Research Article
Acute Biliary Pancreatitis - Optimal Time for Cholecystectomy: A Prospective Randomized Study
Mohammed A. Omar1* and Marwa N. Hamed2
1Department of General Surgery, South Valley University, Qena, Egypt
2Department of Anesthesia, Intensive Care and Pain Therapy, South Valley University, Qena, Egypt
*Corresponding author: Mohammed Ahmed Omar, Department of General surgery, South Valley University, Qena, 83523, Egypt
Published: 11 Oct, 2018
Cite this article as: Omar MA, Marwa N. Acute Biliary
Pancreatitis - Optimal Time for
Cholecystectomy: A Prospective
Randomized Study. Clin Surg. 2018; 3:
2151.
Abstract
Background: Cholecystectomy can prevent recurrent attacks of mild Acute Biliary Pancreatitis
(ABP). However, the optimal timing of cholecystectomy remains controversial. The aim of this
prospective randomized study is to compare the outcomes of Early Laparoscopic Cholecystectomy
(ELC) vs. Delayed Laparoscopic Cholecystectomy (DLC) for patients with mild ABP.
Methods: From June 2014 to December 2017, 131 patients with mild ABP were prospectively
randomized to either an ELC group (70 patients) or control DLC group (61 patients). The primary
outcomes were gallstone-related morbidity and mortality while the secondary outcomes were
success and failure rate, the difficulty of cholecystectomy, operative time, cholecystectomy related
complications, readmission for gallstone-related complications, hospital stay, ICU admission
and additional procedure. The study was registered in the ClinicalTrials.gov PRS register with
identification number NCT03085407.
Results: There were statistically significant differences in the incidence and number of readmission
for gallstone-related complications (5.7% vs. 62.35, P<0.001 & 4.3% vs. 21.3%, P<0.001), and the
total length of hospital stay (4.4 ± 1 vs. 6.9 ± 2.6, p=0.03). There were no statistically significant
differences in the other parameters of evaluation between both groups.
Conclusion: In mild ABP, ELC can be done safely and efficaciously with a significant reduction in
the recurrent biliary events, the total length of hospital stay and frequency of readmission compared
with DLC.
Keywords: Acute biliary pancreatitis; Cholecystectomy; Optimal time
Introduction
Acute biliary pancreatitis (ABP) caused by gallstones and biliary sludge [1] is the most important
cause of Acute Pancreatitis (AP), accounting for up to 75% of cases [2-4]. Although most cases of
ABP are mild and self-limiting, a small group (20%) of patients may develop severe pancreatitis,
which is associated with high morbidity and mortality [5,6]. Commonly, after resolution of the
initial attack of APB, patients may experience a recurrent attack (40% to 60%) within 2 weeks or
other gallstone-related complications such as biliary colics, acute cholecystitis, acute cholangitis or
common bile duct (CBD) obstruction [7,8].
Cholecystectomy or endoscopic biliary tree clearance of stones is indicated to reduce the risk of
these recurrent biliary complications [9,10] and failure to provide definitive treatment exposes the
patient to risks of dangerous biliary events [11]. However, there is a clear consensus that patients
who present with ABP should undergo cholecystectomy to prevent further attacks; the optimal
timing of surgery remains controversial [6,12].
There is an acceptance that cholecystectomy is delayed for patients with the severe attack until
local complications as pancreatic necrosis and organ failure have resolved, typically after 6 weeks
[4,10,13-15]. Whereas for patients with mild ABP, the precise moment for a cholecystectomy remains
unclear [6,12]. It is recently recommended that early cholecystectomy should be performed, on the
basis of prevention of the frequent recurrent attacks and readmission with biliary complications
[10,16,17] with evidence that there is no difference in pre-operative morbi-mortality compared to
patients subjected to delayed cholecystectomy [12,17-19].
Still, the actual timing of “early cholecystectomy” is unsettled between the guidelines from the
index hospital admission up to 4 weeks [2,7,8,10]. These variations may be attributed to the lack of
evidence from prospective randomized controlled trials addressing
the timing and safety of this maneuver [20]. Recently and despite
the revised guidelines [9,10], early cholecystectomy during the same
hospital admission is not commonly practiced [18] and the majority
of surgeons prefer interval or delayed cholecystectomy with doubt
regarding the efficacy and safety of early cholecystectomy [21-24]. The
drawback of this strategy increased the risk of recurrent gallstonerelated
complications with repeated admission and higher costs [20].
Endoscopic retrograde cholangiopancreatography (ERCP) with
Endoscopic Sphincterotomy (ES) may be an alternative measure for
reduction of recurrent attacks of ABP but may result in higher rates
of post-procedure complications when compared with Laparoscopic
Cholecystectomy (LC) [25,26]. It can be used as an accepted definitive
treatment in patients who have multiple co-morbidities and are not
fit for surgery [14,15,20]. In this study, we compare the outcomes of
patients with Early Laparoscopic Cholecystectomy (ELC) vs. delayed
laparoscopic cholecystectomy (DLC) for patients with mild acute
biliary pancreatitis.
Patients and Methods
Study design and setting
This is an open-label, prospective randomized controlled study
including all patients have mild ABP who met the inclusion criteria.
The study was performed at Qena and Sohag University hospitals,
Egypt. They are two tertiary centers and serves a population over 10
million people in Upper Egypt, over a period of 3.5 years.
Hypothesis
We hypothesize that ELC (regardless of whether or not
abdominal symptoms were still present and laboratory parameters
had normalized) can be done safely and efficaciously with reduced
recurrent attacks and hospital stay as compared with DLC (after
resolution of abdominal symptoms and normalization of laboratory
parameters) in patients with mild ABP.
Inclusion criteria
The study included all patient diagnosed with (1) the first attack
of mild ABP, (2) onset <72 hrs, (3) age ≥ 18 years, and (4) American
Society of Anesthesiologists (ASA) grade ≤ III. Acute pancreatitis was
diagnosed by the presence of 2 of the 3 following evidence: (1) clinical
evidence of pancreatitis (epigastric pain, acute onset, persistent,
severe, often radiating to the back); (2) biochemical evidence of
pancreatitis (serum amylase or lipase levels at least 3 times the upper
limit of normal); and/or (3) radiographic evidence of pancreatitis
(characteristic findings on contrast-enhanced computed tomography
or magnetic resonance imaging) [27]. Biliary pancreatitis was
diagnosed by (1) imaging confirmation of gallstones, sludge and/or
CBD dilatation; and (2) no alcohol abuse [27]. Mild pancreatitis was
defined by absence of (1) local complications such as peri-pancreatic
fluid collections, acute necrotic collection and/or walled off pancreatic
necrosis; (2) persistent organ failure (>48 hrs); (3) intensive care unit
(ICU) admission; and (4) associated acute cholangitis [27]. The onset
of AP is defined as the time of onset of abdominal pain not the time
of admission to the hospital. The time interval between the onset
and the hospital admission was noted. ICU admission was advised
with aggressive fluid resuscitation requirement or associated acute
cholangitis [6].
Exclusion criteria
Patients were excluded if they have any of the following: (1) severe
or chronic pancreatitis; (2) acute cholangitis; (3) alcohol abuse; (4)
pregnancy; (5) severe medical conditions contraindicating operation;
(6) previous cholecystectomy: or (7) refusal of participation.
Sample size calculation and randomization
The number of patients needed was calculated on the basis of
the reduction of the recurrent biliary event. Considering a power of
80% and reliability of 0.05 to demonstrate, we found that 53 patients
should be present in each group. With an estimated 10% loss to follow
up, 58 patients will have to be included in each group.
The study was started with a target of 211 patients for the
possible loss of patients and data during the study. Eligible patients
(161 patients) were randomly divided immediately after admission
into two equal groups (A & B) according to a computer-generated
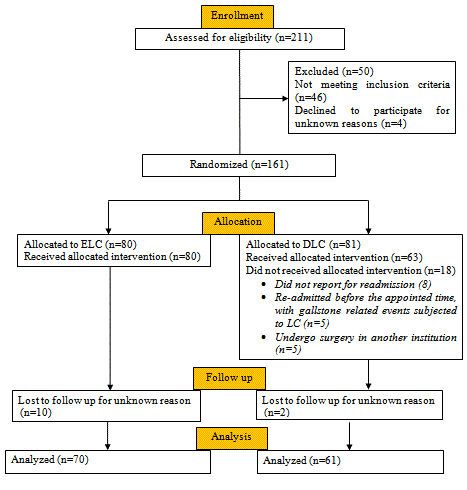
random number and CONSORT guidelines (Figure 1) [28]. Group
(A) received ELC while group (B) received DLC. ELC was defined
as laparoscopic cholecystectomy within 72 hrs after the onset of AP
to allows the diagnosis and organize the operation by surgeons. DLC
was defined as laparoscopic cholecystectomy performed electively
(≥ 6 weeks) after the onset of AP [29]. ES has a protective effect on
the recurrence of biliary pancreatitis and CBD obstruction [30], so
randomization was balanced for ES. This allows for subgroup analysis
with or without ES.
Ethical consideration
The study protocol was approved by the local research ethics
committee of our hospital (No: SVU 148). Also, a written informed
consent was obtained from all patients’ prior recruitment to study.
All patient data were kept privy throughout the study. The study was
registered in the ClinicalTrials.gov PRS register with identification
number NCT03085407.
The procedure
ERCP+ES was done during the first 48 hours of admission in
patients with elevated liver function test and/or imaging confirmation
of biliary dilatation or CBD stones (US, CT, MRI and or MRCP). In
the DLC group, patients were discharged after successful conservative
treatment and scheduled for re-admission and cholecystectomy at the
appointed time (≥ 6 weeks).
All cholecystectomies were done laparoscopically by expert
surgeon. LC was carried out with three ports technique [31]. An
additional fourth port was used when required. All dissections
were performed with the harmonic scalpel. No Intra Operative
Cholangiogram (IOC) was done for any patient of both groups
with the strategy of preoperative endoscopic stone extraction with
excellent and great endoscopic experiences of all participant surgeons.
The abdominal drain was used only in doubtful patients with difficult
dissection.
Postoperatively, all patients were closely monitored in the
inpatient department. They started oral fluid 6 hours after the
operation and subsequently advanced to a regular diet. Patients
were discharged on the second postoperative day if they were able to
tolerate regular diet with no pain with oral medication, and they had
no other indications for continued hospitalization.
Outcomes
The primary endpoint:
Gallstone related morbidity and mortality occurring within 6
months after the onset of ABP, before or after cholecystectomy.
Gallstone related complications include severe biliary colic, recurrent
ABP, acute cholecystitis, and symptomatic choledocholithiasis (acute
cholangitis and/or obstructive jaundice needing ERCP) requiring
readmission [32].
The secondary endpoints:
1. Length of hospital stays of index admission.
2. Patients reporting mild biliary colic treated without
readmission.
3. Success and failure (conversion to open cholecystectomy)
rate of LC.
4. The difficulty of cholecystectomy as measured on a visual
analogue scale (0-10).
5. Operative time.
6. Cholecystectomy related complications (intra-operative
and post-operative).
7. The total length of hospital stays (LOS): (index admission
plus readmission for recurrences and for cholecystectomy).
8. ICU admission (number of patient and total length of stay).
9. Postoperative ERCP.
Follow up
Patients who were discharged after randomization for DLC were
followed up in the outpatient clinic weekly until readmission and
operation at the appointed time with instruction to record all episodes
of biliary colic (i.e., irrespective of readmission). Postoperatively,
patients in both groups were followed up in the outpatient clinic with
a monthly visit over at least 6 months and were stopped follow up if
they remained completely asymptomatic.
Data collection and analysis
Patient data were prospectively collected during hospital
admission for all patients using a case record form. Data entry
was performed using the SPSS software version 16.0 (Chicago, IL,
United States of America). The computer-assisted analysis was
carried out at the end of the study. Results were expressed as means
± standard deviation (SD) or medians with inter-quartile ranges
(IQRs) for continuous variables and Manne Whitney U tests were
performed to assess for significant differences in continuous data
between two groups. Frequencies were presented for categorical
variables and Fischer’s exact test or chi-square tests were used as
appropriate. Statistical significance will be achieved if P-value is less
than 0.05. Subgroup analyses were done based on ES (yes vs. no)
before randomization to assess its potential protective effect on the
occurrence of gallstone-related complications.
Figure 1
Results
A total of 161 patients who had fulfilled the inclusion criteria
of the study from June 2014 to December 2017 were recruited.
The patients were randomized into two equal groups as previously
mentioned (ELC=80, DLC=81). In the ELC group, 10 patients
subsequently withdrawn from the study due to lost to follow up after
the operation. In the DLC group, 20 patients subsequently excluded
due to did not report for re-admission at the appointed time for
operation (8 patients), re-admitted before the appointed time, with
recurrent biliary events (3 patients with obstructive jaundice and 2
patients with ABP) and they all subjected to successful LC during
the re-admission time, undergo surgery in another institution (5
patients), or lost follow up after cholecystectomy (2 patients). The
remaining 131 patients were enrolled in the final analysis of this
study where the ELC group includes 70 patients and the DLC group
includes 61 patients (Figure 1).
Pre-cholecystectomy ERCP/ES was performed for 33 patients in
the ELC group and 28 patients in the DLC group due to CBD stones,
based on laboratory and imaging findings. Stones were found in the
CBD during ERCP in all patients. ES was done a median of 1 day (IQR
1-2 days in ELC group and 1-4 days in DLC group) after the onset
of ABP (Table 1). The only reported post ERCP complication was
minor bleeding in one patient (1.4%) in ELC group A, vs. 2 patients
(3.3%) in DLC group (P=0.89). All cases were successfully treated
with endoscopic technique for achieving hemostasis. There were
no significant differences with respect to age, sex, ASA score, precholecystectomy
ERCP between both groups (Table 1). The median
interval time from onset of ABP to cholecystectomy was statistically
greater among DLC group than among ELC group [56 days (IQR 46-
121 days) vs. 3 days (IQR 3-3 days), respectively, p<0.000] (Table 1).
In the DLC group, 28 (45.9%) underwent LC within 6 to 7 weeks.
Gallstone related complications occurred in 3 patients (4.2%) in
the ELC group, as compared with 11 patients (18.1%) in the DLC group.
In the ELC group, there were no gallstone-related complications in the
short interval between the onset of pancreatitis and cholecystectomy,
and all complications (100%) occurred after the operation with a
median of 50 days (IQR 22-60). In the DLC group, 91% (10 patients)
of gallstone-related complications occurred before LC, with a median
of 41 days (IQR 20-70), and 9% (1 patient) occurred after LC with
a median of 115 days (IQR 70-160). The overall difference between
the two groups was statistically significant (p<0.001) (Table 2). Three
patients readmitted with severe biliary colics (ELC=1, DLC=2), and
treated conservatively. Recurrent biliary pancreatitis occurred in 1
patient (1.4%) in the ELC group, as compared with 5 patients (8.2%)
in the DLC group, 2 patients in the DLC group presented with a
severe pancreatitis with pancreatic necrosis required ICU admission
for a median of 5 days (IQR 4-6). Two patients presented with acute
cholecystitis in the DLC group, with a median of 99 days (IQR 50-
148) and treated successfully with conservative treatment. Three
patients presented with the manifestation of calcular obstructive
jaundice (ELC=1, DLC=2) at a median of (54 & 55 days) and IQR
of (54-54 & 17-93) respectively. They were treated successfully with
ERCP and stone extraction without any post ERCP complications.
No mortality occurred in both groups (Table 2).
In the ELC group, one patient reported postoperative mild biliary
colic, compared with 27 patients in the DLC group (1.4% vs. 44.3%,
p<0.0001). LC was scheduled for all patients in both groups. In ELC
group, it was completed successfully in 68 patients and 2 operations
were converted to open surgery due to severe adhesions and difficult
visualization of Calot’s triangle and uncontrolled bleeding from an
aberrant artery. In DLC group, it was completed successfully in 60
patients and 1 patient was converted to open surgery due to severe
adhesions and difficult dissection of Calot’s triangle. The mean
difficulty of cholecystectomy scale was 5.3 and 4.9 in patients who
underwent ELC and DLC respectively. However it was higher in the
early group, it was statistically insignificant (p=0.74). The operative
time was statistically insignificant (p=0.84) as the mean operative
time was 58.9 ± 18.6 min in the ELC group versus 54 ± 17.6 min in
the DLC group. There was no statistically significant difference in the
cholecystectomy related complication rates between the two groups
(7.1 vs. 5%, p=0.67). There was no difference between the two groups
in the length of index admission (mean of 4.2 days in the early group
and 3.7 days in the delayed group, p=0.21), but the total length of
hospital stay is statistically longer in the DLC group compared with
the ELC group (6.9 ± 2.6 vs. 4.4 ± 1 days; p= 0.01). In DLC group,
the mean of index admission length was 3.7 ± 0.5 days, the mean of
readmissions length due to pre-cholecystectomy gallstone related
events was 1.9 ± 0.4 days, and the mean for cholecystectomy was 2.3
± 0.4 days. There was no difference regarding ICU admission between
both groups. Postoperative ERCP was required for 4 patients in both
groups (ELC=2, DLC=2). In the ELC group, it was done for one
patient with recurrent biliary pancreatitis and another with calcular
obstructive jaundice. In the DLC group, it was done for 2 patients
with calcular obstructive jaundice (Table 3).
In the subgroup analysis, the risk of recurrent biliary events was
reduced in patients who underwent ES before cholecystectomy as
compared to patients who did not undergo ES before cholecystectomy
(p=0.08). The recurrent biliary events occurred in one (3%) patient in
the ELC group, compared with 4 (14.3%) patients in the DLC group.
In the DLC group, one patient developed recurrent ABP, two patients
developed acute cholecystitis, and one was readmitted for severe
biliary colic. One patient in the ELC group was readmitted for severe
biliary colic.
Table 1
Table 2
Table 3
Discussion
This study demonstrates that ELC done within 72 hrs of onset of
mild ABP regardless of normalization of laboratory values or clinical
stabilization, decrease the risk of recurrent biliary complications and
the total LOS compared with DLC after normalization of laboratory
values and clinical condition. In addition, the cholecystectomy
can be done safely and efficaciously with a very low incidence of
cholecystectomy related complications.
The timing of cholecystectomy in patients with ABP remains
a subject of ongoing debate. It is advisable that cholecystectomy is
delayed for patients with severe ABP until local complications have
resolved [12-15]. Regarding mild ABP, The early data recommended
delayed cholecystectomy (6-8 weeks) with the low incidence of
morbidity and mortality [3,33-35]. This was supported by Kelly and
Wagner who showed that early cholecystectomy within 72 hrs will be
associated with difficult dissection and more surgical complications
and conversion to open surgery [36]. Moreover, patients during
this phase can still develop pancreatic necrosis and/or organ failure
which both considered as contraindications for early surgery [36,37].
The recently published studies and guidelines refute this data with
confirmed comparable outcomes of early and delayed LC for patients
with mild ABP. They recommended ELC index admission as the
procedure of choice for patients with mild ABP [5,6,8-17].
Also, the role and timing of ERCP for ABP is a matter of debate.
Moretti et al. [38] showed that early ERCP in patients with severe
ABP is beneficial with decreased pancreatitis related complication
while it has no advantage in patients with mild ABP compared with
conservative management. Bignell et al. [39] showed that ERCP
and ES alone for the patient with ABP will reduce the incidence of
recurrent pancreatitis but they will increase the incidence of gallstonerelated
complications. Chang et al. [40] demonstrated that there was
no difference in pancreatitis related complication rate in patients
with mild ABP underwent ERCP either pre or postoperatively. Early
studies suggested that ERCP with ES alone, can serve as an acceptable
alternative to, and thus can abolish the need for, cholecystectomy
in patients with mild gallstone pancreatitis [41-43]. However, more
recent evidence and guidelines have refuted this suggestion and
conversely recommended early ERCP/ES within 24 hrs to 48 hrs
in patients with mild APB only with clear evidence of CBD stone
or cholangitis followed by ELC as a definitive treatment for these
patients [7,8,10,14,15,44,45].
In our study, we follow the previous international guidelines
recommendations regarding preoperative ERCP [8,10,14,15] with
no significant difference between both groups. Our results showed
that the risk of overall recurrent biliary events was reduced in patients
who underwent ES before cholecystectomy as compared to patients
who did not undergo ES before cholecystectomy (p=0.08). This
finding differs from the results of many studies showed that ES might
mitigate only the risk of recurrent pancreatitis, but it does not affect
the risk of other recurrent complications such as acute cholecystitis,
biliary obstruction and or biliary colic [4,44-47]. Our study revealed a
statistically significant reduction in the recurrent biliary pancreatitis
and biliary obstruction and statistically insignificant difference
regarding recurrent biliary colic and acute cholecystitis between
patients who did and did not undergo ES before cholecystectomy.
Several studies showed that there is a possible risk of gallstonerelated
complications (9%-60%) after index admission for mild ABP
and before delayed cholecystectomy [4,15,17,18,34,41]. This risk is
high (up to 35%) even when the DC will be scheduled within 2 weeks
after the index admission [4,17,18]. Our study revealed statistically
reduced the risk of gallstone-related complications following ELC
as compared with DLC. This was comparable with many studies
[41] and support a shift towards ELC for these patients [48,49].
Recurrent ABP was the only statistically significant one of gallstonerelated
complications between both groups and this was comparable
with Da Costa et al. [47]. Jee et al. [20] showed that although postcholecystectomy
recurrent pancreatitis is very low it can occur as a
result of retained CBD stones or sludge. In the same line, our study
revealed three patients who had post-cholecystectomy recurrent
pancreatitis due to retained CBD stone (ELC=1, DLC=2). Our low
incidence of recurrent biliary events with ELC was reflected on the
low incidence of readmissions and this was comparable with many
studies [6,23,50] concluded that the strategy of early cholecystectomy
results in significant reduction in the number of readmissions. This
is because full treatment will be done during the index admission
for patients scheduled for early cholecystectomy, whereas delayed
cholecystectomy requires two admissions at least, one for initial
conservative treatment of acute pancreatitis and another for delayed
operation. This result will support several previous cost-effectiveness
studies showed that the high cost of ELC was offset by the reduction
gallstone-related complications and readmissions associated with
DLC [51,52].
Our study revealed highly statistically significant difference
between both groups (1.4% vs. 44.3%, p<0.0001) regarding mild
biliary colic which was treated without readmission. This was
comparable with Da Costa et al. [47] who showed the same high
statistically significant difference (3% vs. 51%, p<0.0001).
The success and failure rate showed no statistically significant
differences between both groups with a comparable result to other
series [6,47,53]. On the contrary, several studies showed a higher
conversion rate with ELC. Jee et al. [20] showed a conversion rate
of (10.53% vs. 11.76%; p=1.000), and he attributed these higher
incidences to the chronicity of cholecystitis with high frequency of
adhesions in their population, while Tang et al. too, showed a higher
conversion rate of 67% with ELC and 18% with DLC [53].
The old concept of delayed cholecystectomy was based on the
concept of difficult intervention during the acute stage with difficult
anatomical assessment and dangerous dissection [33,36]. However,
our result was exactly the opposite. There was no statistically
significant difference regarding the difficulty of cholecystectomy
in both groups. And this result was comparable with the recently
published studies [47,54]. Interestingly in contrast to this old concept,
recently a number of studies concluded that delayed cholecystectomy
was significantly more difficult than early cholecystectomy. They
have suggested that soft fibrinous omental adhesions during the acute
stage will allow easy dissection and easier cholecystectomy. On the
contrary, fibrous dense adhesions during the late stage will make the
dissection more difficult with complicated cholecystectomy [54,55].
Our study revealed nearly equal operative time (58.9 vs. 54 mins)
between both groups and this was consistent with literature that
demonstrated no significant difference regarding operative time in
patients who underwent EC and DC [20,49,50,54]. Also, Our study
demonstrated no significant difference regarding cholecystectomy
related complications between both groups and this rate was
comparable to that reported in the literature [6,12,20,54]. The low
incidence of these complications supports the accepted hypothesis of
safety and efficacy of early cholecystectomy after mild ABP [13,47].
Also, this hypothesis is confirmed by previous equal results of surgical
difficulty obtained between both groups [47,54].
Although, our study demonstrated no significant difference
regarding the length of index admission between both groups;
the strategy of early cholecystectomy with a reduced number of
readmission was reflected a statistically insignificant reduction in the
total length of hospital stay in ELC group compared with DLC group.
Similar conclusions have been shown in a number of other studies
[6,12,23,55,56].
Conclusion
In conclusion, ELC during the index admission for patients with mild ABP can be done safely and efficaciously with reduced recurrent biliary events and its subsequent total length of hospital stay and frequency of readmission compared with DLC. In addition, there is no difference in the success and failure rate, difficulty of cholecystectomy, operative time, or complication rate between early or delayed LC. Furthermore, it prevents disabling colics that occurred within about half of those patients awaiting DLC. Therefore, we recommend ELC in patients with mild ABP and although we know the difficulty to change the behavior of many surgeons we hope our results to be a point of attraction and persuasion in favor of early surgery.
References
- Yadav D, Lowenfels AB. The epidemiology of pancreatitis and pancreatic cancer. Gastroenterology. 2013;144(6):1252-61.
- Uhl W, Warshaw A, Imrie C, Bassi C, McKay CJ, Lankisch PG, et al. IAP Guidelines for the Surgical Management of Acute Pancreatitis. Pancreatology. 2002;2(6):565-73.
- Taylor E, Wong C. The optimal timing of laparoscopic cholecystectomy in mild gallstone pancreatitis. Am Surg. 2004;70(11):971-5.
- Ito K, Ito H, Whang EE. Timing of cholecystectomy for biliary pancreatitis: do the data support current guidelines? J Gastrointest Surg. 2008;12(12):2164-70.
- Banks PA, Freeman ML; Practice Parameters Committee of the American College of Gastroenterology. Practice guidelines in acute pancreatitis. Am J Gastroenterol. 2006;101(10):2379-400.
- Aboulian A, Chan T, Yaghoubian A, Kaji AH, Putnam B, Neville A, et al. Early cholecystectomy safely decreases hospital stay in patients with mild gallstone pancreatitis: a randomized prospective study. Ann Surg. 2010;251(4):615-9.
- Forsmark CE, Baillie J; AGA Institute Clinical Practice and Economics Committee; AGA Institute Governing Board. AGA Institute technical review on acute pancreatitis. Gastroenterology. 2007;132(5):2022-44.
- Working Party of the British Society of Gastroenterology; Association of Surgeons of Great Britain and Ireland; Pancreatic Society of Great Britain and Ireland; Association of Upper GI Surgeons of Great Britain and Ireland. UK guidelines for the management of acute pancreatitis. Gut. 2005;54 Suppl 3:iii1-9.
- Working Group IAP/APA Acute Pancreatitis Guidelines. IAP/APA evidence-based guidelines for the management of acute pancreatitis. Pancreatology. 2013;13(4 Suppl 2):e1-15.
- Tenner S, Baillie J, Dewitt J, Vege SS. American College of Gastroenterology Guidelines: management of acute pancreatitis. Am J Gastroenterol. 2013;108:1400-15.
- Gullo L, Migliori M, Pezzilli R, Oláh A, Farkas G, Levy P, et al. An update on recurrent acute pancreatitis: data from five European countries. Am J Gastroenterol. 2002;97(8):1959-62.
- Perez LJR, Parra JF, Dimas GA. The safety of early laparoscopic cholecystectomy (<48 hours) for patients with mild gallstone pancreatitis: a systematic review of the literature and meta-analysis. Cir Esp. 2014;92(2):107-13.
- Nealon WH, Bawduniak J, Walser EM. Appropriate timing of cholecystectomy in patients who present with moderate to severe gallstone-associated acute pancreatitis with peripancreatic fluid collections. Ann Surg. 2004;239(6):741-9.
- Greenberg JA, Hsu J, Bawazeer M, Marshall J, Friedrich JO, Nathens A, et al. Clinical practice guideline: management of acute pancreatitis. Can J Surg. 2016;59(2):128-40.
- Crockett SD, Wani S, Gardner TB, Falck-Ytter Y, Barkun AN. American Gastroenterological Association Institute Guideline on Initial Management of Acute Pancreatitis. Gastroenterology. 2018;154(4):1096-101.
- Wilson CT, De Moya MA. Cholecystectomy for acute gallstone pancreatitis: early vs delayed approach. Scand J Surg. 2010;99(2):81-5.
- Van Baal MC, Besselink MG, Bakker OJ, Van Santvoort HC, Schaapherder AF, Nieuwenhuijs VB, et al. Timing of cholecystectomy after mild biliary pancreatitis: a systematic review. Ann Surg. 2012;255(5):860-6.
- Nguyen GC, Rosenberg M, Chong RY, Chong CA. Early cholecystectomy and ERCP are associated with reduced readmissions for acute biliary pancreatitis: a nationwide, population-based study. Gastrointest Endosc. 2012;75:47-55.
- Bakker OJ, Van Santvoort HC, Hagenaars JC, Besselink MG, Bollen TL, Gooszen HG, et al. Timing of cholecystectomy after mild biliary pancreatitis. Br J Surg. 2011;98(10):1446-54.
- Jee SL, Jarmin R, Lim KF, Raman K. Outcomes of early versus delayed cholecystectomy in patients with mild to moderate acute biliary pancreatitis: A randomized prospective study. Asian J Surg. 2018;41:47-54.
- Lankisch PG, Weber-Dany B, Lerch MM. Clinical perspectives in pancreatology: compliance with acute pancreatitis guidelines in Germany. Pancreatology. 2005;5(6):591-3.
- Pezzilli R, Uomo G, Gabbrielli A, Zerbi A, Frulloni L, De Rai P, et al. A prospective multicentre survey on the treatment of acute pancreatitis in Italy. Dig Liver Dis. 2007;39(9):838-46.
- Monkhouse SJ, Court EL, Dash I, Coombs NJ. Two-week target for laparoscopic cholecystectomy following gallstone pancreatitis is achievable and cost neutral. Br J Surg. 2009;96(7):751-5.
- Nguyen GC, Boudreau H, Jagannath SB. Hospital volume as a predictor for undergoing cholecystectomy after admission for acute biliary pancreatitis. Pancreas. 2010;39:e42-7.
- Sees DW, Martin RR. Comparison of preoperative endoscopic retrograde cholangiopancreatography and laparoscopic cholecystectomy with operative management of gallstone pancreatitis. Am J Surg. 1997;174(6):719-22.
- Kaw M, Al-Antably Y, Kaw P. Management of gallstone pancreatitis: cholecystectomy or ERCP and endoscopic sphincterotomy. Gastrointest Endosc. 2002;56(1):61-5.
- Banks PA, Bollen TL, Dervenis C, Gooszen HG, Johnson CD, Sarr MG, et al. Classification of acute pancreatitis - 2012: Revision of the Atlanta classification and definitions by international consensus. Gut. 2013;62:102-11.
- Schulz KF, Altman DG, Moher D. CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. BMJ. 2010;340:c332.
- Gurusamy KS, Nagendran M, Davidson BR. Early versus delayed laparoscopic cholecystectomy for acute gallstone pancreatitis. Cochrane Database Syst Rev. 2013;9:CD010326.
- Van Geenen EJ, Van der Peet DL, Mulder CJ, Cuesta MA, Bruno MJ. Recurrent acute biliary pancreatitis: the protective role of cholecystectomy and endoscopic sphincterotomy. Surg Endosc. 2009;23(5):950-6.
- Omar MA, Redwan AA, Mahmoud AG. Single-incision versus 3-port laparoscopic cholecystectomy in symptomatic gallstones: A prospective randomized study. Surgery. 2017;162(1):96-103.
- Mayumi T, Takada T, Kawarada Y, Nimura Y, Yoshida M, Sekimoto M, et al. Results of the Tokyo Consensus Meeting Tokyo Guidelines. J Hepatobiliary Pancreat Surg. 2007;14:114-21.
- Ranson JH. The timing of biliary surgery in acute pancreatitis. Ann Surg. 1979;189(5):654-63.
- Osborne DH, Imrie CW, Carter DC. Biliary surgery in the same admission for gallstone-associated acute pancreatitis. Br J Surg. 1981;68(11):758-61.
- Horward JM, Ehrlich EW. Gallstone pancreatitis: A clinical entity. Surgery. 1962;51(2):177-84.
- Kelly TR, Wagner DS. Gallstone pancreatitis: a prospective randomized trial of the timing of surgery. Surgery. 1988;104(4):600-5.
- Mofidi R, Duff MD, Wigmore SJ, Madhavan KK, Garden OJ, Parks RW. Association between early systemic inflammatory response, severity of multiorgan dysfunction and death in acute pancreatitis. Br J Surg. 2006;93(6):738-44.
- Moretti A, Papi C, Aratari A, Festa V, Tanga M, Koch M, et al. Is early endoscopic retrograde cholangiopancreatography useful in the management of acute biliary pancreatitis? A meta-analysis of randomized controlled trials. Dig Liver Dis. 2008;40(5):379-85.
- Bignell M, Dearing M, Hindmarsh A, Rhodes M. ERCP and endoscopic sphincterotomy (ES): a safe and definitive management of gallstone pancreatitis with the gallbladder left in situ. J Gastrointest Surg. 2011;15(12):2205-10.
- Chang L, Lo S, Stabile BE, Lewis RJ, Toosie K, de Virgilio C. Preoperative versus postoperative endoscopic retrograde cholangiopancreatography in mild to moderate gallstone pancreatitis: a prospective randomized trial. Ann Surg. 2000;231:82-7.
- Siegel JH, Veerappan A, Cohen SA, Kasmin FE. Endoscopic sphincterotomy for biliary pancreatitis: an alternative to cholecystectomy in high-risk patients. Gastrointest Endosc. 1994;40(5):573-5.
- Welbourn CR, Beckly DE, Eyre-Brook IA. Endoscopic sphincterotomy without cholecystectomy for gall stone pancreatitis. Gut. 1995;37:119-20.
- Cotton PB, Geenen JE, Sherman S, Cunningham JT, Howell DA, Carr-Locke DL, et al. Endoscopic sphincterotomy for stones by experts is safe, even in younger patients with normal ducts. Ann Surg. 1998;227(2):201-4.
- Sandzen B, Haapamaki MM, Nilsson E, Stenlund HC, Oman M. Cholecystectomy and sphincterotomy in patients with mild acute biliary pancreatitis in Sweden 1988-2003: a nationwide register study. BMC Gastroenterol. 2009;9:80.
- Mador BD, Panton ON, Hameed SM. Early versus delayed cholecystectomy following endoscopic sphincterotomy for mild biliary pancreatitis. Surg Endosc. 2014;28(12):3337-42.
- Hwang SS, Li BH, Haigh PI. Gallstone pancreatitis without cholecystectomy. JAMA Surg. 2013;148(9):867-72.
- Da Costa DW, Bouwense SA, Schepers NJ, Besselink MG, Van Santvoort HC, Van Brunschot S, et al. Same-admission versus interval cholecystectomy for mild gallstone pancreatitis (PONCHO): a multicentre randomised controlled trial. Lancet. 2015;386(10000):1261-8.
- El-Dhuwaib Y, Deakin M, David GG, Durkin D, Corless DJ, Slavin JP. Definitive management of gallstone pancreatitis in England. Ann R Coll Surg Engl. 2012;94(6):402-6.
- Kamal A, Akhuemonkhan E, Akshintala VS, Singh VK, Kalloo AN, Hutfless SM. Effectiveness of Guideline Recommended Cholecystectomy to Prevent Recurrent Pancreatitis. Am J Gastroenterol. 2017;112(3):503-10.
- Al-Qahtani HH. Early versus interval cholecystectomy after mild acute gallstone pancreatitis: A 10 year experience in central Saudi Arabia. J Taibah Univ Med Sci. 2014;9(4):322-7.
- Morris S, Gurusamy KS, Patel N, Davidson BR. Cost-effectiveness of early laparoscopic cholecystectomy for mild acute gallstone pancreatitis. Br J Surg. 2014;101(7):828-35.
- Murphy PB, Paskar D, Hilsden R, Koichopolos J, Mele TS; Western Ontario Research Collaborative on Acute Care Surgery. Acute care surgery: a means for providing cost-effective, quality care for gallstone pancreatitis. World J Emerg Surg. 2017;12:20.
- Werner J, Feuerbach S, Uhl W, Büchler MW. Management of acute pancreatitis: from surgery to interventional intensive care. Gut. 2005;54(3):426-36.
- Sinha R. Early laparoscopic cholecystectomy in acute biliary pancreatitis: the optimal choice? HPB Surg. 2008;10(5):332-5.
- Sanjay M, Kapil S, Mahavir J, Jangvir S, Prakash GS, Pal SV. Comparative Evaluation of Early Laparoscopic Cholecystectomy for Mild Gallstone Pancreatitis vs Acute Cholecystitis. Hellenic J Surg. 2017;89:4-12.
- Rosing DK, De Virgilio C, Yaghoubian A, Putnam BA, El Masry M, Kaji A, et al. Early cholecystectomy for mild to moderate gallstone pancreatitis shortens hospital stay. J Am Coll Surg. 2007;205(6):762-6.