Case Report
Isolated Fourth Ventricle Causes a Mass Effect in the Posterior Fossa. Difficulties of Making a Diagnosis in the Intensive Care Unit in Comatose Patients: Clinical Overview
Jarosław Andrychowski1,2*, Lidia Glinka3, Nastazja Karakina3 and Dagmara Szymkowicz-Kudełko4
1Department of Neurology, Neurological Rehabilitation and Kinesytherapy, The Institute of Physiotherapy, The Faculty of Medicine and Health Sciences, University Jan Kochanowski, Kielce, Poland
2Department of Neurotraumatology, Medical University of Warsaw, Poland
3Department of Anesthesiology and Intensive Care, University of Warmia and Mazury in Olsztyn, Poland
4Department of Neurosurgery, The Children's Memorial Health Institute, Warsaw, Poland
*Corresponding author: Jarosław Andrychowski, Department of Neurology, Neurological Rehabilitation and Kinesytherapy, The Institute of Physiotherapy, The Faculty of Medicine and Health Sciences, University Jan Kochanowski, Kielce, Poland
Published: 10 Oct, 2018
Cite this article as: Andrychowski J, Glinka L, Karakina N,
Szymkowicz-Kudełko D. Isolated Fourth
Ventricle Causes a Mass Effect in the
Posterior Fossa. Difficulties of Making a
Diagnosis in the Intensive Care Unit in
Comatose Patients: Clinical Overview.
Clin Surg. 2018; 3: 2148.
Abstract
Isolated fourth ventricle (IFV) is a rare radiological and clinical complication of the surgical
treatment within the cerebral fluid pathways. It may occur as a result of a neurosurgical procedure
when post resection space communicates with the fourth ventricle, be a complication of shunt
therapy, external drainage or endoscopy of the ventricular system. Neuroinfection or subarachnoid
hemorrhage can predispose to the development of the syndrome. The pathomechanism is associated
with disturbances in the patency of the Sylvian aqueduct and the outflow routes from the fourth
ventricle. An important role in pathology is attributed to the vascular plexus of the fourth ventricle
and its physiological secretion of cerebrospinal fluid. The resulting IFV reservoir causes a mass effect
in the posterior fossa and the development of compression symptoms in the brainstem. Imaging
tests reveal the signs of retention of the cerebrospinal fluid (CSF) inside the surrounding white
matter of the posterior fossa. This causes deterioration of the clinical state which is dependent on the
compression on the brainstem. At the same time, the supratentorial space of the brain is effectively
treated with ventricular drainage or using a shunt. Previous publications mainly concentrated on
pediatric patients. In adult patients, IFV is a rare complication that develops few months after
the first surgical procedure. The mass effect increases consciousness disorders and brainstem
symptoms. We present the diagnosis of IFV in a patient who was unconscious and subjected to
long-term hospitalization in the ICU. We pointed out the importance of a detailed examination
of brainstem symptoms and the necessity to perform the sequence of MRI images with the cine
option after specific neurosurgical procedures. Some neurosurgical procedures may predispose to
the development of IFV.
Keywords: Fourth ventricle; Posterior fossa; Isolated ventricle; Complication; Ventriculostomy; Shunt therapy; Intensive care unit
Introduction
Isolated fourth ventricle (IFV) is a rare complication of neurosurgical treatment. It may occur
after surgical procedures performed within the posterior fossa, after implantation and replacement
of valves, external drainage of the supratentorial ventricular system and endoscopic ventriculostomy
of the third ventricle. IFV may be caused by the mechanical or functional obstruction of the reversed
flow within the Sylvian aqueduct and obstacles of outflow from the fourth ventricle through the
anatomical foramina of Luschka and Magendi. Cerebrospinal fluid (CSF) is produced in the choroid
plexus of the lateral ventricles and third ventricle; according to the views of some clinicians the
production of CSF in the fourth ventricle is small and does not play any role.
According to our observations and literature reports, the production of CSF by the plexus of
the fourth ventricle plays specific role especially for the different pathology in this region. The lack
of communication with the supratentorial and infratentorial CSF spaces causes clinical symptoms,
such as radiological "isolation" of the fourth ventricle (IFV) and the mass effect in the posterior
fossa. Extension of the fourth ventricle dimensions after posterior
fossa surgical procedures, which was described in literature, has
even gained the term "postoperative Dandy - Walker syndrome" or
"trapped fourth ventricle".
The production of CSF by the vascular plexus causes enlargement
of the dimensions fourth ventricle, local mass effect, dislocation of the
posterior fossa structures towards the rostral and caudal direction,
compression and failure of the brainstem, cranial nerve dysfunction
and the symptoms of cerebellar syndrome.
The imaging studies revealed the areas of sub-ependymal leakage
into the white matter similar to PVL around the enlarged fourth
ventricle. The rarity of the syndrome (IFV) in adults may cause
difficulties in the adequate interpretation of post-operative imaging
examinations. We believe that the publication is a good training
resource for all colleagues who assess patients after operations within
the fluid space of the brain.
The routine imaging evaluation of the effectiveness of treatment
in patients after drainage and ventricular shunts is carried out on
the basis of the morphology of the lateral ventricles and the third
ventricle; the assessment estimates the effectiveness of eliminating
supratentorial mass effect. The radiological features of the fourth
ventricle enlargement do not always raise a suspicion of IFV. We
pointed out that the majority of literature publications relates to the
topic of IFV pediatric patients, mainly after complicated ventricularperitoneal
valve implantations. A characteristic feature of IFV is
that development of symptoms takes place long time after the first
operating procedure performed within the fluid system. The course
of the condition in adults is the same; the publications concern
outpatient observation of patients after the ventriculo-peritoneal
shunts and are very scarce. Our study presents a unique situation
when the syndrome of symptomatic mass effect caused by IFV
occurred delayed after the first surgical procedure developed in the
unconscious patient.
A female patient after the operation of the posterior fossa was
treated for a long time in the ICU, initially by implantation of shunt
into lateral ventricle. After the complications and shunt removal
the external ventricular drainage was implanted. The neurological
examination revealed the weak reactivity of brain stem and the
appearance of the symptoms cranial nerves dysfunction. This
examination prompted us to perform control radiological assessment
and adequate diagnosis of deterioration.
Figure 1
Figure 1
The cystic form with the CSF in the posterior fossa located in the
midline with a mass effect and hypodense zones around the fourth ventricle.
Figure 2A and 2B
Figure 2A and 2B
Lack of the flow in the Sylvian aqueduct was observed
in the systolic and diastolic phase both at the speed of 8 cm/s and 15 cm/s.
Case Presentation
A 47-year-old patient (A.N) admitted to the ICU was treated
surgically due to cavernous angioma of the vermis. Due to obstructive
hydrocephalus diagnosed in the postoperative course first external
drainage and then ventriculo-peritoneal shunt system was implanted.
Unfortunately, the infection of central nervous system was observed.
The culture revealed the presence of Staph epidermidis MRCNS. The
valve system was removed; external ventricular drainage was applied
along with targeted antibiotic therapy. After recovery, the valve
system was re-implanted. Unfortunately, inserted shunt led in CT to
the asymmetrical dilation of the lateral ventricle on the side opposite
to the introduced valve drain due to the impeded communication on
the level of Monroe foramen. Deterioration of the clinical condition
and the impairment of consciousness assessed at 5 GCS points created
the need to apply external drainage of the asymmetrically enlarged
lateral ventricle and replacement of the shunt with external drainage.
Then, one of the drains was removed and endoscopic septostomy and
third ventriculostomy were performed. The post-operative CT scan
revealed that the ventricular system was temporarily symmetrically
narrowed. The patient was introduced into analgosedation and
transferred to the Intensive Care Unit. However, after discontinuation
of the analgosedative medication, the patient's condition did not
improve, consciousness was assessed at 5 GCS points, clinically,
respiratory insufficiency was reported, and artificial ventilation was
continued using a ventilator.
The diagnostic and therapeutic period lasted a total of 3 months
of hospital stay in the Department of Neurosurgery and Intensive
Care Unit (ICU) counting from the moment of surgery on cavernous
angioma. During this time, the ventriculo-peritoneal shunt was
implanted and removed, the first neuroinfection was treated. Then,
both implantation and removal of the shunt were repeated, and
another external drainage was established followed by endoscopy
procedure. Second neuroinfection was cured.
Despite intensive treatment the patient's condition did not
improve. Because of respiratory failure the patient was connected to
the ventilator. Ventricular drainage worked properly. The values of
intracranial pressure monitored continuously in the drain were in
the range from 2 mmHg to 12 mmHg. The neurological examination
performed prior to the administration of analgosedation revealed that
the pupils were equal (4 mm in a diameter) with a slow reaction to the
light, circulatory instability manifested as tachycardia alternating into
bradycardia. The examination of the state of consciousness showed
the reaction of flexion of the left upper limb after pain stimulus. The
analgosedation was stopped after 3 days and the neurological condition
was reassessed. External drainage worked properly maintaining the
pressure in the normal range. There was no improvement of the
clinical condition, the patient was still unconscious, and the pupils
were dilated with the slow reaction to the light and inefficient breath.
Reactions to pain stimulus as before. Because of the deterioration
of brainstem reactivity, an imaging examination was ordered. The
computed tomography showed efficiency of lateral ventricular
drainage, narrowing of the supratentorial dimensions of the
ventricular system. The consulting neurosurgeon noted the cystic
form with the CSF in the posterior fossa located in the midline
with a mass effect and hypodense zones around the fourth ventricle
(Figure 1). A suspicion was made of either the presence of pseudocystic
enlargement of the site after the removed cavernous angioma
of the vermis or disturbance of cerebrospinal fluid outflow from the
fourth brain ventricle. The next MRI examination performed with the
cine option revealed the enlarged fourth ventricle and lack of outflow
from this structure. The occlusion of Sylvian aqueduct and isolated
fourth ventricle (IFV) were detected. No flow in the Sylvian aqueduct
was observed in the systolic and diastolic phase both at the speed of 8
cm/s and 15 cm/s (Figure 2a and 2b).
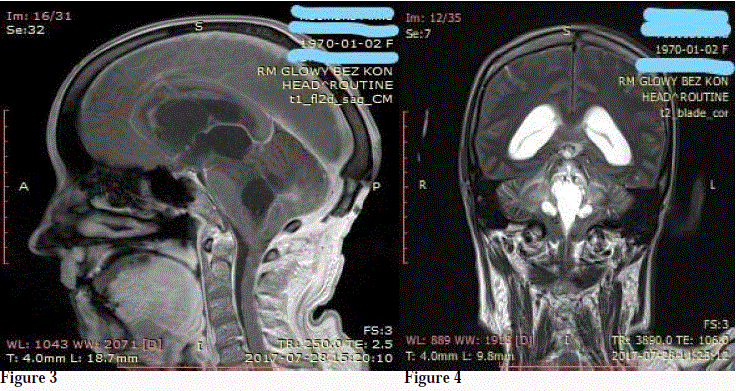
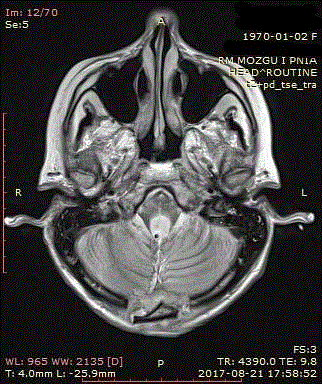
Additionally, Periventricular Lucency (PVL) around the fourth
ventricle and atrophy of the cerebellar vermis were observed. The
MRI examination showed the displacement and tonsillar herniation
(Figure 3 and 4). The presence of mass effect, compression on
the brainstem resulted in a decision to perform suboccipital
decompression and making the connection between the IFV and the
subarachnoid space. The patient was operated in a lying position. After
craniectomy and posterior arch of atlas removing, dura was opened
and the tightly adhering cerebellar tonsills were microsurgically
separated. During this maneuver lack of free outflow of CSF from
Magendie was noticed. The medial foramen was obstacled and due
to the lower medullary velum was cut to improve the outflow. Postinflammatory
changes were observed within the fourth ventricle
lining as an additional membrane blocking the communication
with subarachnoid space. An incision was made in the midline at
the distance of 7 mm long within the Magendi foramen, the lower
medullary velum and the post-inflammatory membrane. The CSF
flowed out under the elevated pressure, the hemispheres of the
cerebellum clearly diminished their volume, they "collapsed" and
began to pulse. The incision was made at a length of 7 mm to avoid
of spontaneous closure caused by arachnoidal adhesions. A soft,
perforated drain was also inserted through the cut line into the
fourth ventricle to a depth of 8 mm, was placed and fixed followed by
suturing to the arachnoid membrane around the Magendi foramen.
The total length of the drain was 15 mm. The distal end of the drain
was placed within the anatomical cerebellomedulary cistern. The free
outflow of CSF via the IFV-ventriculostomy and through drain was
observed. The wound was tightly stitched. The operative procedure
was uneventful and patient was transported to the Intensive Care Unit.
The next day after stopping the analgosedation, pupils reactivity i.e.
light reflexes was improved and reactivity of pain stimulus reported
as intensification of the facial response (facial grimace), which has not
been observed so far. The control MRI performed on the following
day revealed the correct position of the drain in the lumen of fourth
ventricle (Figure 5) and decompression of anatomical structures of
the posterior fossa. External drainage of the lateral ventricle was left.
It could not be internalized due to the high levels of protein in the
cerebrospinal fluid. The ICP in the range of 4 mmHg to 10 mmHg was
measured. In the following days, the examination of CSF taken from
the lateral ventricle revealed the next neuroinfection - S. epidermidis
MRCNS, therefore, targeted antibiotic therapy was implemented.
Unfortunately, suddenly the clinical condition significantly
deteriorated and the patient died due to cardiorespiratory failure.
Figure 3 and 4
Figure 5
Figure 5
The control MRI performed on the following day revealed the correct
position of the drain in the lumen of fourth ventricle and decompression of
anatomical structures of the posterior fossa.
Discussion
Certain types of neurosurgical operations within the cerebral
fluid pathways may predispose to the development of Isolated fourth
ventricle (IFV). This applies to the operation of ventriculo peritoneal
shunt implantation, revision and removal of shunt to infectious
complications. Especially it was observed in pediatric patients. The
use of time extended external ventricular drainage and the surgical
procedure performed within the structures of the posterior fossa
predispose to IFV as well. The postoperative condition complicated
by neuroinfection, formation of arachnoid adhesions within
subarachnoid spaces and post-inflammatory obstruction of the
Sylvian aqueduct can play important role [1-7]. There are reports of
the possible development of IFV after endoscopic ventriculostomy of
the third ventricle too. Reversal flow in Sylvian aqueduct seems the
reason of IFV formation [8].
IFV or "trapped" fourth ventricle encountered in pediatric
neurosurgery can be a serious consequence of intracranial hemorrhage,
infection or post-inflammatory central nervous system complication.
The development of IFV may also occur after properly performed
ventricular -peritoneal shunt implantation. It is characteristic feature
of IFV that the clinical and radiological symptoms can appear in the
course properly shunting and draining supratentorial ventricles few
months after the effective treatment. The development of radiographic
and clinical features of IFV responsible for the mass effect in the
posterior fossa and the symptoms of brainstem compression were
observed after several months. The set of symptoms does not occur
immediately after the surgical procedure [1-8]. IFV was described for
the first time by Dandy [9].
The previous publications about adult patients with radiological
feature and symptomatic IFV were very scarce and concerning
outpatient clinic after ventricular shunt. Our publication presents
the very rare case of IVF feature developed during long lasting in
meaning several months hospital stay.
The treatment of patient after surgery in posterior fossa and shunt
therapy was complicated by infection and finally admitted to ICU. The
patient was in a severe clinical condition during the stay in ICU. The
insight clinical examination was difficult due to deep unconsciousness
and brainstem dysfunction. We observed the increasing of brainstem
dysfunction and the lack of improvement clinical status during
hospitalization. Our suspicion of deterioration was related to the
possibly direct compression of the brainstem in the IFV mechanism.
Therefore, we decided to extend the scope of diagnostic imaging. In
our opinion, this was unique in this publication to perform the Cine
Sequence MRI to confirm the lack of CSF flow through the Sylvian
aqueduct in the systolic and diastolic phase of examination. This
observation revealed the important factor of the IFV pathogenesis.
It should be emphasized that in unconscious patients the lack of
improvement or deterioration after above mentioned surgical
procedures can be caused by IFV. Therefore, so it is very important to
carefully observe brainstem symptoms.
During the debate about the pathophysiology of CSF in the context
of IFV is present a view about low significance of vascular plexus in
fourth ventricle for the production of CSF. In our opinion, this is a
myth, especially when radiologically and clinically IFV is developed.
In certain situations, the secretory activity of the plexus leads to the
features of mass effect in the posterior fossa. The vascular plexus of
the fourth ventricle has rich vascularization and is supplied by AICA
to lower and lateral segment and PICA to the medial segment [10].
In our opinion, it is important the knowledge of the operational
anatomy of this area because this may prevent from the formation
of postoperative CSF reservoirs connected with the fourth ventricle,
causing Pseudo Dandy-Walker syndrome. This was described in the
60’s of the last century [6,7].
Some neurosurgeons, who did not face the problem of IFV due to
the rarity of the syndrome, can believe that the production of CSF in
the fourth ventricle is not relevant. The literature and clinical practice
provide the information that consultants performing control CT scan
after ventricular shunt therapy pay attention mainly to the assessment
of supratentorial space. They analyze the efficiency of draining the
ventricular system by evaluating only the dimensions of the lateral
ventricles and the third ventricle, and ignoring the presence of IFV
development. In this way they can ignore the possibility of fourth
ventricle enlargement and incorrectly evaluate the neurological
symptoms from posterior fossa and brain stem. The isolated fourth
ventricle can be incorrectly interpreted as a site after the surgery in
the area of the posterior fossa too. We recommend that different
consultants should pay attention to this in their work, especially when
they base only on descriptions of radiological imaging. Sometimes,
before a neurosurgeon final decision, the cumulative symptoms of
IFV are incorrectly interpreted as post-traumatic syndrome or toxic
effect of drugs [4,11,12]. Symptoms of brain stem compression and
mass effect of the posterior fossa caused by IFV requires surgical
treatment. In adults, this pathology is very scarce, but treatment
strategies developed for pediatric patients can also be used in adults
[13,15-19].
The discussion on the IFV treatment referring to microsurgical
restoring patency to the outflow routes from the fourth ventricle
[13,14] or endoscopic fenestration of IFV, surgery of the Sylvian
aqueduct aqueductoplasty, introduction of the stent into the aqueduct
or drainage IFV peritoneal shunt. Due to the high risk of complications,
surgical techniques are still improved. Actually in the management
most often is used the IFV peritoneal shunt and aqueductoplasty of
Sylvian aqueduct with a stent [20-23]. The aqueductoplasty without
stenting may cause re-occlusion or obliteration [24], additionally
navigated endoscopy techniques guarantee the precision of stenting
[16,25].
I our clinical situation due to serious symptoms of mass effect in
posterior fossa, we decided to perform suboccipital decompression
and microsurgical patency restoring to the outflow routes from the
fourth ventricle and create the connection between IFV and fluid
spaces. The aim of our decision was to decompress the brainstem
following radiologically diagnosed brain herniation and directly
eliminate the cause of IFV. In this condition the method of IFV
peritoneal shunt, should rule out. On the other hand the high level of
protein in CSF can disturb the patency of drainage and can irritate the
peritoneum additionally.
During the operation I decided to leave a small fragment of the
drain inserted into the IFV lumen. I stitched it with the arachnoid
membrane to avoid the dislocation. I measured the length of drain
to avoid symptomatic irritation of the bottom of the fourth ventricle.
The management to establish IFV peritoneal shunt has the risk of
complications, such as over drainage, occlusion of the shunt, infection,
mechanical irritation of the brainstem (fourth ventricle floor) and the
symptoms of cranial nerve and brainstem dysfunctions.
The aqueductoplasty maneuvers are associated with complications,
such as post-inflammatory or post-infection occlusion and may
require revision. The cranial nerves alterations observed after IFV
peritoneal shunt are evoked by direct irritation of the floor of fourth
ventricle by the tip of inserted drain and as a result of brainstem
dislocation and require revision [11,15,26,27]. The above mentioned
mechanism of cranial nerve dysfunctions and brain stem alteration
may also result of the overdrainage due to siphon effect of the inserted
shunt in the both situation supratentorial ventricle-peritonal and IFV
peritoneal as well. This phenomenon can provoke to collapse of the
Sylvian aqueduct walls as well and deformation of the brainstem due
to changes of the pressure [26-29].
The pathomechanism of the obstacle for reverse flow of CSF
through the Sylvian aqueduct from the fourth to third ventricle
followed the lateral ventricle-peritoneal shunt can refer the suction
mechanism and is associated with CSF flow disturbances on the level
of the cisterna ambiens and the upward herniation of the vermis of
the cerebellum into the tentorium edges. The observed mechanism
of positive feedback causes that the increasing IFV volume creates
additional compression around the Sylvian aqueduct followed by
herniation into the tentorium edges. The difficulties of CSF outflow
from IFV via anatomical foramina causes that the expanding
dimensions fourth ventricle creates the mass effect leading to "upward
herniation" and collapse Sylvian aqueduct followed compression and
dislocation of anatomical structure within tentorial edges.
The functional mechanism of the IFV development due to
the pulsating wave is described in the literature. According to the
dynamic theory of CSF circulation, the flow depends on pulsation of
the arterial vessels and giving the speed of the flow of CSF in a given
direction. The pulsating wave is mechanical and reverberates along
the ventricular system. The fourth ventricle is located at the end of
this route; the mechanical wave is reflected as a result of pulsation
and occurs constructive interference which has an impact on the
ventricular walls being anatomical structures of the brainstem.
It may be possible the mechanism of constructive interference of
the pulsating mechanical waves is responsible for the development
of so called “functional trapped fourth ventricle” described in the
literature and characterized by no mechanical obstacle inside of
Sylvian aqueduct observed during aqueductoplasty [8,30,31].
Conclusion
The presented clinical case of IFV which was diagnosed during the long-term ICU stay is the only one in the literature. The mechanism of the alteration can have a significant impact on the lack of success in therapy due to brain stem compression and mass effect in posterior fossa. The adequate diagnosis of IFV is crucial. It is very important to observe the unconscious patient for possible brainstem dysfunction during long lasting hospital stay in ICU and perform sequential brain image monitoring. According to publications, we can anticipate development of IFV after neurosurgical activity in CSF space, CNS infections, post inflammatory hydrocephalus and external drainage, bleeding to the posterior fossa, complications after the ventricleperitoneal shunt operation or after prolonged external drainage in supratentorial spaces. In ICU the monitoring of the brainstem function and cranial nerve symptoms is especially important, in the context of pharmacotherapy, including sedation, the use of opioids and muscle relaxants.
References
- Ang BT, Steinbok P, Cochrane DD. Etiological differences between the isolated lateral ventricle and the isolated fourth ventricle. Childs Nerv Syst. 2006;22(9):1080-5.
- Tseng JS, Lee YC, Pan HC, Chang MH. Motor neuron disease-like syndrome secondary to trapped fourth ventricle and obstruction of cerebrospinal fluid pathway. Clin Neurol Neurosurg. 2007;109(4):383-7.
- Rekate HL. Etiological differences between isolated lateral ventricle and the isolated fourth ventricle. Childs Nerv Syst. 2007;23(5):479.
- Ali K, Nannapaneni R, Hamandi K. The isolated fourth ventricle. BMJ Case Rep. 2013;2013.
- Mahlmann E, Voth D, Schwarz M. The Isolated Fourth Ventricle: Review of Current Concepts and Report on Three Cases in Children. Tumours of the Central Nervous System in Infancy and Childhood. 1982;26:180-5.
- McLaurin RL, Ford LE. Obstruction following posterior fossa surgery: the post-operative Dandy-Walker Syndrome. Johns Hopkins Med J. 1968;122(5):309-18.
- Scatliff JH, Kummer AJ, Frankel SA, German WJ. Cystic enlargement and obstruction of the fourth ventricle following posterior fossa surgery: The postoperative Dandy-Walker Syndrome. Am J Roentgenol Radium Ther Nucl Med. 1962;88:536-42.
- Ferrer E, De Notaris M. Third ventriculostomy and fourth ventricle outlets obstruction. World Neurosurg. 2013;79(2 Suppl):S20.e9-13.
- Dandy WE. The diagnosis and treatment of hydrocephalus due to occlusion of the foramina of Magendie and Luschka. Surg Gynecol Obstet. 1921;32:112-24.
- Matsushima T, Rhoton AL Jr, Lenkey C. Microsurgery of the fourth ventricle: Part 1. Microsurgical anatomy. Neurosurgery. 1982;11(5):631-67.
- Simonin A, Levivier M, Bloch J, Messerer M. Cranial nerve palsies after shunting of an isolated fourth ventricle. Case Report. BMJ Case Reports. 2015.
- Udayakumaran S, Beni Adani L. Unusual case of 'trapped fourth ventricle' in a child with posthemorrhagic hydrocephalus--lessons learnt. Pediatr Neurosurg. 2011;47:60-5.
- Harter DH. Management strategies for treatment of the trapped fourth ventricle. Childs Nerv Syst. 2004;20(10):710-6.
- Armbruster L, Kunz M, Ertl-Wagner B, Tonn JC, Peraud A. Microsurgical outlet restoration in isolated fourth ventricular hydrocephalus: a single-institutional experience. Childs Nerv Syst. 2012;28(12):2101-7.
- Fritsch MJ, Kienke S, Manwaring KH, Mehdorn HM. Endoscopic aqueductoplasty and interventriculostomy for the treatment of isolated fourth ventricle in children. Neurosurgery. 2004;55(2):372-7.
- Hamada H, Hayashi N, Kurimoto M, Endo S. Endoscopic aqueductal stenting via the fourth ventricle under navigating system guidance: technical note. Neurosurgery. 2005;56(1Suppl):E206.
- Mohanty A. Endoscopic options in the management of isolated fourth ventricles. Case report. J Neurosurg. 2005;103(1 Suppl):73-8.
- Cinalli G, Spennato P, Savarese L, Ruggiero C, Aliberti F, Cuomo L, et al. Endoscopic aqueductoplasty and placement of a stent in the cerebral aqueduct in the management of isolated fourth ventricle in children. J Neurosurg. 2006;104(1 Suppl):21-7.
- Ersahin Y. Endoscopic aqueductoplasty. Childs Nerv Syst. 2007;23(2):143-50.
- Upchurch K, Raifu M, Bergsneider M. Endoscope-assisted placement of a multiperforated shunt catheter into the fourth ventricle via a frontal transventricular approach. Neurosurg Focus. 2007;22(4):E8.
- Mohanty A, Biswas A, Satish S, Vollmer DG. Efficacy of endoscopic third ventriculostomy in fourth ventricular outlet obstruction. Neurosurgery. 2008;63(5):905-13.
- Little AS, Zabramski JM, Nakaji P. Simplified aqueductal stenting for isolated fourth ventricle using a small-caliber flexible endoscope in a patient with neurococcidiomycosis: technical case report. Neurosurgery. 2010;66(6 Suppl Operative):373-4.
- Longatti P, Marton E, Magrini S. The marionette technique for treatment of isolated fourth ventricle: technical note. J Neurosurg Pediatr. 2013;12(4):339-43.
- Fritsch MJ, Schroeder HW. Endoscopic aqueductoplasty and stenting. World Neurosurg. 2013;79(2 Suppl):S20.
- Hamada H, Hayashi N, Asahi T, Kurimoto M, Hirashima Y, Endo S. Efficacy of a navigation system in neuro-endoscopic surgery. Minim Invasive Neurosurg. 2005;48(4):197-201.
- Pang D, Zwienenberg-Lee M, Smith M, Zovickian J. Progressive cranial nerve palsy following shunt placement in an isolated fourth ventricle: case report. J Neurosurg. 2005;102(3 Suppl):326-31.
- Spennato P, O'Brien DF, Fraher JP, Mallucci CL. Bilateral abducent and facial nerve palsies following fourth ventricle shunting: two case reports. Childs Nerv Syst. 2005;21(4):309-16.
- Novak L, Pataki I, Nagy A, Berenyi E. Bilateral transtentorial herniation and isolated fourth ventricle: a scientific note. Neurol India. 2010;58(6):953-4.
- Udayakumaran S. Bilateral transtentorial herniation and isolated fourth ventricle: a scientific note. Neurol India. 2011;59(2):322.
- Williams HF. The central nervous system pressure histogram in hydrocephalus and hydromyelia. Med Hypotheses. 2017;108:117-23.
- Udayakumaran S, Panikar D. Postulating the concept of compensated trapped fourth ventricle: a case-based demonstration with long-term clinicoradiological follow-up. Childs Nerv Syst. 2012;28(5):661-4.