Clinical Image
Dramatic Complications after an Ascending Aortic Aneurism Surgery
Edward Pietrzyk1 and Stanislaw Gluszek2,3*
1Department of Cardiac Surgery, Provincial Polyclinic Hospital, Poland
2Department of Surgery and Surgical Nursery with a Genetics Laboratory, Jan Kochanowski University, Poland
3Department of General Oncology and Endocrinology Surgery, Provincial Polyclinic Hospital, Poland
*Corresponding author: Stanislaw Gluszek, Department of Surgery and Surgical Nursery with a Genetics Laboratory, Faculty of Medicine and Health Sciences, Jan Kochanowski University, Kielce, Poland
Published: 12 Oct, 2018
Cite this article as: Pietrzyk E, Gluszek S. Dramatic
Complications after an Ascending Aortic
Aneurism Surgery. Clin Surg. 2018; 3:
2157.
Clinical Image
A 54-year-old man, who had, 6 months earlier, been suffering from phlegmon of the right forearm
with sepsis, was operated on because of an ascending aortic aneurysm with aortic insufficiency.
Intraoperatively, an atresic pericardial sac was found - it most probably appeared in the course of
pericarditis after sepsis. A Bent all-de Bono operation was performed. Histopathological examination
of the aortic wall: Aneurysmal inflammatorium aortae. The bacteriological examination did not
show any micro-organisms. On the sixth day after the operation, mediastinitis with a sternal splitting
appeared and there was purulent leakage from the wound with symptoms of septic shock. Wound
bacterial culture: methicillin- susceptible S. aureus (MSSA), methicillin- susceptible S. epidermidis
(MSSE). A debridement was performed and flow drainage with betadine was inserted. The sternum
was stitched together. Ciprofloxacin and clindamycin were used intravenously. After 5 days,
exacerbation of sepsis symptoms appeared with abundant, purulent leakage from the wound with
the re-divergence of the sternum, mediastinum inflammation, ascending aorta prosthesis infection
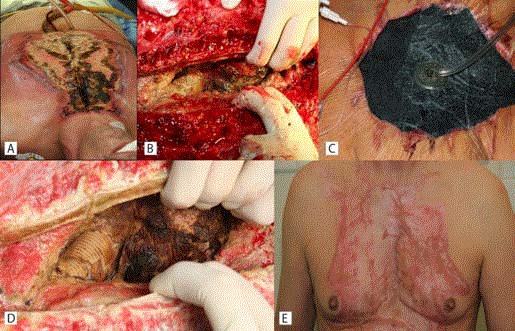
and fulminant phlegmon of the chest wall (Figures A, B). Methicillin-resistant S. epidermidis
(MRSE) was cultured from the wound. The necrotic tissues of the thoracic and mediastinal walls
were surgically removed, and Vacuum Assisted Closure-Negative Pressure Wound Therapy (VAC)
was applied (Figure C). Targeted antibiotic therapy: vancomycin, meropenem, cefepime, amikacin.
VAC dressing was changed every 2 days. One week later, after the mediastinitis subsided, (Figure
D), the sternum was stitched together. After subsequent changes of VAC and resolution of the
inflammation of the integuments, split-thickness skin grafting was performed - one month after the
application of the VAC dressing. The patient was discharged on the 64th day in a generally good
condition, with healed wounds (Figure E).