Research Article
Comparison of Clinical Results by Various Approach in Carpal Tunnel Syndrome
Kong GM, Kim JY, Lee JM and Lee YK*
1Department of Orthopedic Surgery, Busan Paik Hospital, Inje University, Republic of Korea
2Department of Orthopedic Surgery, Busan Korea Hospital, Busan, Republic of Korea
3Department of Orthopedic Surgery, Chonbuk National University Hospital 20, Republic of Korea
*Corresponding author: Young-Keun Lee, Department of Orthopedic Surgery, Chonbuk National University Hospital 20, Geonji-ro, Jeonju, 561-712, Republic of Korea
Published: 31 May, 2016
Cite this article as: Kong GM, Kim JY, Lee JM, Lee YK.
Comparison of Clinical Results by
Various Approach in Carpal Tunnel
Syndrome. Clin Surg. 2016; 1: 1020.
Abstract
Purpose: To examine the effect of diverse incision techniques in carpal tunnel decompression on patients’ postoperative pain and degree of satisfaction.
Materials and Methods: This study concerned 134 cases of 97 patients who were diagnosed with carpal tunnel syndrome from January 2010 to May 2012 and underwent carpal tunnel decompression
surgery at our hospital. The average follow-up period was 16 months (from 12 months to three
years). We compared traditional, minimally invasive, endoscopic carpal tunnel decompression
surgery. The subject’s palmar pain, cosmetic satisfaction, and Boston carpal tunnel questionnaire
result when they visited our hospital prior to the operation, three months postoperatively, six
months postoperatively, and one year postoperatively were used for the assessment of the surgery
outcome. Visual analogue scale (VAS) was used for patients’ subjective evaluation of palmar pain
around their scar. Using Boston carpal tunnel questionnaire, symptom severity and functional
status scores were evaluated separately.
Results: Palmar pain of those who underwent traditional carpal tunnel release significantly increased three months postoperatively compared to those who received the other methods (P=0.39), but
there was no difference in palmar pain among the different surgical techniques in the later followup
period. (P=0.69) Cosmetic satisfaction was gradually improved postoperatively. Cosmetic
satisfaction tended to be low in the subjects who received traditional carpal tunnel release but the
differences were not significant. (P=0.73) According to the Boston carpal tunnel questionnaire
result, symptom severity scale and functional status scale were no significant differences among the
three groups. (P=0.55, P=0.62).
Conclusion: It is considered that there are no great differences in palmar pain, cosmetic satisfaction,and Boston carpal tunnel questionnaire scores among patients who underwent different surgical
techniques for carpal tunnel syndrome in long-term follow-up.
Keywords: Carpal tunnel syndrome; Decompression surgery; Incision method; Prognosis
Introduction
Carpal tunnel syndrome is the most common disease among peripheral nerve entrapment
syndromes and has the symptoms of paresthesia, pain, and muscular atrophy of the dominated
area due to compression of the median nerve in the carpal tunnel. Basic treatment method is
conservative treatment but when the symptoms are severe or there is no response to the conservative
treatment, surgical treatment is recommended [1]. A diversity of surgical treatment methods have
been developed and introduced. Although numerous methods have been reported, they can be
largely classified into open carpal tunnel release and endoscopic carpal tunnel release that has been
attempted much recently, and open carpal tunnel release is subdivided again into traditional carpal
tunnel release and minimally invasive carpal tunnel release [2,3].
The reason why multiple surgical techniques have emerged and have been compared is because
each method’s advantages and disadvantages are obvious. Therefore, it is difficult to answer which
method is best.
Various factors in comparing excellence of the different techniques should be considered
and factors considered much include the degree of postoperative symptom alleviation, the rate of
complications, pain in the postoperative scar, and cosmetic satisfaction. Accordingly, this study
intended to investigate how different incision methods in carpal
tunnel decompression surgery affected pain in the scar patients felt,
cosmetic satisfaction, and functional recovery.
Table 1
Materials and Methods
This study concerned 134 cases of 97 patients who were
diagnosed with carpal tunnel syndrome from January 2010 to May
2012 and underwent carpal tunnel decompression surgery at our
hospital retrospectively. The average follow-up period was 16 months
(from 12 months to three years). In our hospital, three specialists
took charge of outpatients with carpal tunnel syndrome and each
specialist applied a different surgical technique, which enabled such
comparative investigation.
Specialist A performed traditional carpal tunnel decompression
surgery by making an incision from proximal 1cm of the distal wrist
crease to Kaplan’s cardinal line. The number of cases and patients
involving this surgical technique was 49 and 33, respectively. These
patients were classified into Group A. Their average age was 52.4
years old (from 38 years old to 64 years old). The number of males
was 5 and the number of females was 28. As for morbidity area, the
number of patients with carpal tunnel syndrome in one side was 17
and that of those with carpal tunnel syndrome in both sides was 16.
Specialist B performed minimally invasive carpal tunnel
decompression surgery by making an incision of 1.5 to 2.0 cm from
the pillar triangular area to the Kaplan’s cardinal line. The number
of cases and patients involving this surgical technique was 69 and
54, respectively. These patients were classified into Group B. Their
average age was 53.4 years old (from 25 years old to 65 years old).
The number of males was 9 and the number of females was 45. As for
morbidity area, the number of patients with carpal tunnel syndrome
in one side was 39 and that of those with carpal tunnel syndrome in
both sides was 15.
Specialist C made a 1cm transverse incision in the proximal
part of the wrist joint and performed endoscopic carpal tunnel
decompression surgery using a carpal tunnel relief kit (Linvatec R).
The number of cases and patients involving this surgical technique
was 16 and 10, respectively. These patients were classified into Group
C. Their average age was 55.2 years old (from 51 years old to 64 years
old). The number of males was 2 and the number of females was 8.
The number of patients with carpal tunnel syndrome in one side was
4 and that of those with carpal tunnel syndrome in both sides was 6
(Table 1).
Additional surgery such as synovectomy or neurolysis was
performed in none of the operations and whether there was hemorrhage
was identified by tourniquet deflation before postoperative skin
suture. All the patients were immediately allowed to conduct exercise
of the finger joints including the metacarpophalaneal joint. They
conducted flexion and extension exercise to a possible limit and
suture removal was carried out two weeks postoperatively.
Patients were diagnosed with carpal tunnel syndrome when
latency prolongation of motor nerves lasted for longer than 4.5msec
or differed by longer than 0.5msec compared to the normal side under
nerve conduction test together with clinical findings; Indication for a
surgery was not able to generalize because of different application by
each specialist. The criteria for inclusion as subjects were; Those who
underwent a surgery because there was no improvement through
conservative treatment for at least three months; Those who were
diagnosed with primary carpal tunnel syndrome; and those who were
aged between 25 and 65.
The subject’s palmar pain, cosmetic satisfaction, and Boston carpal
tunnel questionnaire result when they visited our hospital prior to the
operation, three months postoperatively, six months postoperatively,
and one year postoperatively were used for the assessment of the
surgery outcome. Visual analogue scale (VAS) was used for patients’
subjective evaluation of palmar pain around their scar. When there
was no symptom, zero point was given and when the symptom was
serious, 10 points were given. As for cosmetic satisfaction, when
the patients were most satisfied, zero point was given and when the
patient was least satisfied, 10 points were given. Using Boston carpal
tunnel questionnaire, symptom severity and functional status scores
were evaluated separately.
The result of this study was analyzed using SPSS version 12.0.
Analysis of variance test was used to verify postoperative effects and
degree of satisfaction of each group classified according to surgical
method. The significance level was set at P<0.05.
Results
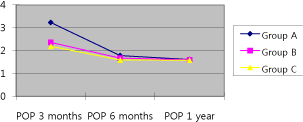
Regarding palmar pain, VAS decreased to an average of 3.23 points
three months after traditional carpal tunnel release, to an average of
1.78 points six months after traditional carpal tunnel release, and to
an average of 1.62 one year after traditional carpal tunnel release.
VAS decreased to an average of 2.36 points three months, an average
of 1.67 points six months, and an average of 1.60 points one year after
minimally invasive carpal tunnel release. VAS decreased to an average
of 2.19 points three months, an average of 1.59 points six months,
and an average of 1.58 points one year after endoscopic carpal tunnel
release (Figure 1). Even if there was statistically significant increase
in VAS of the group that underwent traditional carpal tunnel release
at three months after the surgery (P=0.03), there was no difference
among them in last follow-up (P=0.69).
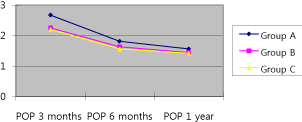
Cosmetic satisfaction decreased to an average of 2.67 points three
months, an average of 1.81 points six months, and an average of
1.56 points one year after traditional carpal tunnel release. Cosmetic
satisfaction decreased to an average of 2.25 points three months,
an average of 1.63 points six months, and an average of 1.44 points
one year after minimally invasive carpal tunnel release. Cosmetic
satisfaction decreased to an average of 2.2 points three months, an
average of 1.56 points six months, and an average of 1.42 points one
year after endoscopic carpal tunnel release (Figure 2). In comparison
among the three groups, the degree of satisfaction of the traditional
carpal tunnel release group was largely low but there was no significant
difference among the three groups (P=0.73).
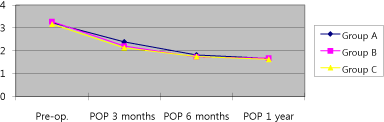
In the Boston questionnaire result of traditional carpal tunnel
release, the symptom intensity score decreased from 3.23 points prior
to the operation, to 2.39 points three months operatively, to 1.82 points
six months operatively, and to 1.67 points one year postoperatively.
In the Boston questionnaire result of minimally invasive carpal tunnel
release, the symptom intensity score decreased from 3.28 prior to the
operation to 2.21 points three months operatively, to 1.73 points six
months operatively, and to 1.68 points one year postoperatively. In the
Boston questionnaire result of endoscopic carpal tunnel release, the
symptom intensity score decreased from 3.17 prior to the operation
to 2.13 points three months operatively, to 1.75 points six months
operatively, and to 1.63 points one year postoperatively (Figure 3).
There was no statistically significant difference among the three groups
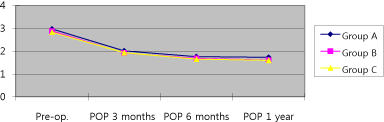
(P=0.55). In the Boston questionnaire result of traditional carpal
tunnel release, the functional state score decreased from 2.97 prior to
the operation to 2.01 points three months operatively, to 1.76 points
six months operatively, and to 1.73 points one year postoperatively.
In the Boston questionnaire result of minimally invasive tunnel
release, the functional state score decreased from 2.88 prior to the
operation to 1.92 points three months operatively, to 1.68 points six
months operatively, and to 1.61 points one year postoperatively. In
the Boston questionnaire result of endoscopic carpal tunnel release,
the functional state score decreased from 2.83 prior to the operation
to 1.93 points three months operatively, to 1.65 points six months
operatively, and to 1.6 points one year postoperatively (Figure 4).
There was no statistical significant difference among the three groups
(P=0.62).
Figure 1
Figure 2
Discussion
Although numerous surgical treatment methods for carpal
tunnel syndrome have been reported, they may be largely divided
into traditional open carpal tunnel release, endoscopic carpal tunnel
release that has been attempted much recently, and minimally
invasive carpal tunnel release [4].
That such many methods have emerged and each method’s
superiority over other methods has been stressed means that they did
not recover patients to their pre-operative, desired state or triggered
new problems, in other words, postoperative side effects.
Decompression surgery that conducts open incision of transverse
carpal ligaments through conventional skin incision has been long
performed as the most universal method and a lot of research has
reported its surgical efficacy as a safe and effective method [5,6].
Nonetheless, this surgical technique poses problems such as reduction
in hand strength, pillar pain, and increase in scars from incisions in
cosmetic terms [7-9]. In order to resolve these problems, endoscopic
carpal tunnel release has been introduced [10,11].
Figure 3
Figure 4
Endoscopic carpal tunnel release has many advantages compared
to traditional method; Patients’ pain is decreased during early
recovery period, problems such as tenderness of the incision area and
weakened mobility of the hand are reduced, and patients are able to
return to their job fast, and as a result, its excellence has been reported
much and it has been widely applied to many patients [12-15].
However, endoscopic method has the risk of neurological damage
because identification of anatomical structure is restricted, has the
possibility of incomplete incision of the transverse carpal ligaments,
costs a lot because of different equipment utilization, has the high
frequency of complications, and requires the surgeon’s proficiency
compared to other surgical techniques; Doubt about whether this
method is more useful than traditional methods has been raised
much [16].
Yu et al. conducted carpal tunnel release for 31 bilateral carpal
tunnel syndrome patients and compared endoscopic and open
methods; Although there were no statistical differences in all aspects
including tenderness of the scar from the surgery, the patients
preferred endoscopic release because the size of surgical incision was
smaller [7]. However, Isam et al. randomly performed open surgery
and 2-portal endoscopic surgery on 128 patients and followedup
them for five years and observed that there were no significant
differences between the two groups when they were compared two
years and five years postoperatively [17]. In particular, the authors
considered meaningful the fact that the two groups were similar in
their pain in the palmar and scar areas and degree of satisfaction in
their paper. Ferdinand and McLean as well performed endoscopic
release and open release on bilateral carpal tunnel syndrome patients
and reported that the two methods did not differ in recovery of
hand functions and the occurrence frequency of complications but
the endoscopic method required more time for the patients to be
accustomed to [18]. Minimal invasive decompression method has
similar advantages to endoscopic decompression method and is
not costly, but has a limitation of the surgery being performed with
restricted identification of anatomical structure [3]. Bromel et al. [19]
introduced minimally invasive incision method as a modification of
conventional open carpal tunnel release; with a small incision of 1.5
to 2.0 cm at the center of the palmar area, postoperative discomfort
and scar is decreased, splinting is unnecessary, and patients’ early
returning to the society is possible. Nevertheless, this surgical
technique does not completely remove pain in the surgical area and
fails to look at the nerves completely [20].
Besides studies that reported excellence of each surgical method,
there have been a lot of studies that compared different surgical
techniques from diverse perspectives.
Nakamichi et al. [21] compared percutaneous carpal tunnel release
and minimally invasive carpal tunnel release performed on 74 carpal
tunnel syndrome patients under ultrasonographic guide and reported
that those who underwent percutaneous carpal tunnel release had
significantly less pain, had more grip and key pinch strength, and
showed a higher degree of satisfaction. However, although the degree
of satisfaction related to pain and sensitivity of scar was higher in
patients who received percutaneous carpal tunnel release and such
degree of satisfaction was statistically significant only within a short
time period of three to six weeks postoperatively and thereafter there
were no great differences between the two groups. They had
compared minimally invasive carpal tunnel release and open carpal
tunnel release and reported that minimally invasive carpal tunnel
release was more excellent because it led to less pain [22]. The authors
regarded meaningful that the fact that the length of incision was
associated with patients’ degree of satisfaction within a short period
of time in their papers.
Cellocco et al. [23] also compared open restricted incision surgical technique and minimal open blind carpal tunnel applied to 185 carpal
tunnel syndrome patients and in their follow-up for 19 months,
minimal open blind surgical technique obtained a higher score but
in their follow-up for 30 months, there was no statistically significant
difference between the two groups. From their experiences they
asserted that not to infiltrate into the subcutaneous palmar space was
an important element to reduce postoperative pain and inflammation
and patients’ subjective cosmetic degree of satisfaction was high when
the incision length was short.
Biyani el al. [24] performed carpal tunnel release using two incision
lines avoiding the pillar area and reported significant decrease in pain
in an early period after the surgery but in a long-term follow-up there
was no difference.
Siegmeth et al. [25] randomly performed existing open decompression
surgery and modified open surgery preserving the cutaneous nerves
on 42 bilateral carpal tunnel syndrome patients in order to examine
whether pain occurred due to damage to the cutnaoues nerves and
reported that there was no difference in pain in the scar area and the
modified surgical method took a longer time to perform.
Despite slight differences among the reporters, in most cases,
there were no significant differences in pain according to the length of
incision in a long-term observation. The present study also obtained
a result that there were no differences in the subjects’ postoperative
pain and degree of satisfaction among the surgical techniques in longterm
follow-up.
However, the present study has some limitations. First, other
elements that may affect patients’ satisfaction with a surgery such as
their preoperative morbidity period, psychological conditions, nerve
pressure degree, and postoperative symptom alleviation were not
considered. Second, merely surgical methods, pain in the scar after a
surgery, and functional scales were compared. Thirds, indication for
a surgery and postoperative rehabilitation procedures were not the
same because multiple surgeons conducted the surgery. Therefore,
future research that well controls variables and accompanies objective
evaluation through pre- and post-operative electromyography and
ultrasound is considered necessary.
Different kinds of approaches to and surgical techniques of
carpal tunnel decompression are possible. Except for some special
cases, it cannot be said that a certain surgical technique is better for
a patient. Nonetheless, it is regarded that each surgeon has his or her
own good surgical technique and knows which surgical technique is
better. In other words, surgeon-dependent, not patient-dependent,
approaches are considered necessary. To sum up, a surgical technique
a surgeon is most accustomed to and most self-confident in is the
most appropriate one and will be able to produce the best outcome.
Conclusion
Palmar pain, cosmetic satisfaction, and Boston questionnaire result were not greatly different in a long-term follow-up according to the method of incision in a carpal tunnel surgery. Thus, selecting a surgical technique the surgeon is most self-confident in and accustomed to will lead to the best result and be appropriate for the patient.
References
- Palmer DH, Hanrahan LP. Social and economic costs of carpa ltunnel surgery. Instr Course Lec. 1995; 44: 167-172.
- Lee WP, Strickland JW: Safe carpal tunnel release via a limited palmar incision. Plast Reconstr Surg. 1998; 101: 418-424.
- Chung DW, Han CS, Shin DJ, Hwang JS. Minimal-incision carpal tunnel release. J Korean Soc Surg Hand. 2004; 9: 73-78.
- Scholten RJ, Mink van der Molen A, Uitdehaag BM, Bouter LM, de Vet HC. Surgical treatment options for carpal tunnel syndrome. Cochrane Database Syst Rev. 2007 4: CD003905.
- Chung DW, Han JS, Lee YG, Chang KS. The Results of Open Release in Carpal Tunnel Syndrome. J Korean Orthop Assoc, 1995; 30: 1733-1738.
- Dias JJ, Bhowal B, Wildin CJ, Thompson JR. Assessing the outcome of disorders of the hand. Is the patient evaluation measure reliable, valid,responsive and without bias? J Bone Joint Surg. 2001; 83B: 235–240.
- Yoo JD, Yun YH, Jung JM, Kim JH, Ko YD, Jung WC. Carpal tunnel release in the Bilateral carpal tunnel syndrome. J Korean Soc Surg Hand.2003; 8: 56-59.
- Phalen GS. The carpal tunnel syndrome. Seventeen years experience in diagnosis & treatment of 654 hands. J bone Joint Surg Am. 1966; 48: 211-228.
- Trumble TE, Diao E, Abrams RA, Gilbert-Anderson MM. Single-Portal Endoscopic Carpal Tunnel Release Compared with Open Release: A prospective, Randomized Trial, J Bone Joint Surg Am. 2002; 84: 1107-1115.
- Kluge W, Simpson RG, Nicol AC. Late complications after open carpal tunnel decompression. J Hand Surg. 1996; 21: 205–207.
- Brown RA, Gelberman RH, Seiler JG III, Abrahamsson SO, Weiland AJ, Urbaniak JR, et al. Carpal tunnel release. A prospective randomized assessment of open and endoscopic methods. J Bone Joint Surg. 1993; 75: 1265–1275
- Wilson KM. Double-incision open carpal tunnel release: an alternative to endoscopic release. J Hand Surg Am. 1994; 19: 907-912.
- Berger RA: Endoscopic carpal tunnel release. Hand Clin. 1994; 10: 625-636.
- Agee JM, McCarrol HR, North ER. Endoscopic carpal tunnel release using the single proximal incision technique. Hand Clin. 1994; 10: 647-659.
- Bozentka DJ, Osterman AL: Complications of endoscopic carpal tunnel release. Hand Clin, 1995; 11: 91-95.
- Chow JC. Endoscopic carpal tunnel release: Two-portal technique. Hand Clin. 1994; 10: 637-646.
- Atroshi I, Hofer M, Larsson GU, Ornstein E, Johnsson R, Ranstam J. Open compared with 2-portal endoscopic carpal tunnel release: a 5-year followup of a randomized controlled trial. J Hand Surg Am. 2009; 34: 266-272.
- Ferdinand RD, MacLean JG. Endoscopic versus open carpal tunnel release in bilateral carpal tunnel syndrome. J Bone Joint Surg. 2002; 84B: 375–379.
- Bromley GS. Minimal-incision open carpal tunnel decompression. J Hand Surg Am. Jan; 1994; 19: 119-120.
- Wheatley MJ, Hall JW, Faringer PD. Are the palmar cutaneous nerves safe during standard carpal tunnel release? Ann Plast Surg. 1996; 37: 251–253.
- Nakamichi K, Tachibana S, Yamamoto S, Ida M. Percutaneous carpal tunnel release compared with mini-open release using ultrasonographic guidance for both techniques. J Hand Surg Am Mar. 2010; 35: 437-445.
- Nakamichi K, Tachibana S. Ultrasonographically assisted carpal tunnel release. J Hand Surg Am. 1997; 22: 853-862.
- Cellocco P, Rossi C, Bizzarri F, Patrizio L, Costanzo G. Mini-open blind procedure versus limited open technique for carpal tunnel release: a 30 month follow-up study. J Hand Surg Am. 2005; 30: 493-499.
- Biyani A and Downes EM. An open twin incision technique of carpal tunnel decompression with reduced incidence of scar tenderness. J Hand Surg. 1993; 18: 331-334.
- Siegmeth AW, Hopkinson-Woolley JA. Standard open decompression in carpal tunnel syndrome compared with a modified open technique preserving the superficial skin nerves: a prospective randomized study. J Hand Surg Am. 2006; 3: 1483-1489.