Research Article
Tips and Tricks to Perform Intraoperative Cholangiogram during Single Incision Laparoscopy for Cholecystectomy
Jeremy Lee Kay Hock1, Roxanne Teo2 and Stephen Chang Kin Yong3,4*
1College of Medicine and Health, University College of Cork, Ireland
2School of Medicine, University of Glasgow, Scotland
3Glad Clinic, Mount Elizabeth Hospital, Singapore
4Department of Surgery, Yong Loo Lin School of Medicine, National University of Singapore, Singapore
*Corresponding author: Stephen Chang Kin Yong, Department of Surgery, Yong Loo Lin School of Medicine, National University of Singapore, Singapore
Published: 19 Jul, 2018
Cite this article as: Hock JLK, Teo R, Yong SCK. Tips
and Tricks to Perform Intraoperative
Cholangiogram during Single Incision
Laparoscopy for Cholecystectomy. Clin
Surg. 2018; 3: 2050.
Abstract
Background: Laparoscopic Cholecystectomy (LC) has been the “gold standard” approach for
the removal of gallbladder to treat gallstone disease since the early 1990’s. Routine Intraoperative
Cholangiography (IOC) is often carried out during Conventional Laparoscopic Cholecystectomy
(CLC) to visualise the biliary anatomy and enable prompt management of unanticipated Common
Bile Duct (CBD) injuries. Single - Incision Laparoscopic Cholecystectomy (SILC) offers better
cosmesis and reduced pain, which was reported by various groups. However, routine IOC is not
performed during SILC due to technical difficulties. Our paper aims to describe a technique that
could be utilised to perform IOC during SILC.
Methods: A total of 18 patients who had undergone IOC during SILC via the umbilical port were
studied in detail. Details of the operative methods and the results of IOC during SILC were discussed
in this article.
Results: All of our 18 patients successfully underwent IOC during SILC (100% success rate). A
total of 15 patients’ IOC (83.3%) were normal and 2 patients’ IOC (11.1%) detected aberrant
anatomy that involved the direct insertion of the sectoral duct into the common hepatic duct. Only
1 patient’s IOC (5.5%) reported the finding of a biliary stone in the lower end of the bile duct, and
the patient required post - operative Endoscopic Retrograde Cholangiopancreatography (ERCP)
for its removal.
Conclusion: We believe that our technique is advantageous in that it does not require any additional
ports or percutaneous needle puncture. It was also successfully performed in all 18 of our patients
without any intraoperative complications.
Keywords: Single - incision Laparoscopic Surgery; Intraoperative Cholangiography; Cholecystectomy
Introduction
LC has been the “gold standard” approach for the removal of gall bladder since the 1990’s [1]. Several tiny incisions are made in the abdomen (usually 4) to enable the insertion of operating ports through which laparoscopic instruments can be introduced intra - abdominally. Over time, with the improvement of medical technology, surgeons have developed a new procedure for this minimally - invasive operation. In 1997, Navarra and his team performed the first SILC [2]. This is achieved through a single incision hole at the navel, thereby leaving a barely perceptible scar after the operation. Several studies have shown that SILC has reduced post - operative pain and improved cosmesis [3,4]. Mirizzi first illustrated routine IOC in 1938, in order to provide a radiologic contrast - based examination of the biliary tree and reduce complications associated with cholecystectomy [5]. Routine IOC during CLC is considered to be safe and helps to reduce CBD injuries and detect them early [6,7]. IOC enables the surgeon to gain access to a “map” of the biliary tree to immediately locate and repair CBD injuries. It also prompts immediate intervention when choledocholithiasis is observed. Few reports have included their experience of routine IOC during SILC via a single umbilical port [8,9], however no groups had provided detailed explanation of the techniques involved when carrying out the procedure. The current lack of procedural steps might deter surgeons from carrying out IOC during SILC and opting for an additional pre - operative imaging procedure instead. The aim of this study is to provide an in - depth analysis of the surgical procedure and techniques involved for routine IOC in SILC via the umbilical port. This is to equip surgeons with the relevant skill - set and knowledge on how to approach IOC during SILC with ease.
Figure 1
Figure 2
Figure 2
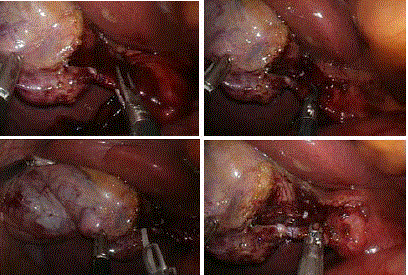
Intraoperative photograph showing A Critical view of safety:(a)
Hepatocystic triangle cleared of fat and connective tissue.(b) Lower one-third
of the gall bladder separated from the liver to expose cystic plate. (c) Two
structures are seen entering the gall bladder. B The “milking” technique using
a grasping forceps to extract biliary stones from the cystic duct for patient
with Choledocholithiasis. C Olsen Reddick clamp with the catheter passing
through the central passageway. D Olsen Reddick clamp is closed around
the catheter and the cystic duct for flushing and IOC procedure.
Materials and Methods
A retrospective case study report was carried out for 18 patients who had undergone routine IOC during SILC by a single surgeon between April 2009 and May 2018. Selection for IOC was made based on biochemical and radiological evidence that suggested the presence of biliary duct stones, which included elevated transaminases, elevated bilirubin and clinical history of jaundice, dilated CBD and obstruction of the bile duct.
Operative Technique
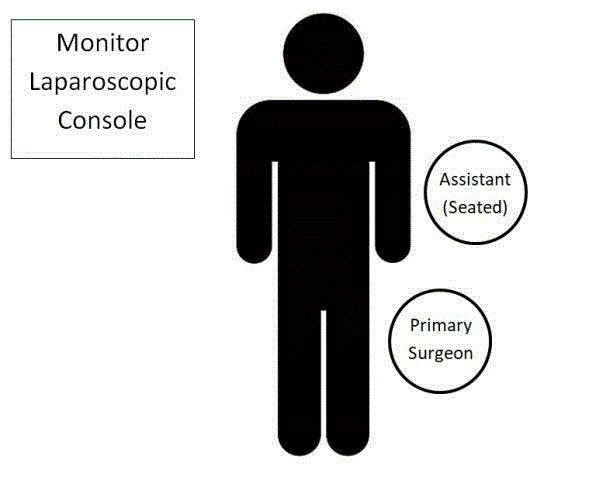
The assistant is positioned on the patient’s left side in front of the surgeon. The assistant is to be seated whilst handling the laparoscopy camera to provide enough room for the surgeon to operate the laparoscopic instruments (Figure 1). A single transumbilical incision of 15 mm is made. Eversion of the umbilicus exposes the fascia, through which a vertical incision is made. A large size Alexis wound protector (Applied Medical, California, USA) is introduced through the incision. A surgical glove is attached to it to serve as a multi - channel port. Wound infiltration with Marcaine was performed prior to incision. Four 5 mm diameter ports and a 10 mm diameter port are inserted through the glove, and a 12 mmHg pneumoperitoneum is created. The Olympus® 5 mm 30o Laparoscope Endoeye is used. The telescope is arranged in the most reliable position, with the instruments superior to the camera and introduced at alternating depths to prevent clashing [10]. An initial assessment of the peritoneal cavity and gall bladder site is performed. Following that, the posterior - lateral peritoneum of the gall bladder is carefully dissected with hook cautery to detach the gall bladder from its lateral aspect. Subsequently, the assistant positioned anterior to the surgeon utilises the grasping forceps to hold the infundibulum of the gall bladder and retract it laterally. This helps to expose Calot’s triangle anterior - medially. Instruments used by the surgeon and his assistant are intersected at the umbilicus to minimise the instances of hand clashing and allow for more precise control of the effector ends of the dissecting instruments [10]. The surgeon uses the Maryland forceps and hook electrocautery to perform dissection of the hepatocystic triangle. This allows for the delineation and exposure of the cystic duct and artery from the underlying fat and connective tissue. During the dissection, the surgeon operates the camera and dissecting instrument in a “snooker cue guide technique” to achieve a greater field of vision as he deems necessary [10]. Instruments are also held in a reverse grip with handles facing upwards to minimise collision with the other hand and instrument. The assistant is to hold the instruments with handles facing laterally to avoid clashing with the surgeon’s instruments. IOC begins after the surgeon attained the critical view of safety (Figure 2A). The cystic duct is then clipped across Hartmann’s pouch, using a 5 mm Hem - o - lok clip (Weck Closure Systems, Research Triangle Park, NC). This prevents the outflow of bile from the gall bladder or contrast into the gallbladder during the procedure. A transverse incision is made on the cystic duct, located below the Hem - o - lok clip. The outflow of bile from the incision hole is observed as a positive indication. The surgeon then utilises the grasping forceps and performed the manoeuvre of “milking” the cystic duct to remove any stones present (Figure 2B). The process is repeated until the surgeon is convinced that any obstruction has been cleared. The liver is then lowered in order to align the cystic duct in the same plane as the direction of the instruments entering the abdomen from the umbilical port. The surgeon then uses the Olsen - Reddick clamp, holding it in a reverse grip with handles facing upwards. The jaws of the clamp are opened, and the 4.0 - Fr flexible tip polyurethane ureteral catheter (Bard Medical, Georgia, USA) is inserted through the centre channel until the catheter tip extends 1 cm beyond the jaws of the clamp (Figure 2C). The catheter is then inserted into the cystic duct. The cholangiogram catheter was pre - bent towards the direction of the cystic duct to facilitate its insertion through the cystic duct ductotomy. The jaws of the clamp are then closed around the cystic duct and cholangiocatheter, so as to prevent leakage through ductotomy (Figure 2D). The use of the pre - bent 4.0 - Fr catheter allows for the insertion of the catheter without kinks. Flushing of the CBD was done with normal saline solution through the cholangiocatheter to check for leaks. The biliary tree is then distended with radioactive iodine - containing dye. This allows the biliary tree to be envisioned under fluorescent scan (Figure 3). In preparation for cholecystectomy, the cystic artery and duct are clipped using the 5 - mm Hem - o - lok clip and then cut using scissors. The gall bladder is then dissected away from the liver bed with hook cautery. Haemostasis is ensured and the surgical field is washed out and all fluid aspirated. The gall bladder is then removed via the umbilical port in a retrieval bag, and the abdomen is closed with two figures - of - eight knots.
Results
All of our 18 patients successfully underwent IOC during SILC (100% success rate). All IOC were completed via a single umbilical incision, and no additional ports or percutaneous needle placement were required. No patients reported any intraoperative complications. Of the 18 patients who underwent IOC during SILC, 15 patients’ IOC (83.3%) were normal, 2 patients’ IOC (11.1%) detected aberrant anatomy that involved the direct insertion of the sectoral duct into the common hepatic duct, and only 1 patient’s IOC (5.5%) reported the finding of a biliary stone in the lower end of the bile duct. This last patient required post - operative ERCP for its removal. Patients’ age ranged from 29 to 71 years, and the mean age was 50 years.
Discussion
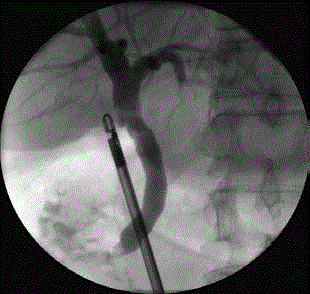
In 1938, Mirizzi first illustrated routine IOC [5]. Since then, surgeons have included routine IOC during CLC as it is generally safe and helps to reduce CBD injuries and detect them early [6,7]. This is the first study illustrating in detail, our techniques involved for routine IOC during SILC via the umbilical port. We hope to equip surgeons with the necessary skill - set and knowledge to perform routine IOC during SILC. The use of routine IOC in LC has been a controversial topic since the introduction of the technique [8,9]. Advocates of the technique have raised points that include protection against CBD transection due to clarification of the biliary tree anatomy [11]. With the increase in use of LC and subsequent surge of CBD injuries [12,13], the use of IOC to prevent misidentification of CBD as a cystic duct seemed to become even more pertinent. Several population - based studies have demonstrated the reduction of CBD injuries in those who underwent IOC compared with those who did not [11,14]. However, opponents of the technique question the protective effect of IOC from CBD injuries, reasoning that the partial ductotomy performed for injection of contrast when CBD has been misidentified, is a CBD injury in itself. Additional points include the increased cost and operative time due to IOC, as well as achieving the critical view of safety to prevent CBD injury [8]. Nevertheless, despite the lack of a conclusion to the debate, several studies have highlighted the role of IOC in reducing CBD injury [9,12], and that selective IOC is necessary in some cases to eliminate the presence of biliary stones. This necessitates the finding of a safer approach to performing IOC during SILC. Some authors have cautioned the use of IOC during SILC could result in increased biliary tract injuries [15]. In this paper, we have demonstrated the operative technique for routine IOC during SILC that can be safely performed through a single laparoscopic incision. The trans- umbilical approach in SILC requires the introduction of the catheter via a perpendicular approach to the cystic duct, and this result in a technical difficulty. However, our technique allows apre - bent catheter to enter the cystic duct without kinking it by lowering the liver. During IOC, the liver is lowered in order to align the cystic duct of the gall bladder with the direction of the Olsen - Reddick clamp. This enables easier access to the cystic duct for the insertion of the catheter. The surgeon uses the Olsen-Reddick clamp, holding it in a reverse grip with handles facing upwards. This prevents clashing with the instruments of his assistant. We find that this technique will help to increase the mobility and control of the laparoscopic instruments, thus reducing the chances of damaging critical structures such as the CBD. In all 18 of our patients where IOC was performed with SILC, IOC was successfully performed without any complications, demonstrating the feasibility and safety of the approach. Several studies have also performed routine IOC during SILC, albeit through an additional skin incision site usually made in the right mid - subcostal region [2,16-22]. One study attributed the need for another incision site for IOC during SILC due to: (i) Technical complications when cannulating the cystic duct via the umbilical port, and (ii) Certain IOC systems require an additional skin incision to be made [22]. The holy grail of SILC is for the procedure to be done through a single tiny incision at the umbilicus, thereby leaving behind a small and barely perceptible scar after surgery [10]. This is unlike CLC which requires multiple incision sites (usually 4) for the insertion of operating ports for the introduction of laparoscopic instruments into the abdomen. The creation of an additional skin incision site for IOC during SILC would therefore undermine the original purpose of performing SILC via a single incision hole. There have been reports of other techniques to performing IOC in SILC. Rawlings et al. [20] reported the routine attempt of IOC using needle puncture techniques, in which a 4.0 - Fr ureteral catheter was inserted into the abdomen through a veress needle or 14 - gauge angiocatheter placed at a mid - clavicular position 2 cm subcostally. This technique reported a success rate of 92.6%, and no intraoperative complications occurred. In comparison to the above - mentioned technique, our approach utilises pre - existing “off - the - shelf” instruments and without the need for extra port or punctures made to the skin. Sato et al. [22] reported the use of the Kumar cholangiography system to achieve a success rate of 90.8%. In this technique, a small needle is used to puncture the gallbladder to insert the catheter, removing the need for partial ductotomy which may result in CBD injury. The use of the Kumar cholangiography system has a downside as the introduction of the catheter and the contrast through the Hartmann’s pouch may result in the flushing of any potential stones within the pouch in the direction of the cystic duct and CBD. This may complicate the surgery and increase intraoperative time. In comparison, our approach avoids this complication as biliary stones are much less likely to be found within the cystic duct, and the cystic duct is palpated prior to insertion of catheter to remove any stones present via the partial ductotomy. Bucher et al. [16], Curcillo II et al. [23] and Yeo et al. [24] have also reported success rates of 90.9%, 97.1% and 96.0% respectively in their attempts with IOC during SILC, although the various techniques were not described in detail. The advantage of IOC in SILC in comparison to IOC performed during CLC lies in the lack of shadowing cast by additional instruments (Figure 3). A typical cholangiogram obtained from CLC approach often shows the presence of shadows cast by additional instruments and catheters. Additional images are required in order to place the instruments in a position to prevent overshadowing of the biliary tree. Additionally, SILC provides various advantages over CLC as described previously, which includes better cosmetic appearance and reduced post - operative pain due to fewer wounds.
Figure 3
Conclusion
In summary, our approach presents an advantageous and feasible approach to performing IOC during SILC. Additional large - scale studies are required to further validate its efficacy and evaluate its clinical value and safety in preventing bile duct injuries in SILC. Although we have yet to attempt this technique with robotic methods, which incidentally are fast gaining traction with patients, it could potentially be applied to single incision robotic cholecystectomy as well. More studies are needed to confirm this.
References
- Soper NJ, Stockmann PT, Dunnegan DL, Ashley SW. Laparoscopic Cholecystectomy The New ‘Gold Standard’? Arch Surg. 1992;127(8):917-23.
- Navarra G, Pozza E, Occhionorelli S, Carcoforo P, Donini I. One-wound laparoscopic cholecystectomy. Br J Surg. 1997;84(5):695.
- Borle FR, Mehra B, Singh AR. Comparison of Cosmetic Outcome between Single-Incision Laparoscopic Cholecystectomy and Conventional Laparoscopic Cholecystectomy in Rural Indian Population: A Randomized Clinical Trial. Indian J Surg. 2015;77(3):877-80.
- Chang SK, Wang YL, Shen L, Iyer SG, Madhavan K. A randomized controlled trial comparing post-operative pain in single-incision laparoscopic cholecystectomy versus conventional laparoscopic cholecystectomy. World J Surg. 2015;39(4):897-904.
- Mirizzi PL. Operative cholangiography its contribution to the physio-pathology of the common bile-duct. The Lancet. 1938;232(5998):366-9.
- Flum DR, Dellinger EP, Cheadle A, Chan L, Koepsell T. Intraoperative cholangiography and risk of common bile duct injury during cholecystectomy. JAMA. 2003; 289(13):1639-44.
- Vezakis A, Davides D, Ammori BJ, Martin IG, Larvin M, McMahon MJ. Intraoperative cholangiography during laparoscopic cholecystectomy. Surg Endosc. 2000;14(12):1118-22.
- Ragulin-Coyne E, Witkowski ER, Chau Z, Ng SC, Santry HP, Callery MP, et al. Is routine intraoperative cholangiogram necessary in the twenty-first century? A national view. J Gastrointest Surg 2013;17(3):434-42.
- Alvarez FA, de Santibañes M, Palavecino M, Sánchez Clariá R, Mazza O, Arbues G, et al. Impact of routine intraoperative cholangiography during laparoscopic cholecystectomy on bile duct injury. Br J Surg. 2014;101(6):677-84.
- Li T, Kim G, Chang S. Tips and tricks to avoid bile duct injury in SILC: an experience of 500 cases. Surg Endosc. 2016;30(11):4750-5.
- Massarweh NN, Flum DR. Role of intraoperative cholangiography in avoiding bile duct injury. J Am Coll Surg. 2007;204(4):656-64.
- Archer SB, Brown DW, Smith CD, Branum GD, Hunter JG. Bile Duct Injury during Laparoscopic Cholecystectomy. Ann Surg. 2001;234(4):549-559.
- Joseph M, Phillips MR, Farrell TM, Rupp CC. Single incision laparoscopic cholecystectomy is associated with a higher bile duct injury rate: a review and a word of caution. Ann Surg. 2012;256(1):1-6.
- Fletcher DR, Hobbs MS, Tan P, Valinsky LJ, Hockey RL, Pikora TJ, et al. Complications of cholecystectomy: risks of the laparoscopic approach and protective effects of operative cholangiography: a population-based study. Ann Surg. 1999;229(4):449-57.
- Saxon C. Single-Port-Access Cholecystectomy: History Should Not Be Allowed to Repeat. World J Surg. 2009;33(5):1020-1.
- Bucher P, Pugin F, Buchs N, Ostermann S, Charara F, Morel P. Single-port-access laparoscopic cholecystectomy. World J Surg. 2009;33(5):1015-9.
- Kravetz AJ, Iddings D, Basson MD, Kia MA. The learning curve with single-port cholecystectomy. JSLS. 2009;13(3):332-6.
- Ponsky TA, Diluciano J, Chwals W, Parry R, Boulanger S. Early experience with single-port laparoscopic surgery in children. J Laparoendosc Adv Surg Tech A. 2009;19(4):551-3.
- Hernandez JM, Morton CA, Ross S, Albrink M, Rosemurgy AS. Laparoendoscopic single-site cholecystectomy: the first 100 patients. Am Surg. 2009;75(8):681-6.
- Rawlings AR, Hodgett SE, Matthews BD, Strasberg SM, Quasebarth M, Brunt LM. Singleincision laparoscopic cholecystectomy: initial experience with critical view of safety dissection and routine intraoperative cholangiography. J Am Coll Surg. 2010;211(1):1-7.
- Hawasli A, Kandeel A, Meguid A. Single-incision laparoscopic cholecystectomy (SILC): a refined technique. Am J Surg. 2010;199(3):289-93.
- Sato N, Shibao K, Akiyama Y, Inoue Y, Mori Y, Minagawa N, et al. Routine Intraoperative Cholangiography During Single-Incision Laparoscopic Cholecystectomy: a Review of 196 Consecutive Patients. J Gastrointest Surg. 2013;17(4):668-74.
- Curcillo II PG , Wu AS, Podolsky ER, Graybeal C, Katkhouda N, Saenz A, et al. Single-port-access (SPA) cholecystectomy: a multi-institutional report of the first 297 cases. Surg Endosc. 2010;24(8):1854-60.
- Yeo D, Mackay S, Martin D. Single- incision laparoscopic cholecystectomy with routine intraoperative cholangiography and common bile duct exploration via the umbilical port. Surg Endosc. 2012;26(4):1122-7.