Research Article
Ipsilateral Lung Resections for Postoperative Recurrent or Second Primary Lung Cancer
Masahiro Miyajima*, Yucky Takahashi, Ryunosuke Maki, Makoto Tada, Kodai Tsuruta, Tajirou Mishina and Atsushi Watanabe
Department of Thoracic Surgery, Sapporo Medical University School of Medicine, Japan
*Corresponding author: Masahiro Miyajima, Department of Thoracic Surgery, Sapporo Medical University School of Medicine, South 1, West 16, Chuo-ku, Sapporo, Hokkaido 060-8543, Japan
Published: 01 Nov, 2018
Cite this article as: Miyajima M, Takahashi Y, Maki R, Tada
M, Tsuruta K, Mishina T, et al. Ipsilateral
Lung Resections for Postoperative
Recurrent or Second Primary Lung
Cancer. Clin Surg. 2018; 3: 2193.
Abstract
Purpose: This study aimed to report our experience with repeated ipsilateral pulmonary resection
in patients with local recurrent and second primary lung cancer, and to assess operative mortality
and long-term outcomes.
Methods: The medical records of all patients who underwent a second ipsilateral lung resection for
local recurrent and second primary lung cancer from 2000 to 2016 were reviewed.
Results: Thirteen (0.9%) patients (group 1) had a local recurrence. The second operation consisted
of completion pneumonectomy in three cases, completion lobectomy in two, segmentectomy in
three, and wedge resection in five. The remaining eight (0.6%) patients (group 2) had a new primary
lung cancer. The second pulmonary resection was completion pneumonectomy in one, completion
lobectomy in one, lobectomy in four, and segmentectomy in two. Overall hospital mortality was
4.8%, including one postoperative death. Five-year survival after the second operation was 35% and
85% with a median survival of 29 and 36 months in groups 1 and 2, respectively (p>0.05).
Conclusion: These long-term results justify the need for complete work-up of patients with
ipsilateral local recurrent or second primary lung cancer in our hospital. Surgical treatment should
be considered when the patients have no distant metastasis and are in good health.
Introduction
The recurrence of lung cancer after complete resection generally results in a poor prognostic status and short life expectancy. When a single lung nodule is detected during follow-up, it sometimes suggests the possibility of systemic metastasis; however, there is always concern regarding the development of second primary lung cancer. Although there are criteria that can be applied in this situation, it is sometimes very difficult to distinguish between a new lung cancer and a recurrent one. Therefore, some researchers have insisted an aggressive surgical approach, whenever possible, as the survival rate after surgery is quite good [1-4]. On the other hand, many doubts have been expressed concerning the utility of repeated surgery for recurrent lung cancer due to the treatment’s poor overall survival [5,6]. In particular, ipsilateral re-operation is technically demanding because of the occurrence of dense adhesions and a high risk of pulmonary artery bleeding. However, the widespread use of video-assisted thoracic surgery for lung cancer has made re-resection of the lung more common. We are convinced of the value of an aggressive surgical approach in all patients whose functional condition makes resection possible. Therefore, the aim of this study was to report the results from ipsilateral re-resection for patients with recurrent or second primary lung cancer, focusing on mortality and survival characteristics of these two groups of patients.
Materials and Methods
From 2000 to 2016, 1,390 patients underwent radical pulmonary resection for non-small-cell
lung carcinoma (NSCLC). Of these, 21 (1.5%) consecutive patients underwent repeated ipsilateral
surgical resections for recurrent lung cancer after curative resection for lung cancer. The second
operation was conducted for local recurrence (n=13, 0.9%; group 1) or second primary lung cancer
(n=8, 0.6%; group 2). The second primary lung cancers were defined using the criteria outlined by
Martini and Melamed [7]. In cases where the histology was the same as the first surgery, subtypes
and the degree of differentiation of the histology were considered to distinguish a new lung cancer
from a recurrent one. Patient and surgical characteristics and outcomes are shown in Table 1.
The operations were performed by a group of three thoracic surgeons' at a single hospital. Every
patient was followed-up by the same surgeons on a regular follow-up
schedule (every 3 months for 2 years, then every 6 months for the
next 3 years). A chest Computed Tomography (CT) was performed
every 6 months. When recurrent disease was suspected in the lung,
repeated CT scan was performed every 2 months, and Positron
Emission Tomography (PET), bronchoscopy and/or percutaneous
needle aspiration were also performed. The descriptive statistics are
summarized as the median or mean for the continuous variables and
as frequencies and percentages for the categorical variables. Survival
and the disease free rate were analyzed by the Kaplan-Meier and
log-rank methods on SPSS for Windows, Version 22.0 (SPSS Inc.,
Chicago, IL, U.S.A.). All differences were considered significant at a
p value less than 0.05.
Table 1
SD: Standard Deviation. Data are presented as number (percentage), unless noted otherwise
Results
Cumulative survival curves of all 21 patients with local recurrent
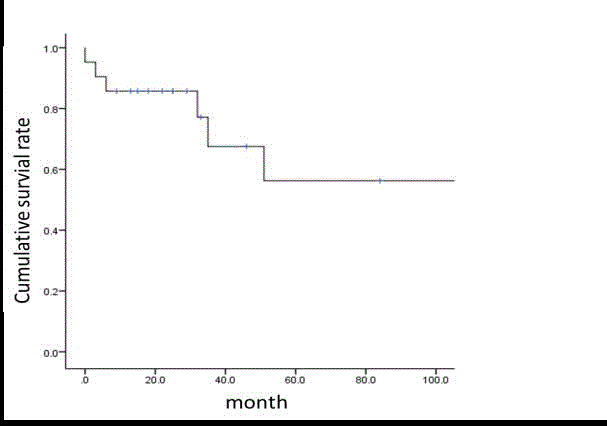
and second primary lung cancer are shown in Figure 1. Five-year
survival after the second operation was 58.0% with a median survival
of 38 months. Overall hospital mortality of all patients was 4.8%.
Group 1: local recurrences
Thirteen patients (male, n=9; female, n=4) underwent a second
pulmonary resection for local recurrence. Mean age at the time of the
first operation was 60 years (range, 40-70 years). Only one patient
was symptomatic at the time of detection. In the other 12 patients,
the cancer recurrence was detected at the scheduled examination at
4-6 months. The local recurrences developed at a mean interval of 59
months (range, 3-126 months). The detailed operative characteristics
of patients in group 1 are described in Table 2, and the cumulative
disease-free survival curve is shown in Figure 2. The 5-year diseasefree survival rate for patients with recurrent tumor after the second
operation was 43%.
In group 1, the first resection was considered radical for all
patients. The second resection was considered radical in all but
one patient; of these 12 patients, complications occurred in three
patients and included cardiac arrhythmias in one, recurrent nerve
paralysis in one, and prolonged air leak in one. No patients died
intra operatively. The mean follow-up period of the 13 patients with
local recurrence who survived the second operation was 38 months
(range, 3-109 months). Currently, six of the 13 patients are alive and
are free from any known recurrent cancer after 109, 33, 29, 25, 22
and 15 months from the second operation, respectively. Of the seven
patients who died, recurrent lung cancer was known to be present,
and was identified as the cause of death in four patients. Five-year
survival after the second operation was 35% with a median survival of
29 months (Figure 3).
Group 2: second primary lung carcinomas
Eight patients (male, n=5; female, n=3) underwent a second
pulmonary resection for second primary lung cancer. Mean age at
the time of the operation for the first primary cancer was 60.0 years
(range 48-74 years). The criteria that were used to distinguish that the
second lung tumor was a new primary cancer included different cell
type in two patients and location in a different ipsilateral lobe in six.
Type of resections, histology, postoperative staging, and the second
operations are shown in Table 3. The second cancer was symptomatic
in only one patient. The mean interval between the initial and second
treatment was 88 months (range, 54-144 months). Resection of the
tumor was complete in all cases. The 5-year disease-free survival
rate for patients with second primary lung cancer after the second
operation was 74% (Figure 2).
One patient died during the follow-up period because of a third
recurrence of the cancer, which were multiple brain metastases.
The mean follow-up for the seven patients who survived the second
operation was 75 months (range, 13-144 months). Currently, all seven
patients are alive with three patients who have evidence of recurrent
cancer. Five-year survival after the second operation was 85% with a
median survival of 36 months (Figure 3).
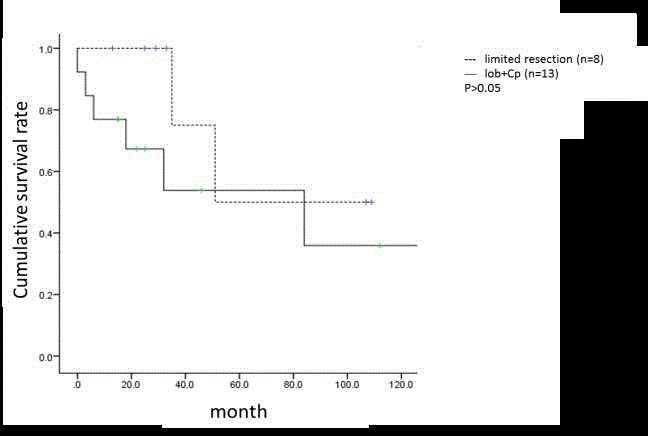
Actuarial survival of all 21 patients according to the surgical
procedure is shown in Figure 4. No significant difference was detected
in survival between the limited resection group (n=8) and lobectomy/
completion peumonectoy group (n=13) in this study.
Figure 1
Figure 1
Actuarial survival from the time of the second operation for patients
with local recurrent and second primary lung tumor (21 cases).
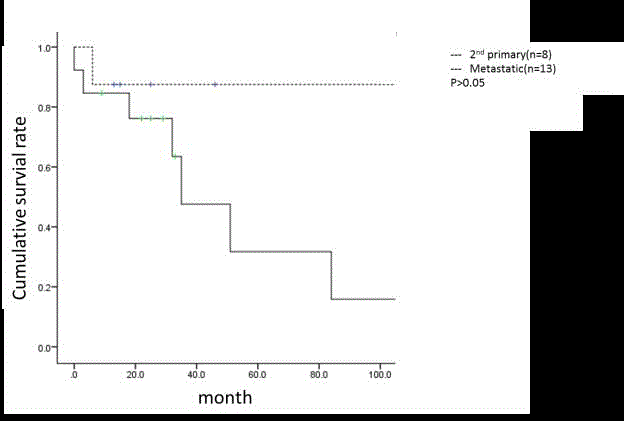
Figure 2
Figure 2
Actuarial survival for recurrent lung cancer with 2nd primary and
metastatic tumor after the second operations.
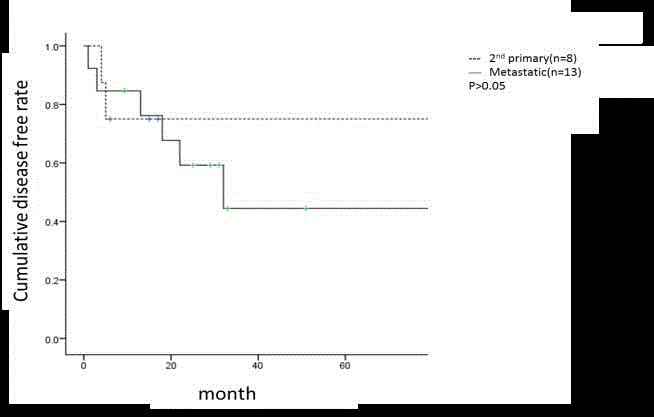
Figure 3
Figure 3
Cumulative disease free rates of recurrent lung cancer with 2nd
primary and metastatic tumor.
Table 2
C: Completion; LLL: Left Lower Lobectomy; LP: Left Pneumonectomy; LUL: Left Upper Lobectomy; RLL: Right Lower Lobectomy; RML: Right Middle Lobectomy; RP: Right Pneumonectomy; RUL: Right Upper Lobectomy; Seg: Segmentectomy; W: Wedge resection
Figure 4
Figure 4
Acturial survival of recurrent lung cancer with 2nd primary and
metastatic tumor according to the surgical procedure.
Table 3
C-RP: Completion Right Pneumonectomy; LLL: Left Lower Lobectomy; LUL: Left Upper Lobectomy; RLL: Right Lower Lobectomy; RML: Right Middle Lobectomy; RUL: Right Upper Lobectomy; Seg: Segmentectomy; W: Wedge resection
Discussion
Recent improvements in diagnostic tools, such as high-resolution
CT scan and PET scan, allow physicians to detect recurrent lung
cancer much earlier than before. Westeel et al. [8] reported that
intensive follow-up may improve patient survival through the
detection of recurrences at an asymptomatic stage after surgery for
NSCLC. For the detection of residual or recurrent NSCLC, Haberkorn
et al. reported that, PET had a sensitivity of 100% and a specificity of
61.5% to 92.0%, showing the superiority of PET scan compared to
conventional CT scan [9]. The early detection of recurrences may be
more effective in improving patient outcomes compared to therapy
that is administered when the patient becomes symptomatic from
the tumor [10]. Moreover, early detection of the tumor enables the
use of limited resection, thereby avoiding riskier surgeries, such as
completion lobectomy or completion pneumonectomy.
The Lung Cancer Study Group reported that for primary lung
cancer [11], a resection is less extensive than lobotomy, which places
the patient at an increased risk of local recurrence, and subsequently
decreases the chances of long-term survival. The limited resections
that were completed in the second primary lung cancer group (group
2) might have increased the risk for locoregional recurrence, but our
study did not show that the extent of the resections influenced the
survival, as was reported in other studies [12,13]. Major complications
occurred in 14% of our patients after the second resection, which is
comparable to the previously reported results of pulmonary resection
for recurrent lung cancers [14,15].
Voltolini et al. [14] investigated the type of surgical treatment
used in cases of metachronous second primary lung tumor, and
reported that wedge resection was a reasonable and safe alternative to
the standard resections in elderly patients or in those patients with a
poor respiratory reserve and after a pneumonectomy.
Some reports have suggested that patients with a second primary
lung cancer have a more favorable prognosis than patients with
locally recurrent disease [3,5]. However, other studies did not reveal a
significantly different survival between patients surgically treated for
a second primary lung cancer or those surgically treated for locally
recurrent disease [14]. Similarly, our data showed that the 5-year
survival rates were not significantly different between patients with
second primary lung cancer and those with recurrent lung cancer.
Overall, our 5-year survival of 74% for second primary lung cancers
and 43% for recurrent lung cancers was far better than what would be
expected for local recurrent disease.
Although we did not show a statistically significant positive
association of sublobar resection on survival rate, sublobar resection
was not inferior to lobar and completion pneumonectomy. From our
experience with surgical treatment of second primary or recurrent
lung cancer, we conclude that sublobar resection and wedge resection,
when feasible, are the treatments of choice. Neither anatomical
lobectomy nor completion lobectomy yielded a significant overall
survival advantage compared with these limited resection methods.
Therefore, segmentectomy is an ideal surgical procedure to minimize
recurrence in situations where a parenchymal-sparing technique is
indicated or recommended. Completion pneumonectomy should
only be performed in carefully-selected patients.
The main limitation of this study was its retrospective nature and
lack of randomization, which may have led to potential bias in patient
selection and surgeon’s choice of operative approach. Prospective,
randomized studies are necessary to further understand the feasibility
of ipsilateral re-resection for second primary or recurrent lung cancer.
Conclusion
The long-term patient outcomes of this study justify the need for complete work-up of patients with ipsilateral local recurrent and ipsilateral second primary lung cancer at our hospital. Surgical treatment should be considered when patients have no distant metastasis and are in good health.
References
- Rosengart TK, Martini N, Ghosn P, Burt M. Multiple primary lung carcinomas: prognosis and treatment. Ann Thorac Surg. 1991;52(4):773-9.
- Antakli T, Schaefer RF, Rutherford JE, Read RC. Second primary lung cancer. Ann Thorac Surg. 1995;59(4):863-7.
- Okada M, Tsubota N, Yoshimura M, Miyamoto Y. Operative approach for multiple primary lung carcinomas. J Thorac Cardiovasc Surg. 1998;115(4):836-40.
- Deschamps C, Pairolero PC, Trastek VF, Payne WS. Multiple primary lung cancers. Results of surgical treatment. J Thorac Cardiovasc Surg. 1990;99(5):769-78.
- Pairolero PC, Williams DE, Bergstralh EJ, Piehler JM, Bernatz PE, Payne WS. Postsurgical stage I bronchogenic carcinoma: morbid implications of recurrent disease. Ann Thorac Surg. 1984;38(4):331-8.
- Nielsen OS, Boas J, Bertelsen S. Reoperation for recurrent bronchogenic carcinoma. Scand J Thorac Cardiovasc Surg. 1984;18(3):249-50.
- Martini N, Melamed MR. Multiple primary lung cancers. J Thorac Cardiovasc Surg. 1975;70(4):606-12.
- Westeel V, Choma D, Clément F, Woronoff-Lemsi MC, Pugin JF, Dubiez A, et al. Relevance of the intensive postoperative follow-up after surgery for non-small cell lung cancer. Ann Thorac Surg. 2000;70(4):1185-90.
- Haberkorn U. Positron emission tomography (PET) of non-small cell lung cancer. Lung Cancer. 2001;34(2):S115-21.
- Aziz TM, Saad RA, Glasser J, Jilaihawi AN, Prakash D. The management of second primary lung cancers. A single centre experience in 15 years. Eur J Cardiothorac Surg. 2002;21(3):527-33.
- Ginsberg RJ, Rubinstein LV. Randomized trial of lobectomy versus limitedresection for T1N0 non-small cell lung cancer. Lung Cancer Study Group. Ann Thorac Surg. 1995;60(3):615-23.
- Fujimoto T, Zaboura G, Fechner S, Hillejan L, Schröder T, Marra A, et al. Completion pneumonectomy: current indications, complications, and results. J Thorac Cardiovasc Surg. 2001;121(3):484-90.
- Zuin A, Andriolo LG, Marulli G, Schiavon M, Nicotra S, Calabrese F, et al. Is lobectomy really moreeffective than sublobar resection in the surgical treatment of second primary lung cancer? Eur J Cardiothorac Surg. 2013;44(2):e120-5.
- Voltolini L, Paladini P, Luzzi L, Ghiribelli C, Di Bisceglie M, Gotti G. Iterative surgical resections for local recurrent and second primary bronchogenic carcinoma. Eur J Cardiothorac Surg. 2000;18(5):529-34.
- Hamaji M, Allen MS, Cassivi SD, Deschamps C, Nichols FC, Wigle DA, et al. Surgical treatment of metachronous second primary lung cancer after complete resection of non-small cell lung cancer. J Thorac Cardiovasc Surg. 2013;145(3):683-91.