Editorial
Gynecomastia Correction in Individuals with Below Average Skin Elasticity
Jay M Pensler*
Department of Plastic Surgery, Northwestern University Feinberg School of Medicine, USA
*Corresponding author: Jay M Pensler, Department of Plastic Surgery, Northwestern University Feinberg School of Medicine, 680 N Lake Shore Drive Suite, USA
Published: 09 Mar, 2018
Cite this article as: Pensler JM. Gynecomastia Correction
in Individuals with Below Average Skin
Elasticity. Clin Surg. 2018; 3: 1929.
Editorial
Gynecomastia or enlarged breasts in men is a problem attracting increased attention [1-14].
Gynecomastia has been our primary clinical interest for over twenty years. We have fortunately
been able to treat a range of individuals presenting with this deformity. We have on the basis of our
experience continuously refined our surgical approach. Combining the physical resection of the
breast tissue involved in each case of gynecomastia with redistribution of the thoraco-abdominal
skin envelope we have reduced the need for skin resection in patients with below average skin
elasticity.
Between January of 1997 and December of 2017, we have treated two thousand three hundred
and seventeen patients with gynecomastia. Age range of the patients is ten years old to seventynine
years of age. Patients are categorized based on the amount of glandular (breast tissue) present
and the amount of adipose tissue present. A ratio is determined pre-operatively and recorded for
each patient. In addition, the patients’ skin elasticity is recorded as above average, average or below
average. Based on the aforementioned metrics combined with the individual’s Body Mass Index
(BMI) and medical history, a definitive treatment plan is established. Patients with decreased skin
elasticity remain some of the most challenging patients and formed the basis of this report. Over
the aforementioned time period, we have treated six hundred eighty-eight patients with below
average skin elasticity. Virtually all patients require a combination of liposuction and glandular
tissue excision to remove the involved tissue. The remaining component of surgery, (50%) deals
with optimizing the final result. Patients with poor skin elasticity in addition to resection and
liposuction require a specialized treatment strategy to optimize the final result. Skin resection leaves obvious scarring which is irreversible. In an effort to minimize its
requirement for skin resection we have designed a protocol to widely
undermine the skin to facilitate an increased area where skin elasticity
is allowed to interact with the area of resection to optimize the result.
Undermining occurs inferiorly into the mid abdominal area, typically
6cm above the umbilicus in most severe cases. This approach has
reduced the need for skin resection to twenty-nine patients in our
series.
The following patient is illustrative of the technique involved:
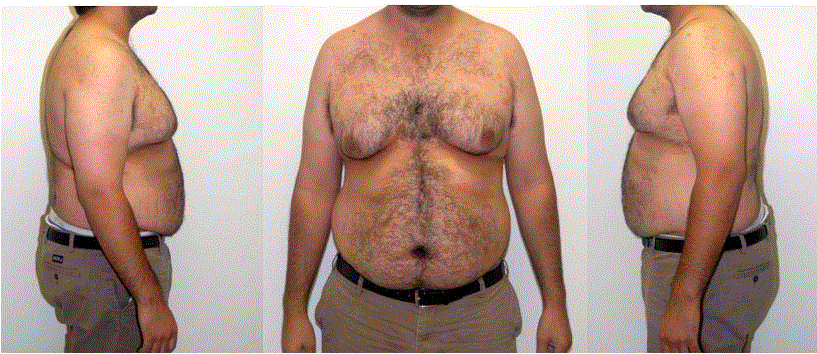
Thirty-five year old Male presents with approximately seventy
percent glandular tissue and thirty percent fat (Figure 1). His skin
elasticity is below average. In addition to resection of glandular tissue
and liposuction of the fat, wide undermining was performed into
the abdomen to approximately half way between the inframammary
crease and the umbilicus to facilitate redistribution of the fat of
the skin and the soft tissue. A compression vest was applied postoperative
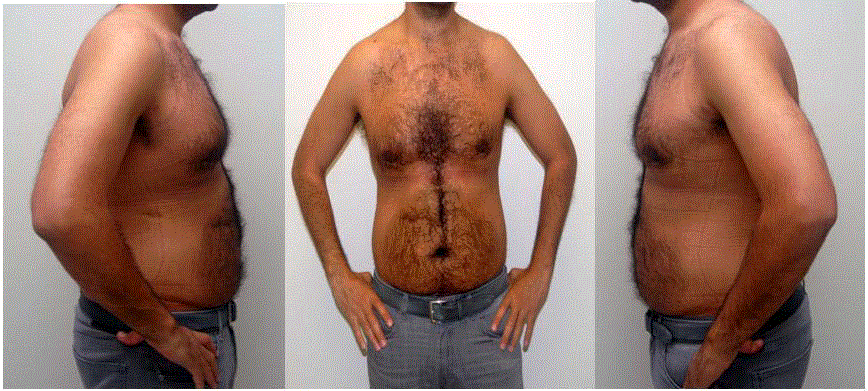
to facilitate healing. The post-operative views illustrate the
resection of the large volume of tissue and an improved redistribution
of the skin (Figure 2). Skin redistribution allows much better contour
of the chest wall which is appreciated from the lateral and anterior
views (Figure 2) in patients with reduced skin elasticity. The increased
degree of undermining facilitates recruitment of a larger skin area to
absorb the laxity present in these patients. Clearly this is not applicable
for massive weight loss patients with tremendous skin laxity and very
poor elasticity. In cases with massive weight loss, a total body lift is
the only option. We have found that in the majority of Gynecomastia
cases with below average skin elasticity, wide undermining and
repositioning of the thoraco-abdominal skin envelope can be effective
in optimizing the final result and avoiding the requirement for skin
resection and the inevitable
Figure 1
Figure 2
References
- Pensler JM, Delgado Jr MA, Yost JM. Plastic Surgery for Gynecomastia. d 2016.
- Devalia HL, Layer GT. Current concepts in gynaecomastia. Surgeon. 2009;7(2):114-9.
- Nydick M, Bustos J, Dale JH Jr, Rawson RW. Gynecomastia in adolescent boys. JAMA. 1961;178:449-54.
- Webster GV. Gynecomastia in the Navy. Mil Surg. 1944;95:375-9.
- Williams GM. Gynecomastia. N Engl J Med. 1993;329(3):209.
- Eckman A, Dobs A. Drug-induced gynecomastia. Expert Opin Drug Saf. 2008;7(6):691-702.
- Morrone N, Morrone Junior N, Braz AG, Maia JA. Gynecomastia: a rare adverse effect of isoniazid. J Bras Pneumol. 2008;34(11):978-81.
- Parker LN, Gray DR, Lai MK, Levin ER. Treatment of gynecomastia with tamoxifen: a double-blind crossover study. Metabolism. 1986;35(8):705-8.
- Parker S. A male breast lesion. Surgical-tutor.org.uk. 2003.
- Pensler JM, Silverman BL, Sanghavi J, Goolsby C, Speck G, Brizio-Molteni L, et al. Estrogen and progesterone receptors in gynecomastia. Plast Reconstr Surg. 2000;106(5):1011-3.
- Simon BE, Hoffman S, Kahn S. Classification and surgical correction of gynecomastia. Plast Reconstr Surg. 1973;51(1):48-52.
- Yost M. Demystifying Gynecomastia: Men with Breasts. Mens Health. 2006;1:1-122.
- Singer-Granick CJ, Granick MS. Gynecomastia what the surgeon needs to know. Eplasty. 2009;9:e6.
- Athwal RK, Donovan R, Mirza M. Clinical examination allied to ultrasonography in the assessment of new onset gynaecomastia: an observational study. J Clin Diagn Res. 2014;8(6):NC09-11.