Case Report
Multifocal Central Giant Cell Granuloma of the Mandible in 9 Year Old Boy with One Stage Surgery using Fibula Free Flaps with Virtual Surgical Planning
Łukasz Krakowczyk1*, Krzysztof Dowgierd2, Maciej Borowiec2 and Dominika Smyczek3
1Department of Oncological and Reconstructive Surgery, Maria Sklodowska-Curie Institute-Oncology Center Gliwice Branch, Poland
2Department of Head and Neck Surgery-Maxillofacial Surgery in Olsztyn, Voivoid Children Hospital, Poland
3Department of Pediatric Surgery and Urology, Medical University of Silesia in Katowice, Poland
*Corresponding author: Łukasz Krakowczyk, Department of Oncological and Reconstructive Surgery, Maria Sklodowska-Curie Institute-Oncology Center Gliwice Branch, 44-100 Gliwice, ul. Wybrzeże AK 15, Poland
Published: 16 Aug, 2018
Cite this article as: Krakowczyk Ł, Dowgierd K, Borowiec
M, Smyczek D. Multifocal Central Giant
Cell Granuloma of the Mandible in 9
Year Old Boy with One Stage Surgery
using Fibula Free Flaps with Virtual
Surgical Planning. Clin Surg. 2018; 3:
2072.
Abstract
Central Giant Cell Granuloma (CGCG) accounts for 1% to 7% of all benign lesions of the head and neck. It often arises in the maxilla followed by mandible and affects children and young adults. Free flap surgery in the pediatric population has gained widespread acceptance regarding its technical utility and reliability. One-stage reconstruction combining osseous free flaps with virtual surgical planning are becoming the standard for mandibular defects. The aim of this study was the present the case with fibula free flap with virtual surgical planning for reconstruction after resection of multiple central giant cell granulomas of the mandible and to assess the feasibility and safety of this technique.
Introduction
Central Giant Cell Granuloma (CGCG) is not a true neoplasm but rather a reactive process;
its origin can be triggered by trauma or inflammation. Most commonly the disease affects maxilla
followed by the mandible and often seen in children and young adults, predominantly females, in
the second and third decade of life [1]. Fast-growing lesions have rarely been reported. In these
six cases, CGCG are characterized by an aggressive behavior against an innocent histological
appearance, pain, and rapid facial swelling. The clinical importance of these benign tumors is that
they clinically mimic a malignant lesion [2,3]. The present case illustrates a rare aggressive variety of
CGCG, with an atypical clinical presentation in young boy; attention has been focused in particular
on surgical treatment with custom-made 3D models.
Free flaps are a useful reconstructive option in the management of mandible defects, even in
the pediatric population [4]. Initial concerns as to the feasibility and reliability of the procedure in
children were readily overcome by the fact that the relative size of the pedicle vessels is larger than
those in adults [5].
The aim of this study was the present the case with fibula free flap with virtual surgical planning
for reconstruction after resection of multiple central giant cell granulomas of the mandible and to
assess the feasibility and safety of this technique.
Case Presentation
The 9-year-old boy who underwent fibula free flap reconstruction using the virtual surgical
planning following resection of mandible multiple tumors at the Children’s’ Hospital in Olsztyn
in 2016. The patient has undergone ablative surgery and primary free flap reconstruction at our
institution and the pathology report was confirming the aggressive variety of CGCG. Follow-up
notes from surgical and medical outpatient clinics were reviewed for late complications, evaluation
of growth and function of the reconstructed area and donor sites, and outcome. The follow-up is
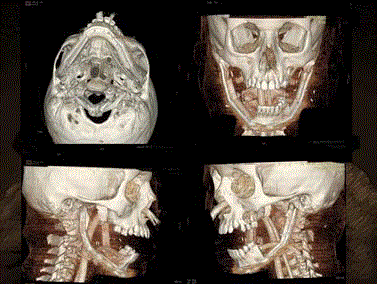
24 month. As a part of our workup imaging studies were obtained, including a craniofacial CT and
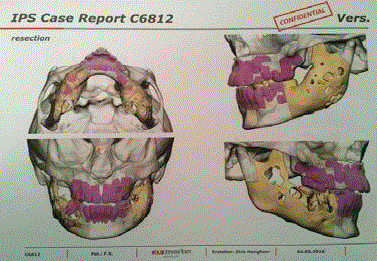
lower extremity CT. Virtual surgical planning was used to provide fibular cutting guidelines and to
provide custom contoured plates and splints.
The fibula free flap for reconstruction of defects following surgery for giant cell granuloma of
the mandible was performed. In this case almost whole mandible without mental protuberance was
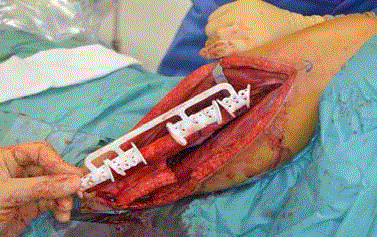
performed. The fibula osteoseptocutaneous flap was designed with
small 2 cm x 5 cm skin paddle as a survival monitor with isolated
about 15 cm peroneal vessel pedicle. Prior to pedicle division the
fibula cutting guide was attached to the fibula. Proximal and distal
osteotomies were then performed and connected to the individual
titanium plate. A limited neck dissection exposing the facial artery
and vein was performed. Using a Gore tunneler, the peroneal vessels
were passed down to the exposed neck vessels. After osteosynthesis
fibula with mandible the microvascular anastomosis were performed,
connecting the facial artery with the peroneal artery using coupler
size 1.5 mm, and facial vein with peroneal vein using coupler size 2.5
mm. The skin island was sutured as a survival monitor to the sub
mental region; he did not require a tracheostomy. There was no
donor site complication. Functional outcome, including mastication,
deglutition, and speech was very satisfactory. The boy has intelligible
speech and the cosmetic result was excellent. There was no impairment
of donor site growth or function.
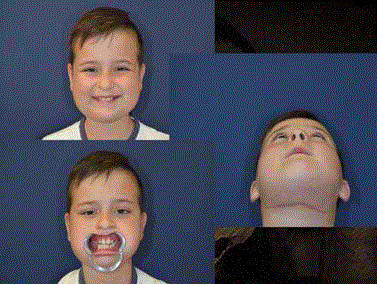
Figure 1
Figure 2
Figure 3
Figure 4
Figure 5
Figure 6
Discussion
Central Giant Cell Granuloma (CGCG) is found in 75% in the
mandible, usually near the mental foramen, also in the region of
molar teeth. In the presented case, the multifocal tumor was detected
in mandible. From slow and asymptomatic growth, associated with
non-aggressive form, which applies to 60% to 80% of cases that
stay unnoticed for a long time, because of their growth inside of the
trabecular bone and no pain or neurological disorders. However
migration of teeth can be observed. To the rarely occurring aggressive
type, usually found in 19 to 40% of all CGCG cases, which causes
bone mutilation, migration and loss of teeth, root resorption and
infiltration of the soft tissues. Frequent symptoms are pain and
paresthesia, pathological fractures and recurrences [1,2].
The use of a vascularized composite bone flap for functional
mandible reconstruction represents the current state-of the-art
technique. Satisfactory aesthetic results can be achieved using the
fibula flap with virtual surgical planning, which is the ideal choice
for mandible reconstruction [5,6]. In the present case, the autologous
reconstruction utilized digital technology and custom-made models
were performed with excellent functional and aesthetic results.
However, the short-term outcome particularly if this does not
extend through puberty-may differ significantly from the final result
following the adolescent growth spurt and resultant anatomical
changes and asymmetries.
The surgical result of this case demonstrate that free flap
reconstruction using virtual planning is an efficient and relatively safe
technique for reconstructing surgical defects of the head and neck
in children undergoing extensive surgery. Despite the difficulties
in performing the surgery and in the postoperative care of these
children, free flap reconstruction provides satisfactory functional and
esthetic results.
References
- Bataineh AB, Al-Khateeb T, Rawashdeh MA. The surgical treatment of central giant cell granuloma of the mandible. J Oral Maxillofac Surg. 2002;60(7):756-61.
- Thompson SH, Bischoff P, Bender S. Central giant cell granuloma of the mandible. J Oral Maxillofac Surg. 1983;41(11):743-6.
- Harii K, Ohmori K. Free groin flaps in children. Plast Reconstr Surg. 1975;55(5):588-92.
- Akçal A, Karşıdağ S, Sucu DÖ, Turgut G, Uğurlu K. Microsurgical reconstruction in pediatric patients:a series of 30 patients. Ulus Trauma Acil Cerr Derg. 2013;19(5):411-6.
- Parry SW, Toth BA, Elliott LF. Microvascular free-tissue transfer in chidren. Plast Reconstr Surg. 1988;81(6):838-40.
- Runyan CM, Sharma V, Staffenberg DA, Levine JP, Brecht LE, Wexler LH, et al. Jaw in a day-state of the art in maxillary reconstruction. J Craniofac Surg. 2016;27(8):2101-4.
- Arnold DJ, Wax MK. Microvascular Committee of the American Academy of Otolaryngology-Head and Neck Surgery, Pediatric microvascular reconstruction; a report from the Microvascular Committee. Otolaryngol Head Neck Surg. 2007;136:848-51.