Case Report
Pigmented Villonodular Synovitis with Gross Extraarticular Extension and Intraarticular Infiltration
Takatomo Mine*, Koichiro Ihara, Hiroyuki Kawamura, Ryutaro Kuriyama and Ryo Date
Department of Orthopaedic Surgery, National Hospital Organization Kanmon Medical Center, Japan
*Corresponding author: Takatomo Mine, Department of Orthopaedic Surgery, National Hospital Organization Kanmon Medical Center, 1-1 Choufusotoura, Simonoseki, Yamaguchi 752-8510, Japan
Published: 12 May, 2016
Cite this article as: Mine T, Ihara K, Kawamura H, Kuriyama R, Date R. Pigmented Villonodular Synovitis with Gross Extraarticular Extension and Intraarticular Infiltration. Clin Surg. 2016; 1: 1005.
Abstract
Pigmented Villonodular Synovitis (PVNS) is an unusual condition of unknown etiology. It is
divided into localized and diffuse forms. Once diagnosed, treatment usually consists of surgical
synovectomy. However, postoperative recurrence of PVNS occurs relatively frequently. This
is a case report of a 78-year-old woman who suffered PVNS recurrence in her knee twice. Gross
extraarticular extension and intraarticular infiltration is very rare. It is assumed that the lesion that
originated in the extraarticular bursa or peritendineum infiltrated the intraarticular site. The patient
was recurrence-free at 12 months after the operation, but six months later a few tumors were noted
in her knee. The subsequent recurrences were due to incomplete excision of the previous tumors
resulting from technical difficulties.
Keywords: Pigmented villonodular synovitis; Knee joint; Recurrence; Extra articular site
Introduction
Pigmented villonodular synovitis is a disease of unknown etiology that mainly develops in the synovial membrane of the knee joint [1,2]. It is said that the estimated incidence of PVNS is around 1.8 per million population [3]. It rarely involves multiple joints and often recurs after surgery. Gross extraarticular extension and intraarticular infiltration in the knee joint is very rare. We report a case of Diffuse Pigmented Villonodular Synovitis (DPVNS) that occurred in the popliteal region and that recurred after several surgical procedures.
Case Presentation
Fourteen years ago, a 78-year-old female, noted that she had a tumor on the medial side of the
popliteal region of her knee. As there were no notable symptoms (such as pain), she left it untreated.
However, over the years the tumor gradually grew, and due to restricted knee flexion, she became
unable to sit with her knees bent. Four years later, she underwent an open synovectomy for PVNS,
which was performed by another physician. After the operation, she was symptom-free, and her
postoperative course was generally satisfactory. However, three years after surgery, another tumor
developed on the lateral side of the left popliteal region, which caused her pain in her left knee joint
during ambulation. Under a diagnosis of recurrent PVNS, a second synovectomy was performed.
Four years after the second surgery, a tumor developed in the left popliteal region, which gradually
caused numbness in the lower left leg and a heavy sensation in the same leg during walking. The
patient was referred to our department for another surgical procedure.
A physical examination revealed swelling and slight local heat in the left knee joint. The range
of motion of the left knee was 0 to 125o. She has no muscular weakness and sensory disturbance in
her leg. A giant tumor, which was soft and elastic and displayed no adhesion to the skin, was found
to extend from the medial to the lateral side of the left popliteal region.
A radiograph showed an imaging feature that was indicative of a soft tissue tumor on the medial
side of the left popliteal region. No obvious bone destruction or osseous infiltration was noted.
MRI showed that the tumor in the popliteal region extended from the medial to the lateral side.
On T1-weighted images, it was displayed as an uneven low intensity signal, and on T2-weighted
images it exhibited a mixture of low and high intensity signals. Osseous infiltration was noted in part
of the posterior femoral condyle. On a coronal MRI image, the tumor appeared to enclose part of
the popliteal artery and vein in the popliteal region (Figure 1A and B). When Gd-enhanced images
were taken, the tumor appeared to be diffusely enhanced (Figure 1c).
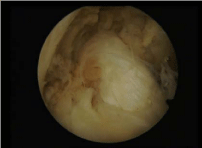
Arthroscopic inspection did not detect synovial proliferation in the supra-patellar pouch or the tibiofemoral joint on the medial or lateral side; however, in the intercondylar fossa, villous synovial proliferation, as well as the growth of a yellowish-brown nodular synovium measuring 5 mm in diameter was noted around the anterior and posterior cruciate ligaments (PCL) (Figure 2).
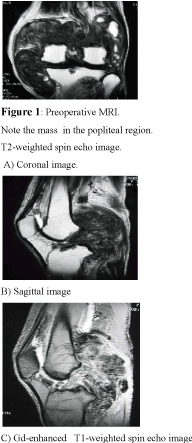
Figure 1
Figure 1
reoperative MRI.
Note the mass in the popliteal region.
T2-weighted spin echo image.
A) Coronal image.B) Sagittal image C) Gd-enhanced T1-weighted spin echo image
Figure 2
Figure 2
Arthroscopic view from an anterolateral portal the nodular synovium
at the intercondylar fossa.
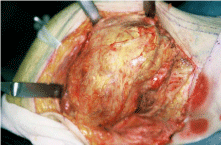
Upon macroscopic examination, a brownish tumor measuring 15 x 10 x 7 cm on the medial side and 7 x 7 x 5 cm on the lateral side was found in the popliteal region (Figure 3). On the medial side,the tumor had displaced the popliteal artery and vein, pushing them in the lateral direction. It had also infiltrated the medial head of the gastrocnemius, semimembranosus, semitendinosus, and gracilis muscles and the area around the associated tendons. The tumor, the medial head of the gastrocnemius muscle, and the semimembranosus muscle were excised en bloc. The tumor had also proliferated in the region where the PCL is attached to the tibia.
Figure 3
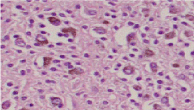
Figure 4
Figure 4
Photomicrograph showing diffuse proliferation of synovial cells and
a conglomeration of foam cells with iron deposition.
A histopathological examination revealed the diffuse proliferation
of synovial cells, a conglomeration of foam cells with iron deposition,
and a scattering of multinucleated giant cells. There were no mitotic
figures (Figure 4). These histopathological findings were consistent
with those of pigmented villonodular synovitis.
As a postoperative treatment, the patient’s leg was immobilized
with a plaster cast for 3 weeks. After the cast was removed, the patient
wore an orthosis with a support and underwent weight-bearing
training while taking care not to cause herself pain. One year after
surgery, the pain at her left knee joint was still associated with slight
swelling and fever. The range of motion of the joint was 5o during
extension (hyperextension) and 130o during flexion. Her muscle
strength was slightly reduced (flexion G, according to the manual
muscle test). However, the patient was no longer dependent on
orthotic devices, and there were no restrictions on her activities of
daily living. The patient remained recurrence-free 12 months after the
operation, but six months later a few tumors were noted on her knee.
Discussion
PVNS, a condition that mainly develops within the knee joints of
young and mature adults, is a tumor-like proliferative disease of the
synovium that involves chronic swelling and articular hematoma as
its major symptoms. There are various theories concerning its etiology
(e.g., inflammation, tumor formation, abnormal lipid metabolism, and trauma) but none have been conclusively proven. However, it
is believed that a synovium- or tendon-sheath-originating giant cell
tumor and an associated non-specific inflammatory reaction are most
the likely cause of this disease.
Gross extraarticular extension is very rare in this condition.
Flandry noted that pigmented villonodular synovitis penetrates
compartmental boundaries by mechanical means when the capacity
of a given compartment no longer accommodates the expanding
synovial mass [4]. One may consider the following two routes for
the progression of the disease in this case: the lesion that originated
at the intraarticular synovium infiltrated the extraarticular region or
it originated in the extraarticular bursa or peritendineum and then
infiltrated the intraarticular site. Enzinger et al. stated that PVNS
that develops outside of a joint often represents tumor proliferation
from the intra- to extraarticular regions [5]. However, the findings
in the present case did not include a history of intraarticular
hematoma; a tumor that was contiguous with the articular capsule
at the initial synovectomy; the localization of the intraarticular
lesion in the intercondylar region, despite the extensive spreading
of an extraarticular lesion; or infiltration of the extraarticular lesion
into intra- and intermuscular sites. Based on these findings, it was
concluded that in the present case the lesion that originated in the
extraarticular bursa or peritendineum had infiltrated the intraarticular
site, while the subsequent recurrences were due to incomplete tumor
excision.
The following have been employed for the surgical treatment
of PVNS: endoscopic synovectomy for the localized type, synovial
resection or therapy combining synovectomy and radiotherapy for
the diffuse type, and arthrodesis or joint replacement with a prosthesis
for the progressive type with osseous infiltration or joint deformation
[2-5]. Despite improvements due to advances in surgical technology
and in contrast to the localized type, synovectomy for diffuse PVNS
(as was performed in the present case) is still reported to be associated
with relatively high recurrence rates, even when the excision is
complete [6,7]. Due to problems, e.g., infiltration of the lesion into
the muscles, incomplete excision due to conditions such as adhesion,
damage to the articular components, and compromised articular
functions, the efficacy of synovectomy is limited when applied to
a diffuse-type PVNS that recurs at an extraarticular site. Diffuse
PVNS is an inflammatory disease when classified according to its
histopathology. However, it has been suggested that PVNS might be benign synovial neoplasm rather than an inflammatory disorder
[8]. The approach combining surgical synovectomy and radiotherapy
could be an interesting option for the diffuse type at a high risk of
recurrence [7,9-11]. However, little known about the long-term effect
of radiation used for knee joint PVNS, and long-term complication
should be considered after radiotherapy to prevent recurrence
References
- Atmore WG, Dahlin DC, Ghormley RK. Pigmented villonodular synovitis: A clinical and pathological study. Minnesota Med. 1956; 39: 196-202.
- Byers PD, Cotton RE, Deacon OW, Lowy M, Newman PH, Sissons HA, et al. The diagnosis and treatment of pigmented villonodular synovitis. J Bone Joint Surg. 1968; 50B: 223-238.
- Enzinger FM, Weiss SW. Soft Tissue Tumors. 3rd ed. Philadelphia, 1995; Pa: CV Mosby: 749-751.
- Flandry FC. Surgical treatment of diffuse pigmented villonodular synovitis of the knee. Clin Orthop. 1994; 300: 183-192.
- Ogilvie-Harris DJ, Basinski A. Pigmented villonodular synovitis of the knee; the results of total arthroscopic synovectomy, partial arthroscopic synovectomy, and arthroscopic local excision. J Bone Joint Surg. 1992; 74A: 119-123.
- . Rao AS, Vigorita VJ. Pigmented villonodular synovitis (giant-cell tumor of tendon sheath and synovial membrane). A review of eighty-one cases. J Bone Joint Surg. 1984; 66A: 76-94.
- Wiss DA. Recurrent villonodular synovitis of the knee; successful treatment with yttrium-90. Clin Orthop. 1982; 169: 139-144.
- Myers BW, Masi AT. Pigmented villonodular synovitis and tenosynovitis:A clinical epidemiologic study of 166 cases and literature review. Medicine (Balimore). 1980; 59: 223-238.
- Blanco CER, Leon HO, Guthrie TB. Combined partial arthroscopic synovectomy and radiation therapy for diffuse pigmented villonodular synovitis of the knee. Arthroscopy 2001; 17: 527-531.
- de Carvalho LH Jr, Soares LFM, Gocalves MBJ, Temoni EF, de Melo Silva O Jr. Long-term success in the treatment of diffuse pigmented villonodular synovitis of the knee with subtotal synovectomy and radiothrapy. Arthroscopy 2012; 28: 1271-1274.
- O’Sullivan B, Cummings B, Catton C, Bell R, Davis A, Fornasier V, et al. Outcome following radiation treatment for treatment for high-risk pigmented villonodular synovitis. Int Radiat Oncol Biol Phys. 1995; 32: 777-786.