Research Article
Value of Vessel Sealing System in Skin-Sparing Mastectomy in Patients with Early Breast Cancer
Jun Hirano, Satoki Kinoshita*, Takashi Kazama, Naoko Shimada, Ryo Miyake, Ken Uchida and Hiroshi Takeyama
Department of Surgery, Jikei University School of Medicine, Japan
*Corresponding author: Satoki Kinoshita, Department of Surgery, Jikei University School of Medicine, 3-25-8 Nishishimbashi, Minato-ku, Tokyo, 105-8461, Japan
Published: 31 Jul, 2018
Cite this article as: Hirano J, Kinoshita S, Kazama T,
Shimada N, Miyake R, Uchida K, et al.
Value of Vessel Sealing System in Skin-
Sparing Mastectomy in Patients with
Early Breast Cancer. Clin Surg. 2018;
3: 2055.
Abstract
Purpose: Skin-Sparing Mastectomy (SSM) with immediate breast reconstruction is generally chosen
to achieve radical cure with favorable cosmetic outcome in patients with breast cancer, but some
skin approaches limit exposure of the surgical field. We evaluated our results using a Vessel Sealing
System (VSS) to determine if its use counterbalanced limitations associated with these approaches.
Methods: We retrospectively reviewed records of 365 consecutive patients with breast cancer who
underwent mastectomy between February 2007 and August 2017 to identify 148 cases that employed
either of 2 skin approaches-a periareolar incision with midaxillary line incision or areola-sparing
incision with midaxillary line incision.
Results: We divided cases into 2 groups of 74 each that either did or did not employ the VSS system
and observed significant differences between the groups in intraoperative hemorrhage (214 g vs. 106
g, p<0.000), length of midaxillary line incision scar (136 mm vs. 86 mm, p<0.000), and postoperative
hospital stay (14.9 days vs. 10.9 days, p<0.000), findings that suggested the system’s use improved
outcomes.
Conclusions: Significant advantages using the vessel sealing system in skin-sparing mastectomy
compensated for drawbacks associated with inadequate operative field exposure with some
approaches.
Keywords: Breast cancer; Skin-sparing mastectomy; Vessel sealing system
Introduction
Since Halsted [1] first performed radical surgery for breast cancer in 1882, therapeutic strategies
and surgical techniques have evolved [2]. Today, the major objective of surgical treatment is the local
control of cancer as a part of systemic therapy [3], and breast-conserving surgery is the mainstream
treatment.
The breast surgeon faces the ongoing challenge to cure the cancer and achieve a favorable
cosmetic outcome in that process, and Skin-Sparing Mastectomy (SSM) with immediate breast
reconstruction, reported by Toth and Lappert [4] in 1991, has become the generally acknowledged
best method to accomplish those sometimes seemingly conflicting tasks.
At Jikei University hospitals, we have adopted this method in cooperation with plastic surgeons
and achieved excellent results since 2003 [2], developing, after some trial and error, 4 types (5
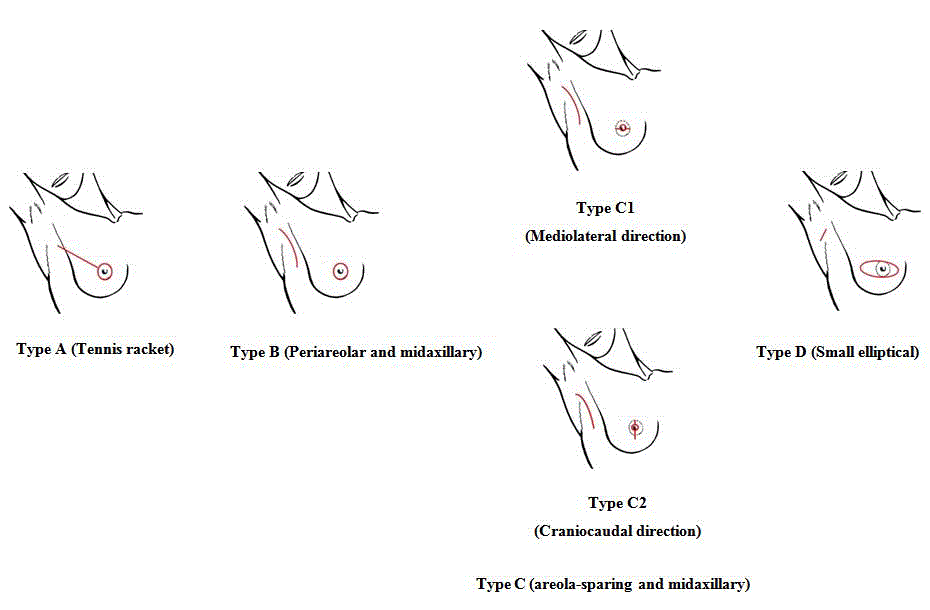
approaches) of skin incision for SSM (Figure 1) [5-7].
These include a periareolar incision with lateral extension that is described as a “tennis racket”
incision (Type A in Figure 1); a periareolar incision with a midaxillary line incision (Type B); an
“areola-sparing” incision (Type C) that combines a straight incision in either a mediolateral (Type
C1) or craniocaudal direction (Type C2) with a small elliptical incision at the base line of the nipple
within the areola complex (Type C2 adds a caudal extension if needed) with a midaxillary line
incision; and a small transverse elliptical incision that contains the entire nipple areolar complex
combined with a transverse axillary incision (Type D).
We have achieved superior postoperative aesthetic results using 2 of the 4 approaches, the
periareolar incision with midaxillary line incision (Type B in the figure 1) and areola-sparing
incision with midaxillary line incision (Type C), but optimal exposure of the operative field with
either of these approaches is difficult and requires particular skill. To address this issue, we began
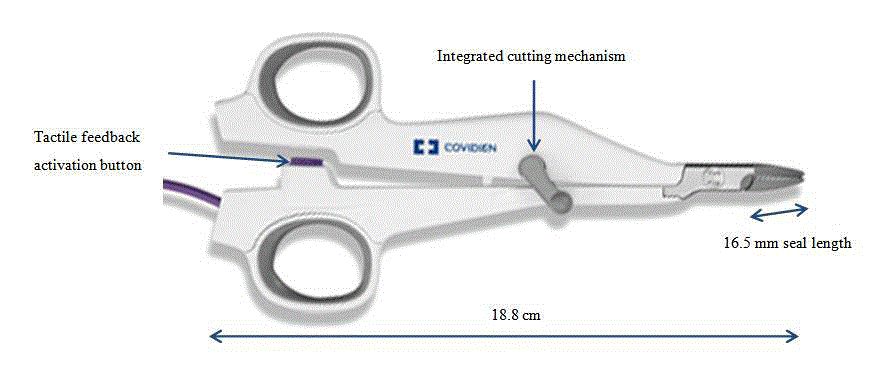
using a Vessel Sealing System (VSS) (LigaSure Small Jaw™, Covidien,
Boulder, Colorado, USA) in April 2012 (Figure 2) that achieves
simultaneous hemostasis with severing.
We herein report our experience of the vessel sealing system’s
contributions to improving surgical and cosmetic outcomes in these
patients despite the limitations associated with these approaches.
Figure 1
Figure 2
Patients and Methods
Among 365 Japanese women with breast cancer who underwent
mastectomy at Jikei University hospitals between February 1, 2007
and August 31, 2017, we identified 148 skin-sparing mastectomy
cases that employed either the periareolar incision with midaxillary
line incision (Type B) or areola-sparing incision with midaxillary
line incision (Type C) that was immediately followed by breast
reconstruction by plastic surgeons. Skin-sparing mastectomy was
planned to remove the nipple with or without the areola complex,
biopsy scars (excluding the core needle biopsy scar), and the entire
breast parenchyma [4].
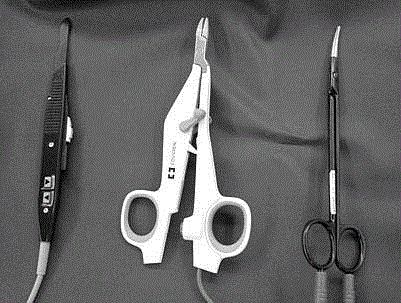
Figure 3 shows our favorite devices for SSM: a heated scalpel
system (Thermal Scalpel™, Hemostatix Medical Technologies, LLC,
Bartlett, TN, USA), vessel sealing system (LigaSure Small Jaw™,
Covidien, Boulder, Colorado, USA), bipolar scissors (Ethicon
POWERSTAR™ scissors, Johnson & Johnson Co, New Brunswick,
NJ, USA). We have used bipolar scissors, heated scalpel system and
conventional electrocautery in creating skin flap between February
2007 and March 2012. Since April 2012, we have applied VSS instead
of bipolar scissors.
We assigned the 148 patients to either of 2 groups of 74 each,
those in whom VSS was not used (non-VSS group) and those in
whom it was used (VSS group), retrospectively evaluated the duration
of SSM, blood loss during SSM, length of midaxillary line incision,
and duration of postoperative hospital stays, and then analyzed
statistics using the chi-square test and t-test, with p< 0.05 considered
significant difference.
Figure 3
Figure 3
The authors’ favorite devices for SSM:
(a) Thermal ScalpelTM, (b) LigaSure Small JawTM, (c) Power Star scissorsTM.
Table 1
Table 1
Results and characteristics of patients, tumors, operative procedures, type of axillary management.
Results
Table 1 delineates the characteristics of our study patients and
their tumors, operative procedures, and type of axillary management.
Tumors were staged based on the system of the American Joint
Committee on Cancer. The mean age of patients was 48.2 years in
the non-VSS group and 47.3 years in the VSS group. The 2 groups
did not differ significantly with regard to staging classification or
average operation time (133.2 minutes [non-VSS group]; 132.7
minutes [VSS group]). However, they did differ significantly with
regard to intraoperative blood loss (213.6 g [non-VSS]; 105.8 g [VSS])
(p<0.000), length of midaxillary line incision (135.7 mm [non-VSS];
86.3 mm [VSS]) (p<0.000), and postoperative hospital stays (14.9
days [non-VSS]; 10.9 days [VSS]) (p<0.000) as well as type of skin
approach employed (p=0.03), axillary management (p=0.002), and
reconstruction procedure (p<0.000).
When performing ALND or SLNB alone in the non-VSS group
and the VSS group respectively, there were no significant differences
of the results (time of SSM, blood loss during SSM, and length of
axillary incision) and the type of skin approaches (Table 2).
Table 3 shows the characteristics of 48 cases with axillary dissection
alone, 33 that were classified in the non-VSS group and 15 in the VSS
group. Those in the non-VSS group experienced significantly shorter
operation duration (158.5 minutes) than that of the VSS group (172.9
minutes) (p=0.01) and significantly longer midaxillary line incision
(p<0.000) and included significantly fewer cases that utilized devicebased
reconstruction (p=0.05).
Table 4 delineates the characteristics of 100 cases with sentinel
lymph node biopsy alone, 41 that were classified in the non-VSS
group and 59 in the VSS group. The non-VSS group experienced
significantly shorter operation duration than the VSS group (112.9
minutes [non-VSS]; 122.6 minutes [VSS]) and underwent significantly
fewer device-based reconstructions (p<0.000). However, the VSS
group demonstrated significantly better findings with regard to blood
loss during SSM (200.5 g [non-VSS]; 96.8 g [VSS]) (p<0.000), length
of midaxillary line incision (132.1 mm [non-VSS]; 82.8 mm [VSS])
(p<0.000), and postoperative hospital stay (13.8 days [non-VSS]; 10.3
days [VSS]) (p<0.000).
Table 5 shows the characteristics of cases using the periareolar
incision with midaxillary line incision (Type B) approach with sentinel
lymph node biopsy alone. None of these cases utilized device-based
reconstructions. Of these 57 cases, 27 were classified in the non-VSS
group and 30 in the VSS group. Operation time was significantly
shorter for the non-VSS group than the VSS group (109.4 minutes
[non-VSS]; 124.1 minutes [VSS]) (p=0.004). However, results for
the VSS group were better with regard to blood loss during SSM
(179.6 g [non-VSS]; 100.2 g [VSS]) (p=0.003), length of midaxillary
line incision (127.0 mm [non-VSS]; 87.8 mm [VSS]) (p<0.000), and
duration of postoperative hospital stays (14.0 days [non-VSS]; 11.9
days [VSS]) (p=0.001).
Postoperative complications included one case with hemorrhage
that required reoperation, 5 cases with insufficient circulation that
resulted in skin necrosis (4 cases) and flap loss (one case), and 2
cases in which infection developed at the surgical site, one of which
required removal of the tissue expander.
Table 2
Table 2
Relationship between type of skin approaches and results (time of SSM, blood loss during SSM, length of axillary incision) when performing ALND or SLNB
alone in the non-VSS group and the VSS group respectively.
Table 3
Discussion
Skin-Sparing Mastectomy (SSM) attempts to preserve all the
breast skin. When we began these surgeries at the beginning of
2003, as previously reported, we initially used a periareolar incision
with lateral extension (Type A) and then adopted a small transverse
elliptical incision that contained the entire nipple areolar complex
with a transverse axillary incision (Type D) just after the introduction
of device-based breast reconstruction [6].
Just as in non-skin-sparing mastectomy, these 2 incision types
allowed clear exposure of the surgical field with relative ease, but
the periareolar incision with midaxillary line incision (Type B) and
areola-sparing incision with midaxillary line incision (Type C) that
are frequently used to improve postoperative cosmetic outcomes
require greater specific surgical skill for sufficient exposure of the
operative field to remove total breast tissue.
Prior to the introduction of the VSS (LigaSure Small Jaw™) in
the spring of 2012, exposure of the surgical field was accomplished
by extending the midaxillary line incision, a technique that reduced
operation time but could not address issues associated with
intraoperative hemorrhage. Vessel sealing system was expected to
overcome these issues. This is accomplished by placing the vessels
and bundle tissues between the 2 electrodes in the jaw of the unit’s
handpiece and applying high‐frequency current from the ForceTriad™
energy platform between the 2 poles to generate Joule heat that fuses
collagen in the vessel wall to seal the vessels as tissue is severed with
the blade of the jaw. Although the length of the instrument is only
18.8 cm, the lengths of the seal (16.5 mm) and cut (14.7 mm) are
considered sufficient to treat relatively small breasts, and it was
adequate in our patients. In addition, the 28.8° jaw angle is suitable
for the subcutaneous detachment, and the reduced thermogenesis
compared to that of other devices is convenient to avoid heat damage
of the skin [8].
The utility of the vessel sealing system (LigaSure Small Jaw™)
to reduce operation time and control hemorrhage in surgery of the
thyroid area has been reported [9], and Chang and associates have
reported similar advantages in its use in SSM for breast cancer [10].
We did not observe significant shorter operation time in our cases,
but differences were significant in blood loss during SSM, length of
midaxillary line incision, and duration of postoperative hospital stays
which is determined based on the volume of fluid drain loss. Because
axillary management differed between the 2 groups, to exclude bias
we compared patients who underwent only axillary lymph node
dissection, and those who underwent only sentinel lymph node
biopsy, between non-VSS group and VSS group. Surprisingly, the
results showed significantly longer operation time in the VSS group,
though in both ALND and SLNB cases, the length of the midaxillary
line incision was about 4 cm to 5 cm shorter in the VSS group. If there
was no such difference in length of midaxillary line incision, we believe
that the use of VSS had contributed to shorten the operation time. We
have used VSS, heated scalpel system and conventional electrocautery
in creating skin flap of SSM since April 2012, although we had used
bipolar scissors instead of VSS between February 2007 and March
2012. When using VSS that can achieve simultaneous hemostasis and
severing, we can perform creating skin flap even under poor exposure
of operative field. Therefore when using VSS, we can complete
almost whole skin flap creation from areolar approach alone. And we
consider that VSS contributes to reduce the intraoperative blood loss
and to shorten the length of axillary incision.
The length of blade part of bipolar scissors is about twice as
compared with VSS one. It contributed to the speedy creating skin
flap, resulting in shortening of operation time. However, when using
bipolar scissors instead of VSS, once an intraoperative bleeding was
happened under the poor exposure of operative field, it was more
difficult for hemostasis compared with VSS. Therefore we have tried
to remove the whole breast under using gauze compression as fast as
possible to complete hemostasis. Furthermore, in creating skin flap
we had preferred axillary approach to get better exposure of operative
field than areolar one even if needed longer length of axillary incision
when using bipolar scissors. And as a result, longer axillary incision
contributed to shorten the time of SSM. Although extending the
midaxillary line incision can shorten operation time without use of
the VSS, the resulting longer surgical scar can compromise cosmetic
results.
In addition, reconstructive procedures may affect the duration of
postoperative hospital stays. Focusing on cases with only SLNB who
underwent the Type B incision with autologous tissue reconstruction
(Table 4), we observed significantly reduced postoperative hospital
stays in the VSS group, which suggests a cost-saving advantage in the
use of the vessel sealing system.
Our findings suggest that use of the current vessel sealing system
in skin-sparing mastectomies that employ Types B and C incisions
can reduce intraoperative hemorrhage, length of midaxillary line
incision, and duration of postoperative hospital stays. And thereby
we consider that use of VSS compensate for the drawbacks such as
limited exposure of the surgical field with these approaches.
From our experience of using VSS, hopefully, we believe that
lengthening the device from the tip of the jaw to the integrated cutting
mechanism by about 3 cm would yield a more user-friendly tool.
Table 4
Table 5
Table 5
Results and characteristics of patients, operative procedure using Type B approach with SLNB alone.
Conclusion
Our use of the vessel sealing system in skin-sparing mastectomies significantly reduced intraoperative hemorrhage, improved postoperative cosmetic outcomes by shortening the midaxillary line surgical wound scar, and reduced costs by reducing the duration of postoperative hospital stays. We therefore consider the system useful as a means to compensate for drawbacks associated with this surgical procedure.
Acknowledgement
The authors would like to thank Rosalyn A Uhrig for Englishlanguage editorial assistance in the preparation of our manuscript.
References
- Halsted WS. I. The Results of Radical Operations for the Cure of Carcinoma of the Breast. Ann Surg. 1907;46(1):1-19.
- Kinoshita S, Nojima K, Takeishi M, Imawari Y, Kyoda S, Hirano A, et al. Retrospective comparison of non-skin-sparing mastectomy and skin-sparing mastectomy with immediate breast reconstruction. Int J Surg Oncol. 2011;2011:876520.
- Fisher B. From Halsted to prevention and beyond: advances in the management of breast cancer during the twentieth century. Eur J Cancer. 1999;35(14):1963-73.
- Toth BA1, Lappert P. Modified skin incisions for mastectomy: the need for plastic surgical input in preoperative planning. Plast Reconstr Surg. 1991;87(6):1048-53.
- Kinoshita S, Kyoda S, Hirano A, Akiba T, Nojima K, Uchida K, et al. Clinical comparison of four types of skin incisions for skin sparing mastectomy and immediate breast reconstruction. Surg Today. 2014;44:1470-5.
- Kinoshita S, Nojima K, Miyake R, Shimada N, Hirano A, Uchida K, et al. Clinical assessment of skin incisions used for skin-sparing mastectomy. Internal Med Review. 2016;2(8):197.
- Kinoshita S, Nojima K, Takeyama H, Uchida K. Four types of skin incisions for skin-sparing mastectomy with immediate breast reconstruction. In: Shiffman MA, editor. Breast reconstruction: art, science, and new clinical techniques. Cham, Switzerland: Springer; 2016. p. 547-54.
- Smith CT, Zarebczan B, Alhefdhi A, Chen H. Infrared thermographic profiles of vessel sealing devices on thyroid parenchyma. J Surg Res. 2011;170(1):64-8.
- Vidal O, Saavedra-Perez D, Valentini M, Astudillo E, Fernández-Cruz L, García-Valdecasas JC. Surgical outcomes of total thyroidectomy using the LigaSure™ SmallJaw versus LigaSure Precise™: A retrospective study of 2000consecutive patients. Int J Surg. 2017;37:8-12.
- Chang YW, Kim HS, Jung SP, Woo SU, Lee JB, Bae JW, et al. Comparison of skin-sparing mastectomy using LigaSure™ Small Jaw and electrocautery. World J Surg Oncol. 2017;15(1):129.