft-tissue tumors, characterized by deregulated fibroblastic
proliferation. They are usually slow growing and locally aggressive.
Although they lack the capacity to metastasize, they are associated
with a high rate of recurrence after resection [1]. Desmoid tumors
account for roughly 0.03% of neoplasms and are not known to
have any significant racial or ethnic predilection [2]. However,
some studies have shown that there is a slight increase incidence
for desmoid tumors in women [3]. This may be due in part to the
potential influence of estrogen on the local environment, since
studies have linked higher incidences of desmoid tumors in pregnant
women and women using oral contraceptives [1]. The fact that
estrogen plays a role in the development of desmoid tumors has
further been strengthened by the fact that spontaneous regression of
desmoid tumors have been noted in women undergoing menopause
[4]. Desmoid tumors have also been linked to patients who have
undergone surgery or experienced soft tissue trauma [5].
Desmoid tumors have been reported to affect all sites of
the body, however, they are generally classified into three main
anatomic locations: extra-abdominal, intra-abdominal, and along the
abdominal wall [6]. Although there is an association between desmoid
tumors and FAP, the majority of desmoid tumors arise sporadically
[7]. It is important to note that the most common location for FAP
associated desmoid tumors is intra-abdominal, while sporadic
desmoid tumors are more commonly found deep in the shoulder
girdle, the extremities, and the buttock region [8]. Desmoid tumors
that arise intra-abdominally most commonly originate from the small
bowel mesentery, thus they have been routinely named mesenteric
fibromatosis or mesenteric desmoid tumors in the literature [9].
One important risk factor for the development of intra-abdominal
mesenteric desmoid tumors is a history of abdominal surgery. This risk
factor is especially linked to patients who have been diagnosed with
FAP, specifically those patients who have the Gardner’s syndrome
variant [9,10]. Although a history of trauma has also been linked to
the development of desmoid tumors, it is usually associated with the
extra-abdominal variant. One study showed that a history of trauma
was seen in 19-63% of patients who developed extra-abdominal
desmoid tumors [11]. Typically, desmoid tumors are isolated single
tumors; nonetheless, patients with multiple desmoid tumors have
been reported, specifically in patients with Gardner’s syndrome [12].
Most patients with desmoid tumors are clinically asymptomatic; however, patients who present with symptomatic mesenteric desmoid tumors usually present late [13]. Patients who present with intra-abdominal desmoids usually present with symptoms that can be attributed to the tumor’s mass effect [14]. These symptoms include a palpable abdominal mass, abdominal pain, vomiting, weight loss, fever, malaise, small bowel obstruction, small bowel perforation, gastrointestinal bleeding, peritonitis, and ureteric obstruction [15- 17]. Desmoid tumors have unpredictable clinical courses that range from small, asymptomatic tumors that remain static to small tumors that rapidly enlarge causing severe disability and possible death within months or years. The morbidity and mortality associated with intraabdominal desmoid tumors are directly related to the tumor’s location, and therefore, the abutting structures the tumor may infiltrate or compress [18].
Mesenteric desmoid tumors have variable radiological features
which make them difficult to diagnose with imaging alone [19].
Desmoid tumors can appear as either illor well circumscribed masses
with variable attenuation and contrast enhancement when viewed
on CT and magnetic resonance imaging (MRI). Most mesenteric
desmoid tumors present as large (>15cm in diameter) abdominal
masses that have a generally higher attenuation, when compared
to muscle, on contrast enhanced CT [19]. MRI has been described
as the imaging modality of choice in patients suspected to have a
mesenteric desmoid tumor. MRI typically reveals masses with a low
signal intensity on T1 weighted images and variable signal intensity
on T2 weighted images when comparing its attenuation to muscle
[20,21]. Ultrasound is another imaging modality that has been used
in the clinical work up of desmoid tumors. Although it does not have
the multi planar capabilities of both MRI and CT, it is an important
tool in the evaluation of abdominal discomfort, one of the common
complaints seen in patients presenting with mesenteric desmoid
tumors [15-17]. Like MRI and CT, desmoid tumors can have multiple
presentations when seen on sonography, ranging from smooth, well
circumscribed masses with a high, medium, or low echo texture, to
ill-defined masses with multiple echo textures [22].
The most specific and conclusive diagnostic test for desmoid
tumors is a tissue biopsy [23]. The pathophysiology of desmoid
tumor formation has been linked to excess production of the protein
Beta-catenin [24]. This excess production is believed to be caused
by different mutations in the APC gene and/or the Beta-catenin
(CTNNB1) gene [25]. In one case series, done by Huss et al, 91.6% of
all desmoid tumors showed nuclear expression of Beta-catenin [26].
Those desmoid tumors that were shown to not express Beta-catenin
either carried a CTNNB1 mutation or had an association with patients
diagnosed with Gardner’s syndrome [26]. It is good practice to test
all patients diagnosed with a desmoid tumor for mutations in the
APC gene, even though APC mutations are uncommon in sporadic
desmoid tumors [27,28]. This is due to the fact that patients with
APC gene mutations have an increased risk of colorectal cancer [28].
Similarly, Wang et al. proposed that all pediatric patients diagnosed
with a desmoid tumor should be referred for FAP evaluation, APC
gene mutation testing, and genetic counseling [29].
The treatment of choice for desmoid tumors is surgical excision
with wide margins [30]. However, wide margins may not always
be possible given that some desmoid tumors are inoperable due to
their large size or their involvement with vital structures. Another
common problem seen when treating mesenteric desmoid tumors
with surgical excision is the not insignificant recurrence rate (25-
50%) [31]. Neoadjuvant radiotherapy has been utilized prior to
surgical excision in order to shrink tumors to an operable size and
to reduce the recurrence rate [31]. For patients who are not good
surgical candidates or for those with local recurrence, cytotoxic
pharmaceutical agents, estrogen receptor antagonists, non-steroidal
anti-inflammatory drugs, and tyrosine kinase inhibitors have been
shown to have some efficacy in the medical management of desmoid
tumors [32-36]. However, these agents are not considered first line
therapy since only a small number of patients have been treated with
these agents, and the responses seen from these agents have been
poorly documented [37].
Because of the high rate of recurrence, despite the achievement
of histopathological negative margins during surgical resection,
long term follow up is essential in the post-operative management
of desmoid tumors. The median time to tumor recurrence has been
found to be around 23 months, with more than 90% of recurrences
evident by 5 years [37]. Currently, there are no evidence based
protocols for tumor surveillance following surgical treatment.
However, the National Comprehensive Cancer Network suggests
completing a history and physical, with appropriate imaging, every
3-6 months for the first three years. After the first 3 years of postoperative
follow up, an annual history and physical with appropriate
imaging is sufficient for surveillance of tumor recurrence [38].
References
- Kasper B, Ströbel P, Hohenberger P. Desmoid Tumors: Clinical Features and Treatment Options for Advanced Disease. The Oncologist. 2011; 16: 682-693.
- Eltabbakh GH, Shamonki MI, Moody JM, Garafano LL. Laparoscopy as the primary modality for the treatment of women with endometrial carcinoma. Cancer 2001; 91: 378-387.
- Malur S, Possover M, Michels W, Schneider A. Laparoscopic-assisted vaginal versus abdominal surgery in patients with endometrial cancer--a prospective randomized trial. Gynecologic oncology 2001; 80: 239-244.
- Bijen CB, Briët JM, de Bock GH, Arts HJ, Bergsma-Kadijk JA, Mourits MJ. Total laparoscopic hysterectomy versus abdominal hysterectomy in the treatment of patients with early stage endometrial cancer: a randomized multi center study. BMC cancer 2009; 15: 23.
- Malzoni M, Tinelli R, Cosentino F, Perone C, Rasile M, Iuzzolino D, Malzoni C, Reich H. Total laparoscopic hysterectomy versus abdominal hysterectomy with lymphadenectomy for early-stage endometrial cancer: a prospective randomized study. Gynecol Oncol 2009; 112: 126-133.
- International Federation of Gynecology and Obstetrics – FIGO. Staging Classifications and Clinical Practice Guidelines for Gynaecological Cancers. 2006, 88p. Available in: http://www.figo.org/publications. Retrieved on 21-oct-2009.
- Scribner J, Dennis R, Walker JL, Johnson GA, McMeekin SD, Gold MA. Surgical Management of Early-Stage Endometrial Cancer in the Elderly: Is Laparoscopy Feasible? Gynecologic Oncology 2001; 83: 563-568.
- Tozzi R, Malur S, Koehler C, Schneider A. Title Analysis of morbidity in patients with endometrial cancer: is there a commitment to offer laparoscopy? Gynecol Oncol 2005; 97: 4-9.
- Janda M, Gebski V, Forder P, Jackson D, Williams G, Obermair A. Total laparoscopic versus open surgery for stage 1 endometrial cancer: the LACE randomized controlled trial., LACE Trial Committee Source Contemporary clinical trials 2006; 27: 353-363.
- Zullo F, Palomba S, Falbo A, Russo T, Mocciaro R, Tartaglia E, et al. Laparoscopic surgery vs laparotomy for early stage endometrial cancer: long-term data of a randomized controlled trial. American Journal of Obstetrics and Gynecology 2009; 200: 296.e1-9.
- Eltabbakh GH, Mount SL. Laparoscopic surgery does not increase the positive peritoneal cytology among women with endometrial carcinoma. Gynecol Oncol 2006; 100: 361-364.
- Palomba S, Falbo A, Mocciaro R, Russo T, Zullo F. Laparoscopic treatment for endometrial cancer: a meta-analysis of randomized controlled trials (RCTs). Gynecol Oncol 2009; 112: 415-421.
- Faria SC, Iyer RB, Rashid A, Ellis L, Whitman GJ. Desmoid tumor of the small bowel and the mesentery. AJR Am J Roentgenol. 2004; 183: 118.
- Easter DW, Halasz NA. Recent trends in the management of desmoid tumors. Summary of 19 cases and review of the literature. Ann Surg. 2010: 765-769.
- Batori M, Chatelou E, Mariotta G, G Sportelli, A Straniero, G Casella, et al. Giant mesenteric fibromatosis. Eur Rev Med Pharmacol Sci. 2005; 9: 223-225.
- Polat C, Aktepe F, Turel S, Yazicioglu B, Ozkececi T, Arikan Y. A giant mesenteric fibromatosis case presenting with mechanical intestinal obstruction and successfully resected with partial duodeno-jejunectomy and right hemicolectomy. Clinics (Sao Paulo). 2010; 65: 110-113.
- Lewis JJ, Boland PJ, Leung DH, Woodruff JM, Brennan MF. The enigma of desmoid tumor. Ann Surg. 1999; 229: 866-872.
- Constantinidou A, Scurr M, Judson I, Litchman C. Clinical presentation of desmoid tumors. Desmoid Tumors. Springer. 2012; 5-16.
- Casillas J, Sais GJ, Greve JL, Iparraguirre MC, Morillo G. Imaging of intraand extraabdominaldesmoid tumors. Radiographics. 1991; 11: 959-968.
- Lee J, Glazer H. Controversy in the MR imaging of fibrosis. Radiology 1990; 177: 21-22.
- Hamlin DJ, Paige R, Pettersson H, Bland KJ. Magnetic resonance characteristics of an abdominal desmoid tumor. Comput Radiol. 1986; 10:11-13.
- Mantello MT, Haller JO, Marquis JR. Sonography of abdominal desmoid tumors in adolescents. J Ultrasound Med. 1989; 8: 467-470.
- Schwartz RA, Trovato MJ, Lambert PC. The desmoid tumor -a locally aggressive neoplasm.Cesko-Slovenska Dermatologie. 2007; 82: 34-38.
- Tejpar S, Nollet F, Li C, Wunder JS, Michils G, dal Cin P, et al. Predominance of beta-catenin mutations andbeta-catenin dysregulation in sporadic aggressive fibromatosis (desmoid tumor).Oncogene. 1999; 18: 6615-6620.
- Lips DJ, Barker N, Clevers H, Hennipman A. The role of APC and betacatenin inthe aetiology of aggressive fibromatosis (desmoid tumors). Eur J Surg Oncol. 2009; 35: 3-10.
- Huss S, Nehles J, Binot E, Wardelmann E, Mittler J, Kleine MA, et al. β-catenin (CTNNB1) mutations and clinicopathological features of mesenteric desmoid-type fibromatosis. Histopathology. 2013; 62: 294-304.
- Escobar C, Munker R, Thomas JO, Li BD, Burton GV. Update on desmoid tumors. Ann Oncol. 2012; 23: 562-569.
- Mangat C, Inoue S, Kader M, Debelenko L, Onwuzurike N. Sudden progressive abdominal pain due to large peritoneal desmoid tumor: A case report with review of literature. Journal of Pediatric Surgery Case Reports. 2013; 1: 241-243.
- Wang WL, Nero C, Pappo A, Lev D, Lazar AJ, López-Terrada D. CTNNB1 genotyping and APC screening in pediatric desmoid tumors: a proposed algorithm. Pediatric and Developmental Pathology. 2012; 15: 361-367.
- Yang CH, Sheen-Chen SM, Lu CC, Ko SF, Eng HL. Computed tomographic presentation of mesenteric fibromatosis. Dig Dis Sci. 2005; 50: 348-350.
- Baliski CR, Temple WJ, Arthur K, Schachar NS. Desmoid tumors: A Novel approach for local control. J Surg Oncol. 2002; 80: 96-99.
- Smith AJ, Lewis JJ, Merchant NB, Leung DH, Woodruff JM, Brennan MF. Brennan. Surgical management of intra-abdominal desmoidtumours. Br J Surg. 2000; 87: 608-613.
- Mace J, Sybil Biermann J, Sondak V, McGinn C, Hayes C, Thomas D, et al. Response of extraabdominal desmoid tumors to therapy with imatinibmesylate. Cancer 2002; 95: 2373-2379.
- Nishida Y, Tsukushi S, Shido Y, Wasa J, Ishiguro N, Yamada Y. Successful treatment with meloxicam, a cyclooxygenase-2 inhibitor, of patients with extra-abdominal desmoid tumors: a pilot study. J Clin Oncol. 2010; 28: 107-109.
- Klein WA, Miller HH, Anderson M, DeCosse JJ. The use of indomethacin, sulindac, and tamoxifen for the treatment of desmoid tumors associated with familial polyposis. Cancer. 1987; 60: 2863-2868.
- Tonelli F, Ficari F, Valanzano R, Brandi ML. Treatment of desmoids and mesenteric fibromatosis in familial adenomatous polyposis with raloxifene. Tumori. 2003; 89: 391.
- Patel SR, Benjamin RS. Desmoid tumors respond to chemotherapy: defying the dogma in oncology. J Clin Oncol. 2006; 24: 11.
- Ballo MT, Zagars GK, Pollack A, Pisters PW, Pollack RA. Desmoid tumor: prognostic factors and outcome after surgery, radiation therapy, or combined surgery and radiation therapy. Journal of Clinical Oncology. 1999; 17: 158-167.