Case Report
Hybrid Approach to Complex Arch and Thoracoabdominal Aneurysms in a Case of High-Risk Patient
Ohta H1*, Ohki T2, Kanaoka Y2, Kurosawa K2, Fukushima S3 and Toya N3
1Division of Vascular Surgery, Department of Surgery, Jikei University Graduate School of Medicine, Japan
2Division of Vascular Surgery, Department of Surgery, Jikei University School of Medicine, Japan
3Division of Vascular Surgery, Department of Surgery, Jikei University Kashiwa Hospital, Japan
*Corresponding author: Hiroki Ohta, Division of Vascular Surgery, Department of Surgery, Jikei University Graduate School of Medicine3-25-8 Nishi-shinbashi, Minato-ku, Tokyo 105-8461, Japan
Published: 04 May 2016
Cite this article as: Ohta H,Ohki T, Kanaoka Y, Kurosawa
K, Fukushima S, ToyaN. Hybrid
Approach to Complex Arch and
Thoracoabdominal Aneurysms in a
Case of High-Risk Patient. Clin Surg.
2016; 1: 1011.
Abstract
Endovascular therapy is a less invasive alternative treatment with aortic aneurysm. However in patients with multiple aneurysms, the surgical procedures orders of operating are controversial. The present report describes the case of a 65-year-old man with aneurysms in which the aortic arch (Zone 1) and the thoracoabdominal aorta (Crawford extent IV) presented challenge for complex aortic morphology. The patient had diagnosed as being inoperable at other university hospitals, because of a marked decrease of cardiopulmonary function. Therefore we preformed two-stage stent graft operations. Endovascular repair was achieved using additional common carotid artery (CCA) to CCA bypass into the aortic arch, and using fenestrated and branched stent graft into the visceral aortic segment. Before secondary operation, the patient had a contained rupture of the TAAA. His postoperative course was uneventful. The hybrid approach of surgical debranching and endovascular stent grafting for high-risk patients makes it possible to obtain a chance for effectively treating the multiple aneurysms.
Introduction
TWhen we perform endovascular treatment of aortic arch aneurysm or distal aortic aneurysm
with high-risk of cardiac arrest and thoracotomy, we secure a proximal sealing zone by performing
a carotid-carotid bypass or debranching prior to thoracic endovascular aortic repair (TEVAR).
Endovascular treatment of thoracoabdominal aortic aneurysm (TAAA) involving the visceral
arteries, the use of a branched stent graft or a hybrid technique combining a surgical debranching
with endovascular treatment is required.
We report a case of a patient with aortic arch aneurysm and TAAA who had diagnosed as being
inoperable at other university hospitals, because of a marked decrease of cardiopulmonary function,
in whom we undertook two-stage stent graft operations and obtained favorable results.
Case Presentation
A 65-year-old man with atrial fibrillation, diabetes mellitus, and hyperlipidemia was referred to
our division for TAAA. At the age of 39 years, he had undergone cholecystectomy, age of 56 years,
received a coronary artery bypass (left internal thoracic artery-left anterior descending coronary
artery: LITA-LAD). and, received a right lobectomy for lung cancer. An aortic arch aneurysm
(saccular type), 61 mm in diameter, and a Crawford extent IV TAAA, 74×54 mm in size (Figure 1), were revealed on the follow-up computed tomography (CT) after lobectomy. However, he was
diagnosed as being inoperable, because of the underlying cardiovascular and respiratory diseases,
therefore got a simply follow-up examination. As the patient had many risk factors, including reduced
cardiopulmonary function and diabetes, he was judged to be a high-risk candidate for the required
thoracolaparotomy. However, as both of the aneurysms had no neck with the proximal sealing zone,
they could not be treated with conventional stent grafts. Therefore, we made a treatment strategy to
perform two-staged operation using a hybrid operation and a branched TEVAR.
We decided to treat the aortic arch aneurysm first; as it was a saccular aneurysm, 61 mm in
diameter that required urgent treatment. And, if a branched TEVAR was performed first, the sheath
may cause migration of the stent graft at the time of zone 1 TEVAR as the second operation. Because
the aneurysm originated from the area adjacent to the left CCA, we planned to perform zone 1
TEVAR after securing the proximal neck by a CCA-CCA bypass.
As it takes several months to design and create a branched stent graft, we performed a branchedstent graft operation as the second operation two months after zone1 TEVAR. Prior to the operation, we explained to the patient and his
family that it was only a clinical attempt and obtained informed
consent from the patient. CT showed the aortic arch aneurysm, close
to the left CCA, the left subclavian artery arose from the aneurysm,
previous LITA-LAD bypass. Therefore we performed left CCA
and left SCA revascularization using CCA-CCA-LSCA bypass in
anticipation of zone 1 landing (Figure 2).
Three months later, the patient presented with abdominal pain.
He was diagnosed as having contained rupture of the TAAA at a local
general hospital. But he was told that it was inoperable. At the time,
we received a transport request to our hospital, as the branched stent
graft under preparation was to be completed soon; the patient was
transferred to our hospital for the operation. CT showed that the
aortic arch aneurysm was excluded completely and reduced, however,
the TAAA had increased in size to 75 × 68 mm (Figure 3) at the time of
readmission in our hospital.
After one week hypotensive treatment, we performed the branched stent graft operation.
A Palmaz stent, 7 mm, was placed in the celiac artery by
fenestration alone, while branches were created using balloonexpandable
covered stents (AdvantaV12, Atrium Medical, Hudson,
NH) measuring 6 mm in diameter for the superior mesenteric artery and left and right renal arteries (Figure 4 and 5). The patient had a
favorable postoperative course and was discharged 7 days after the
operation without complications such as renal failure or paraplegia.
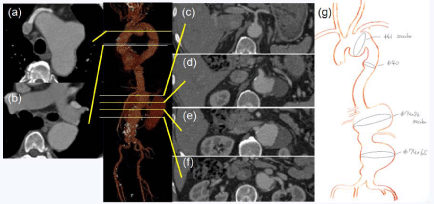
Figure 1
Figure 1
Axial computed tomography image showed saccular 61mm distal
aortic aneurysm (a), 40 mm descending aortic aneurysm (b), at the level of
the celiac artery origin (c), superior mesenteric artery origin (d), the level of
the right renal artery origin (e), the level of the left renal artery origin (f), 74×54
mm-saccular thoracoabdominal aortic aneurysm, 74×65 mm abdominal
aortic aneurysm. The schema of this patient's aneurysms (g).
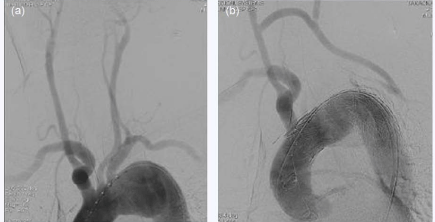
Figure 2
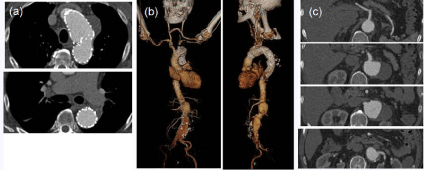
Figure 3
Figure 3
Computed tomography images after initial thoracic endovascular
aortic repair distal arch aneurysm is decreased the size of aneurysm. While
the size of thoracoabdominal aortic aneurysm is increasing gradually
Figure 4
Figure 5
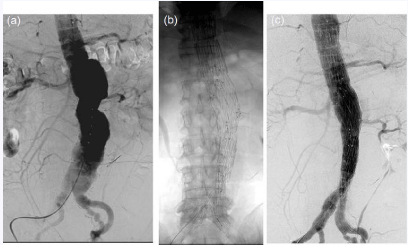
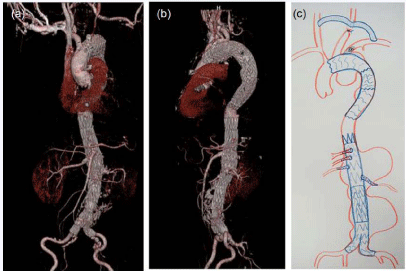
Figure 5
Volume-rendering reconstruction computed tomography images
(a,b) and completion schema (c) after hybrid operation.
Discussion
In patients with multiple aneurysms like this case, the surgical
procedures and order of operating are controversial, especially
when surgical treatment is indicated for both of lesions. If one-stage surgery is selected, the risk of paraplegia may be increased because
of high invasiveness [1]. While two-stage surgery is less invasive, a
high mortality rate has been reported during the interval between
operations and the most common cause of death is rupture of the
residual aneurysm [2].
Stent grafts are considered to be useful for the treatment of
multiple aneurysms, because patients can recover from surgery more
rapidly or the aneurysms can be treated simultaneously.
However, the present patient had complex aneurysms (an aortic
arch aneurysm and a thoracoabdominal aortic aneurysm), making
it difficult to treat either aneurysm with a stent graft alone. Surgical
replacement with a vascular graft was the standard treatment for both
aneurysms. However, if this method was selected, there would be a
long interval from the initial operation to the second procedure and
the completion of surgery would be delayed, resulting in an increased
risk of rupture of the residual aneurysm [3]. Therefore, we performed
the first operation by using a stent graft to shorten the recovery period
as much as possible.
We selected debranching TEVAR, which allowed the use of an offthe-shelf
stent graft, for the aortic arch aneurysm and simultaneously
placed an order for a branching stent graft. Fortunately, the patient
had no appreciable complications after debranching TEVAR and
soon returned to his full range of normal activities. According to
a recent report, the incidence of cerebral infarction is high after
debranching TEVAR [4]. If available, chimney grafts or branching
stent grafts may be used. This patient developed abdominal pain at 3
months after the initial procedure and this was considered to indicate
threatened aneurysm rupture. Because the branching stent graft
had already dispatched, we could salvage the patient by performing
surgery immediately after we received it.
If a branching stent graft had been selected for both the aortic
arch aneurysm and the thoracoabdominal aneurysm, initial surgery
on the arch region could not have been performed until completion of
the branching graft, resulting in a delay of 2-3 months. Accordingly,
it was better to treat the aortic arch aneurysm earlier with an off-theshelf
stent graft.
In patients like ours with multiple aneurysms both of which
require treatment, employing a stent graft is more effective than
replacement with a vascular graft, but a branching stent grafts cannot
be used for emergencies. It seems important to urgently develop
branching stent grafts that can also be used for emergency procedures.
Until then, we will have to rely on alternatives such as tailor-made
branching stent grafts and in-situ fenestration [5].
References
- Patel HJ, Upchurch GR Jr, Eliason JL, Criado E, Rectenwald J, Williams DM, et al. Hybrid debranching with endovascular repair for thoracoabdominal aneurysms: a comparison with open repair. Ann Thorac Surg. 2010; 89: 1475-1481.
- LeMaire SA, Carter SA, Coselli JS. The elephant trunk technique for staged repair of complex aneurysms of the entire thoracic aorta. Ann Thorac Surg. 2006; 81: 1561-1569.
- Saito Y, Fukuda I, Fukui K, Minakawa M, Suzuki Y. Simultaneous repair of multiple aortic aneurysms: be courageous in minimally invasive era. Ann Thorac Surg. 2014; 97: 1051-1053.
- Hirotaka A. Clinical outcomes of different approaches to aortic arch disease. J Vasc Surg. 2015; 61: 88-95.
- Canaud L, Faure EM, Branchereau P, Ozdemir BA, Marty-Ané C, Alric P. Experimental evaluation of complete endovascular arch reconstruction by in situ retrograde fenestration. Ann Thorac Surg. 2014; 98: 2086-2090.