Research Article
Use of Intravenous Acetaminophen to Control Pain and Improve Outcomes in Thoracic Surgery
Mehul Patel3, Naveen Jayakumar3, Kian Bagheri4, Kaveh Bagheri2 and Ara S. Klijian1*
1Department of Thoracic Surgery, Sharp and Scripps Hospitals, USA
2Department of Critical Care and Pulmonary Medicine, Sharp Grossmont Hospital, USA
3Department of Internal Medicine, Eisenhower Health, Rancho Mirage, CA, USA
4University of Michigan, USA
*Corresponding author: Ara S. Klijian, Department of Thoracic Surgery, Sharp and Scripps Hospitals, USA
Published: 14 Sep, 2018
Cite this article as: Patel M, Jayakumar N, Bagheri
K, Bagheri K, Klijian AS. Use of
Intravenous Acetaminophen to Control
Pain and Improve Outcomes in
Thoracic Surgery. Clin Surg. 2018; 3:
2105.
Abstract
Objective: The primary objective was to assess whether the addition of IV acetaminophen (Ofirmev)
to standard opioid and ketorolac pain relievers for thoracotomy, Video Assisted Thoracic Surgery
(VATS), and Awake Video Assisted Thoracic Surgery (AVATS) patients reduced ICU length of
stay (LOS), time to extubation, hospital LOS, or opioid use. The secondary outcomes evaluated
were reintubation, patient satisfaction and pain index. We also looked at the occurrence of ileus,
pneumonia, Deep Venous Thrombosis (DVT), Pulmonary Emboli (PE), Urinary Tract Infection
(UTI), Atrial Fibrillation (AF), IV phlebitis, and development of delirium.
Methods: This was a retrospective cohort study conducted in adults who had undergone traditional
thoracotomies, VATS, and AVATS procedures between 2012 to 2018 at two academic centers. We
evaluated 199 cases. There were 98 patients who received only opioids and ketorolac (OK) and 101
patients who received IV acetaminophen in conjunction with opioid and ketorolac and (OK+A).
Patients who did not receive IV Tylenol did so do to lack of availability of IV Tylenol at location/
time of surgery. Treatment groups were not randomized. All procedures were performed by a single
surgeon.
Results: Analysis included all 199 patients. The average LOS, in days, for the OK+A group was 2.33
(95% CI 2.16 - 2.49) after VATS, 1.53 (95% CI 1.37 - 1.69) after AVATS, and 3.57 (95% CI 3.31 -
3.82) after thoracotomy, respectively. In contrast, for the comparator group receiving traditional
pain relievers, mean LOS values were 2.95 (95% CI 2.80 - 3.10), 2.45 (95% CI 2.17 - 2.73), and 5.16
(95% CI 4.64 - 5.677). The average time to extubation (hours) for these procedures in the OK+A
group was 0.33 (95% CI 0.15 - 0.52) for VATS and 1.30 (95% CI 0.94 - 1.66) for thoracotomy, versus,
in the traditional group, 8.37 (95% CI 4.36 - 12.39) for VATS and 18.13 (95% CI 15.69 - 20.56) for
thoracotomy. The average ICU LOS (in days) for the OK+A group was 0.51 (95% CI 0.42 - 0.60)
for VATS, 0.36 (95% CI 0.25 - 0.46) for AVATS, and 1.47 (95% CI 1.34 - 1.60) for thoracotomy. In
contrast, for the traditional group, the ICU LOS was 1.14 (95% CI 1.01 - 1.27) for VATS, 1.39 (95%
CI 1.19 - 1.59) for AVATS, and 2.36 (95% CI 1.90 - 2.82) for thoracotomy. We saw a trend towards
decreased opioid use in patients receiving IV acetaminophen compared to the traditional regimen.
Conclusion: In this non-randomized cohort, addition of IV acetaminophen to traditional pain
management with opioids and ketorolac for both thoracoscopic surgeries and open thoracotomy
led to clinically significant decreases in the average hospital LOS, time to extubation, and ICU LOS.
This effect was most marked in patients having AVATS. Integrating routine IV acetaminophen
usage in patients undergoing thoracic surgery was associated with improved patient comfort
and satisfaction, and helped improve compliance with incentive spirometry, earlier ambulation,
and lower urinary catheter dependence. This would be expected to reduce complications such as
pneumonia, DVT, PE, and UTI. The demonstrated reduced LOS should also translate to improved
hospital cost saving.
Keywords: IV acetaminophen; Ofirmev; Thoracotomy; VATS; AVATS; Multimodal analgesia
Background
Thoracic surgery can lead to nociceptive, neuropathic, and referred pain, which can make
managing pain difficult following thoracic surgeries [1]. Pain in thoracic surgeries can lead to
respiratory splinting which can increase the risks of atelectasis
and development of pneumonia in patients. Poor pain control is
associated with increased catecholamine release, which can trigger
myocardial infarction, strokes, and bleeding complications [2]. This
has led to increased emphasis on controlling pain following surgical
procedures. Optimal pain-controlling strategies remain a challenge
for many surgeons, even in minimally invasive pain sparing thoracic
surgical techniques, such as Awake Video-Assisted Thoracic Surgery
(AVATS), which has been shown to be safe in complex thoracic
surgery with equal or improved outcomes without compromise in
safety [3].
For over two decades, multimodal or balanced pain strategies
have been researched with the goal of combining analgesics from
different pharmacologic groups with differing mechanisms of action
with additive or synergistic effects to improve analgesia efficacy and
safety [4]. Opioid analgesia has traditionally been used to manage
pain in the post-procedure period. However, the adverse effects of
opioids on respiratory depression, Gastrointestinal (GI) motility,
and delirium make it difficult to balance patient's analgesia with
avoiding adverse events. Such adverse events lead to increased ICU
time, hospital stay, re-intubations, and hospital-associated infections.
Inadequate analgesic control can lead to decreased mobility, which
can increase the risk for DVTs, PE, and UTIs. These adverse events
and inadequate pain control can increase healthcare costs and place
unnecessary burden on the healthcare system. Integrating nonopioid
analgesia is increasingly becoming important, especially as
opioid abuse and opioid overdose is increasing. Newer modalities
have become available to manage pain in patients undergoing
thoracic surgery, including thoracic epidural analgesia, paravertebral
analgesia, and intrathecal opioids [1]. However, these all rely on use
of opioids. NSAIDs have also been shown to be beneficial to help
reduce pain and opioid requirement in thoracotomy [1]. However,
NSAIDs in the elderly are associated with acute renal failure and GI
bleed.
Small studies have suggested that IV acetaminophen does not
decrease PACU stay [5]. Other small studies have also suggested
that IV acetaminophen can reduce pain after cardiac surgery but
does not reduce opioid consumption [6]. Douzjian and Kulik et al.
[2] performed a nine-article database review of the routine use of IV
acetaminophen when added to a background of opioid therapy in
post-cardiac surgery patients; they concluded that IV acetaminophen
provided minimal clinical benefits and the potential cost outweighs
the benefits [2]. However, currently there are no clear studies that
examine the role of IV acetaminophen in post thoracotomy, VATS,
and AVATS patients. Here we examine the effect of IV acetaminophen
on hospital length of stay, time to extubation, ICU length of stay,
opioid use, and pain index in patients after thoracotomies, VATS,
and AVATS. In this study we use a multimodal approach for thoracic
procedures, with the use of IV acetaminophen prior to incision, in
combination with NSAID and opioids.
Figure 1
Figure 1
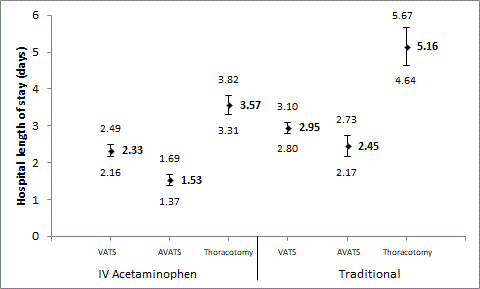
Scatter plot comparing average hospital length of stay (diamond, in
bold) in days between IV acetaminophen and traditional pain management.
Error bars from the mean show 95% confidence intervals. VATS -
video-assisted thoracoscopic surgery; AVATS - Awake Video-Assisted
Thoracoscopic Surgery.
Figure 2
Figure 2
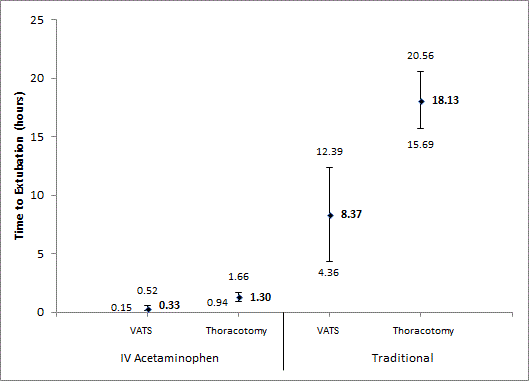
Scatter plot comparing average time to extubation (Diamond, in
bold) in hours between the different groups. Error bars from the mean show
95% confidence intervals.
Figure 3
Figure 3
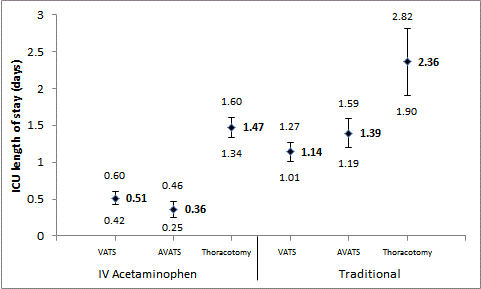
Scatter plot comparing average length of stay in ICU (diamond, in
bold) in days between IV acetaminophen and traditional pain management.
Error bars from the mean show 95% confidence intervals. VATS -
video-assisted thoracoscopic surgery, AVATS - Awake video-assisted
thoracoscopic surgery.
Methods
We extracted data from two academic centers for patients who
had undergone thoracotomy, VATS, and AVATS. The specific types
of procedures we looked at were: lobectomy, segmentectomy, wedge
resection, decortication, pericardial window, bronchopulmonary
fistula repair, and esophageal perforation repair. All procedures
were performed between 2012 and 2018 by a single surgeon (author
A. Klijian). This was a nonrandomized, retrospective chart review
cohort study. We analyzed patients who had undergone the above
procedures and looked at patients who received IV acetaminophen
in conjunction with opioid and ketorolac (OK+A), and those who
received only opioids and ketorolac (OK, traditional treatment
group). Post-procedure patients in both groups were given a standard
opioid protocol of 2 mg IV morphine sulfate and 0.5 mg of IV
hydromorphone, while those in the IV acetaminophen group also
received 1 g IV acetaminophen prior to skin incision, followed by 1
gram every 6 hr as needed to a maximum of 36 hr. All patients, except
for five with renal insufficiency in the IV acetaminophen arm and
four patients in the traditional arm with renal insufficiency received
15 mg IV ketorolac every 8 hours for a total of three doses in both
VATS and AVATS groups and 15 mg IV ketorolac every eight hours
for a total of six doses in the thoracotomy group in both arms. We
looked at how much additional opioid were required in both groups.
There were 199 cases evaluated. There were 101 patients who
received IV acetaminophen in combination with opioids and
ketorolac, and 98 patients who received only opioids and ketorolac
(Table 1). Primary outcomes were time to extubation, ICU Length of
Stay (LOS), hospital LOS, and total opioid use. Secondary outcomes
evaluated included rates of reintubation, patient satisfaction, and pain
index. We also looked at the occurrence of ileus, pneumonia, DVTs,
PE, UTI, atrial fibrillation, IV phlebitis, and development of delirium.
Table 1
Table 2
Results
Patients and treatment
A total of 199 patient charts were analyzed retrospectively from
two academic centers. Baseline demographic data and comorbidities
were well balanced between the two groups (Table 2). Out of the
199 patients, 101 received IV acetaminophen, and 98 underwent
traditional opioid-based analgesic regiment. Similar to the balanced
demographic data, specific procedures performed (i.e. lobectomy,
segmentectomy etc.) were also relatively well-distributed between the
two groups (supplementary data, Tables S1 and S2).
Outcomes
The average LOS in days for the IV acetaminophen group for
VATS, AVATS, and thoracotomies was 2.33 (95% CI 2.16 - 2.49),
1.53 (95% CI 1.37 - 1.69), and 3.57 (95% CI 3.31 - 3.82) respectively.
For the traditional group, the mean LOS was 2.95 (95% CI 2.80 -
3.10), 2.45 (95% CI 2.17 - 2.73), and 5.16 (95% CI 4.64 - 5.677) for
VATS, AVATS and thoracotomies respectively. As demonstrated
in Figure 1, the average length of stay was significantly lower for
the IV acetaminophen groups in comparison to traditional opioidbased
regimens. A similar statistically significant trend was noted for
extubation time, with the exception that AVATS was not included
in the data analysis since these patients were not mechanically
during or after the procedure (Figure 2). The average time
to extubation (hours) for these procedures was 0.33 (95% CI 0.15 -
0.52) for VATS and 1.30 (95% CI 0.94 - 1.66) for thoracotomy in the
IV acetaminophen group and 8.37 (95% CI 4.36 - 12.39) for VATS
and 18.13 (95% CI 15.69 - 20.56) for thoracotomy for the traditional
opioid-based regimen. We also performed similar statistical analysis
for ICU LOS for the traditional pain management and found the
IV acetaminophen group had statistically significant lower values
(Figure 3). The average ICU LOS (in days) for the IV acetaminophen
group was 0.51 (95% CI 0.42 - 0.60) for VATS, 0.36 (95% CI 0.25 -
0.46) for AVATS, and 1.47 (95% CI 1.34 - 1.60) for thoracotomy. For
the traditional group the ICU LOS was 1.14 (95% CI 1.01 - 1.27) for
VATS, 1.39 (95% CI 1.19 - 1.59) for AVATS and 2.36 (95% CI 1.90 -
2.82) for thoracotomy.
Pain control
To investigate if the pain control was affected by using IV
acetaminophen vs. the traditional method, we also compared the
Visual Analogue Pain scale and patient satisfaction scores (0-100%)
between the two groups. Unfortunately, we could not calculate
statistical significance for this data group, since the raw data was not
available for analysis. Overall, we found improved pain scores and
increased patient satisfaction scores (Table 3).
Adverse events
We compared the incidence of adverse events between the
two treatment groups and found them to be lower in the IV
acetaminophen group. The only adverse events noted in this group
were 3 cases of uncomplicated atrial fibrillation compared with 2
cases in the traditional control group. However, more compellingly,
in the traditional opioid-based pain management group, there were
4 incidences of ileus, 3 occurrences of pneumonia, 1 case of deep
vein thrombosis, 2 occurrences of urinary tract infections, 2 episodes
of atrial fibrillation, one occurrence of IV phlebitis, 4 occurrences
of mild delirium, 4 occurrences of moderate delirium, and 1 case
requiring reintubation. Breakdown of the types of procedures are
available in the supplemental data section (Table S3).
Opioid usage
There was a trend towards decreased opioid use in patients receiving
IV acetaminophen. Patients who did not receive IV acetaminophen
required additional doses of morphine and hydromorphone when
undergoing VATS, AVATs, and thoracotomy. For instance, 80%
of the patients who underwent video assisted thoracoscopy in the
IV acetaminophen group received morphine sulfate, and 82% of
patients in the traditional group required morphine, however those
in the traditional group required 5 additional doses of morphine
when compared to the IV acetaminophen group. While statistical
significance of this trend could not be established, this trend was
important to note (Table 4).
Table S1
Table S2
Table 3
Table S3
Table 4
Discussion
Control of pain after thoracic surgery can be difficult. As noted
above, inadequate pain control leads to decreased mobility, with
increased risk for DVTs, PE, and UTIs. Opioids have generally been
the mainstay treatment, but adverse events associated with opioid
use include respiratory depression and ileus. Previous studies have
looked at a multimodal post-operative pain management approach
in which acetaminophen is combined with centrally-acting opioids
for synergistic pain relief after surgery [7]. A systematic review
by Douzjian et al. [10] evaluated the use of IV acetaminophen in
combination with opioids in post-cardiac surgery patients and
found mixed results for reduction in pain, opioid consumption,
and improvement in pulmonary function, and incidence of nausea
and vomiting [2]. Its benefits for pain control were marginal at best.
However, Tzortzopoulou et al. [8] noted that surgical patients who
received a single dose of IV acetaminophen experienced effective
post-operative analgesia for 4 hr, which was associated with a 30%
reduction in opioid consumption over 4 hr.
In this study we assessed the use of IV acetaminophen status-post
thoracotomy, VATS, and AVATS to see its effects on ICU length of
stay, time to extubation, hospital length of stay, and opioid use. In this
retrospective study we evaluated patients who received pre-emptive
IV acetaminophen in conjunction with opioids and those who
received only traditional opioids. Pre-emptive IV acetaminophen
followed by prn use of IV acetaminophen led to clinically significant
decrease in the average length of stay when compared to traditional
opioid-based regiments. There was a statistically significant trend
also noted for extubation time, with the exception of AVATS. The
IV acetaminophen group also had statistically significant lower
values for ICU LOS. There were also improved pain control and
patient satisfaction in the IV acetaminophen group. Patients in the
IV acetaminophen group had lower adverse events such as ileus,
pneumonia, DVT, UTI, delirium, and reintubation. There were more
cases of uncomplicated atrial fibrillation in the IV acetaminophen
group. The exact reason for this is unclear. There was a trend towards
decreased opioid use in patients receiving IV acetaminophen. While
it is important to note that statistical significance for opioid reduction,
pain control, and patient satisfaction was not established, the trends
were favorable.
It is important to note that this was a single center nonrandomized
study, which is a weakness of this study. Further studies
are needed to validate the pre-emptive use of IV acetaminophen and
its regularly scheduled use after thoracic procedures. In this study we
implemented a balanced analgesia approach, but there were no strict
guidelines on the dosing of the IV acetaminophen in the post-op
period. The results from this study do suggest that IV acetaminophen
can play a significant role in thoracic surgical procedures as part of a
multimodal analgesic approach to help pain control, decrease opioid
use, and improve overall outcomes.
Conclusion
Use of IV acetaminophen routinely in conjunction with traditional pain management for both thoracoscopic surgery and open thoracotomy led to significant decreases in the average hospital length of stay, time to extubation, and ICU length of stay, with best results seen in the patients having AVATS with IV acetaminophen use. AVATS has been shown to improve outcomes compared to traditional VATS cases [3,9-11] combined with use of IV acetaminophen obtained best results. Integrating routine IV acetaminophen usage in patients undergoing thoracic surgery also improves patient comfort and satisfaction, helping to improve compliance with incentive spirometry usage, earlier ambulation, and lower urinary catheter dependence. This in turn minimized complications such as pneumonia, DVT, PE, and UTI. These improvements are expected to translate to improved hospital cost savings.
Financial Disclosures
This work was funded through a medical writing grant from Mallinckrodt Pharmaceuticals.
References
- Mesbah A, Yeung J, Gao F. Pain after thoracotomy. BJA Education. 2016;16(1):1-7.
- Douzjian DJ, Kulik A. Old Drug, New Route: A Systematic Review of Intravenous Acetaminophen After Adult Cardiac Surgery. J Cardiothorac Vasc Anesth. 2007;31(2):694-701.
- Klijian A, Kourajian P, Gibbs MW. AVATS: Awake Video-Assisted Thoracic Surgery in Complex Thoracic Procedures. Clinics in Surgery-Thoracic Surgery. 2016;1:1006:1-3.
- White PF, Kehlet H. Improving Postoperative Pain Management. Anesthesiology. 2010;112(1):220-5.
- Mamoun NF, Lin P, Zimmerman NM, Mascha EJ, Mick SL, Insler SR, et al. Intravenous acetaminophen analgesia after cardiac surgery: a randomized, blinded, controlled superiority trial. J Thorac Cardiovasc Surg. 2016; 152(3):881-9.
- Khobrani AM, Camamo JM, Patanwala AE. Effect of Intravenous Acetaminophen on Post-Anesthesia Care Unit Length of Stay, Opioid Consumption, Pain, and Analgesic Drug Costs after Ambulatory Surgery. P T. 2017;42(2):125-39.
- Kehlet H, Dahl JB. The value of “multimodal” or “balanced analgesia” in postoperative pain treatment. Anesth Analg. 1993;77(5):1048-56.
- Tzortzopoulou A, McNicol ED, Cepeda MS. Single dose intravenous propacetamol or intravenous paracetamol for postoperative pain. Cochrane Database Syst Rev. 2011;CD007126.
- Klijian AS. AVATS: Awake Video Assisted Thoracic Surgery for Patients with Poor Pulmonary Function. American Journal of Respiratory & Critical Care Medicine. 2018;197:A6416.
- Klijian AS, Gibbs M, Andonian NT. AVATS: Awake Video Assisted Thoracic Surgery- extended series report. J Cardiothorac Surg. 2014;9:149.
- Klijian AS. Awake Video Assisted Surgery (AVATS): Performing Complex Thoracic Surgical Procedures without General Anesthesia. Journal Chest. 2016;150(Suppl 4):30A.