Review Article
Multiple Pilomatrixomas: Review of Genetic Associations – The Surgeon Perspective
Adeeb Paddy Naasan1, Hannah Naasan2 and Anas Naasan1*
1Department of Plastic Surgery, Institute of Ninewells Hospital, UK
2Department of Dermatology, Institute of Ninewells hospital, UK
*Corresponding author: Anas Naasan, Department of Plastic Surgery, Ninewells Hospital and Medical School, Dundee DD1 9SY 01382660111, Scotland, UK
Published: 30 Apr, 2018
Cite this article as: Naasan AP, Naasan H, Naasan A.
Multiple Pilomatrixomas: Review of
Genetic Associations – The Surgeon
Perspective. Clin Surg. 2018; 3: 1957.
Abstract
Pilomatrixoma, or calcifying epithelioma of Malherbe, was first described in 1880 by Malherbe and
Chenantais. It is a benign neoplasm arising from hair follicle matrix cells. It usually presents as a hard
subcutaneous slowly growing mass. It accounts for 1.04% of all benign skin lesions. The overlying
skin is mostly skin-coloured but could be pigmented. The mass is either deeply subcutaneous and
invisible or superficial with possible erosion. Bullous appearance has also been described but is rare.
Multiple pilomatrixomas is found to be associated with several genetic conditions, most commonly
myotonic dystrophy, Turner’s syndrome, and Gardner’s syndrome. Recent associations with MYHassociated
polyposis, Rubinstein-Taybi syndrome, Trisomy 9, Sotos syndrome and sarcoidosis have
also been reported in the literature. A review of the literature assessing the genetic implications
for multiple pilomatrixomas is analysed. Areas for future research into some of these associations
currently suggested by the literature are highlighted.
Keywords: Multiple pilomatrixomas; Pilomatrixoma; Pilomatricoma; Genetic; Skin
Introduction
Pilomatrixoma, sometimes spelled as ‘pilomatricoma’, is also known as a calcifying epithelioma of Malherbe, since it was first described in 1880 by Malherbe and Chenantais [1]. It was thought initially to be a calcified tumour of sebaceous glands. However, Forbis and Holwig demonstrated in 1961 that the benign tumour originates from hair cell matrix, thus the term Pilomatrixoma was introduced [2]. Lesions usually present as a solitary, skin-coloured or pigmented cystic or firm nodules on the head, neck or upper extremities [1]. It lies either deeply subcutaneously and invisible or superficial with possible erosion (Figure 1 and 2). It is characterised by calcification within the lesion, which accounts for the firm feel, and often results in an angulated shape (the ‘tent sign’). Bullous appearance of pilomatrixomas is rare (Figure 3) [3]. The fluid has been shown to be lymphatic. Aetiology remains debatable, although various theories have been proposed as possible explanation. Multiple lesions are found in 3.5% of cases [4]. Familial pilomatrixomas and multiple familial pilomatrixomas are even rarer [5]. Four distinct morphological stages have been proposed: early small and cystic, fully developed or large lesions, early regression and late regression with calcification [6]. A study in the 1970s by Moehlenbeck found that pilomatrixomas accounted for 0.12% of 140000 skin tumours [7]. A case review of 107 pilomatrixomas found that the mean age of patient is 13.2 years, while the location of Pilomatrixoma is most commonly in the head (64.5%), neck (14.0%) and upper extremities (12.2%) [8]. The two commonest ages for Pilomatrixomas are the under-20s (>60%) and the elderly [9]. Hence it should be considered in the differential diagnosis of any solitary skin lump in the head, neck and upper extremities [2]. Malignant transformation is rare, but should be considered in a patient with multiple recurrences. Sau et al. [9] reported 43 pilomatrix carcinoma. It has been found that clinicians have a poor diagnostic prediction for this condition; the literature has reported correct pre-operative diagnosis in 35.5% [9] and 28.9% [10] in studies consisting of 107 cases and 346 cases respectively. Surgical excision is the treatment of choice [9], although local recurrences may occur [3].
Literature Review
Sporadic pilomatrixomas are commonly associated with mutations in the beta-catenin (CTNNB)
gene, which is only found within the tumour itself. The Beta-catenin gene is located at the 3p22-p21.3
locus, and functions as a cell-cell adhesion molecule and transcription factor. It is a mediator in the
Wnt signal transduction pathway [11]. These mutations have a similar role in the pathogenesis of
pilomatrixoma in sporadic and multiple tumours [12]. A few cases of
multiple pilomatrixomas have been reported in the literature in the
past. Most notably, the case of a 68-year-old Caucasian woman with a
total of 4 pilomatrixomas (1 facial and 3 upper extremity) was reported
[11]. Another case of a 23-year-old black woman with lesions on her
face and back was clinically suggestive of calcified sebaceous cysts or
lymph nodes, but on histopathology were found to be pilomatrixomas
[12]. A similar case of an 18-year-old Indian man found a history of
4 current and 2 past pilomatrixomas, which were initially suspected
to be neurofibromata. The incidence of multiple pilomatrixoma is
estimated to be 3.5% [5].The most widely reported association of
multiple pilomatrixomas is with myotonic dystrophy. Myotonic
dystrophy is an autosomal disease with variable penetrance. It is a
dysfunction of skeletal muscle, and also involves cardiac conduction
tissues, smooth muscle, the eyes and central nervous system. The
clinical severity varies from death in utero to a mild asymptomatic
condition [13]. The clinical features may appear in early childhood
and include: muscle wasting, weakness, frontal balding, cataract,
expressionless facies, mental retardation, diabetes mellitus, heart
block and hyperostosis frontalis externa. The molecular basis is an
expansion of the unstable trinucleotide repeat in a gene coding for a
novel protein kinase [14].The association of multiple pilomatrixomas
and myotonic dystrophy was first described in the literature in 1965,
by Cantwell and Reed [15]. That this association was also familial was
reported by Harper, in 1971 [16]. The number of lesions reported in
association with myotonic dystrophy varies between 1 and 31 [17].
The recognition of the potential for use of multiple pilomatrixoma as
a cutaneous marker for myotonic dystrophy was recognised in 1978.
They may precede the signs of myotonic dystrophy, and as such may
be a potential early cutaneous marker [18]. In these cases genetic
testing may be warranted [19]. A figure for the number of cases of
multiple pilomatrixoma which then go on to develop myotonic
dystrophy is not available in the research; this may be an interesting
area for future research into this association. Another association
of multiple pilomatrixomas is with Gardner’s syndrome. Gardner’s
syndrome is a variant of adenomatous polyposis coli (APC), and is an
autosomal dominant disease characterised by gastrointestinal polyps,
multiple osteomas, hypertrophy of the retinal pigment epithelium,
and skin and soft tissue tumours. The APC protein is a negative
regulator of Beta-catenin; the relationship of this with pilomatrixoma
has already been mentioned [20]. A study analysing epidermal cysts
excised from subjects with Gardner’s syndrome found 63% had
features histologically similar to those of a pilomatrixoma [21]. A case
study of two familial cases of multiple pilomatrixoma leading to the
diagnosis of Gardner’s syndrome in one of the subjects suggests that
multiple pilomatrixoma may be a cutaneous marker for Gardner’s
syndrome [22]. MYH-associated polyposis (MAP) is a recessive form
of adenomatoous polyposis coli (APC) associated with susceptibility
to colorectal carcinoma [23]. A case report of two siblings found
both had developed a low number of colonic lesions and early-onset
colorectal carcinoma, and had a history multiple pilomatrixomas
excised in childhood [24]. This study suggests that a history of multiple
pilomatrixomas may predispose to MAP. There are 3 reports in the
literature of an association with Turner’s syndrome. One reports
2 cases of multiple pilomatrixomas in childhood associated with
Turner’s syndrome [25]. The second report is of a 10-year-old girl
with Turner’s syndrome who presents with multiple pilomatrixomas.
The author suggests the predisposition may be due to abnormalities
of hair-bearing skin in Turner’s syndrome. The third report is of a13-
year-old girl with Turner’s syndrome in association with 10 separate
facial pilomatrixomas [26]. Most recently, a multicentre study
demonstrated a high prevalence (2.6%) of pilomatrixomas among
patients with Turner syndrome [27].
Trisomy 9 is a rare chromosomal disorder, characterised by
facial anomalies, joint abnormalities, cardiac abnormalities, growth
retardation and mental retardation, with a poor prognosis. Known
skin abnormalities include deep palmar and plantar creases and
hyperconvex nails [28]. One case report describes a four-yearold
Japanese girl with trisomy 9 in whom a diagnosis of multiple
pilomatrixomas was confirmed histopathologically after excision of
the lesions from her left lower eyelid and median precordium [29]. To
date, there are two further case reports in the literature with multiple
pilomatrixoma in patients with Trisomy 9 [30,31]. The association of
multiple pilomatrixomas with three cases of Trisomy 9 suggests the
likely possibility of a link between them. Soto’s syndrome is a very
rare genetic disorder with excessive physical growth during the first
2-3 years of life, mild mental retardation, delayed motor, cognitive
and social development, hypotonia and speech impairment [32].
Patients with Soto’s syndrome have an increased risk of developing
neoplasms. There is one report in the literature of an association
between Soto’s syndrome and multiple pilomatrixomas; although
this may be an incidental finding [33]. Rubinstein Taybi syndrome
is caused by an autosomal dominant mutation, and is characterised
by short stature, learning difficulties, broad thumbs and first toes,
small head and distinctive facies [34]. The association with multiple
pilomatrixomas was first reported in 1994 [35]. Another case,
reported in 2004, is that of multiple pilomatrixomas associated with
both Rubinstein-Taybi syndrome and Churg-strauss syndrome [36].
Another case was reported in 2015 in the German literature [37]. There
has been one case report in the literature of an association of multiple
pilomatrixomas with sarcoidosis; however there are no other similar
reports [38]. Sarcoidosis is characterised by the presence of noncaseating
granulomas of unknown aetiology affecting two or more
organs. It includes lung, skin, eyes, liver, cardiac and neurological
manifestations. The skin is the second most commonly affected organ
in sarcoidosis. Skin manifestations include hyperpigmentation,
hypopigmentation, keloid reaction, lupus pernio, and erythema
nodosum [39]. Recently, there is a single case report of a 15-yearold
patient with gliomatosis cerebri- a rare primary brain tumour -
developing four histologically-confirmed pilomatrixomas on his face
and upper arm in the course of 1 year [40]. This is hypothesised to be
a new association and would represent an interesting area for further
research.
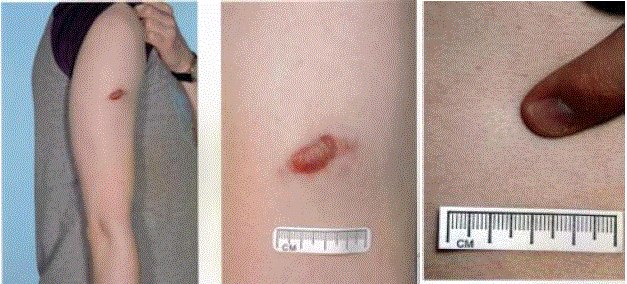
Figure 1 and 2
Figure 1 and 2
Lesions usually present as a solitary, skin-colored or
pigmented cystic or firm nodules on the head, neck or upper extremities. It
lies either deeply subcutaneously and invisible or superficial with possible
erosion.
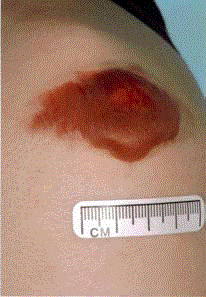
Figure 3
Conclusion
Multiple pilomatrixomas has been reported widely in the literature, with an incidence of 3.5%. Definite associations have been formed with myotonic dystrophy, Gardner’s syndrome, MYH-associated polyposis and possibly Turner’s Syndrome. Rarer associations with Trisomy 9, Soto’s syndrome and Rubinstein Taybi syndrome have been mentioned in the literature, but have yet to be confirmed. The importance of the genetic associations must be taken into consideration when patients present with multiple pilomatrixomas, to facilitate further investigation of the underlying cause.
References
- Malherbe A, Chenantais J. Note sur L'epitheliome calcife des glandes sebacees. Prog Med (Paris). 1880;8:826-37.
- Wolff K, Goldsmith L, Katz SI, Gilchrest B, Paller AS, Leffell D. Fitzpatrick’s dermatology in general medicine. In: Wolff K, Goldsmith L, Katz SI, et al editors. Vol 1. 7th ed. New York: McGraw Hill Medical; 2008;1081-2.
- Inui S, Kanda R, Hata S. Pilomatricoma with a bullous appearance. J Dermatol. 1997;24(1):57-9.
- Geh JLC, Wilson GR. Unusual multiple pilomatrixomata: case report and review of the literature. Br J Plast Surg. 1999;52(4):320-1.
- Hills RJ, Ive FA. Familial multiple pilomatrixomas. Br J Dermatol. 1992;127(2):194-5.
- Kaddu S, Soyer HP, Hodl S, Kerl H. Morphological stages of pilomatricoma. Am J Dermatopathol. 1996;18:333-8.
- Moehlenbeck FW. Pilomatrixoma (calcifying epithelioma): A statistical study. Arch Dermatol. 1973;108(4):532-4.
- Lee SJ, Park HJ, Kim SK. Clinical Analysis of Pilomatrixoma: A Review of 107 Cases. J Korean Soc Plast Reconstr Surg. 2004;31(5):676-81.
- Sau P, Lupton GP, Graham JH. Pilomatrix carcinoma. Cancer. 1993;71(8):2491-8.
- Aslan G, Erdogan B, Akoz T, Görgü M, Seçkin S, Terzioğlu A. Multiple Occurrence of Pilomatrixoma. Plast Reconstr Surg. 1996;98(3):510-3.
- Wolff K, Goldsmith LA, Katz SI, et al, editors. Fitzpatrick’s Dermatology in General Medicine. Volume 1. 7th ed. New York: McGraw Hill Medical, 2008.
- Reddy SS, Gadre SA, Adegboyega P, Gadre AK. Multiple pilomatrixomas: case report and literature review. Ear, Nose and Throat Journal. 2008;87(4):230-3.
- Warrell OA, Cox TM, Firth JD, Benz EJ, editors. Oxford Textbook of Medicine. 4th ed. Oxford: OUP, 2003;1235-9.
- Berberian BJ, Colonna TM, Battaglia M, Sulica VI. Multiple pilomatricomas in association with myotonic dystrophy and a family history of melanoma. J Am Acad Dermatol. 1997;37(2):268-9.
- Cantwell AR, Reed WB. Myotonia atrophica and multiple calcifying epithelioma of Malherbe. Acta Derm Venereol. 1965;45(5):387-90.
- Harper PS. Calcifying epithelioma of malherbe and myotonic dystrophy in sisters.Birth Defects Orig Artic Ser. 1971;7(8):343-5.
- Geh JL, Moss AL. Multiple pilomatrixomata and myotonic dystrophy: A familial association. Br J Plast Surg. 1999;52(2):143-5.
- Chiaramonti A, Gilgor RS. Pilomatricomas associated with myotonic dystrophy. Arch Dermatol. 1978;114(9):1363-5.
- Sherrod QJ, Chiu MW, Gutierrez M. Multiple pilomatricomas: Cutaneous marker for myotonic dystrophy. Dermatol Online J. 2008;14(7):22.
- Warrell OA, Cox TM, Firth JD, Benz EJ, editors. Oxford Textbook of Medicine. Vol 1. 4th ed. Oxford: OUP; 2003;233.
- Berberian BJ, Colonna TM, Battaglia M, Sulica VI. Multiple pilomatricomas in association with myotonic dystrophy and a family history of melanoma. J Am Acad Dermatol. 1997;37:268-9.
- Pujol RM, Casanova JM, Egido R, Pujol J, de Moragas JM. Multiple familial pilomatricomas: a cutaneous marker for Gardner syndrome? Pediatr Dermatol. 1995;12(4):331-5.
- Baglioni S, Melean G, Gensini F, Santucci M, Scatizzi M, Papi L, et al. A kindred with MYH-associated polyposis and pilomatricomas. Am J Med Genet A. 2005;134A(2):212-4.
- Noguchia H, Kayashimaa K, Nishiyamab S, Onoa T. Two Cases of Pilomatrixoma in Turner's Syndrome. Dermatology. 1999;199(4):338-40.
- Wood S, Nguyen D, Hutton K, Dickson W. Pilomatricomas in Turner syndrome. Pediatr Dermatol. 2008;25:449-51.
- Bengtzen AR, Grossniklaus HE, Bernardino CR. Multiple Pilomatrixoma in Turner Syndrome. Ophthal Plast Reconstr Surg. 2009;25(3):229-30.
- Handler MZ, Derrick KM, Lutz RE, Davenport ML, Armstrong AW, Morrell DS. Prevalence of pilomatricoma in Turner Syndrome: findings from multicentre study. JAMA Dermatol. 2013;149(5):559-64.
- Arnold GL, Kirby RS, Stem TP, Sawyer JR. Trisomy 9: review and report of two new cases. Am J Med Genet. 1995; 56(3):252-7.
- Matsuura H, Hatamochi A, Nakamura Y, Endo H, Shinkai H. Multiplepilomatr icomaintrisomy. Dermatology. 2002;204(1):82-3.
- Kurata K, Masahiro M, Yasui Y, et al. A case with multiple pilomatricomas and 9p trisomy due to de novo duplication. Acta Dermatol Kyoto. 1997;92:249-52.
- Blaya B, Gonzalez-Hermosa R, Gardeazabal J, Diaz-Perez JL. Multiple pilomatricoma in association with trisomy 9. Pediatr Dermatol. 2009;26(4):482-4.
- Warrell OA, Cox TM, Firth JD, Benz EJ, editors. Oxford Textbook of Medicine. Vol 2. 3th ed. Oxford: OUP; 2003;305
- Gilaberte Y, Ferrer-LozanoM, Oliván MJ, Coscojuela C, Abascal M, Lapunzina P. Multiple giant pilomatricoma in familial Sotos syndrome. Pediatr Dermatol. 2008;25(1):122-5.
- Mijuskovic ZP, Karadaglic D, Stojanov L. Dermatologic manifestations of Rubinstein-Taybi Syndrome. 2016.
- Cambiaghi S, Ermacora E, Brusasco A, Canzi L, Caputo R. Multiple pilomatricomas in Rubinstein-Taybi syndrome: a case report. Pediatr Dermatol. 1994;11(1):21-5.
- Bayle P, Bazex J, Lamant L, Lauque D, Durieu C, Albes B. Multiple perforating and non perforating pilomatricomas in a patient with ChurgStrauss syndrome and Rubinstein-Taybi syndrome. J Eur Acad Dermatol Venereol. 2004;18(5):607-10.
- Papathemeli D, Schulzendorff N, Kohlhase J, Coppner D, Franke I, Gollnick H. Pilomatricomas in Rubinstein-Taybi Syndrome. J Dtsch Dermatol Ges. 2015;13(3):240-2.
- Sonoda, S. A case of sarcoidosis: Sarcoid reaction in a case of calcifying epithelioma. Rinsho Derma. 1974;16:897.
- Warrell OA, Cox TM, Firth JD, Benz EJ, editors. Oxford Textbook of Medicine. Vol 1. 4th ed. Oxford: OUP; 2003;1466
- Wachter-Giner T, Bieber I, Warmuth-Metz M, Brocker EB, Hamm H. Multiple pilomatricomas and gliomatosis cerebri –a new association? Paediatr Dermatol. 2009;26(1):75-8.