Review Article
Peri-Articular Reconstruction for Intra-Articular Calcaneal Fractures Utilizing the Ilizarov Method with Orthofix Truelok Circular External Fixator: A Technique Guide and Orthoplastic Considerations
Edgardo Rodriguez-Collazo1* and Joseph Agyen2
*Corresponding author: Edgardo Rodriguez-Collazo, Department of Surgery, Director Chicago Foot & Ankle Deformity Correction Center, Illizarov Correction & Microsurgical Limb Reconstruction Presence Saint Joseph Hospital, Chicago, USA
Published: 28 Jun, 2018
Cite this article as: Rodriguez-Collazo E, Agyen J. Peri-
Articular Reconstruction for Intra-
Articular Calcaneal Fractures Utilizing
the Ilizarov Method with Orthofix
Truelok Circular External Fixator: A
Technique Guide and Orthoplastic
Considerations. Clin Surg. 2018; 3:
1998.
Abstract
Calcaneal fractures have been a challenging injury for the surgeon to treat for some time. Poor soft
tissue envelope, vascular compromise and poor overall health are some of the obstacles surgeons
face before entering the operating room. Several techniques exist including Open Reduction and
Internal Fixation (ORIF) with lateral plate and screws, percutaneous techniques of reduction with
k-wires and reduction by external fixation. The purpose of this technique guide is to provide a
comprehensive approach to the treatment of calcaneal fractures when ORIF is not indicated. One
long-term study showed that the functional outcomes of ORIF were statistically the same as nonoperative
treatment in displaced intra-articular fractures. Forty-seven patients with 47 calcaneal
fractures were treated with the reduction traction and Ilizarov method of circular external fixation.
All fractures were classified using the Sanders CT classification system with 27 patients Sanders III
or IV fractures (20 patients). The average age was 37 with a range of 28 to 55. The mean follow-up
time was 32 months with a minimum of 28 months. The average post-op AOFAS hindfoot score was
81.25. All patients were allowed to bear 20% of weight starting at post-operative day #0. We present a
technique for reduction of Sanders stage III and IV calcaneal fractures by means of external fixation.
The senior author presents a long-term retrospective analysis using this particular technique with
favorable outcomes. Using indirect reduction and external fixation with the Ilizarov method we can
limit complications and improve functional outcomes of intra-articular calcaneal fractures.
Keywords: Calcaneal fracture; Ilizarov; Trauma; External fixator; Orthoplastic approach; Orthofix truelok; Reduction traction
Introduction
Historical perspective
Calcaneal fractures are relatively common injuries to the foot amounting to approximately
60% of foot fractures. The large majority is extra-articular and can be treated non-operatively. The
small portions of fractures that involve the articular surface are the injuries that become difficult to
treat and fuel the debate on appropriate technique for reduction. Cotton and Wilson were some of
the first to recognize difficulty in open reduction internal fixation and became advocates of closed
reduction. Their method included reducing the lateral blow out fragment by impacting the fracture
fragments [1].
Bohler was originally involved in describing mechanics of the fracture back in the 1930’s. He
pushed for anatomic reduction by hanging the foot in plantar flexion and using traction to reduce
the fracture. By plantar flexion of the foot, the space between talus and calcaneus was increased to
restore height and joint space. He measured success by the tuber-joint angle, now known as Bohler’s
angle, in his post-reduction radiographs [2]. Later in the 1930’s techniques for percutaneous pin
placement were described with plaster cast immobilization to maintain reduction.
In 1935, dissatisfied with long term outcomes, Conn became a proponent of the triple arthrodesis
for improperly aligned fractures that went on to heal. He discussed loss of arch height and increase
pronation that provided disabling pain to the patient [3]. Gallie, approximately 10 years later,
recommended isolated subtalar joint arthrodesis for fractures that
had healed with persistent joint pain [4]. In the late 1940’s to early
1950’s, Essex-Lopresti and Palmer published results of 90% excellent
patient satisfaction and return to work 4 to 8 months later with open
reduction and restoration of the joint surface augmented with bone
graft [5,6].
Ali in 2009 reduced intra-articular fractures of the calcaneus with
the Ilizarov technique and found it as a good alternative to traditional
methods with fewer secondary problems [7]. Throughout the years
to follow mixed opinions of open reduction and closed reduction
ensued. Large complication rates pushed some to pursue nonoperative
therapy. Despite several advances in technique and fixation,
there is still a debate on this topic.
Indications and contraindications
Poor soft tissue envelope indicated clinically by significant
edema, fracture blisters and lack of signal on Doppler analysis of
the descending peroneal artery are several indications for choosing
external fixation. Others include severe comminuted and displaced
fractures, consistent with sanders III and IV classifications. Patients
with co-morbidities that may delay healing including diabetes, history
of alcohol or tobacco use, vitamin and protein deficiencies also favor
reduction by external fixation in severe fractures. It is the author’s
opinion that the only contraindication to using this method is the
patient’s ability to tolerate the visual concept of wearing an external
fixation device for several months.
Surgical technique
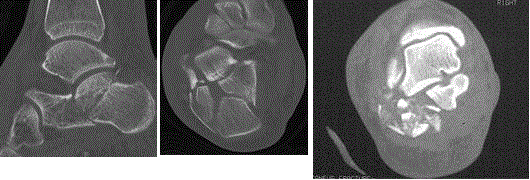
Patient preparation: Three radiographic views of the tibia-fibula
including the foot are obtained as well at a CT scan prior to surgery for
perioperative planning (Figure 1). Routine pre-op labs in addition to
vitamin D and calcium levels are obtained. A nutritional assessment
is obtained on a per patient basis that may include protein, albumin,
pre-albumin, vitamin D and total lymphocyte counts. Furthermore,
measurement of patient’s leg diameter for proper fixator rings size
and length of tibial block. The need for suspensory wire and proper
pin placement can also be determined with use of pre-operative
imaging.
Pre-op adjunct procedure: A pre-operative popliteal block is
recommended to aid in post-op analgesia.
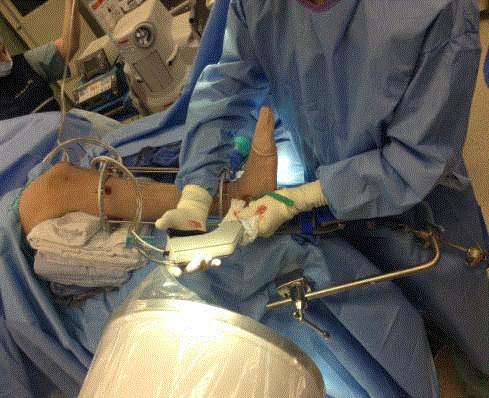
Patient positioning: The first step in the application is proper
positioning of the patient. Anatomic landmarks should be evaluated
to ensure appropriate positioning. The anterior crest of the tibia
should align with the second metatarsal and second toe to ensure
the foot is neither internally nor externally rotated. A leg holder
positioned at knee joint allowing the leg to hang approximately at a
60-degree angle to allow traction of the posterior tuber improving the
calcaneus inclination and height of the calcaneus.
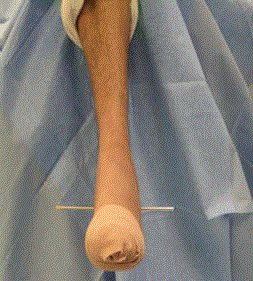
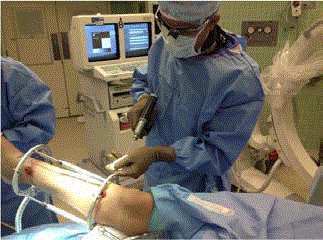
Axial traction: With the foot placed at 90 degrees to the leg, a
3/16-inch Steinman pin is driven just inferior to the peroneal tendons
from lateral to medial through tuber of the calcaneus (Figure 2). The
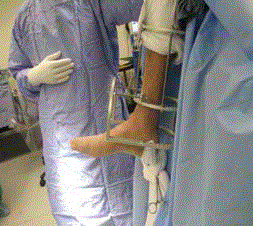
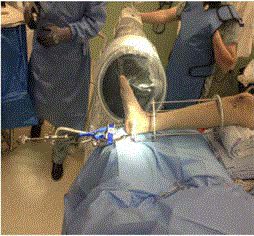
Steinman pin should exit inferior to the tarsal tunnel following the
varus or valgus hindfoot malalignment allowing the surgeon to derotate
the heel with weights (Figure 3) or traction external device
(Figure 4). We suggest using 20 to 25 Ibs of weight hung from the
Steinman pin while manually manipulating the calcaneus to restore
length and width. One can also use a traction table to assist in distal
and plantar distraction.
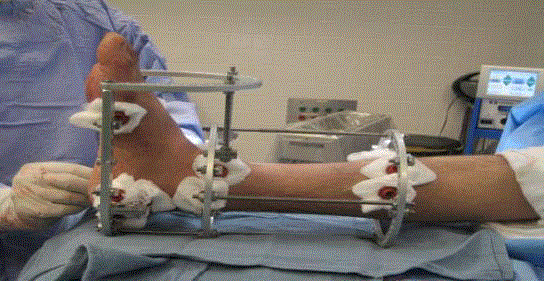
Frame construct
A static external fixator (Orthofix truelok external fixator) is used
for treatment of calcaneal fractures while being distracted. It should
be assembled intra-op without wire placement so that it can be applied
around the calcaneal pin used for skeletal traction. It consists of a long
tibial block with 2 full rings connected by threaded rods, a foot plate,
and half ring. The tibial rings should be sized based on the patient’s
leg girth so that 2 fingers breadths are able to fit between ring and leg.
Four threaded rods are equally spaced and used for the connection
and the frame is then checked in the frontal and sagittal planes.
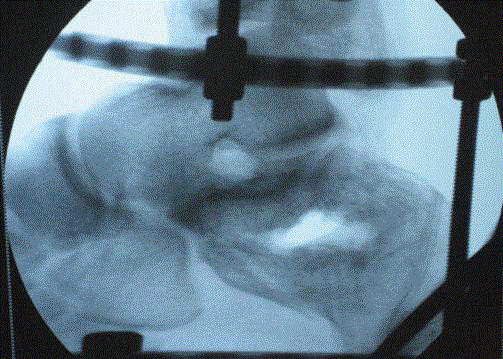
Fracture Reduction: Under fluoroscopic guidance, triangulate the
posterior facet and insert a3/16-inch Steinman pin from inferior to
superior to elevate posterior facet. This pin is used in conjunction with
skeletal tractionto joystick and manipulates the posterior fragment. A
small incision is made to the lateral aspect of the calcaneal tuber just
inferior to the posterior facet. Under fluoroscopy, a small to medium
straight osteotome is placed just inferior to the posterior facet and
maneuvered (Figure 5).
This allows the surgeon to elevate the facet until joint realignment
is achieved under fluoroscopy. If in your pre-operative imaging studies
the fragment is found to be severely depressed, a pair of pliers can be
used for extra leverage in conjunction to the osteotome. Lavage of the
joint after realignment can be preformed to help prevent arthrosis
(Figure 6). Often times a large bone void will be created and can be
backfilled with allograft (Figure 7).
When proper realignment is established, the lateral radiograph
will show an overlap of the lateral process of the talus with the
posterior facet, thus giving the appearance that the joint is not
congruent; however, in reality realignment is established.
Application of the external fixator
Wire placement technique: Minimum of two wires per ring
is essential for stability with wire angles at 60 degrees. One wire is
placed above the ring and one wire below (Figure 8). Simultaneous
tensioning at 130 kg is performed to ensure adequate wire tension
when fixed to frame. The tibial block wires are secured prior to
fracture reduction.
The external fixation frame is provisionally stabilized with one
transverse transosseous wire for each ring and bone segment. The
author prefers to hold the transosseous wire with an alcohol or cold
saline soaked gauze during the insertion process to minimize crosscontamination
and to decrease the temperature across the wire
during insertion. We have found by placing all transosseous wires
(smooth transosseous wires, olive wires) and half pins in a sterile
ice bath in turn decreasing thermal necrosis during application.
After placement of the transverse transosseous wires, positioning is
performed clinically.
The second step is to further stabilize each bone segment and
level of the external fixator with an additional tensioned transosseous
wire. The oblique transosseous wires are placed on the opposite side
of the ring, superior or inferior, to which the transverse transosseous
wire were place to increase stability. These wires should be inserted
at approximately 60-degree angle from the transverse transosseous
wire. After appropriate positioning of the wires and external fixator,
the transosseous wires are tensioned with a dynamometric tensioner.
The transosseous wires exiting posteriorly should be tightened with
a wrench and the anterior wires should be finger tightened and dual
tension to 130 kg of force. Next a transosseous wires should be placed
through the forefoot taking care to plantar flex the 1st ray during
insertion. The forefoot wire will be tensioned at the end to 90 kg.
Once the wires are secured and proper tensioning is achieved, the
calcaneal olive wire is inserted. This wire is directed from medial to
lateral and inferior to the tarsal tunnel. This wire is tightened with
a wrench medially and tensioned with a dynamometric tensioner
laterally. Fracture reduction is held in place via ligamentotaxis. To
maintain distraction, the nuts are tightened to secure the tibial block
to the foot plate. The traction is disengaged and removed at this time.
A posterior facet suspensory wire is inserted from lateral to medial
with fluoroscopic guidance so that the wire sits just inferior the facet
to prevent any future joint depression. The wire often will not sit flush
with fixator and may need to be posted to allow for attachment of the
wire to the ring. This wire should then be tensioned to approximately
90 kg of force. The forefoot wire can now be tension to approximately
90 kg of force (Figure 9). Only applied if after reduction and bone
grafting there is radiographic evidence of declination of the posterior
facet (not needed if reduction is seen).
Any incisions are now sutured together with suture of the
surgeon’s choice including the larger opening from the Steinman pins
using peroxide, the skin and fixator are cleaned thoroughly (Figure
10). A bulky sterile dressing consisting of abdominal padding and
kerlix is placed and left intact for 12-14 days.
Post-op protocol
Weight-bearing status
• Patients are allowed to start weight bearing at 20% with a
4-point pick-up rolling walker immediately post operatively. Explain
to the patient that weight bearing is strongly encouraged as it promotes
callus formation and bone healing. Furthermore, ambulatory activity
decreases the formation of post-operative deep vein thrombosis.
• Patients are discharged with a rolling walker or crutches.
Rolling walkers are preferred due to increased stability and better
control of a 20% weight bearing status. A consult to physical therapy
is needed prior to patient discharge to ensure adequate ambulation
capabilities using the rolling walker.
Dressing
• The original post-op dressing is to remain intact for 12-14
days.
• After the initial dressing change within the office setting,
the ex-fix can be sprayed with Isopropyl alcohol around each pin.
Sterile 4 × 4’s are placed around each wire to protect the skin/pin
interface from the environment.
• After the initial dressing change, the patient is education
on cleaning the frame themselves. Instruct the patient to no touch
the wire or remove any eschar. Patient’s with poor soft tissue envelop
are advised not to clean wires on their own and should be done only
by the surgeon. The patient can clean the frame approximately every
3 days. Furthermore, once all wires are dry/stable and there is no
evidence of drainage/irritation, the patient is allowed to shower and
swim with application of alcohol immediately after (not earlier than 2
weeks). Patients with poor soft tissue envelop, long-standing diabetes
and poor compliance rate may never submerse the external fixator in
water and pin site care must be performed by surgeon or professional
care provider.
• A footpad can be made with foam heel protector and
incorporated into the dressing for assistance in weight bearing
activity. A rigid sole surgical shoe can also be modified and applied.
• The entire frame is to be covered with either elastic bandage
to protect the frame from the environment.
Warning signs
• During the post-operative course, the patient is educated on
the signs and presentation of a pin site infection (Redness, swelling,
pain and discharge). A prescription for antibiotics is dispensed to the
patient. The patient is also instructed to return to the office within
24 hours. Infections that appear deep or non-resolving require
admission for IV antibiotics to prevent osteomyelitis.
• Erythema and mild drainage is normally due to a loose,
unstable wires (not due to infection), which can be resolved by
tightening using the “Russian Technique.” Another cause may be
due to increased skin tension around the wire that can be relieved
by performing a stab incision. Granulomas are common around pin
sites and can be resolved with silver nitrate.
• Deep vein thrombosis is minimized by the patient’s early
weight bearing status.
• Wire breakage is occasionally seen but by proper tensioning
of the wires intra-operatively decreases this complication. The
suspensory wire aids in prevention of joint collapse, which is left in
place until complete consolidation is noted.
Antibiotics
• Oral antibiotics are a surgeon’s preference, but Augmentin
875 mg 1 tab PO BID × 14 day is commonly used for superficial pin
infection.
• Ciprofloxacin and Clindamycin combination for Penicillin
allergic patients.
• Zyvox 600 mg for infection that do not respond to
Augmentin.
Post-op pain
• Patients are generally admitted 23 hours for pain control
immediately post-operatively, but upon discharge should be placed
on Tylenol #3 or any oral analgesic regimen the surgeon prefers.
We prefer using a triad off pain relievers including; Tramadol 100
mg, Lyrica 50 mg and Tylenol #3 for post-operative outpatient pain
management.
• While in the hospital a PCA pump is ordered per anesthesia.
Titration off the PCA is recommended by day 2 and transitioned to
Tylenol #3 upon discharge. Tramadol can also be used in conjunction
with the Tylenol #3.
• Recommend a popliteal block pre-operatively by anesthesia
to greatly minimize post-operative pain or possibly eliminate the
need for admission.
• Never use Toradol or NSAIDS due to decrease of bone
healing. Communication with anesthesia is important as Toradol is
frequently administered at the end of cases.
Removal of Ex-Fix
• A CT scan is ordered to confirm bone regeneration and
consolidation of fracture fragments. Once this is verified the patient
can be scheduled for fixator removal (Figure 11).
Figure 1
Figure 2
Figure 2
After the foot is placed at 90 degrees to the leg, a 3/16-inch
Steinman pin is driven just inferior to the peroneal tendons from lateral to
medial through the tuber of the calcaneus.
Figure 3
Figure 4
Figure 5
Figure 6
Figure 7
Figure 8
Figure 8
A minimum of two wires per ring is essential for stability with wire
angles at 60 degrees and one placed above and below the ring.
Figure 9
Figure 10
Figure 11
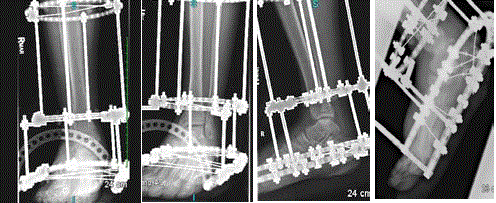
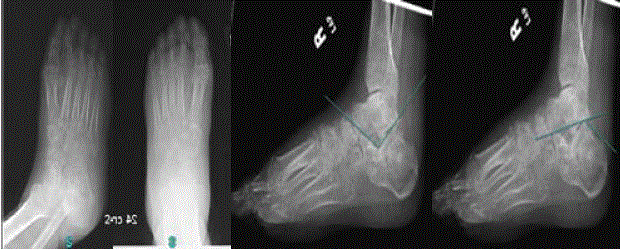
Figure 11
Post-operative films of a stage IV sanders calcaneal fracture
reduction utilizing ilizarov method with orthofix truelok circular external fixator.
A) Oblique view. B) AP view. C) Lateral view showing angle of Gisseane’s
after reduction approximately 105 degrees. (Normal~120-140) D) Lateral
view showing Bohler’s angle after approximately 36 degrees (Normal~25-40).
Results
Data collected from 2000 to 2013, 47 calcaneal fractures were
treated with the above method. All were classified to be Sanders III (27
patients) or IV fractures (20 patient).Of the 47-calcaneal fractures, 12
were female and 35 were male. The average age was 37 with a range of
28-55. The mean follow-up time was 32 months with a minimum of
28 months. Co-morbidities included 33 patients with osteoporosis, 16
patients with DM type 2, 7 patients with renal disease and 8 patients
(males) with severely poor soft tissue envelope. Furthermore, 11
patients had a current history of smoking (8 males) and 21 patients
were considered to have obesity due to abnormal BMI (18 Male; 3
Female). There were no open fractures and 1 case was a bilateral
injury. All cases were done under fluoroscopy using demineralized
bone matrix (Integra-Evo3c). The average time in the fixator was 13
weeks, which corresponds to radiographic healing time.
Once the external fixator was removed and patient returned to
pre-injury activities, the patients were evaluated with the AOFAS
hindfoot and ankle score for pain and functionality. The average
post-op score was 81.25. All patients were allowed to bear 20% of
weight starting at post-operative day #0. In this series of 47 calcaneal
fractures, no cases of wound dehiscence from the lateral incision were
reported. In 3 cases, superficial pin tract infections were reported, all
of which whom were DM type II and resolved with oral antibiotics. In
3 cases transient sural neuritis was reported. Residual varus deformity
was reported in 5 subjects that further required subsequent calcaneal
slide procedures to correct. Subtalar joint collapse was reported in 7
patients. Finally, additional corrective procedures involving subtalar
joint fusion was performed in7 patients with symptomatic Subtalar
joint arthrosis.
Discussion
We present a series of comminuted calcaneal fractures reduced
with Ilizarov method utilizing the truelok orthofix external fixation.
Talarico et al. [8] reviewed 25 fractures over 7 years and noted 92%
good and excellent results with the Maryland Foot Score (MFS). They
also noted ROM >50% of the uninjured side in 21 of 25 fractures.
It is our opinion that skeletal traction and reduction of calcaneal
fracture with the Ilizarov method is a viable technique for the
treatment of comminuted sanders III and IV injuries. It can also
be used in open fractures as well as those associated with soft tissue
compromise, whether that is from the injury itself or patient’s comorbidities.
It allows immediate reduction of the fracture, while open
methods often mandate a delay in repair due to the poor soft tissue
envelope. This technique also allows for immediate weight bearing
after surgery.
Conclusion
The application of the external fixator can be technically challenging and requires a basic knowledge of frame biomechanics and cross-sectionalanatomy; however, the reduction of the fracture follows the basic principles of skeletal traction. Joint distraction can also be incorporated and maintained with the repair. The complications are limited and with proper technique and attention to detail, these complications are further minimized. The outcomes of the reduction with Ilizarov stabilization then become predictable and favorable compared to the open technique.
References
- Cotton FJ, Wilson LT. Fractures of the os calcis. Boston Med Surg J. 1908;159(18):559-65.
- Böhler L. Diagnosis, pathology and treatment of fractures of the os calcis. J Bone Joint Surg. 1931;13(1):75-89.
- Conn HR. The treatment of fractures of the os calcis. J Bone Joint Surg. 1935;17:392.
- Gallie WE. Subastragalar arthrodesis in fractures of the os calcis. J Bone Joint Surg. 1943;25(4):731-6.
- Essex-Lopresti P. The mechanism, reduction technique and results in fractures of the os calcis. Br J Surg. 1952;39(157):395-419.
- Palmer I. Mechanisms and treatment of fractures of the os calcis. J Bone Surg. 30-SA, 2-8.
- Ali AM, Elsaied MA, Elmoghazy N. Management of calcaneal fractures using the Ilizarov external fixator. Acta Ortho Belg. 2009;75(1);51-6.
- Talarico L, Vito GR, Zyryanov SY. Management of displaced intra-articular calcaneal fractures by using external ring fixation, minimally invasive open reduction and early weight bearing. J Foot Ankle Surg. 2004:43(1);43-50.