Research Article
Evaluation of Transanal Endorectal Pull-Through Results
Ahmed A Modaber1*, Ahmed Hammad1 and Vusal Aliyev2
1Department of General Surgery, Mansoura University Hospitals, Egypt
2Department of General Surgery, Emsey Hospital, Turkey
*Corresponding author: Ahmed Abdel Modaber, Department of General Surgery, Mansoura University, Egypt
Published: 16 Jul, 2018
Cite this article as: Modaber AA, Hammad A, Aliyev V.
Evaluation of Transanal Endorectal
Pull-Through Results. Clin Surg. 2018;
3: 2031
Abstract
Background: Harold Hirschsprung, a Danish pediatrician, is credited with the first definitive
description of the disease that bears his name. Over the next 30 years, poorly understood
procedures that were intended to reduce sympathetic hyperactivity of the colon were reported to
be, at least temporarily, successful in treating HD. Complications can be classified as either early
(weeks to months) or late (months to years). The transanal endorectal pull-through approach
represents a major revolution in treating Hirschsprung's disease.
Objectives: The aim of this study was to evaluate the outcome of transanal endorectal pull-through
operation clinically and radio logically in patient with Hirschsprung's disease.
Patients and Methods: This prospective quasi-experimental cohort study was conducted on 40
children with Hirschsprung's disease operated beyond 2 years, in whom transanal endorectal pullthrough
was indicated. For each patient, the following was done prior to the surgical procedure:
Full clinical history taking, Full physical examination, Laboratory investigations, Radiological
examination and rectal biopsy.
Results: Our results showed that; As regards abdominal distension, 14 cases showed no distension,
24 cases showed mild distension and 2 cases showed moderate to severe abdominal distension.
History of previous attack of enterocolitis was positive in all cases. Fourteen patients (35%) had a
normal defecation. Fourteen patients (35%) had a frequency of defecation of 3-5 days. Eight patients
(20%) had a frequency of defecation of 6-7 days. Four patients (10%) had a frequency of defecation
of 8 or more days. Thirty two patients had true fecal incontinence and had a non-dilated colon
on contrast enema and a tendency to have diarrhea and did not respond to medical treatment.
Four patients had partial fetal incontinence and no patients had incontinence. Postoperative soiling
accidents were observed occasionally in 4 patients (10%), often in 18 patients (45%). Perianal skin
excoriation was absent in 36 patients (90%) and present in 4 patients only (10%). Rectal sensation
was preserved in 30 patients (75%).
Conclusion: Transanal Endorectal Pull-Through (TEPT) is a good technique for surgical correction
of Hirschsprung's disease with few operation-related complications. The transanal procedure needs
a special experience and it has to be born in mind that laparotomy may be resorted to any time if
any difficulty was encountered during the procedure. The clinical outcome is satisfactory. Many
children with Hirschsprung's disease have a good outcome following surgical treatment, but longterm
follow-up studies have identified a number of concerns. The predominant cause for persistent
or recurrent unresponsive obstructive symptoms after initial pull-through procedure is incomplete
resection of the transition zone. Fecal incontinence after operative management of Hirschsprung's
disease represents a serious problem. To avoid incontinence after transanal endorectal pull-through,
we recommend the following: overstretching of anal canal, very low colo-anal anastomosi, injury to
sensory mucosa, injury to mussels and inadequate resection of dilated colon. The majority of longterm
follow-up studies have concentrated only on the functional outcome. Although most patients
had good or fair quality of life after surgical correction for Hirschsprung's disease, the long-term
outcome and quality of life are not as good as surgeons expected. Satisfaction of the parents with
the results is a subjective object varies with the socioeconomic levels of the parents; their education
and their residency.
Keywords: Transanal Endorectal Pull-through Hirschsprung; Anal canal; Sbdominal distension
Introduction
Hirschsprung (HD) Disease is a relatively common neonatal developmental disorder of the
enteric nervous system. It is characterized by the absence of ganglion cells in the myenteric and
sub mucosal plexuses of the distal intestine. This results in absent
peristalsis in the affected bowel, and the development of a functional
intestinal obstruction. The pathogenesis and genetic basis of the
disease is yet unclear [1]. The surgical management of Hirschsprungs
Disease (HD) has developed, from full-thickness recto sigmoid
dissection (Swenson and Bill), an endorectal dissection (Soave) and
retro rectal pouch procedure (Duhamel), to more recently a primary
repair that can be done transanally [2]. Langer et al. [3] described
the one-stage transanal pull-through operation for Hirschsprung's
disease Since then, the procedure has become increasingly
popular and compared with the traditional open laparotomy, the
advantages of the operation are that it is minimally invasive, it
eliminates the abdominal incision, so there is no abdominal scar, and
it avoids complications of traditional laparotomy such as intestinal
adhesion and wound infection postoperatively. The operating time
and hospital stay are also shortened. The complications occurring
after the surgical repair of Hirschsprung's disease can be categorized
into early and late complications. However, there is significant
overlap in regard to the time period during which these may occur
[4]. The early complications include wound infection, bleeding and
anastomotic complications as (leak, pelvic abcess, retraction of pullthrough
segment) [4].
The late complications are usually present within the first few
postoperative months. They include: enterocolitis, stricture and
constipation [5]. In another review of the patients undergoing
Swenson procedure, Kim et al. [6] noted that continence as Fecal
soiling has the greatest negative impact on the quality of life in
children with Hirschsprung`s disease, 12% of their patients less than
5 years of age had some degree of soiling, however between 10 and 15
years age its declined to only 6%. The incidence of soiling decreased
from 8% at 5 years old follow-up to less than 2% at 20 years old followup.
Finally, for post-operative Duhamel patients, they noted that only
5.3% showed evidence of soiling. Rates of fecal incontinence post
pull-through for HD ranges from 3% to 53% at long term follow-up
only 10.3% had fecal incontinence. The anorectal function are greatly
affected after the surgical treatment of the Hirschsprung`s disease.
It can be assessed clinically by interviews and questionnaires to the
patients and the parents. It also can be assessed by investigations as
endorectal ultrasound, anorectal manometer, Colonic transit time
and defecography [7]. The aim of this study is to evaluate the outcome
of transanal endorectal pull-through operation clinically and radio
logically in patient with Hirschsprung's disease.
Table 1
Figure 1
Figure 2
Figure 3
Patients and Methods
This prospective quasi-experimental cohort study was conducted
on 40 children with Hirschsprung's disease operated beyond 2 years,
in whom transanal endorectal pull-through was indicated.
Inclusion criteria
• Patients with histopathologically documented Hirschsprung
disease operated on by transanal endorectal pull-through in the
last 5 years.
• Transitional zone in the rectosegmoid colon (classic type of
Hirschsprung’s disease) diagnosed by contrast enema.
Exclusion criteria
• Patients operated in the last 2 years.
• Previous colorectal surgery for Hirschsprung’s disease other
than rectal biopsy.
• Associated congenital syndromes (e.g. Down syndrome).
• Neurological impairment (e.g. menengiomyelocoele).
Methods
For each patient, the following was done prior to the surgical
procedure:
• Full clinical history taking.
• Full physical examination: General condition, weight,
abdominal examination: abdominal distension, palpable colon,
and rectal examination.
• Laboratory investigations: CBC, coagulation profile, liver and
renal function tests and CRP.
• Radiological examination: Plain X-ray of the abdomen (erect
and supine) for suspected HAEC and Contrast [Barium or
Gastrograffin (GG)] enema.
• Rectal biopsy.
Evaluation criteria
• Age at presentation.
• Age at surgery.
• Associated major congenital anomalies.
• Defecation frequency per Day.
• Rectal sensation is persevered or not.
• Soiling of clothes in between defecation times.
• If incontinence present, It is for stool only, or flatus only or
both.
• Number of attacks of enterocolitis in general.
• Number of attacks of enterocolitis required hospital admission.
• Abdominal distension.
• Faecal Impaction.
• Perianal skin excoriation.
• Anal sphincter tone.
• Feeding.
Results
We followed up 40 pediatric patients with Hirschsprung’s
disease, in whom transanal endorectal pull-through was indicated.
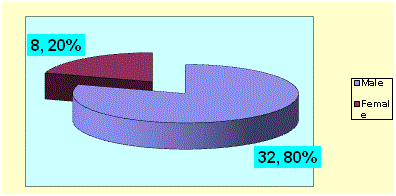
There were 32 males and 8 females. Mean age was 9.2 months (Figure
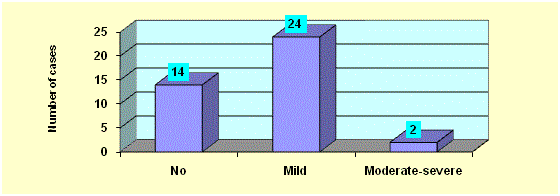
1 and Table 1). As regards abdominal distension, 14 cases showed
no distension, 24 cases showed mild distension and 2 cases showed
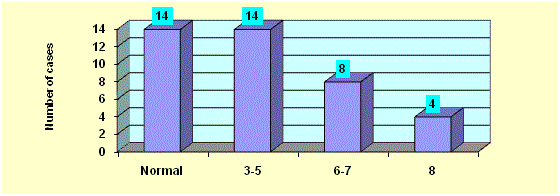
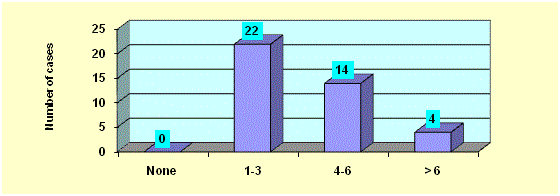
moderate to severe abdominal distension (Figure 2). Fourteen
patients (35%) had a normal defecation. Fourteen patients (35%)
had a frequency of defecation of 3-5 days. Eight patients (20%)
had a frequency of defecation of 6-7 days. Four patients (10%) had
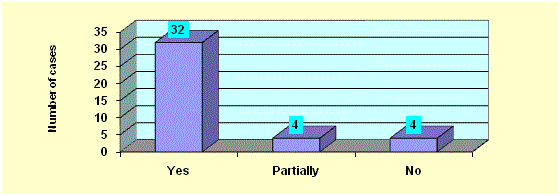
a frequency of defecation of 8 or more days (Figure 3). Thirty two
patients had true fecal continence and had a non-dilated colon on
contrast enema and a tendency to have diarrhea and did not respond
to medical treatment. Four patients had partial fetal incontinence and
no patients had incontinence (Figure 4).
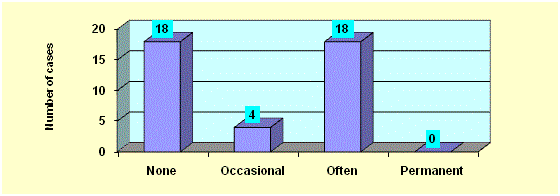
Postoperative soiling accidents were observed occasionally in 4
patients (10%), often in 18 patients (45%). Soiling was not observed
in 18 patients (45%) (Figure 5). Perianal skin excoriation was absent
in 36 patients (90%) and present in 4 patients only (10%) (Figure 6).
Rectal sensation was preserved in 30 patients (75%) (Figure 7).
Discussion
Hirschsprung's disease is one of the most common congenital
malformations, which occurs in 1:2000 to 5000 live births. There are
three ways that Hirschsprung's disease characteristically presents
neonatal bowel obstruction, chronic constipation, and enterocolitis
[8]. The treatment of Hirschsprung's disease is primarily surgical.
Surgical therapy for Hirschsprung's disease implies removal of
aganglionic bowel and bringing of normally innervated intestine to
the anus. Although all of the three most commonly performed basic
techniques for the correction of Hirschsprung's disease (Swenson,
Soave and Duhmel) accomplish this goal, the modified Soave operation
has the important advantage of helping to avoid injury to the pelvic
nerves responsible for urinary incontinence and sexual dysfunction
[9]. The use of transanal approach is relatively a new concept. The
risks of contamination and adhesion formation are eliminated. The
procedure does not damage the pelvic structures, is not expensive,
and has the most optimal cosmetic result [10]. The aim of this study
is to evaluate the outcome of transanal endorectal pull-through
operation clinically and radio logically in patient with Hirschsprung's
disease. The study was performed on 40 patients with Hirschsprung
disease operated on by transanal endorectal pull-through in the last 5
years. Zhang et al. [11] performed long-term follow up of 73 children
who had undergone surgical correction of Hirschsprung's disease
with transanal-one stage pull-through operation, of these children,
58 responded and 15 were lost to follow up; the losing rate was 20%.
We exclude patients with Hirschsprung's disease operated in the last
2 years. Fourteen patients (35%) had a normal defecation. Fourteen
patients (35%) had a frequency of defecation of 3-5 days. Eight
patients (20%) had a frequency of defecation of 6-7 days. Four patients
(10%) had a frequency of defecation of 8 or more days. Thirty two
patients had true fecal incontinence and had a non-dilated colon on
contrast enema and a tendency to have diarrhea and did not respond
to medical treatment. Four patients had partial fetal incontinence
and no patients had incontinence. As regards abdominal distension,
14 cases showed no distension, 24 cases showed mild distension and
2 cases showed moderate to severe abdominal distension. History
of previous attack of enterocolitis was positive in all cases. Hadidi
et al. [12] reported a 4.4% enterocolitis rate utilizing the transanal
approach in comparison to a 12% incidence in a preceding series of
open pull-through procedures. This is very low incidence of post pullthrough
enterocolitis which differs from most of studies reported in
the literature. The rate of enterocolitis varies widely in published
reports, from a higher rate of 54% by Van Leeuwen et al. [13] to a
lower rate of 4.55% in Zhang et al. [11] study of which may attribute
to criteria of enterocolitis used in different studies.
Postoperative soiling accidents were observed occasionally in 4
patients (10%), often in 18 patients (45%). Soiling was not observed
in 18 patients (45%). Soiling was observed at night in 16 patients
(40%) and at day and night in 6 patients (15%). Most episodes of
enterocolitis occur within the first two years after the pull-through
procedure. Engum et al. [14] have noted the infants that experience
enterocolitis before operative intervention have an increased risk
of occurrence of this complication following the pull-through
procedure. Zhang et al. [11] studied 58 patients who underwent
transanal pull-through operation for Hirschsprung's disease, the
results were soiling in 9 patients (15.5%) and constipation in 5 (8.6%)
and no incontinence was obtained in any patient. Indications for the
second pull-through include: retained or acquired aganglionosis,
severe stricture, dysfunctional bowel segment, marked dilation of the
bowel as a result of years of constipation, anocultaneous fistula, and
intestinal neuronal dysplasia (Gobran et al., 2007). El-Sawaf et al. [15]
studied 41 patients who underwent transanal pull-through operation
for Hirschsprung's disease, there was a 53.7% overall incidence of
post-pull-through enterocolitis. This higher rate of enterocolitis may
be because of low threshold in diagnosing early cases of enterocolitis.
Levitt et al. [16] reported that postoperative enterocolitis was more
frequent in patients who had enterocolitis before the pull-through
procedure. We explained that satisfaction of the parents with the
results is a subjective object varies with the socioeconomic levels of
the parents; their education and their residency (rural or urban).
Moreover, one other point deserving recognition is that, currently,
the purpose of the management of Hirschsprung's disease is not only
to ensure survival, but also to achieve normal bowel function and,
more importantly, to achieve and good quality of life in all possible
ways. Surgery is not the end of the treatment. We feel it is necessary to
emphasize the long-term regular follow up of patients after surgery for
Hirschsprung's disease because it is the prerequisite for improvement
of the quality of life. Strategies, including psychological counseling,
medication therapy, and toilet training, are needed.
Figure 4
Figure 5
Figure 6
Conclusion
• Transanal Endorectal Pull-Through (TEPT) is a good
technique for surgical correction of Hirschsprung's disease with few
operation-related complications.
• The transanal procedure needs a special experience and it
has to be born in mind that laparotomy may be resorted to any time if
any difficulty was encountered during the procedure.
• The clinical outcome is satisfactory.
• Many children with Hirschsprung's disease have a good
outcome following surgical treatment, but long-term follow-up
studies have identified a number of concerns.
• The predominant cause for persistent or recurrent
unresponsive obstructive symptoms after initial pull-through
procedure is incomplete resection of the transition zone.
• Fecal incontinence after operative management of
Hirschsprung's disease represents a serious problem.
• To avoid incontinence after transanal endorectal pullthrough,
we recommend the following: overstretching of anal canal,
very low colo-anal anastomosi, injury to sensory mucosa, injury to
mussels and inadequate resection of dilated colon.
• The majority of long-term follow-up studies have
concentrated only on the functional outcome.
• Although most patients had good or fair quality of life
after surgical correction for Hirschsprung's disease, the long-term
outcome and quality of life are not as good as surgeons expected.
• Satisfaction of the parents with the results is a subjective
object varies with the socioeconomic levels of the parents; their
education and their residency.
References
- Temple S, Shawyer AC, Langer JC. Is daily dilatation by parents necessary after surgery for Hirschsprung's disease and anorectal malformations? J Pediatr Surg. 2012;47(1):209-12.
- Sookpotarom P, Vejchapipat P. Primary transanal Swenson pull-through operation for Hirschsprung's disease. Pediatr Surg Int. 2009;25(9):767-73.
- Langer J, Caty M, de la Torre-Mondragon L, Georgeson K, Haddad M, Hutson J, et al. IPEG colorectal panel. J Laparoendosc Adv Surg Tech A. 2007;17(1):77-100.
- Teitelbaum DH, Caniano DA, Qualman SJ. The pathophysiology of Hirschsprung’s –associated enterocolitis: importance of histologic correlates. J Pediatr Surg. 1998;24(12):1271-7.
- Pastor AC, Osman F, Teitelbaum DH, Caty MG, Langer JC. Development of a standardized definition for Hirschsprung's-associated enterocolitis: A Delphi analysis. J Pediatr Surg. 2009;44(1):251-6.
- Kim AC, Langer JC, Aimee C, Zhang L, Sloots CE, Hamilton NA, et al. Endorectal pull-through for Hirschsprung's disease-a multicenter, long-term comparison of results: transanal vs transabdominal approach. J Ped Surg. 2010;45(6):1213-20.
- Dasgupta R, Langer JC. Evaluation and management of persistent problems after surgery for Hirschsprung's disease in a child. J Pediatr Gastroenterol Nutr. 2008;46(1):13-19.
- Langer J, Oldham K, Keith T. Principles and practice of pediatric surgery, 4th ed. Section II: Surgical practice. Part E: Colon. Chapter 86: Hirschsprng's Disease. 2005;2.
- Ekema G, Falchetti D, Torri F, Merulla VE, Manciana A, Caccia G. Further evidence on totally transanal one-stage pul-through procedure for Hirschsprung's disease. J Pediatr Surg. 2003;38(10):1434-9.
- Langer J, Durrant A, de la Torre L, Teitelbaum DH, Minkes RK, Caty MG, et al. One-stage transanal Soave pull-through for Hirschsprung's disease: A multicenter experience with 141 children. Ann Surg. 2003;238(4):569-85.
- Zhang S, Bai Y, Wang W, Wang WL. Clinical outcome in children after transanal one-stage endorectal pull-through operation for Hirschsprung's disease. J Pediatr Surg. 2005;40(8):1307-11.
- Hadidi A. Transanal endorectal pull-through for Hirschsprung’s disease: a comparison with the open technique. Eur J Pediatr Surg. 2003;13(3):176-80.
- Van Leeuwen K, Geiger J, Barnett L, Coran AG, Teitelbaum DH. Stooling and manometric findings after primary pull-through in Hirschsprung's disease: Perineal versus abdominal approaches. J Pediatr Surg. 2002;37(9):1321-5.
- Engum G, Grosfeld E. Long-term results of treatment: Seminars in pediatric surgery. 2004;13(4).
- El-Sawaf M, Drongowski R, Chamberlain J, Coran AG, Teitelbaum DH. Are the long-term results of the trnsanal pull-through equal to those of the transabdominal pull-through? J Pediatr Surg. 2007;42(1):41-7.
- Levitt M, Martin C, Olesevich M, Bauer CL, Jackson LE, Peña A. Hirschsprung's diseased and fecal incontinence: Diagnostic and management strategies. J Pediatr Surg. 2009;44(1):271-7.