Case Report
Advanced Colorectal Carcinoma with Testicular Metastasis in an Adolescent: A Case Report
Adarsh Pratap Singh1, Amit Kumar1*, Anita Dhar2, Shipra Agarwal3 and Sudhir Bhimaniya4
1Department of Surgery, AIIMS, New Delhi, India
2Department of Surgery, New Delhi, India
3Department of Pathology, AIIMS, New Delhi, India
4Department of Cardiovascular Radiology, AIIMS, New Delhi, India
*Corresponding author: Amit Kumar, Department of Surgery, AIIMS, New Delhi, India
Published: 09 Oct, 2018
Cite this article as: Singh AP, Kumar A, Dhar A, Agarwal
S, Bhimaniya S. Advanced Colorectal
Carcinoma with Testicular Metastasis
in an Adolescent: A Case Report. Clin
Surg. 2018; 3: 2144.
Abstract
Introduction: Colorectal carcinoma in pediatric age group is rare and tends to be very aggressive
and present late, due to which it has a very poor prognosis. It may present itself with distant
metastasis. But metastasis to the testes is very rare and signifies an advanced stage of the disease.
Surgery is the only effective modality to cure patients with localized colorectal carcinomas. However
statistics show a higher incidence of unrespectable disease and a higher metastasis rate in childhood
colorectal carcinomas. We are presenting a case of advanced colorectal carcinoma in an adolescent
with testicular metastasis.
Case Presentation: A 15 year old Indian male presented to surgical emergency with signs
and symptoms of intestinal obstruction. He also had a history of passing blood and mucus per
rectum. On examination he was having abdominal distension. On digital rectal examination, a
circumferential proliferative growth was felt 1cm above the anal verge. On scrotal examination,
a small nodule was felt in the right testes. In view of intestinal obstruction, the patient was taken
into the emergency operation theatre and a diverting loop sigmoid colostomy was performed to
relieve the obstruction. Punch biopsy from ano-rectal growth taken which suggested signet ring cell
adenocarcinoma. CECT chest, abdomen and pelvis showed advanced colorectal carcinoma with
distant metastasis. Ultrasonography of testes showed a hypoechoic nodule in the right testis from
which a needle aspiration biopsy was done which revealed metastatic adenocarcnoma.
Conclusion: Childhood colorectal carcinomas have very poor prognosis due to their aggressive
nature and late presentation. In spite of all the advances in diagnosis and treatments, the overall
long term survival is still dismal in these patients. Due to rarity of this disease, screening is not
recommended for individuals under the age of 50. Thus, to improve outcome, early diagnosis and
treatment is paramount. For that to happen, awareness needs to be created regarding pediatric
colorectal carcinoma and its signs and symptoms.
Keywords: Adolescent; Colorectal carcinoma; Testicular metastasis; Intestinal obstruction; Signet ring cell adenocarcinoma
Introduction
Colorectal carcinoma is the second most common alimentary tract carcinoma after liver tumors in children with an incidence of 1.3 to 2 cases per million populations, mostly present in the second decade of life [1-4]. It tends to be very aggressive and present late, due to which it has very poor prognosis. It may present itself with distant metastasis. But metastasis to the testes is very rare and signifies advanced stage of the disease. Surgery is the only effective modality to cure patients with localized colorectal carcinomas. We are presenting a case of advanced colorectal carcinoma in an adolescent with testicular metastasis.
Case Presentation
A 15 years old Indian male presented to Surgical emergency with complaints of difficulty
in passing stool for one month, passage of blood and mucus per rectum for 15 days, abdominal
distension for 1week and obstipation for 3 days. These symptoms were associated with significant
appetite and weight loss but there was no history of fever, jaundice, malena, hemetemesis,
hemoptysis, cough, chest pain, shortness of breath. There was no history of similar illness in family,
and any other malignancy.
On examination patient was conscious with thin built and pallor
was present. Abdomen was distended with no local bulge. On digital
rectal examination, a circumferential proliferative growth was felt
1 cm above the anal verge, which was occluding the lumen near
completely. On scrotal examination, a small nodule was felt in Right
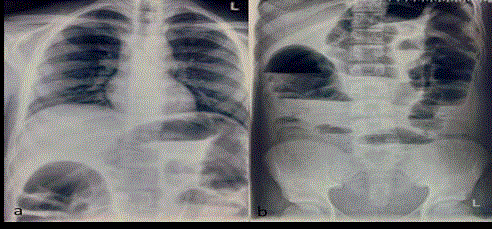
testis. Rest systemic examination was normal. An abdominal and
chest X-ray was done as preliminary investigations which revealed
signs of intestinal obstruction (Figure 1).
In view of intestinal obstruction, the patient was taken into the
emergency operation theatre and a diverting loop sigmoid colostomy
was performed. Patient symptomatically relieved, stoma was well
functioning and healthy.
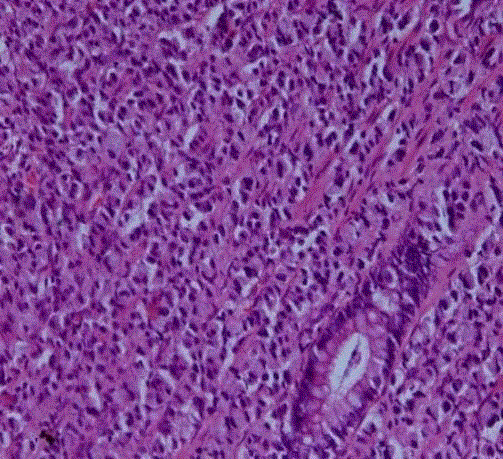
Punch biopsy was taken from ano-rectal growth. HPE report
suggested Signet ring cell adenocarcinoma of rectum (Figure 2).
Tumor markers report: CEA-499.93, AFP-2.42, beta HCG- <1.2,
LDH- 593.
Routine investigations including CBC, LFT, KFT were within
Normal limit.
CECT Chest, Abdomen, Pelvis and Brain was done as a part of
metastatic workup which showed diffuse circumferential homogenous
thickening involving rectum approx 1cm from the anal verge and
extending into sigmoid colon proximally up to colostomy site.
Multiple enlarged lymph nodes, few showing necrosis are noted in
perirectal, iliac, b/l paraortic, periportal and celiac regions. Moreover,
multiple enlarged lymph nodes were seen in the mediastinum in
bilateral paratracheal, prevascular and subcarinal regions, and also
in left supraclavicular region. In addition, hepatomegaly with liver
measuring 17.8 cm was present. However, no lesion was seen in liver
parenchyma. There was mild left sided pleural effusion (Figure 3 and
4). There was no lesion in brain suggestive of metastasis. The right
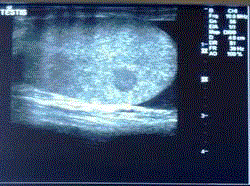
testis was enlarged. Ultrasonography showed a hypoechoic nodule
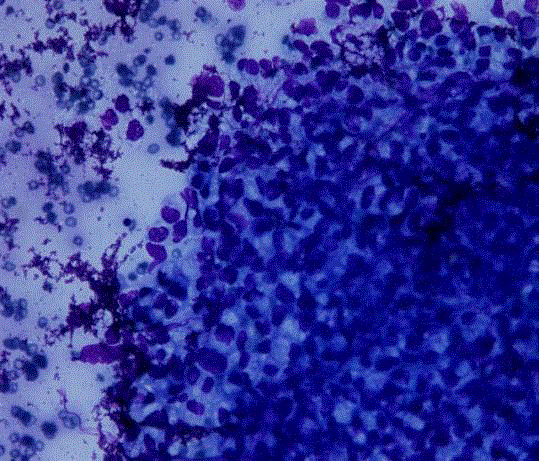
(Figure 5) in the right testis from which a needle aspiration biopsy
was done, which revealed metastatic adenocarcnoma (Figure 6).
In view of distant metastasis, it was planned to give neoadjuvent
chemotherapy to the patient. But within 2 weeks of surgery the patient
developed progressive respiratory distress. Chest X-ray showed
infiltrations and bilateral pleural effusion. Patient got intubated and
was kept in ICU. But his condition deteriorated and he developed
Multiple Organ Dysfunction Syndrome (MODS) in the next few
days. Eventually patient died with multiple organs failure. The entire
course of illness from appearance of first symptom to death was only
2 months.
Figure 1
Figure 2
Figure 3
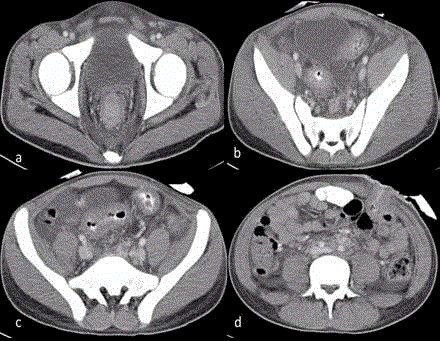
Figure 3
CECT Abdomen and Pelvis. a,b,c - Circumferential growth
involving rectum and sigmoid colon. d-Colostomy site.
Figure 4
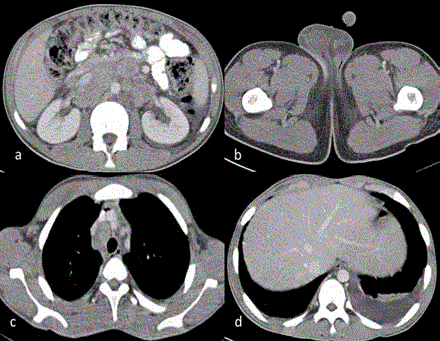
Figure 4
CECT Abdomen, Pelvis and Chest. a) Retroperitoneal
lymphadenopathy; b) Right testicular enlargement; c) Mediastinal
lymphadenopathy; d) Left pleural effusion.
Figure 5
Figure 6
Discussion
Globally, CRC is the third most commonly diagnosed cancer
in males and the second in females, with 1.4 million new cases and
almost 694,000 deaths estimated to have occurred in 2012 [5]. Age is
a major risk factor for sporadic CRC. It is generally considered to be
disease of the elderly, with more than 90% of the patients of colorectal
carcinoma being above 55 years of age. It rarely occurs in teenagers
and adolescents [6].
More recent data from the United States Surveillance,
Epidemiology, and End Results Reporting (SEER) database and
other Western cancer registries [7] suggests that CRC incidence is
increasing in the under-50 age group while it is decreasing in older
groups [8,9]. These increases are driven predominantly by left-sided
cancers in general and rectal cancer in particular [10]. At present,
screening is not recommended for individuals under the age of 50
unless they have a positive family history or a predisposing inherited
syndrome.
Risk factors associated with young patients are Inflammatory
Bowel Disease, HNPCC, Polyposis syndromes of gastrointestinal
tract. APC gene mutation produces classic or attenuated familial
polyposis coli [11]. Mutations in mismatch repair (MMR) genes,
principally MSH2 and MLH1 but also PMS1 and PMS2, cause
HNPCC [12].
Data from the Surveillance, Epidemiology, and End Results
(SEER) program [13] suggests that CRC has a similar natural history
in patient's age 15 years to 29 years as in older patients. However,
current literature suggests that over 86 percent of those diagnosed
under the age of 50 are symptomatic at diagnosis, and this is associated
with more advanced stage at diagnosis and poorer outcomes [11].
Approximately 60% to 86% of pediatric and adolescent patients
have Dukes stage C or D [14]. The increased frequency of mucinous
variants and preponderance of right-sided lesions contribute to the
advanced stage at diagnosis [15,16].
Typical symptoms/signs associated with CRC include
hematochezia or melena, abdominal pain, otherwise unexplained
iron deficiency anemia, and/or a change in bowel habits [17]. Patient
may sometimes present with obstruction or perforation which carry a
poor prognosis, independent of stage [18].
Patients may also present with signs/symptoms of metastatic
disease. CRC can spread by lymphatic and hematogenous
dissemination, as well as by contiguous and transperitoneal routes.
The most common metastatic sites are the regional lymph nodes,
liver, lungs, and peritoneum. Patients may present with signs or
symptoms referable to any of these areas. The presence of right upper
quadrant pain, abdominal distension, early satiety, supraclavicular
adenopathy, or periumbilical nodules usually signals advanced often
metastatic disease.
Metastatic carcinoma to the testis is rare and most often
incidentally found on autopsy [19]. The most common tumor to
metastasize to the testis is prostate (35%), lung (18%), melanoma
(18%), and kidney (9%) [9] and colorectal less than 8% [20].
There are less than 25 reported cases of colorectal cancer
presenting as metastases to testis [21]. The exact mechanism of spread
is unknown but many theories have been suggested. Since most cases
of testicular metastases presented as a hydrocele, it is proposed that
there may be microscopic channels of communications present
between the peritoneum and testes. Other theories include retrograde
venous and lymphatic extension, direct invasion and arterial
embolism [22]. In our case, the patient did not present primarily
with testicular symptoms neither he had hydrocele. He had testicular
nodule which was diagnosed to be metastatic adenocarcinoma on
USG guided needle biopsy. Surgery is the only effective modality
to cure patients with localized CRCs. However, for patients with
cancer staging ≥ III, adjuvant chemotherapy is important to eradicate
micrometastases, thereby reducing disease recurrence and increasing
the cure rate [23]. Statistics show a higher incidence of unresectable,
residual disease and a higher metastasis rate in childhood CRCs [24].
Patients with unresectable tumors diagnosis should undergo only
biopsy and neoadjuvant chemotherapy, with or without radiation
therapy.
The result of many series reported that the overall survival of
the patient depends upon the complete surgical resection of the
tumor and the radical resection of lymph nodes [25], thus, it is the
goal of surgery. However, only 40% to 69% of pediatric patients are
candidates for curative resection, a much lower number than in
adults [26]. Debunking is of little benefit for patients with extensive
metastatic disease. Occasionally, resections of bulky tumors or
metastases offer palliation [26].
Predictors of poor prognosis, apart from the stage of the disease,
are incomplete resection, mucinous histology, proportion of signetring
cells >10%, and absence of an in situ component [23,24]. In spite
of all the advances in diagnosis and treatments, an overall 5-year
survival is around 75% in adult patients but only around 51% in
pediatric population [23].
Conclusion
Colorectal carcinoma in pediatric age group along with testicular metastasis is rare. It tends to be very aggressive and present at a very advanced stage in pediatric patients, due to which it has very a poor prognosis. Due to its rarity, screening is not recommended for individuals under the age of 50. Thus, to improve outcome, early diagnosis and treatment is paramount. For that to happen, awareness among Pediatricians and Surgeons needs to be created regarding pediatric CRC and its signs and symptoms.
References
- Rao BN, Pratt CB, Fleming ID, Dilawari RA, Green AA, Austin BA. Colon Carcinoma in children and adolescents. A review of 30 cases. Cancer. 1985;55(6):1322-6.
- Odone V, Chang L, Caces J, George SL, Pratt CB. The natural history of colorectal carcinoma in Adolescents. Cancer. 1982;49(8):1716-20.
- LaQuaglia MP, Heller G, Filippa DA, Karasakalides A, Vlamis V, Wollner N, et al. Prognostic factors and outcome in patients 21 years and under with colorectal carcinoma. J Pediatr Surg. 1992;27(8):1085-90.
- Steinberg JB, Tuggle DW, Postier RG. Adenocarcinoma of the colon in adolescents. Am J Surg. 1988;156(6):460-2.
- Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65(2):87-108.
- O’Connell JB, Maggard MA, Livingston EH, Yo CK. Colorectal cancer in the young. Am J Surg. 2004;187(3):343-8.
- Cancer in Victoria Statistics & Trends 2010.
- Siegel RL, Miller KD, Jemel A. Cancer Statistics, 2017. CA Cancer J Clin. 2017;67:7-30.
- Davis DM, Marcet JE, Frattini JC, Prather AD, Mateka JJ, Nfonsam VN. Is it time to lower the recommended screening age for colorectal cancer? J Am Coll Surg. 2011;213(3):352-61.
- Ahnen DJ, Wade SW, Jones WF, Sifri R, Mendoza Silveiras J, Greenamyer J, et al. The increasing incidence of young-onset colorectal cancer: a call to action. Mayo clin Proc. 2014;89(2):216-24.
- Dozois EJ, Boardman LA, Suwanthanma W, Limburg PJ, Cima RR, Bakken JL, et al. Young-onset colorectal cancer in patients with no known genetic predisposition: can we increase early recognition and improve outcome? Medicine (Baltimore). 2008;87(5):259-63.
- Brassett C, Joyce JA, Froggatt NJ, Williams G, Furniss D, Walsh S, et al. Microsatellite instability in early onset and familial colorectal cancer. J Med Genet. 1996;33(12):981-5.
- Spunt S, Furman W, La Quaglia M. Colon and rectal cancer. In: Bleyer A, O’Leary M, Barr R, editors. Cancer Epidemiology in Older Adolescents and Young Adults 15 to 29 Years of Age, Including SEER Incidence and Survival: 1975-2000. Bethesda, MD, National Cancer Institute, NIH Pub. No. 06-5767, 2006, pp. 123-134.
- Heiss KF, Schaffner D, Ricketts RR, Winn K. Malignant risk in juvenile polyposis coli: increasing documentation in the pediatric age group. J Pediatr Surg. 1993;28(9):1188-93.
- Mi Yeon Chung, Park YS, Ryu SR, Ahn SB, Kim SH, Jo YJ, et al. A Case of Colonic Mucinous Adenocarcinoma in 19 year-old Male Patient. Clin Endosc. 2012;45:103-7.
- Gupta SK, Fitzgerald JF, Croffie JM, Chong SK, Pfeffekorn MC, Davis MM, et al. Experience with juvenile polyps in North American children: the need for pancolonoscopy. Am J Gastroenterol. 2001;96(6):1695-7.
- Speights VO, Jhonson MW, Stoltenberg PH, Rappaport ES, Helbert B, Riggs M. Colorectal cancer: Current trends in initial clinical manifestations. South Med J. 1991;84(5):575-8.
- Steinberg SM, Barkin JS, Kaplan RS, Stablein DM. Prognostic indicators of colon tumors. The Gastrointestinal Tumor Study Group experience. Cancer. 1986;57(9):1866-70.
- Charles W, Joseph G, Hunis B, Rankin L. Metastatic colon cancer to the testicle presenting as testicular hydrocele. J Clin Oncol. 2005;23(22):5256-7.
- Meacham RB, Mata JA, Espada R, Wheeler TM, Schum CW, Scardino PT. Testicular metastasis as the first manifestation of colon carcinoma. J Urol. 1988;140(3):621-2.
- Ouellette JR, Harboe-Schmidt JE, Luthringer D, Brackert S, Silberman AW. Colorectal cancer metastasis presenting as a testicular mass: case report and review of the literature. Am Surg. 2007;73:79-81.
- Moreno Antón F, Sastre Valera J, Loboff de León B, Lopez-tarruella S, Ortega Medina L, Diaz-Rubio E. Epididymal metastases as the first sign of a colon cancer recurrence. Clin Transl Oncol. 2005;7(7):321-3.
- Koh KJ, Lin LH, Huang SH, Wong JU. CARE--pediatric colon adenocarcinoma: a case report and literature review comparing differences in clinical features between children and adult patients. Medicine (Baltimore). 2015; 94(6):e503.
- Hill DA, Furman WL, Billups CA, Riedley SE, Cain AM, Rao BN, et al. Colorectal carcinoma in childhood and adolescence: a clinicopathologic review. J Clin Oncol. 2007;25(36):5808-14.
- Salas-Valverde S, Lizano A, Gamboa Y, Vega S, Barrantes M, Santamaria S, et al. Colon carcinoma in children and adolescents: prognostic factors and outcome-a review of 11 cases. Pediatr Surg Int. 2009;25(12):1073-6.
- Pediatric Colorectal Tumors. 2016.