Research Article
Low Incidence Complication with Anteromedial Angiosome Based Approach to Total Ankle Arthroplasty: A Retrospective Analysis of 27 Cases
Edgardo Rodriguez-Collazo1* and Joseph Agyen2
*Corresponding author: Edgardo Rodriguez-Collazo, Department of Surgery, Director Chicago Foot & Ankle Deformity Correction Center, Illizarov Correction & Microsurgical Limb Reconstruction Presence Saint Joseph Hospital, Chicago, USA
Published: 28 Jun, 2018
Cite this article as: Rodriguez-Collazo E, Agyen J.
Low Incidence Complication with
Anteromedial Angiosome Based
Approach to Total Ankle Arthroplasty:
A Retrospective Analysis of 27 Cases.
Clin Surg. 2018; 3: 2000.
Abstract
Background: Classical anterior approach to total ankle arthroplasty has been associated with high
rate of wound healing complications. High complication rates have been due to poor tissue handling
by surgeon or poor patient selection. Orthoplastic angiosome based approach would be to place the
incision between two angiosomes for ideal wound healing. Here we describe a novel anteromedial
orthoplastic dissection approach with low incidence of complications.
Method: We reviewed medical charts of 27 patients who underwent anteromedial total ankle
arthroplasty approach. We evaluated charts for wound healing complications, patient age, comorbidities
and when passive and active ankle range of motion initiated from the day of surgery.
Results: We found one out of 27 patients (3.7%) had wound healing complications. This patient
required surgery for soft tissue coverage. Five out of the 27 (18.5%) patients were noted to be
type II diabetic. We did not observe a correlation between diabetes as co-morbidity and wound
complication.
Conclusion: Anteromedial orthoplastic angiosome based dissection approach for total ankle
arthroplasty is associated with low wound healing complications. This is very valuable in patients
with poor tissue envelope from prior surgery or injuries as well as in patients with co-morbidities
such as diabetes and inflammatory pathologies which have been shown to increase post operative
complications with total ankle arthroplasty.
Keywords: Total ankle replacement; Anteromedial ankle; Orthoplastic; Total ankle arthroplasty
Introduction
Classical anterior approach to Total Ankle Arthroplasty (TAA) has been met with high wound
healing complications rates. In modern studies these have varied as high as 36% of wound healing
complications [1-6]. Despite wound healing complication rates total ankle replacement have
gained in popularity in the past decade due to advanced surgical technique and improved implant
technology. The classic anterocentral approach allows for excellent visualization and maximal
placement of implants. However perforator arteries arising from anterior tibial and dorsalis pedis
arteries have to be sacrificed with this approach. Incision healing occurs through choke vessels
which open up due to retrograde flow when perforator vessels are not functional. Ian Taylor first
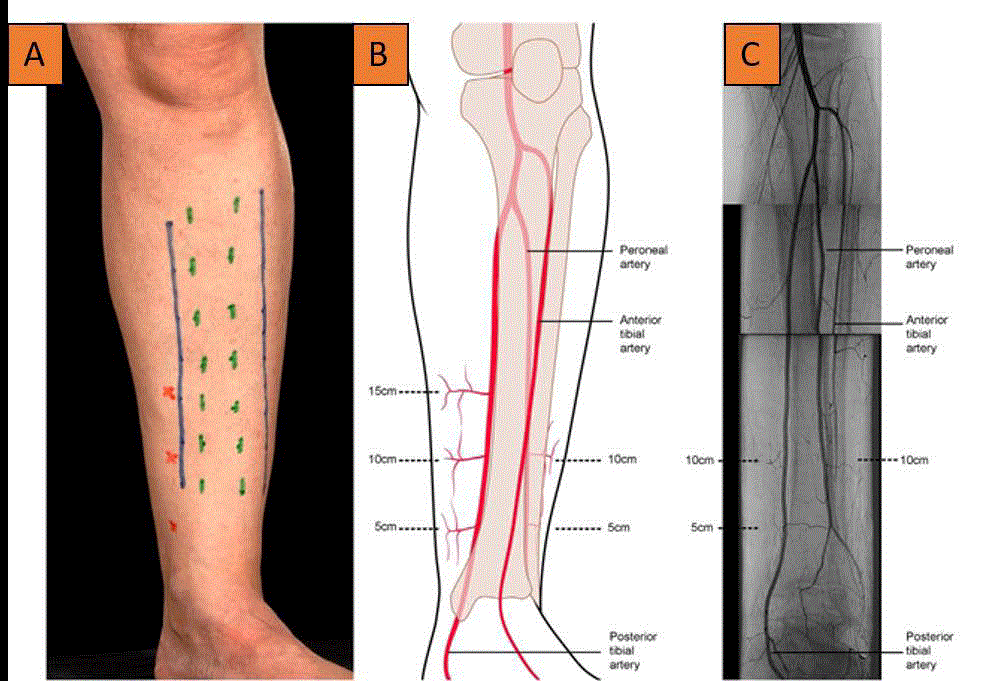
described foot and ankle angiosomes [7,8]. Figure 1 shows angiosome, perforator vessel and choke
vessel anatomy [9]. The safest incision placement is at the junction of two angiosomes which are
anterior tibial and posterior tibial angiosomes at the ankle joint level [10,11].
Wound healing complications associated with classical anterocentral approach have been
attributed to poor tissue handling, poor patient selection and longer operative time. Many studies
have shown diabetes, smoking and increased operative time to be associated with high post-operative
complications [12,13]. Incisional Negative Pressure Wound Therapy (NPWT) and compression
dressings as well as other novel dressing modalities including continuous external tissue expander
have been employed to improve wound healing potential after TAA [14-16]. However there have not
been any studies to our knowledge that has evaluated effects of perforator arteries in tissue healing
for total ankle arthroplasty or ankle arthrodesis. We hypothesized that leaving perforators intact by
anteromedial dissection instead of standard anterocentral incision for total ankle arthroplasty will
result in fewer wound healing complications.
Table 1
Table 1
Shows co-morbidities, implant used, days when active and passive ankle range of motion was initiated.
Methods
Chart review
We retrospectively evaluated medical charts of all patient that
underwent anteromedial total ankle arthroplasty approach for any
wound complications, co-morbidities, days from initial surgery
till range of motion was initiated and infection rate. We found 28
patients who underwent this approach between 2012 and 2017.
Surgical approach
Patient was placed in supine position and underwent general
anesthesia. All patients received popliteal and saphenous nerve
block prior to surgery and thigh tourniquet was employed. Doppler
examination was performed pre operatively in all patients and
perforator vessels were identified and marked. Incision was placed
over the medial border of anterior tibialis tendon and curved medially
distally. Tibialis anterior tendon sheath was incised and tibialis anterior
tendon was retracted medially or laterally as needed. Neurovascular
bundle was retracted laterally. The floor of the tibialis anterior tendon
was identified and full thickness incision was placed over the ankle
joint. Cobb elevator was used to reflect capsular and periosteal
fibers and ankle joint was exposed (Figure 2). Ankle arthroplasty
with appropriate implant was performed as per the guidelines of
the respective implant. Skin closure was performed with absorbable
suture for deep and subcutaneous tissue and non-absorbable suture
or skin staples were used for skin closure. All patients were placed in
a posterior splint with ankle in neutral position.
Post operative course
All patients were placed in a posterior splint with ankle in neutral
position. Patients were kept non weight bearing for six weeks. Patients
were transitioned in to Controlled Ankle Motion (CAM) boot at one
week. Sutures or staples were removed at two weeks. Passive ankle
range of motion was initiated at 1 to 3 weeks post operatively and
active range of motion was allowed at 3 to 4 weeks post operatively
depending on clinical evaluation. Physical therapy was initiated at
approximately 3 weeks post operatively.
Results
We found one out of 27 (3.7%) patients who developed wound
dehiscence and required repeat surgery for debridement and skin
graft. One patient with wound complications required free flap with
split thickness skin graft. No other incidences of wound complications
were noted. We did not find any incidences of superficial or deep
infections.
Patients were allowed passive range of motion between 1 to 3
weeks with an average of 8 days and active ankle range of motion
between 2 to 4 weeks with an average of 21 days except the two
patients with wound healing complications. Of note six patients
had type 2 diabetes mellitus. Patient age ranged between 45 and 76
years with an average of 62.26 years. We did not see any correlation
between co-morbidities such as diabetes and wound complications in
our study. Patient with wound complications did not have diabetes
mellitus.
Figure 1
Figure 2
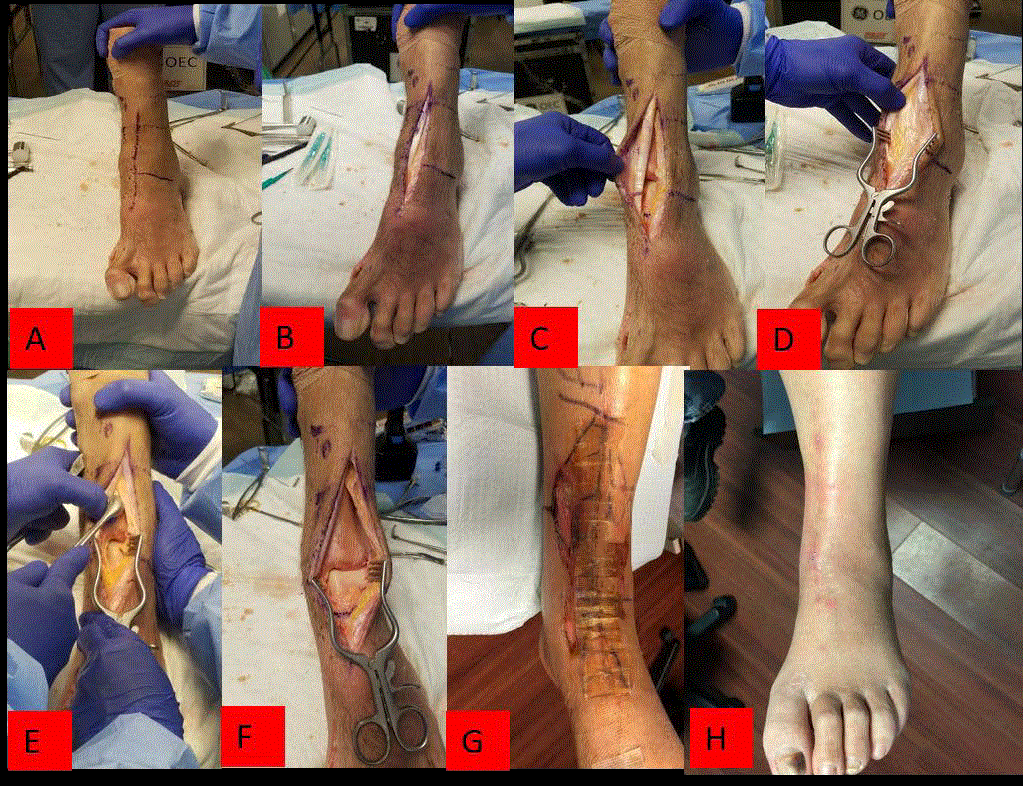
Figure 2
Cobb elevator was used to reflect capsular and periosteal fibers and ankle joint was exposed.
Discussion
Classical anteriocentral approach to ankle arthrodesis, pilon
fracture or total ankle arthroplasty allows for excellent visualization of
ankle joint however high incidences of wound healing complications
have been found in many studies. Many factors dictate wound
healing including patient’s co-morbidities such as peripheral artery
disease, inflammatory pathologies, smoking and diabetes [5,6,12,13].
Soft tissue healing is greatly compromised in acute trauma such
as high energy pilon fracture or history of previous such injury
requiring surgery. Surgeon’s tissue handling has been attributed to
poor wound healing rates. We believe sacrificing perforators during
the anterocentral approach is factor leading to such high wound
complication rates as choke vessels needed for central incision healing
do not readily open up until two to three weeks.
Superficial and minor wounds can be managed with modalities
such as compression therapy, negative pressure wound therapy,
wound care and split thickness skin graft [12,13]. However
avoiding any wound complications is most ideal. Complex wounds
arising from anterocentral surgical approach can have devastating
consequences for the patient. Soft tissue coverage in this region of the
lower extremity remains a challenge for the orthopedic and plastic
surgeon to this day. Free flaps and perforator pedicle flaps are the
mainstay for achieving wound closure for anterior ankle wounds that
are not amenable to local wound care [12].
Detailed knowledge of the angiosome of the foot and ankle is
needed for the best surgical technique. Perforators arise from anterior
tibial, peroneal and posterior tibial artery at approximately 5 cm,
10 cm and 15 cm from the ankle joint. (Figure 1) [9]. Orthoplastic
approach dictates that we respect these vessels not only for best
outcomes but also for potential muscle or fasciocutaneous flap
that may be needed should the wound complications arise. The
safest placement of incision is at two angiosome borders [10]. We
believe our anteromedial approach gives us adequate exposure for
arthroplasty and implant insertion as well as preserve perforator
vessels. This is of great value especially in compromised hosts with
multiple co-morbidities.
Limitations of our study include retrospective nature of it and lack
of a control group. Prospective randomized studies would give us a
better power to conclude if anteromedial approach decreases wound
healing complications for total ankle arthroplasty or arthrodesis. This
however does not detract from clinical importance of knowledge of
perforator and angiosome anatomy for incision planning prior of any
major foot and ankle surgery.
References
- Glazebrook MA, Arsenault K, Dunbar M. Evidence-based classification of complications in total ankle arthroplasty. Foot Ankle Int. 2009;30(10):945-9.
- Gougoulias N, Khanna A, Maffulli N. How successful are current ankle replacements. A systematic review of the literature. Clin Orthop Relat Res. 2010;468(1):199-208.
- Matsumoto T, Parekh SG. Use of negative pressure wound therapy on closed surgical incision after total ankle arthroplasty. Foot Ankle Int. 2015;36(7):787-94.
- Myerson MS, Shariff R, Zonno AJ. The management of infection following total ankle replacement: demographics and treatment. Foot Ankle Int. 2014;35(9):855-62.
- Raikin SM, Kane J, Ciminiello ME. Risk factors for incision healing complications following total ankle arthroplasty. J Bone Joint Surg Am. 2010;92(12):2150-5.
- Whalen JL, Spelsberg SC, Murray P. Wound breakdown after total ankle arthroplasty. Foot Ankle Int. 2010;31(4):301-5.
- Taylor GI, Palmer JM. The vascular territories (angiosomes) of the body: experimental study and clinical observations. Br J Plast Surg. 1987;40:113-41.
- Taylor GI, Pan WR. Angiosomes of the leg: anatomic study and clinical implications. Plast Reconstr Surg. 1998;102(3):599-616.
- Nanchahal J, Nayagam S, Khan U, Moran C, Barrett S, Sanderson F, et al. Standards for the management of open fractures of the lower extremity. 2009.
- Attinger C, Cooper P, Blume P, Bulan E. The safest surgical incisions and amputations applying the angiosome principles and using the Doppler to assess the arterial-arterial connections of the foot and ankle. Foot Ankle Clin. 2001;6(4):745-99.
- Attinger CE, Evans KK, Bulan E, Blume P, Cooper P. Angiosomes of the foot and ankle and clinical implications for limb salvage: reconstruction, incisions, and revascularization. Plast Reconstr Surg. 2006;117(7):261S -93S.
- Avashia Y, Shammas RL, Mithani SK, Parekh SG. Soft tissue reconstruction after total ankle arthroplasty. Foot Ankle Clin. 2017;22(2)391-404.
- Lampley A, Gross CE, Green CL, De Orio JK, Easley M, Adams S, et al. Association of cigarette use and complication rates and outcomes following total ankle arthroplasty. Foot Ankle Int. 2016;37(10):1052-9.
- Hsu AR, Franceschina D, Haddad SL. A Novel method of postoperative wound care following total ankle arthroplasty. Foot Ankle Int. 2015;35(7)719-24.
- Huh J, Parekh SG. Use of a continuous external tissue expander in total ankle arthroplasty: a novel augment to wound closure. Foot Ankle Spec. 2016;9(1):43-7.
- Schipper ON, Hsu AR, Haddad SL. Reduction in wound complications after total ankle arthroplasty using a compression wrap protocol. Foot Ankle Int. 2015;36(12):1448-54.