Research Article
Patient-Reported Outcomes (Pros) in Surgical Humanitarian Missions to Low- And Middle-Income Countries: A Scoping Review
Cheng H1, Webster F2,3, Platt J1,Causarano N4, Baxter NN3,5,6and Zhong T1,4*
1Department of Surgery, University of Toronto, Canada
2Departments of Family and Community Medicine, University of Toronto, Canada
3Institute of Health Policy, Management, and Evaluation, University of Toronto, Canada
4Departments of Surgery and Surgical Oncology, University Health Network, Canada
5Department of Surgery and Keenan Research Centre, Li Ka Shing Knowledge Institute, Canada
6Institute for Clinical Evaluative Studies (ICES), Canada
*Corresponding author: Toni Zhong, University Health Network, 8NU – 871, 200 Elizabeth Street, Toronto, Ontario, M5G 2C4, Canada
Published: 16 Jun 2016
Cite this article as: Cheng H, Webster F, Platt J, Causarano
N, Baxter NN, Zhong T. PatientReported
Outcomes (Pros) in Surgical
Humanitarian Missions to Low- And
Middle-Income Countries: A Scoping
Review. Clin Surg. 2016; 1: 1032.
Abstract
Background:Every year, health care personnel from developed nations travel to low- and middleincome countries (LMICs) to provide free surgical care to the local population. While the number of procedures performed by surgical humanitarian missions continues to increase, their impact on patients and their communities is not fully known. In particular, patient-reported outcome (PRO) reporting is lacking in surgical humanitarian missions.
Methods:A scoping review was conducted on PROs in surgical humanitarian mission to summarize the existing body of knowledge and identify gaps. The findings were presented at a plenary meeting of the Surgical Missions Outcomes Working Group.
Results:There were 43 articles in the literature that reported PROs from surgical humanitarian missions. The majority of studies (81%) were retrospective, and 12% were prospective. Sample sizes ranged from 15 to 18,653 patients. Short-term outcomes were reported in 62% of studies, intermediate outcomes in 41%, and long-term outcomes in 18%. Complication rates (81%) and performance indicators (72%), known as process indicators, were the most common outcome measures reported. Only four studies (9%) collected PROs and in none of the studies were the patient-reported outcome measures (PROMs) validated or pre-tested. At the plenary meeting, working group members reached a consensus that systematic reporting of all relevant mission outcomes and PROs in particular, is currently lacking and requires further research.
Conclusions:There is a paucity of literature on PROs for surgical humanitarian missions, with studies reporting mostly process indicators and lacking in long-term follow-up. More research is critically needed to validate existing PROMs or create new ones. Stakeholders involved in surgical humanitarian missions are urged to become aware of the multi-dimensional impact of their activities on patients and communities.
Background
Global Impact of Surgical Humanitarian Missions
Governments, non-governmental organizations (NGOs), and donors have worked for years
to improve essential surgical care to low- and middle-income countries (LMICs) by deploying
individual and teams of volunteers on short-term missions to provide surgical care in communities
where health infrastructure is lacking [1]. The extent and impact of the health services provided by the
uncounted surgical humanitarian missions around the world is unknown. In 2011, the International
Committee of the Red Cross and Médecins Sans Frontières together performed 211,300 surgeries
[2,3]. A survey conducted by the American College of Surgeons, Operation Giving Back, and the
Harvard Humanitarian Initiative found that NGOs play a substantial role in the delivery of surgical
services in LMICs, with some providing over 50,000 procedures annually [1]. While the number of
procedures performed by surgical humanitarian missions continues to rise, their impact on patients
and local communities has not been adequately assessed [4]. Standardized data reporting by surgical
missions is essential to determine their impact on the health of local
patients and communities.
Table 1
Measuring the success of surgical humanitarian missions
The disaster response following the 2004 South Asian tsunami
and 2010 Haitian earthquake raised international concerns about
the practices of some foreign medical teams. In response, the United
Nations’ Inter-Agency Standing Committee called for “greater
accountability, coordination, and more stringent oversight and
documentation of their work” [5]. As early as 2004, Roberts et al. [6]
reviewed 15 surgical mission publications and found that only four
reported health outcomes. In 2012, a systematic review concluded
that surgical missions commonly failed to meet data collection and
reporting standards required by national and international health
authorities [7]. Missions commonly aimed to measure health
outcomes but instead collected performance indicators, which
measure the process of implementation (i.e. geographical area
reached) and mission outputs (i.e. number of procedures performed).
Performance indicators are not proxies for actual health benefits. This
deficiency was similarly identified by a study from the United States
Department of Defense, which found only seven reports of health
outcomes of the total 178 mission impact reports [8].
PROMs in surgical humanitarian missions
Across health care, stakeholders (including the general public,
insurance companies and government) increasingly expects health
care providers and institutions to report on health-related outcomes
and make improvements where shortcomings are identified. The
growing attention on quality improvement has helped drive the
development of patient-reported outcome measures (PROMs) across
health disciplines. For instance, the Center for Medicaid and Medicare
Services and other agencies have historically used process measures
or adverse events for quality assessment. However, the use of patient
reported outcomes (PROs) has become a priority based on stated
goals by the National Quality Strategy and Institute of Medicine for a
more patient-centered approach [9]. PROs are increasingly required
as part of health care standards and reporting in the United States.
For example, the Food and Drug Administration now mandates
the use PROs to support medical product labeling claims, the US
government’s Affordable Care Act has created a Patient-Centered
Outcomes Research Institute, and the NIH has created the Patient
Reported Outcomes Measurement Information System (PROMIS)
initiative [10].
There remains considerable discussion regarding how to measure the quality of surgical care delivered by numerous humanitarian missions in communities around the world. To date, the majority of quality improvement initiatives in surgical missions have focused on measuring the frequency of adverse events such as peri-operative morbidity and mortality [11]. Adverse evente reporting is important when evaluating the outcome of life- or limb-saving surgeries; but for low-risk elective surgeries where the goal is to improve quality of life, the adverse event rate is less relevant and does not provide information about the patient's quality of life. For example, reporting low perioperative mortality following burn contracture release is expected but does not indicate if patients actually benefited from surgery. More meaningful outcomes in this case might include the ability of patients to independently perform daily activities and satisfaction with appearance. As this example demonstrates, PROs are better indicators of quality when the goal of surgery is to improve patient health-related quality of life. Their implementation would provide much-needed transparency and accountability, highly valuable data for policy making and fundraising, and stimulate improvements in patient care.
Methods
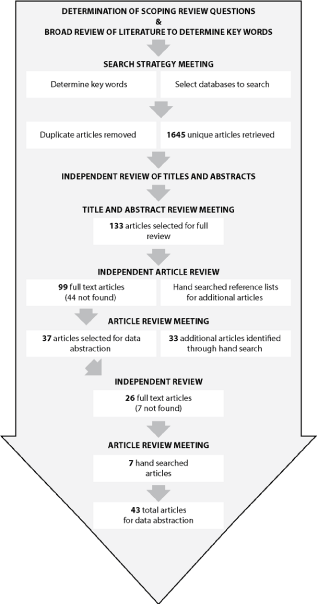
As described by Arksey and O’Mally, a scoping review is a ‘technique to map relevant literature in a field of interest’ [12]. In contrast with a systematic review, which more narrowly focuses on a particular question or study design, the scoping review tackles ‘broader topics where many different study designs might be applicable’ [12]. For this reason, the scoping review methodology is well-suited for surveying surgical humanitarian missions, which vary widely in content, study methodology, and outcome measures. We conducted a scoping review to identify existing literature reporting outcomes of surgical humanitarian mission. The keywords “surgical mission”, “medical mission”, “surgery”, and “developing countries” were used to search the Medline, Cochrane Library, and PsycINFO databases. After removing duplicates, the remaining 1645 abstracts were hand searched by three researchers (HC, JP, TZ) to select English-language articles from civilian surgical missions that reported outcome measures. We broadly defined ‘outcome measure’ as any data generated from mission activities, including performance indicators (e.g. number of surgeries performed), quality indicators (e.g. operative-site infections), and PROs (e.g. patient surveys). Only humanitarian missions providing elective procedures were included in this review. Disagreements in study inclusion were resolved through discussion and consensus amongst all members of the research team. Full-text articles were reviewed and reference lists of all articles meeting study inclusion criteria were searched for additional relevant articles.
The final step of our scoping review was to present and discuss
our findings with a committee of experts. Stakeholders from the
surgical humanitarian field, including surgeons, researchers, public
health experts, NGO leaders, and qualitative researchers, were invited
to form the Surgical Missions Outcomes Working Group working
group (Table 1). The working group met at a Canadian Institutes of
Health Research funded plenary meeting that was facilitated by an
independent moderator. The goals of the meeting were to: 1) review
and contextualize the findings of the modified scoping review, and 2)
identify emerging issues, research questions, and study methodologies
that will be the basis for future research protocols.
Figure 1
Results
Our modified scoping review yielded 43 unique articles published in 31 journals from 1990 to 2012 (Figure 1). The most common elective surgeries were cleft lip and palate reconstruction (20%), cataract correction (17%), and cardiac surgery (12%). The majority (81%) of studies were retrospective and 12% were prospective. Sample sizes ranged from 15 patients treated on two surgical missions to 18,653 patients treated by one humanitarian organization in 13 LMICs over an 8-year period [13,14]. Short-term outcomes (collected during the mission) were reported in 62% of studies, intermediate outcomes (collected less than one year from surgery) in 41% and long-term outcomes (collected one year or longer after surgery) in only 18%. Of the outcome measures reported, complication rates (81%) and performance indicators (72%) were the most common. Objective outcome measures (e.g. audiometry, visual acuity, facial measurements) were used in 40% of studies. Only four of the 43 articles (9%) collected PROMs (summarized in Table 2), with none using any validated PROM measures.
Table 2
1) Egbert et al. [15] reported a case series of 77 patients in Ghana who received outpatient cataract surgery. Forty-nine patients (64%) returned for a post-operative eye examination and structured interview between 12 and 29 months after surgery. The interview consisted of closed-ended questions about activities of daily living (e.g. reading, walking without assistance) that were created ad hoc. Patient responses were tabulated and no further data analysis was performed.
2) Lehnerdt et al. [16] presented a case series of 38 pediatric ear surgeries performed in northern Namibia. The surgical team returned six months after surgery and 31 patients (82%) received follow-up examinations and an ad hoc questionnaire. Performance indicators (e.g. types of tympanoplasties performed) and objective outcome measures (e.g. pure tone audiometry) were reported. In addition, patients were asked if their hearing had improved and if they still had ear pain.
3) Roux et al. [17] published a case series of 52 patients in Cambodia who underwent fronto-ethmoidal meningoencephalocele (MEC) repair. Four criteria were used to evaluate the surgical outcomes: 1) Patient and parent ratings of the cosmetic outcomes; 2) Surgeon rating of cosmetic outcomes; 3) Pre- and post-operative facial measurements; 4) Social impact of surgery as measured using a questionnaire administered pre- and post-operatively. Fifty patients (96%) were followed-up at least six months after surgery. The primary outcome measures used in this study (e.g. rating scale and social impact questionnaire) were developed ad hoc. Patient and surgeon ratings were tabulated and there was no further data analysis.
4) Sharp et al. [18] conducted a retrospective cohort studyin Cebu, Philippines to test the feasibility of conducting outcomes research during a surgical mission and to identify the salient outcome measures for cleft lip and/or palate patients and caregivers. Structured interviews (n=75) were conducted with patients and caregivers in the local dialect at least six months after surgery. Researchers asked three open-ended questions, and responses were analyzed using qualitative coding techniques.
Discussion
Although the profiled studies utilized PROMs, each has critical
methodological limitations. For example, none of the studies identified
specific measurable program goals, so despite using PROMs, it was
difficult to assess whether the mission met its objectives. In the study
by Lehnerdt et al. [16] the relationship between mission goals and
outcomes was not clear. Children were selected to receive surgery
because they had ear pathologies that prevented the use of hearing
aids, but the ability to use hearing aids after surgery was not one of
the outcomes measured. Follow-up was limited to a single visit six
months following surgery in three studies, and one study had a single
follow-up visit 12 to 29 months after surgery. Although we recognize
the immense challenge of coordinating follow-up in mission settings,
patients should ideally be reassessed at multiple time points over
longer periods of time. All four studies conducted interviews or
questionnaires that were developed ad hoc by the research team,
with no mention of having sought input from stakeholders, or pretesting
or validating the tool. With the exception of the questionnaire
described by Sharp et al. [18] researchers asked closed-ended
questions about specific symptoms and activities that cannot be
assumed to correlate with functional domains or HR-QOL. Roux et
al. [17] asked patients “Do you go to school?” and “Are you happy
at school”, but school attendance in Cambodia can be influenced
by other factors not related to the outcome of MEC reconstruction.
Questionnaire responses were also simply tabulated, and without
further data analysis, it is difficult to interpret the study findings and
draw conclusions.
Working Group Consensus / Recommendations
All working group participants agreed that more systematic reporting of relevant PROs was needed in order to understand the impact of surgical humanitarian missions, and that current knowledge was insufficient to develop the needed outcome measures. Key recommendations from the plenary meeting are summarized below.
Establishing appropriate outcome measures: Surgical missions must identify the salient health outcomes for the communities they wish to serve and the appropriate tools to evaluate them. A number of validated HR-QOL measures already exist, and their ability to measure surgical mission outcomes must be systematically evaluated. Alternately, researchers may develop and validate novel tools specifically for humanitarian missions. Researchers must also determine whether a single tool can be used for different countries and cultures and for specific mission objectives.
Study methodology: The working group proposed a mixed
methods approach to identifying key PROs and developing a pilot
measurement tool. Qualitative techniques would be used initially
to explore patient experiences, establish definitions, and generate
hypothesises for quantitative testing. Quantitative methods would
then ben needed to validate existing or newly-developed patient-
reported outcomes measures. Researchers must collaborate with local
health workers and other stakeholders to overcome language barriers
and ensure their work has contextual relevance. Health research
conducted in this setting must be sensitive to patient culture, social
values, and safety (both physical and psychological).
Conclusions
This is the first report to address the knowledge gap in PROs in surgical humanitarian missions. Research is needed to create valid and reliable PROMs, and also to implement them in a systematic, sustainable, and cost-efficient manner. We propose a rational research program developed through methodical review of current literature and consultation with key stakeholders and experts in the field. Our goal is to stimulate research interest and collaboration, and to urge all healthcare personnel involved in humanitarian missions to become more aware of the multi-dimensional impact of their activities on patients and their communities. Lessons learned from pre-testing, measuring and validating PROMs during surgical humanitarian missions to LMICs promises to advance the quality of care in nations across all incomes.
References
- Perkins RS, Casey KM, McQueen KA. Addressing the global burden of surgical disease: proceedings from the 2nd annual symposium at the American College of Surgeons. World J Surg. 2010; 34: 371-373.
- . ICRC Annual Report 2011. 2012: 83-86.
- Medecins Sans Frontiers Activity Report 2011. 2012: 9
- Burkle FM Jr, Nickerson JW, von Schreeb J, Redmond AD, McQueen KA, Norton I, et al. Emergency surgery data and documentation reporting forms for sudden-onset humanitarian crises, natural disasters and the existing burden of surgical disease. Prehosp disaster med. 2012; 27: 577- 582.
- Team WHOWI-ASCGPaS. Coordination and registration of providers of foreign medical teams in the humanitarian response to sudden-onset disasters: a Health Cluster concept paper. 2009. Accessed August 7, 2013.
- Roberts L, Hofmann CA. Assessing the impact of humanitarian assistance in the health sector. Emerg Themes Epidemiol. 2004; 1: 3.
- Nickerson JW, Chackungal S, Knowlton L, McQueen K, Burkle FM. Surgical care during humanitarian crises: a systematic review of published surgical caseload data from foreign medical teams. Prehosp disaster med. 2012; 27: 184-189.
- Reaves EJ, Schor KW, Burkle FM, Jr. Implementation of evidence-based humanitarian programs in military-led missions: part I. Qualitative gap analysis of current military and international aid programs. Disaster med public health prep. 2008; 2: 230-236.
- Lyman S, Hidaka C. Patient-Reported Outcome Measures-What Data Do We Really Need? J Arthroplasty. 2016; 31: 1144-1147.
- Brandon TG, Becker BD, Bevans KB, Weiss PF. Patient Reported Outcomes Measurement Information System® (PROMIS®) Tools for Collecting Patient-Reported Outcomes in Children with Juvenile Arthritis. Arthritis Care Res (Hoboken). 2016.
- Birkmeyer JD, Dimick JB, Birkmeyer NJ. Measuring the quality of surgical care: structure, process, or outcomes? J Am Coll Surg. 2004; 198: 626-632.
- Arksey H OML. Scoping studies: towards a methodological framework. International Journal of Social Research Methodology: Theory & Practice. 2005; 8: 19-32.
- Adams C, Kiefer P, Ryan K, Smith D, McCabe G, Allen P, et al. Humanitarian cardiac care in Arequipa, Peru: experiences of a multidisciplinary Canadian cardiovascular team. Can J Surg. 2012; 55: 171-176.
- Chu KM, Ford N, Trelles M. Operative mortality in resource-limited settings: the experience of Medecins Sans Frontieres in 13 countries. Arch Surg. 2010; 145: 721-725.
- Egbert PR, Buchanan M. Results of extracapsular cataract surgery and intraocular lens implantation in Ghana. Arch Ophthalmol. 1991; 109: 1764-1768.
- Lehnerdt G, van Delden A, Lautermann J. Management of an "Ear Camp" for children in Namibia. Int J Pediatr Otorhinolaryngol. 2005; 69: 663-668.
- Roux FE, Lauwers F, Oucheng N, Say B, Joly B, Gollogly J. Treatment of frontoethmoidal meningoencephalocele in Cambodia: a low-cost procedure for developing countries. J Neurosurg. 2007; 107: 11-21.
- Sharp HM, Canady JW, Ligot FA, Hague RA, Gutierrez J, Gutierrez J. Caregiver and patient reported outcomes after repair of cleft lip and/or palate in the Philippines. Cleft Palate-Craniofac J. 2008; 45: 163-171.