Editorial
Persistent Groin Pain after Urogynecologic Surgery
Michael Ting1*, Sonya Ephraim2 and Vincent Lucente2
1Department of Obstetrics and Gynecology, St. Luke’s University Hospital, Pennsylvania, USA
2Department of Obstetrics and Gynecology, Institute for Female Pelvic Medicine and Reconstructive Surgery,
Pennsylvania, USA
*Corresponding author: Michael Ting, Department of Obstetrics and Gynecology, St. Luke’s University Hospital, Allentown, 18103, Pennsylvania, USA
Published: Editorial
Cite this article as: Ting M, Ephraim S, Lucente
V. Persistent Groin Pain after
Urogynecologic Surgery. Clin Surg.
2018; 3: 1922.
Editorial
Pelvic Organ Prolapse (POP) and Stress Urinary Incontinence (SUI) commonly occur in today’s
older yet active women [1]. Symptoms that arise from these conditions can dramatically lower a
woman’s quality of life and herself esteem [2]. The most definitive treatment for both POP and
SUI is surgical correction. A worrisome complication of any urogynecological reconstructive pelvic
surgery is postoperative pain continuing beyond the expected twelve week convalescent period [3].
Postoperative groin pain can be challenging to both evaluate and effectively manage. In addition to
the physical discomfort, the patient is often distressed by her physician being unsure of the etiology
of her groin pain and therefore unable to completely treat her symptoms. Such persistent pain can
occur after native tissue reconstructive surgeries as well as those utilizing synthetic mesh implants
with a reported rate of 9.5% to 15.6% respectively even up to a year after the patient’s index surgery
[4,5]. Unfortunately due to the widespread plaintiff lawyer solicitation of “mesh complications”
both patients and implanting surgeons become erroneously convinced that the mesh implant itself
is causing the groin pain. The medial compartment of the thigh is often overlooked during the
evaluation of patients with chronic “pelvic” pain after surgery. This medial compartment of the
thigh, also commonly referred to as the groin, consists of ligaments, tendons, muscles and fascia.
All of these structures attach to the pubic bone and assist with hip flexion, extension, and rotation.
It is important to note that the abdominal muscles of the trunk also attach to the pubic bone. As
a result of this complex anatomical arrangement, the groin functions as a “central hub” linking
the muscles of the abdominal wall with those of the ipsilateral lower extremity. During prolonged
extensive reconstructive pelvic surgery in the dorsal lithotomy position, or when the hips can be
slightly hyperflexed during some portion of the surgery (i.e. Midurethral sling procedures), microtears
can occur in the ligaments, tendons, and muscles located in the groin. These tears can lead to a
weakening in the afflicted structures and compromise the stability of the pelvis. When other muscles
try to provide compensatory stability, additional micro-tears will occur to create a cycle of chronic
groin pain which can also radiate up towards the abdomen, down the inner aspect of the thigh, or
across laterally towards the inferior aspect of the anterior inferior iliac spine. In some cases, this pain
caused by localized inflammation from these micro-tears is misinterpreted as an “inflammatory
response” to synthetic implants used in urogynecologic procedures. Primary excisional surgery
to remove implanted transvaginal mesh to treat such chronic groin pain as a result of these soft
tissue injuries will more often prove to be unsuccessful [6]. The groin pain caused from these micro
tears can be of insidious onset, slowly progressing over several months. A thorough history with
a detailed description of the pain complaint including timing of onset, the nature of the pain,
exacerbating and alleviating factors, radiation of pain, and daily pain “cycle” is paramount for
proper diagnosis. Usually the reported discomfort is similar to patients suffering with enthesopathy
or tendonitis. Patients complain of pain that is unilateral, often “pulling” or sharp in nature that
progresses to a consistent dull ache as the pain persists beyond the normal recovery period. Due
to the interconnectivity of the groin musculature, the discomfort can radiate to surrounding areas
like the lower hip, lower abdomen, proximal thigh, and the vagina. Patients can typically sleep
fairly comfortably through the night but may experience extreme pain trying to get out of bed.
Although the symptoms may partially resolve with periods of rest, the pain will return with activity
and is exacerbated by strenuous exercise. On physical exam, several maneuvers can be performed to
confirm that the patient’s pain truly originates from the groin. Palpation along the inguinal ligament
often reproduces the pain symptoms reported by the patient. Typically the pain can also be elicited
on resisted hip flexion, resisted adduction of the thighs, and full passive abduction of the thighs. Since
the pubic tubercle serves as an attachment point for most of the tendons and associated muscles in
the groin, a careful examination of this bony prominence should be completed. One finger deep
palpation right over the lateral aspect of the pubic tubercle usually results in the patient expressing acute discomfort. Although rare, the existence of a concomitant
neuropathy should be evaluated, especially an injury to the Obturator
nerve [7]. Obturator neuropathy is often associated with adductor
muscle weakness (inability to bring the leg from a lateral to midline
position), muscle spasm, and paresthesia over the medial aspect of the
distal thigh. The Institute for Female Pelvic Medicine is a nationally
recognized center for transvaginal mesh procedures and pelvic
reconstructive surgery; therefore patients are commonly referred to
the Institute for persistent groin pain possibly related to previous
pelvic surgeries. If the patient’s history and physical exam isolates the
pain to the groin, our initial approach utilizes a trigger point injection
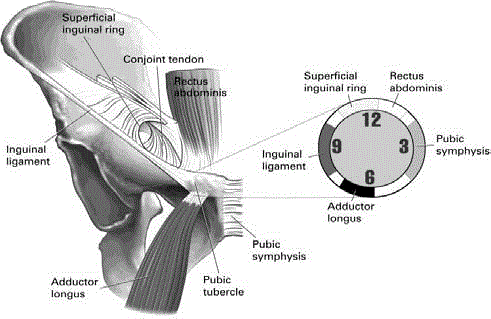
which is both diagnostic and therapeutic. First the pubic tubercle
is identified and a slow palpation is performed around the tubercle
in a clockwise fashion to identify the point(s) of pain and anatomic
structures involved [8] (Figure 1). Next the skin over the tubercle is
appropriately cleansed. Since the pubic tubercle is fairly superficial
in most patients, the injection is not deep. The needle is then angled
towards the direction of the affected muscle, ligament, or tendon
followed by slow injection of a Steroid/anesthetic solution (2 cc of
Sensorcaine 0.5% mixed with 1 cc of Depo Medrol 40 mg/ml in 10
cc syringe). Typically a total volume of 3 cc is injected or 1 cc at each
trigger point if multiple points are identified. Patients will typically
feel immediate relief from their groin pain after the injection followed
by a slower period of pain resolution. If a patient demonstrates only
a partial response the injection is repeated in 4 to 6 weeks until their
symptoms are minimized. In between injections pelvic rest, ice and
deep massage to the trigger point area are recommended. A 7 to 10
day course of NSAIDs is also recommended to decrease baseline
inflammation. A physical therapy program consisting of isometric
exercises to strengthen the hip stabilizing muscles and proprioceptive
training should be started. No increase in pain should be experienced
during or after the exercises in order for the affected tissues to heal
appropriately.
If a patient reports no abatement from their discomfort after
the initial two injections, radiologic studies are used to investigate
other etiologies of groin pain since the history and physical exams
are similar amongst the various groin pathologies. Radiologic
studies may confirm the findings on physical exam and provide a
definitive diagnosis for a patient’s persistent postoperative groin
pain. Ultrasound is the first-line imaging modality owing to its
greater availability. Dynamic evaluation of structures with muscle
contraction, joint movement, or position change of the patient
may also add significant information that may not be obtainable
with static MRI [9]. However given the anatomic complexity of
the groin, MRI is currently regarded as the gold standard imaging
modality [10]. In some cases, a multidisciplinary team approach
may be needed to address the groin pain completely. Neurology
consultation for suspected nerve involvement is crucial. A general
surgeon can evaluate for a previously undiagnosed inguinal hernia.
Other specialists may be needed depending on the imaging findings.
Unless a concomitant material exposure or extrusion is present,
excisional surgery to remove any vaginal mesh implants for groin
pain is reserved until other etiologies are investigated and excluded.
Acknowledgment
Dr. Lucente serves as an expert witness for Bard, receives research support, and is a surgical preceptor as well as a consultant for Coloplast and Boston Scientific. Dr. Lucente receives research support and is a consultant for A Cell.
Figure 1
References
- Nygaard I, Bradley C, Brandt D; Women's Health Initiative. "Pelvic organ prolapse in older women: prevalence and risk factors". Obstet Gynecol. 2004;104(3):489-97.
- Jelovsek JE, Barber MD. "Women seeking treatment for advanced pelvic organ prolapse have decreased body image and quality of life". Am J Obstet Gynecol. 2006;194(5):1455-61.
- Vonk Noordegraaf A, Huirne JA, Brölmann HA, van Mechelen W, Anema JR. Multidisciplinary convalescence recommendations after gynaecological surgery: a modified Delphi method among experts. BJOG. 2011;118(13):1557-67.
- Oversand SH, Staff AC, Spydslaug AE, Svenningsen R, Borstad E. "Long-term follow-up after native tissue repair for pelvic organ prolapse". Int Urogynecol J. 2014;25(1):81-9.
- Geller EJ, Babb E, Nackley AG, Zolnoun D. "Incidence and risk factors for pelvic pain after mesh implant surgery for the treatment of pelvic floor disorders". J Minim Invasive Gynecol. 2017;24(1):67-73.
- Crosby EC, Abernethy M, Berger MB, DeLancey JO, Fenner DE, Morgan DM. "Symptom resolution after operative management of complications from transvaginal mesh". Obstet Gynecol. 2014:123(1):134-9.
- Cardosi RJ, Cox CS, Hoffman MS. "Postoperative neuropathies after major pelvic surgery". Obstet Gynecol. 2002;100(2):240-4.
- Falvey EC, Franklyn-Miller A, McCrory PR. "The groin triangle: a patho-anatomic approach to the diagnosis of chronic groin pain in athletes". Br J Sports Med. 2009;43(3):213-20.
- Kälebo P, Karlsson J, Swärd L, Peterson L. "Ultrasonography of chronic tendon injuries in the groin". Am J Sports Med. 1992;20(6):634-9.
- Lee SC, Endo Y, Potter HG. "Imaging of Groin Pain: Magnetic Resonance and Ultrasound Imaging Features". Sports Health. 2017;9(5):428-35.