Research Article
Long-term Quality of Life and Chronic Pain after Inguinal Hernia Repair in Women
Raphael N Vuille-dit-Bille1, Lukas Fink2, Svenja Leu1, Christopher Soll1, Peter Villiger3 and Ralph F Staerkle*1
1Department of Surgery, Cantonal Hospital Winterthur, Winterthur, Switzerland
2Department of Mathematics, Cantonal School of Wil, St. Gallen, Switzerland
3Department of Surgery, Cantonal Hospital Chur, Chur, Switzerland
*Corresponding author: Ralph Staerkle, Department of Surgery, Kantonsspital Winterthur, Brauerstrasse 158401 Winterthur, Switzerland
Published: 12 Jul, 2018
Cite this article as: Vuille-dit-Bille RN, Fink L, Leu S, Soll
C, Villiger P, Staerkle RF. Long-term
Quality of Life and Chronic Pain after
Inguinal Hernia Repair in Women. Clin
Surg. 2018; 3: 2007.
Abstract
Background: Groin hernias in women are rare and most published studies only assess different
operation techniques and the associated recurrence rates. Information about chronic postoperative
pain and quality of life following groin hernia repair in women is sparse.
Methods: In total, 24 female patients following groin hernia repair were included in this prospective
study. Median follow-up was 6.25 years. The Core Outcome Measure Index (COMI) hernia
questionnaire was used to assess quality of life and chronic postoperative pain.
Results: The COMI-hernia total score and COMI-hernia pain score both decreased significantly after
surgery (p=0.00018 and p=0.0095, respectively). Both scores correlated with patients’ satisfaction.
High preoperative COMI-hernia total score and low American Society of Anaesthesiologists (ASA)
score were identified as risk factors for an adverse outcome after surgery. Similarly, low ASA score
was shown as a risk factor for postoperative high COMI-hernia pain score.
Conclusions: Risk factors for adverse outcome after groin hernia repair seem to be different between
males and females. Patient’s fitness prior to surgery seems to inversely correlate with outcome after
groin hernia repair in females.
Keywords: Inguinal hernia repair; Quality assessment; Quality of life; Chronic pain; Core outcome measure index; Patient satisfaction
Introduction
Groin hernia repair is one of the most frequently performed operations in general surgery and
the majority of affected patients are males [1]. Only 8% of all groin hernia repairs are performed in
females [2], and outcome data after groin hernia repair in women are relatively rare [3]. There are
important differences between groin hernias in women and men. Groin hernias are less common in
women with an incidence of 0.3% compared to 2-5% in men [4]. Femoral hernias account for about
one third of all groin hernias in females compared to only 2.4% in males [4]. This may be explained
by anatomical differences in the inguinal region between males and females [5].
These differences could imply that treatment in women may have to be different from treatment
in men. However, the optimal treatment of groin hernias in women remains controversial [6]. There
have not been any systematic reviews or randomized controlled trials, which deal exclusively with
the treatment of groin hernias in women. The European Hernia Society recommends to perform a –
preferably endoscopic - preperitoneal repair in women due to the high frequency of femoral hernias
[7]. This recommendation is mainly based on two epidemiological studies from national databases
and therefore the grade of recommendation is low (D) [3,8]. The vast majority of published
studies about groin hernia repair in women compare different surgical techniques and assess the
concomitant recurrence rate as primary outcome [3,4,8-13]. Also the latest international guidelines
from Hernia Surg group recommend a preperitoneal repair in women [14].
However, since the routine use of mesh in groin hernia repair in adults, the recurrence rates
are considerably low (around 0.5%) [15]. Furthermore, female gender has been identified as risk
factor for chronic postoperative pain following groin hernia repair [7,13]. From the view of the
patients, chronic inguinal pain impairing quality of life (QOL) reflects the most relevant adverse
outcome after groin hernia repair [16]. Published studies about QOL following groin hernia repair
are difficult to compare, since different tools are used to assess these
outcomes [17]. We recently proposed the Core Outcome Measure
Index-hernia (COMI-hernia) as such an instrument [18] and have
already reported on its utility and reliability in a large cohort of male
patients [19].
There is a lack of prospectively assessed, long-term follow-up
data, evaluating chronic inguinal pain and QOL following groin
hernia repair in women. Therefore, the primary aim of this study was
to prospectively assess QOL and chronic postoperative pain following
groin hernia repair in females using the COMI-hernia. The secondary
goal was to identify risk factors for adverse COMI-hernia scores.
Figure 1
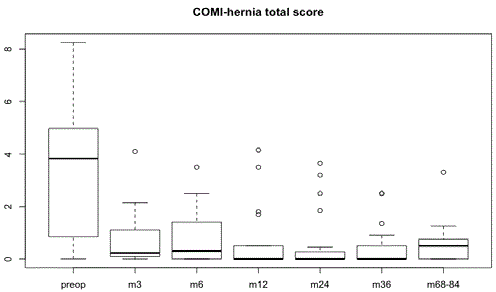
Figure 1
Boxplot of COMI-hernia total scores preoperatively (preop), after 3
months (m3), 6 months (m6), 12 months (m12), 24 months (m24), 36 months
(m36), and after 68-84 months (m68-84).
Solid line = median, box limits = 25th and 75th percentiles, whiskers = 1.5x
interquartile range (IQR), circles = maximum observations.
Figure 2
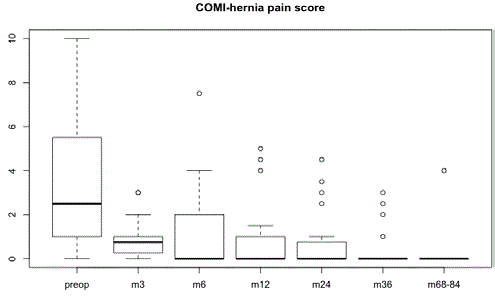
Figure 2
Boxplot of COMI-hernia pain scores preoperatively (preop), after
3 months (m3), 6 months (m6), 12 months, 24 months (m24), 36 months
(m36), and after 68-84 months (m68-84).
Solid line = median, box limits = 25th and 75th percentiles, whiskers = 1.5x
interquartile range (IQR), circles = maximum observations.
Materials and Methods
The study has been approved by the local ethics committee
in Zurich (Switzerland) on January 29, 2009 (Chairperson Prof
R Maurer, protocol number 22/08). All patients have given their
informed consent for participation in this study. Patients were
treated at four different Swiss institutions: Cantonal Hospital of
Graubuenden, Hospital Maennedorf, Hospital Ilanz, and Hospital
Grabs.
The inclusion criteria were as follows: ≥ 18 years of age, female
gender, and diagnosis of primary groin hernia. Exclusion criteria
were defined as emergent hernia repair (i.e. due to incarceration),
recurrent hernia, and previous groin radiation. Each included patient
completed seven questionnaires (before, as well as 3, 6, 12, 24, 36, and
68 to 84 months after surgery).
Questionnaire
The COMI questionnaire was initially developed to assess chronic
back pain [20]. Subsequently, it was adapted to assess chronic pain and
QOL after groin hernia repair [18]. Briefly, it assesses the following
domains: pain, function, quality of live, symptom-specific well-being,
work and social disability by using a graphic rating scale ranging from
0 to 10 (pain) or from 0 to 5, with higher scores representing a worse
QOL and increased pain.
Operative technique
Surgeries included open repair (Lichtenstein), as well as minimal
invasive techniques (Transabdominal Preperitoneal (TAPP) and
Total Extra Peritoneal (TEP) inguinal hernia repair). Surgeries were
performed according to the surgeon’s preference. Lightweight, large
pore meshes were used in all cases. All surgeries were performed under
the guidance of a board-certified surgeon or by himself. To assess
these putative confounding factors, surgical technique (i.e. minimal
invasive versus open) and surgeon’s experience were included in a
linear regression analysis assessing risk factors for adverse COMIhernia
scores.
Statistics
Results are represented as median and range or as mean and
Standard Deviation (SD). The following statistical tests were
performed: Friedman rank sum test with post-hoc Wilcoxon signed
rank tests (for COMI-hernia total and COMI-hernia pain scores over
time). Risk factors for high postoperative COMI-hernia scores were
assessed using linear regression analysis with patient’s satisfaction
being analysed as metric data. P-values of less than 0.05 were
considered significant. The open source statistical program R was
used for analysis. (http://www.R-project.org/).
Figure 3
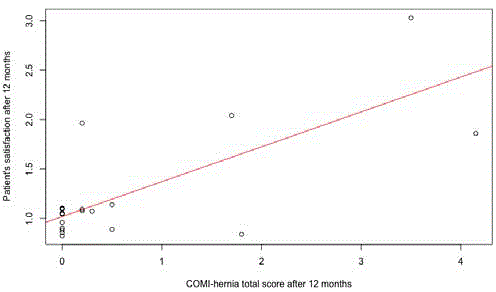
Figure 3
Patients’ satisfaction versus COMI-hernia total score (after 12
months).
R2=0.6034, p=0.00003455, coeff: 0.35255
Figure 4
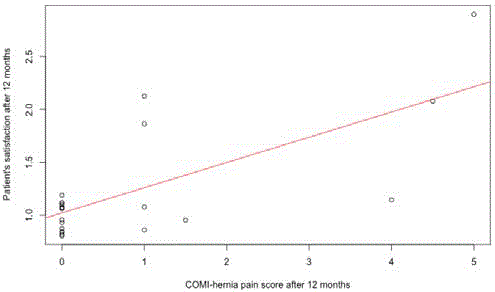
Figure 4
Patients’ satisfaction versus COMI-hernia pain score (after 12
months)
R2=0.4954, p=0.0002571, coeff: 0.238
Table 1
Results
Patients’ data
Twenty-four female patients with 26 hernias (two bilateral
hernias) were included in this study. Patients’ ages ranged from 18 to
83 years (median: 50 years). Nineteen patients (79%) had minimally
invasive procedures. All patients had primary hernias. Median
operation time was 53 min, ranging from 30 to 130 min. Median
follow-up was 75 months, ranging from 68 to 84 months. Drop-out
rates were 0% after 3 months, 8% after 6 and 12 months, 21% after 2
years, 29% after 3 years, and 21% after 75 months respectively (Table
1).
COMI-hernia total scores over time
COMI-hernia total scores were significantly lower following
surgery (preoperative COMI-hernia total score of 3.24 versus COMIhernia
total score of 0.7 after 3 months: p=0.00018) (Figure 1 and
Table 2). There were no differences among post-operative COMIhernia
total scores comparing the following time points: 3 months
versus 6 months (p=0.53), 6 months versus 12 months (p=0.52), 12
months versus 24 months (p=0.45), 24 months versus 36 months
(p=0.50), and 36 months versus 68 to 84 months (p=0.32) respectively.
The highest postoperative COMI-hernia total score was observed
after 6 months and the lowest after 3 years. Multivariate analysis was
performed using the data from 12 months postoperatively.
COMI-hernia pain scores over time
COMI-hernia pain scores were likewise significantly lower
following surgery (mean: 0.90) when compared to preoperative
values (mean: 2.83) (p=0.0095) (Figure 2 and Table 3). Comparing
3 months versus 6 months (p=0.54), 6 months versus 12 months
(p=0.48), 12 months versus 24 months (p=0.76), 24 months versus
36 months (p=0.55), and 36 months versus 68 to 84 months (p=0.15),
COMI-hernia pain scores were not different. Similarly, as for COMIhernia
total scores, highest postoperative COMI-hernia pain scores
were seen after 6 months and lowest after 68 to 84 months. As for
COMI-hernia total scores, linear regression analysis was performed
using the data from 12 months postoperatively.
Risk factors for high postoperative (12 months
postoperatively) COMI-hernia total scores
Ten variables were included in the multivariate analysis assessing
risk factors for high postoperative COMI-hernia total scores (at 12
months after surgery): American Society of Anaesthesiologists (ASA)
score, Body Mass Index (BMI), surgeon’s experience (i.e. number
of executed hernia surgeries), age, type of anesthesia (i.e. general vs.
spinal vs. local), surgical technique (i.e. laparoscopic vs. open), side
of the hernia (i.e. unilateral vs. bilateral disease), hernia type (i.e.
femoral vs. inguinal), operation time, and preoperative COMI-hernia
total score. High preoperative COMI-hernia total score (p=0.045)
and low ASA score (p=0.045) were identified as risk factors for
high postoperative COMI-hernia total scores. Patients’ satisfaction
correlated with COMI-hernia total score (12 months postoperative
time point used for analysis) (Figure 3) (R2=0.6034, p=0.00003455,
coefficient: 0.35255).
Risk factors for high postoperative (12 months
postoperatively) COMI-hernia pain scores
The identical 10 putative risk factors for high postoperative COMIhernia
pain scores were tested with the exception of preoperative
COMI-hernia pain score instead of preoperative COMI-hernia total
score. Only low ASA score (p=0.038) was identified as a risk factor
for high postoperative COMI-hernia pain scores (Table 4). Similarly,
as for COMI-hernia total score, patients’ satisfaction correlated with
COMI-hernia pain score (12-month postoperative time point used
for analysis) (Figure 4) (R2=0.4954, p=0.0002571, coefficient: 0.238).
Table 2
Table 3
Table 4
Discussion
To our knowledge, this is the first study, which prospectively
assesses chronic postoperative pain and long-term quality of
life following groin hernia repair in women using a validated
questionnaire. Additionally, this study aimed to identify risk factors
for an adverse outcome. QOL increased and chronic postoperative
pain decreased significantly after groin hernia repair in woman
measured with the COMI-hernia score (COMI-hernia total
p=0.00018; COMI-hernia pain p=0.0095). No significant differences
among postoperative COMI-hernia total and pain scores were
observed between different time points assessed with highest scores
seen 6 months postoperatively. Whereas COMI total scores remained
about the same over time with similar levels after 68-84 months
as e.g. after 12 months, COMI pain scores continuously (but nonsignificantly)
decreased over time. This finding is important especially
in the context of patients presenting with early postoperative pain. In
our cohort of patients, a high preoperative COMI-hernia total score
was identified as risk factor for high postoperative COMI-hernia total
scores. Furthermore, both, COMI-hernia total and pain score were
indirectly correlated with patients’ satisfaction. These two findings
are in line with our results from a recently published male cohort and
reflect the validity of the COMI-hernia score [19].
A low ASA score was the only identified risk factor for a high
postoperative COMI-hernia pain score. Young age, which is an
accepted risk factor for an adverse outcome after groin hernia repair
in males, did not correlate with a high COMI-hernia total or high
COMI-hernia pain score. This is in contrast to our recently published
male cohort.19 One could argue that a low ASA score is mostly found
in young and healthy patients and this argument could support
our finding. However, a low ASA score is a statistically significant
finding for an adverse outcome in our study, but the result is probably
clinically irrelevant. The reason for this finding could be based on the
small sample size and the fact that 96% of the patients had an ASA I
or II score.
It has to be taken into consideration that women may have
different risk factors for an adverse outcome after groin hernia repair
then men. Unfortunately, our prospective series is too small to answer
this question definitively.
Long-term follow-up in the present study was 79%. This might
reflect that the COMI-hernia Questionnaire is short and easy to
understand for patients. Furthermore, pre- and postoperative values
may be compared [18,19,21]. This makes the COMI-hernia – at
our opinion - preferable over other scores such as e.g. the Inguinal
Pain Questionnaire which is longer (18 items) and only made for
postoperative assessment [22].
Only a few studies focus exclusively on the treatment and
outcome of groin hernia repair in women. Historically, there have
been some large studies on groin hernia repair in women, which were
mainly published by the Shouldice Clinic [23-29]. More recently, two
larger studies from national databases were published evaluating the
outcome after groin hernia repair in women [3,8]. The main outcome
of these recently published studies was the recurrence rate after
different surgical approaches [3,4,8-10,12,30].
The strengths of this study are the prospective study design and
thus reduction of bias in comparison to most analogue studies that
were performed retrospectively. A further strength is represented
through the long-term and frequently performed follow-ups together
with a relatively low dropout rate.
An obvious limitation of the current study is the low number
and heterogeneous treatment of patients. This problem is due to the
low incidence of groin hernias in women and the prospective study
design. Limiting included patients to minimal invasive or open repair
only would have further decreased the number of study participants.
To address this issue and to estimate the impact of other possible
confounding factors (such as patients’ BMI, hernia type, etc.), these
variables were evaluated in a multivariate analysis assessing risk
factors for adverse outcome following groin hernia repair in women.
Type of surgery had no effect on patients’ outcome in our cohort
of patients. This finding does not match with two published studies
showing that an open anterior repair was associated with a higher
incidence of postoperative pain compared with women undergoing a
laparoscopic, total extraperitoneal repair [10,11].
Despite high preoperative COMI-hernia total and low ASA
scores, none of the assessed risk factors correlated with an adverse
outcome in the present study. It is questionable if accepted risk factors
for males such as open repair, younger age, preoperative pain, early
postoperative pain cannot be transferred one-to-one to females due to
the different entity of female groin hernias (different anatomy, more
femoral hernias, etc.) [31], or if our study was underpowered to show
these effects. Further prospective trials are needed to assess quality of
life and chronic pain in females after groin hernia repair. Due to the
relative rareness of groin hernias in women, these studies should be
done as multicentre trials. The COMI-hernia reflects a valuable and
easy tool to assess patient outcome following groin hernia repair and
should be used for such trials.
Conclusion
Non-of the known risk factors for adverse outcome (concerning quality of life and chronic pain) following groin hernia repair in males (such as young age, open repair, etc.) seem to affect the outcome in females. High quality prospective trials are needed to assess quality of life and chronic pain after groin repair in women to identify riskfactors for an adverse outcome in women.
Acknowledgment
The authors thank Angela Munson for language editing of the manuscript.
References
- Bay-Nielsen M, Kehlet H, Strand L, Malmstrøm J, Andersen FH, Wara P, et al. Quality assessment of 26,304 herniorrhaphies in Denmark: a prospective nationwide study. Lancet. 2001;358(9288):1124-8.
- Nilsson E, Kald A, Anderberg B, Bragmark M, Fordell R, Haapaniemi S, et al. Hernia surgery in a defined population: a prospective three year audit. Eur J Surg. 1997;163(11):823-9.
- Bay-Nielsen M, Kehlet H. Inguinal herniorrhaphy in women. Hernia. 2006;10(1):30-3.
- Schouten N, Burgmans JP, van Dalen T, Smakman N, Clevers GJ, Davids PH, et al. Female 'groin' hernia: totally extraperitoneal (TEP) endoscopic repair seems the most appropriate treatment modality. Hernia. 2012;16(4):387-92.
- Rosen A, Nathan H, Luciansky E, Orda R. The inguinal region: anatomic differences in men and women with reference to hernia formation. Acta Anat (Basel). 1989;136(4):306-10.
- Bendavid R. Inguinal herniorrhaphy in women. Hernia. 2006;10(1):103-4.
- Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, et al. European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia. 2009;13(4):343-403.
- Koch A, Edwards A, Haapaniemi S, Nordin P, Kald A. Prospective evaluation of 6895 groin hernia repairs in women. Br J Surg. 2005;92(12):1553-8.
- Ashfaq A, McGhan LJ, Chapital AB, Harold KL, Johnson DJ. Inguinal hernia repair in women: is the laparoscopic approach superior? Hernia. 2014;18(3):369-73.
- Kark AE, Kurzer M. Groin hernias in women. Hernia. 2008;12(3):267-70.
- Lau H, Patil NG, Yuen WK. Is endoscopic totally extraperitoneal hernioplasty justified for the repair of groin hernia in female patients? Surg Endosc. 2005;19(12):1544-8.
- Thairu NM, Heather BP, Earnshaw JJ. Open inguinal hernia repair in women: is mesh necessary? Hernia. 2008;12(2):173-5.
- Tolver MA, Strandfelt P, Rosenberg J, Bisgaard T. Female gender is a risk factor for pain, discomfort, and fatigue after laparoscopic groin hernia repair. Hernia. 2013;17(3):321-7.
- HerniaSurge G. International guidelines for groin hernia management. Hernia. 2018;22(1):1-165.
- Gopal SV, Warrier A. Recurrence after groin hernia repair-revisited. Int J Surg. 2013;11(5):374-7.
- Kurzer M, Kark AE, Hussain T. Hernia repair: Outcomes other than recurrence should be analysed. BMJ. 2008;336(7652):1033.
- van Hanswijck de Jonge P, Lloyd A, Horsfall L, Tan R, O'Dwyer PJ. The measurement of chronic pain and health-related quality of life following inguinal hernia repair: a review of the literature. Hernia. 2008;12(6):561-9.
- Staerkle RF, Villiger P. Simple questionnaire for assessing core outcomes in inguinal hernia repair. Br J Surg. 2011;98(1):148-55.
- Staerkle RF, Vuille-Dit-Bille RN, Fink L, Soll C, Villiger P. Chronic pain and quality of life after inguinal hernia repair using the COMI-hernia score. Langenbecks Arch Surg. 2017;402(6):935-47.
- Mannion AF, Elfering A, Staerkle R, Junge A, Grob D, Semmer NK, et al. Outcome assessment in low back pain: how low can you go? Eur Spine J. 2005;14(10):1014-26.
- Mommers EHH, Hunen DRM, van Hout J, Guit M, Wegdam JA, Nienhuijs SW, et al. Patient-reported outcomes (PROs) after total extraperitoneal hernia repair (TEP). Hernia. 2017;21(1):45-50.
- Fränneby U, Gunnarsson U, Andersson M, Heuman R, Nordin P, Nyrén O, et al. Validation of an Inguinal Pain Questionnaire for assessment of chronic pain after groin hernia repair. Br J Surg. 2008;95(4):488-93.
- Bendavid R. Femoral hernias: primary versus recurrence. Int Surg. 1989;74(2):99-100.
- GLASSOW F. Inguinal hernia in the female. Surg Gynecol Obstet. 1963;116:701-4.
- GLASSOW F. RECURRENT INGUINAL AND FEMORAL HERNIA: 3000 CASES. Can J Surg. 1964;7:284-8.
- Glassow F. Femoral hernia in the female. Can Med Assoc J. 1965;93(26):1346-50.
- Glassow F. Bilateral hernias in the female. Can Med Assoc J. 1969;101(9):66-8.
- Glassow F. Inguinal and femoral hernia in women. Int Surg. 1972;57(1):34-6.
- Glassow F. The surgical repair of inguinal and femoral hernias. Can Med Assoc J. 1973;108(3):308-13.
- Federmann G, Brauckmann M. Inguinal herniorrhaphy in women: should the mesh be implanted preperitoneal? Hernia. 2007;11(2):203.
- Miserez M, Peeters E, Aufenacker T, Bouillot JL, Campanelli G, Conze J, et al. Update with level 1 studies of the European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia. 2014;18(2):151-63.