Research Article
Seminal Vesicle-Rectal Fistula: A Review of an Unusual Complication Following Low Anterior Resection for Rectal Cancer
Steven Dixon1, Iain JD McCallum1, Chris Dennison2 and Mark Katory3*
1Department of Colorectal Surgery, Queen Elizabeth Hospital, UK
2Department of Radiology, Queen Elizabeth Hospital, UK
3Department of Surgery, Queen Elizabeth Hospital, UK
*Corresponding author: Mark Katory, Department of Colorectal Surgery, Queen Elizabeth Hospital, Gateshead Colorectal Unit, Sherriff Hill, Gateshead, UK
Published: 21 Sep, 2016
Cite this article as: Dixon S, McCallum IJD, Dennison
C, Katory M. Seminal Vesicle-Rectal
Fistula: A Review of an Unusual
Complication Following Low Anterior
Resection for Rectal Cancer. Clin Surg.
2016; 1: 1136.
Abstract
Introduction: Low anterior resection is the commonest operation in the United States of America undertaken for low rectal cancers. Seminal vesicle-rectal fistula is an extremely uncommon complication of this operation. The objective of this literature review is to investigate risk factors that lead to the development of seminal vesicle-rectal fistula; clinical presentation; and investigation and management options.
Methods: There were 9 articles of relevance which reported a total of 12 cases of seminal vesiclerectal fistula. All other iatrogenic or cryptogenic fistula was excluded.
Results: 12 cases were identified in the literature, and we describe 1 further case. Pneumaturia and fever were presenting symptoms in 10 of 13 cases. 69.2% (n=9) of cases presented within 2 weeks of the procedure. CT was the investigation of choice in 9 of 13 cases. A variety of surgical and conservative management plans were utilized. Conservative management was successful in 46.1% (n=6) of cases.
Discussion: This study provides the first concise review of seminal vesicle-rectal fistula following low anterior resection and also adds a further case. It is also the first article of its kind to recommend a treatment algorithm which consists of a trial of conservative management.
Introduction
In the United States of America there are 39 220 new cases of rectal cancer diagnosed each
year [1]. Low anterior resection is a sphincter-saving procedure undertaken to treat low rectal
cancers and can be undertaken laparoscopically or through an open procedure. Morbidity following
anterior resection for rectal cancer is common and has been reported in up to 32.6% of cases [2].
Complications following low rectal anastomosis include leak, abscess, fistulae and anastomotic
stenosis. Seminal vesicle-rectal (SV-R) fistulation is an uncommonly reported complication and as
such there is no algorithm for the management of these patients [3-11]. In this review risk factors
that lead to the development of SV-Rfistula are highlighted and management options for this
uncommon and challenging morbidity are proposed.
Surgical technique
Laparoscopic ultra-low anterior resection is typically performed with de-functioning loop
ileostomy for patients with rectal cancer within 12 cm from the anal verge. Pre-operatively these
patients often receive down-staging neo-adjuvant chemo-radiotherapy. Laparoscopic anterior
resection is then performed after an interval of six to ten weeks to achieve R0 resection. A double
staple technique using linear and trans-anal circular staple devices (e.g., CDH-29 Johnson & Johnson
Ethicon) is performed to achieve anastomosis and restoration of bowel continuity. A de-functioning
ileostomy is usually performed in the setting of previously irradiated tissue.
Methods
A MEDLINE search was undertaken over the date range 1974 to 2016. Inclusion criteria with search terms ‘fistula’, ‘anterior resection’ and ‘seminal vesicle’ were used. There were 9 articles of relevance which reported a total of 12 cases. All other iatrogenic or cryptogenic fistula was excluded.
Compliance with Ethical Standards
- Conflicts of interest
- Author A declares there he has no conflicts of interest
- Author B declares there he has no conflicts of interest
- Author C declares there he has no conflicts of interest
- Author D declares there he has no conflicts of interest
- Ethical approval
- The article does not contain ant studies with human participants or animals performed by any of the authors
- Informed consent
- Informed consent was obtained from all individual participants included in the study
Risk factors
SV-Rfistula is an extremely rare occurrence following low
anterior resection for rectal cancer. Only 12 cases have ever been
described in the literature [3-11]. As such there is no clear consensus
to explain why they occur or which patients are at risk. Neo-adjuvant
radiotherapy is routinely used to downstage rectal cancer prior to low
anterior resection. This can be associated with a more challenging
surgical dissection as tissue planes can be fibrosed as a result of
radiotherapy and dissection at the level of the distal rectum and
seminal vesicles can be extremely difficult.
Previously reported SV-Rfistulae invariably occurred after ‘low’
anterior resection. No fistulation has been reported following high
anterior resection where distal dissection of tissues does not routinely
extend to the level of the seminal vesicles. Several reports suggest
anastomotic dehiscence as a preceding event in the formation of
SV-Rfistula. Gaining access to a narrow male pelvis can be difficult.
Safe and accurate dissection avoiding injury to the seminal vesicles
and fascial planes can be challenging. Laparoscopic techniques may
provide the surgeon with an improved view using angled laparoscopes
and greater access low in a male pelvis. However laparoscopic access
does not appear to be protective as SV-Rfistulae is equally described
in the literature in open and laparoscopic cases [3-11].
Iatrogenic injury either by enbloc seminal vesicle resection or
inadvertent incorporation of the seminal vesicles during stapling at
the time of anastomosis is also postulated as a potential risk factor
[5]. In this single reported case the patient had malignant disease
invading the seminal vesicles which were resected enbloc [5].
Table 1
Clinical Presentation
On review of the literature it is widely accepted that fever and
pneumaturia are the commonest presenting symptoms. Fever is
described in 10 of 13 cases [4-7,9-12] and pneumaturia in 10 of 13
cases [3-6,8-11]. Fever is of course a very non-specific symptom
whereas pneumaturia should be considered highly suggestive of
fistulation between urinary tract and a newly formed low rectal
anastomosis in any setting. Other presenting symptoms of urinary
tract irritation or infection were also described such as frequency,
dysuria and testicular pain or swelling. Presentation of symptoms is
reported anywhere between post-operative day 5 to 53, however the
majority of patients presented within the first 2 weeks post operatively
(Table 1).
Investigation
The most common investigation of choice for detection of SVRfistulae
is computed tomography. This was used to identify 11
of 13 cases [4-11] and would also be the best modality to identify
evidence of anastomotic leak. Contrast studies such as water soluble
contrast enema, fistulography, vasogram and irrigoscopy were also
used in some cases. In order to confirm resolution or healing a water
soluble contrast enema was found to be the most widely used imaging
modality (Table 1).
Management
There are several options for the management of SV-Rfistula,
ranging from conservative measures to rather extensive surgical
intervention. Conservative treatment with antibiotics only can be
successful [5,6,8-10]. In four cases authors described catheterization
of the bladder in order to reduce intra-vesical pressure and encourage
healing. This was achieved trans-urethrally in three cases [5] and
supra-pubically in one [6]. Four of the thirteen reported cases
underwent de-functioning of the anastomosis using a proximal stoma;
two via colostomy [4,5] and two via an ileostomy [7,11]. Seven cases
reported successful resolution without stoma formation [3,5,6,8-10].
The earliest case of SV-R fistula was documented in 1989 by
Goldman who described undertaking a cutaneous vasostomy in
order to drain sepsis [3]. In this case clinical symptoms settled after a
prolonged period however the patient then developed recurrence and
died of metastatic disease. The use of cutaneous vasostomy is unlikely
to be necessary and subsequently has not been used in any other cases.
Nakajima reported SV-R fistulation in a patient with an extensive
rectal cancer invading the seminal vesicles requiring enbloc excision
[5]. Following failed conservative management, subsequent attempted
fistula closure using initially a gracilis muscle flap followed by a rectus
muscle flap was attempted both unsuccessfully. The patient eventually
developed recurrence and underwent successful pelvic exenteration.
Soda described fibrin glue administration directly into the fistula
tract via colonoscopy [8]. The authors describe resolution of fistula
symptoms with no recurrence at six months. Other studies have also
shown safe and effective use of endoscopic fistula management in the
form of fibrin glue [12]. Time to resolution appears to take months
as opposed to years although there is not consistent documentation
of resolution of symptoms and radiological evidence of fistula closure
[3-11].
It can be hypothesized that a de-functioning loop ileostomy is
either protective in the development of seminal vesicle-rectal fistulae,
or prevents the detection of the phenomena and masks symptoms
prior to ileostomy closure and clinical sequelae.
Aetiology
The commonest explanation given in the literature for the
sequence of events leading to SV-R fistula is anastomotic leak, small
pelvic abscess followed by development of fistula. Exposure of the
seminal vesicles following dissection at the level of Denonvilliers
fascia and subsequent local sepsis also at this anatomical level is a
logical theory to fistulae development [3-5,9]. This was described in 3
cases with radiological evidence of a leak (Figure 1).
Post-operative colitis has also been proposed as a hypotheses
associated with fistulae development [3 and 10]. Two authors described the
development of bloody diarrhea following microscopic inflammation
of the colonic mucosa (with or without positive clostridium difficile)
and suggested that this level of intraluminal inflammation either lead
to anastomotic incompetence or spontaneous fistula.
The anatomical difficulties encountered low down in a male
pelvis can provide challenges in respect to view and access of surgical
instruments. We hypothesize that on creation of the low anastomosis
inadvertent involvement of erroneous tissue such as the seminal
vesicle into the circular stapling device may go unrecognized and
could potentially provide an explanation for the development of SVRfistulae.
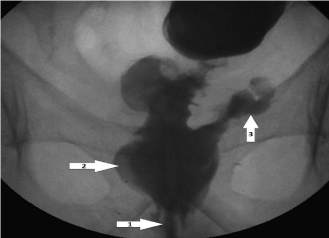
Figure 1
Figure 1
Water soluble contrast study demonstrating extravasation of contrast out of the neo-rectum with no clear fistula tract (1. Foley catheter in anal canal, 2. Contrast in neo-rectum, 3. Contrast extravasation out of bowel).
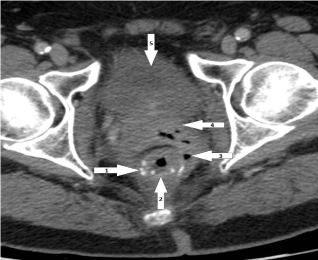
Figure 2
Figure 2
Axial view Computed Tomography imaging demonstrates fistula between neo-rectum, left seminal vesicle and bladder (1. Anastomosis staple line, 2.Neo-rectum, 3. Gas in fistula tract, 4. Seminal vesicle, 5.Urinary bladder).
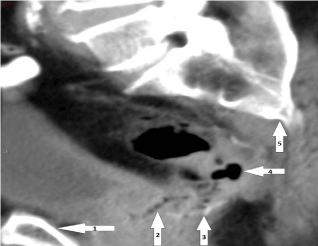
Figure 3
Figure 3
Oblique-sagittal reconstruction Computed Tomography imaging demonstrating fistula tract between neo-rectum and seminal vesicle. (1. Pubic symphysis, 2. Fistula tract 3. Anastomosisstaple line, 4. Neo-rectum, 5. Sacrum).
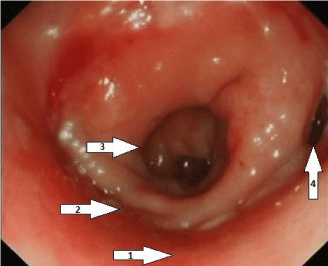
Figure 4
Figure 4
Flexible sigmoidoscopy demonstrates the anastomosis, true lumen and the fistula tract opening (1. Anal canal, 2. Anastomosis staple line, 3. Neo-rectal lumen, SV-R fistula tract).
Conclusion
SV-Rfistula following low anterior resection is an extremely rare
phenomenon. This usually presents with pneumaturia and fever
within two weeks following a low anterior resection in patients
who have not had a defunctioning loop ileostomy. CT provides
radiological proof of the abnormal communication and also evidence
of an anastomotic leak. Clinical presentation may be delayed in the
setting of a proximal diverting stoma. Conservative approach with
antibiotics is successful in 46% of cases and is appropriate as most
patients remain clinically well. However, if a conservative approach
fails, a de-functioning stoma or endoscopic fistula management with
fibrin glue can be considered.
Disruption of anastomotic integrity identified on contrast enema
is associated with subsequent SV-R fistulation (Figure 1). CT scan can
be used to demonstrate fistulae between the neo-rectum, left seminal
vesicle, prostate and urinary bladder (Figure 2 and 3). Abnormal
flexible sigmoidoscopy should also alert the clinician to the possibility
of SV-R fistulation and may be used to access the abnormal tract if
fibrin glue is deployed as a treatment modality (Figure 3). A third-line
treatment modality which is reported with poor success but may be
considered includes a muscular rotational flap in combination with
proximal diversion (Figure 4) .
Author Contributions
Study conception and design: Mark Katory.
Acquisition of data: Steven Dixon, Iain JD McCallum, Mark
Katory.
Analysis and interpretation of data: Mark Katory, Steven Dixon,
Iain JD McCallum, Chris Dennison.
Writing manuscript: Steven Dixon, Iain JD McCallum, Mark
Katory.
References
- American Cancer Society.
- Law WL, Chu KW. Anterior resection for rectal cancer with mesorectal excision: a prospective evaluation of 622 patients. Ann Surg. 2004; 240: 260-268.
- Goldman HS, Sapkin SL, Foote RF, Taylor JB. Seminal vesicle-rectal fistula. Report of a case. Dis Colon Rectum. 1989; 32: 67-69.
- Kawasaki S, Saito S, Hazama H, Tomioka H, Akamoto S, Okumoto T, et al. Seminal Vesicle-Rectal Fistula Secondary to Anastomotic Leakage after Low Anterior Resection for Rectal Cancer: Report of A Case. Jpn J Gastroenterol Surg. 2008; 41:1854-1859.
- Nakajima K, Sugito M, Nishizawa Y, Ito M, Kobayashi A, Nishizawa Y, Suzuki T. Rectoseminal vesicle fistula as a rare complication after low anterior resection: a report of three cases. Surg Today. 2013; 43: 574-579.
- Sykora R, Krhut J, Jonszta T, Nemec D, Havranek O, Martinek L. Fistula between anterior rectum wall and seminal vesicles as a rare complication of low-anterior resection of the rectum. Wideochir Inne Tech Maloinwazyjne. 2012; 7: 63-66.
- Hiraki M, Tokuoka M, Morita S. Seminal Vesicle-Rectal Fistula due to Anastomotic Leakage after Low Anterior Resection for Rectal Cancer: Report of A Case. Journal of Japan Society of Coloproctology. 2012; 65: 214-218.
- Soda T, Kiuchi H, Kakuta Y, Nakai Y, Mizushima T, Tsujimura A, et al. [Fibrin glue sealant for management of seminal vesicle-rectal fistula : a case report]. Hinyokika Kiyo. 2013; 59: 795-798.
- Mishima T, Fujita F, Okada S, Sakimura C, Matsushima H, Fujii M, et al. Rectovesical Fistula as a Rare Complication after Laparoscopic Low Anterior Resection: a Report of Two Cases. Jpn J Gastroenterol Surg. 2014; 47: 244-250.
- Kitazawa M, Hiraguri M, Maeda C, Yoshiki M, Horigome N, Kaneko G. Seminal vesicle-rectal fistula secondary to anastomotic leakage after low anterior resection for rectal cancer: a case report and brief literature review. Int Surg. 2014; 99: 23-27.
- Akahane M, Yoshimitsu M, Emi M, Mukaida H, Ohmori I, Kano M, et al. Seminal Vesicle-Rectal Fistula after Lap-LAR: Report of a Case. ESSR. 2014.
- Lippert E, Klebl FH, Schweller F, Ott C, Gelbmann CM, Schölmerich J, et al. Fibrin glue in the endoscopic treatment of fistulae and anastomotic leakages of the gastrointestinal tract. Int J Colorectal Dis. 2011; 26: 303- 311.