Case Series
Elevated Serum Creatinine Levels Can be a Novel Prognostic Parameter in Patients with Extra Peritoneal Bladder Rupture due to Blunt Trauma: A Report of Two Cases
Keisuke Ymamoto1, Motoo Fujita2* and Shigeki Kushimoto2,3
1Osaki City Hospital Emergency Center, Japan
2Tohoku University Hospital Emergency Center, Japan
3Division of Emergency and Critical Care Medicine, Tohoku University Graduate School of Medicine, Japan
*Corresponding author: Motoo Fujita, Tohoku University Hospital Emergency Center,1-1 seiryomachi, Aobaku, Sendai 980-8574, Japan
Published: 18 May, 2018
Cite this article as: Ymamoto K, Fujita M, Kushimoto S.
Elevated Serum Creatinine Levels Can
be a Novel Prognostic Parameter in
Patients with Extra Peritoneal Bladder
Rupture due to Blunt Trauma: A Report
of Two Cases. Clin Surg. 2018; 3: 1970.
Abstract
Introduction: Non-operative management is the standard approach to extra peritoneal bladder
rupture and urethral catheter drainage is usually effective. However, surgical treatment may be
considered in selected patients to shorten the treatment period and reduce complications. However,
no reliable clinical indicator has been developed to help determine the optimal management strategy.
We report two cases of extra peritoneal bladder rupture due to Blunt trauma with persistent mild
elevation of serum creatinine and mild pseudo-acute kidney injury during the prolonged period of
non-operative management.
Case Presentation: Case 1: A 76-year-old woman was diagnosed with a pelvic fracture and multiple
traumatic injuries after being hit by a car. Her circulatory status was stable. Extra peritoneal bladder
rupture was diagnosed by Computed Tomography (CT) cystography on day 5. We elected nonoperative
management and continued bladder drainage through the urethral catheter until day 72.
Case 2: A 53-year-old man was hit by a car while riding his motorcycle. He suffered a pelvic fracture,
which required embolization of the bilateral internal iliac arteries. A CT scan on day 3 showed
leakage of contrast material near the pubis and he was diagnosed with extra peritoneal bladder
rupture. He required bladder drainage until the leakage resolved on day 68. In both cases, a mild
elevation of serum creatinine was present, which only decreased after the improvement of urinary
extravasation from the bladder to the retroperitoneal space.
Conclusion: Serum creatinine levels may be a novel parameter to assess the status of extra peritoneal
bladder rupture. Mild elevation of serum creatine may be an important indicator in determining the
timing of surgery and bladder contrast examination during non-operative management of patients
with extra peritoneal bladder rupture.
Keywords: Extra peritoneal bladder rupture; Blunt trauma; Pseudo-acute kidney injury
Abbreviations
AKI: acute Kidney Injury; CT: Computed Tomography
Introduction
The standard approach to extra peritoneal bladder rupture caused by blunt trauma is conservative management. Studies in the1970s and 1980s reported that most patients with isolated, uncomplicated injuries can be treated with catheter drainage with acceptable outcomes [1-3]. Although non-operative management for bladder injuries has also been expanded to intra peritoneal bladder rupture, recent reports have suggested that in patients with extra peritoneal rupture, this approach may increase the incidence of complications, including infection and persistent urinary leakage [4,5]. Surgical treatment in selected patients with extra peritoneal rupture may be considered to shorten the treatment period and reduce complications [6]. Cystography with full bladder distension is the mainstay method for the evaluation of bladder status [7], however, the procedure may disturb the healing process. Creatinine equilibration across the peritoneal membrane is a well-characterized phenomenon and is the foundation for peritoneal dialysis. Pseudo-renal failure is a rare condition with laboratory abnormalities that mimic Acute Kidney Injury (AKI) in the setting of normal kidney function [8]. Although patients with pseudo-AKI due to intra peritoneal bladder rupture have been reported, pseudo-AKI in patients with extra peritoneal rupture of the bladder due to blunt trauma has never been reported. We report two cases of extra peritoneal bladder rupture due to blunt trauma with persistent mild elevation of serum creatinine and mild pseudo-AKI during the prolonged non-operative management period.
Figure 1
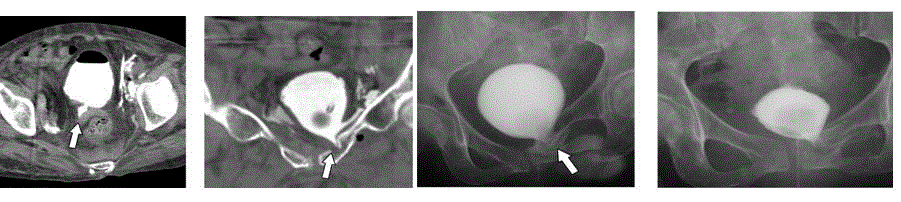
Figure 1
Computed tomography and fluoroscopic imaging of the bladder.
Case 1 A-D: Multiple bladder injuries were evident on day 5 (A, B). The healing of the bladder injury was prolonged and the leakage only disappeared on day 72.
The arrows demonstrate the extra luminal contrast material leaking from the ruptured bladder into extra peritoneal space.
Figure 2
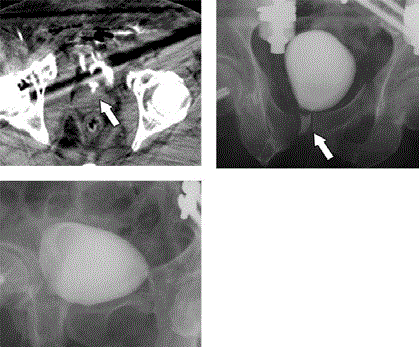
Figure 2
Computed tomography and fluoroscopic imaging of the bladder.
Case 2 A-C: The fractures and bladder injuries were adjacent. The healing of
the bladder injury was prolonged and the leakage only disappeared on day
68. The arrows demonstrate the extra luminal contrast material leaking from
the ruptured bladder into extra peritoneal space.
Case Presentation
Case 1
A 76-year-old woman was struck by a passenger car while
walking. She was diagnosed with a right humerus open fracture,
bilateral pulmonary contusions, multiple rib fractures, and pelvic
fracture. Although her hemodynamic status was stable, Computed
Tomography (CT) with contrast enhancement demonstrated
extravasation of the contrast medium, which required embolization
of the bilateral internal iliac arteries. She was managed with positive
pressure ventilation for her flail chest. Extra peritoneal bladder rupture
was definitively diagnosed by CT cystography on day 5. Defects in the
medial and left side of the anterior walls of the bladder with leakage
of contrast material into the pelvic wall were recognized. We elected
non-operative management and continued bladder drainage through
the urethral catheter. She subsequently suffered from bacteremia
due to Escherichia coli, causing abscess formation on the left side
of the pubis, and Candida glabrate, requiring the administration of
antibiotics. Although extra luminal enhancement in the left side of the
anterior bladder wall was observed on fluoroscopic imaging on day
47, the leakage had disappeared by day 73, and she was discharged on
day 136 (Figure 1). There were no specific etiologic events that may
have contributed to the serum creatinine elevation during her clinical
course, except for intravenous contrast agent administration and
infectious complication. Elevated serum creatinine values decreased
after the urinary extravasation from the bladder to the retroperitoneal
space improved (Figure 3).
Case 2
A 53-year-old man was struck by a passenger car while riding his
motorcycle. He suffered pelvic, right femoral trochanter, left femoral
shaft, and right humeral shaft fractures, as well as macroscopic
hematuria. Although his hemodynamic status was stable, a CT
scan with contract enhancement demonstrated extravasation of
the contrast medium, which required embolization of the bilateral
internal iliac arteries. A CT scan on day 3 showed leakage of contrast
material near the pubis and he was diagnosed with extra peritoneal
bladder rupture. His intermittent macroscopic hematuria persisted,
and a fluoroscopic imaging study on day 40 showed that leakage of
the contrast agent to the extra peritoneal space was still present. On
day 68 his leakage resolved and the urethral catheter was removed
(Figure 2). There were no specific etiologic events that may have
contributed to the serum creatinine elevation during his clinical
course, except for intravenous administration of the contrast agent
and antibiotics. Elevated serum creatinine values decreased after the
urinary extravasation from the bladder to the retroperitoneal space
improved (Figure 3).
Figure 3
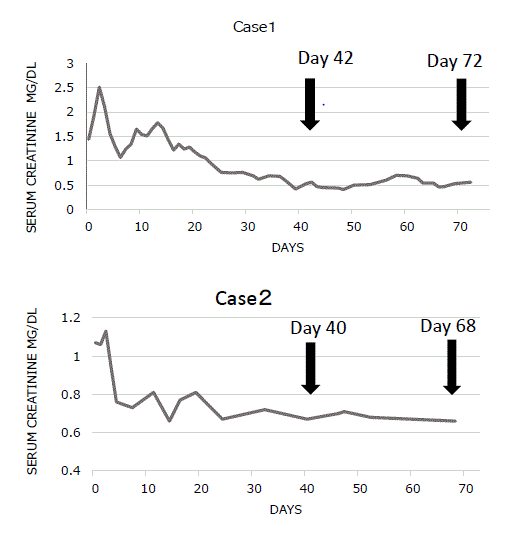
Figure 3
Changes in serum creatinine levels The arrows indicate the days
on which cystography was performed. In case 1, contrast medium leakage
was recognized on day 42 and had resolved on day 72. In case 2, contrast
medium leakage was present on day 40 and had resolved on day 68.
Discussion
Non-operative management is the standard treatment approach for extra peritoneal bladder rupture, and urethral catheter drainage usually leads to improvement within 3 weeks [9]. However, some patients may still need prolonged healing periods, and early surgical intervention can be a useful option in such cases [6]. In general, continuity between the fracture site and the bladder, the site and degree of bladder, the presence of intra vesical and intramural hematoma, and persistent hematuria can inhibit the healing process [10], and the present cases exhibited some of these factors. Serum creatinine elevation in the acute phase that cannot be explained by a specific factor, such as urine leakage from the bladder, may be considered as a predictor of the course of healing. Pseudo-renal failure with laboratory abnormalities that mimic AKI in the setting of normal kidney function has been reported in patients with intra peritoneal bladder rupture due to several traumatic and nontraumatic etiologies [8]. However, no similar reports after extra peritoneal rupture of the bladder exist. In addition, cystography with full bladder distension, which may disturb the healing process, can be postponed, if elevation of serum creatinine with no specific etiology continued. We report first two cases of extra peritoneal bladder rupture due to blunt trauma with persistent mild elevation of serum creatinine during the prolonged period of non-operative management. The serum creatinine levels started to decrease once the bladder status improved. In conclusion, serum creatinine levels may be a novel marker of improvement after bladder rupture and an indicator for cystography and surgical intervention.
Funding
The manuscript was supported by Tohoku-kyuikai.
References
- Corriere JN Jr, Sandler CM. Management of the ruptured bladder: seven years of experience with 111 cases. J Trauma. 1986;26(9):830-3.
- Cass AS, Luxenberg M. Management of extraperitoneal ruptures of bladder caused by external trauma. Urology. 1989;33(3):179-83.
- Cass AS, Luxenberg M. Features of 164 bladder ruptures. J Urol. 1987;138(4):743-5.
- Kotkin L, Koch MO. Morbidity associated with nonoperative management of extraperitoneal bladder injuries. J Trauma. 1995;38(6):895-8.
- Elliott SP1, McAninch JW. Extraperitoneal bladder trauma: delayed surgical management can lead to prolonged convalescence. J Trauma. 2009;66(1):274-5.
- Johnsen NV, Young JB, Reynolds WS, Kaufman MR, Milam DF, Guillamondegui OD, et al. Evaluating the Role of Operative Repair of Extraperitoneal Bladder Rupture Following Blunt Pelvic Trauma. J Urol. 2016;195(3):661-5.
- Carlin BI, Resnick MI. Indications and techniques for urologic evaluation of the trauma patient with suspected urologic injury. Semin Urol. 1995;13(1):9-24.
- Dees A, Kluchert SA, van Vliet AC. Pseudo-renal failure associated with internal leakage of urine. Neth J Med. 1990;37(5-6):197-201.
- Gomez RG, Ceballos L, Coburn M, Corriere JN Jr, Dixon CM, Lobel B, et al. Consensus statement on bladder injuries. BJU Int. 2004;94(1):27-32.
- Avey G, Blackmore CC, Wessells H, Wright JL, Talner LB. Radiographic and clinical predictors of bladder rupture in blunt trauma patients with pelvic fracture. Acad Radiol. 2006;13(5):573-9.