Research Article
Comparison of Wear Rate between Ceramic on Ceramic, Metal on Highly Cross-Linked Polyethylene and Metal on Metal Bearings: A 5-10-Year Follow-Up Study
Yoshitoshi Higuchi*, Taisuke Seki, Daigo Morita, Daigo Komatsu, Takehiro Kasai, Yasuhiko Takegami and Naoki Ishiguro
Department of Orthopedic Surgery, Nagoya University Graduate School of Medicine, Japan
*Corresponding author: Yoshitoshi Higuchi, Department of Orthopedic Surgery, Nagoya University Graduate School of Medicine, 65 Tsurumai-cho, Showa-ku Nagoya, 466- 8550, Japan
Published: 16 Feb, 2018
Cite this article as: Higuchi Y, Seki T, Morita D, Komatsu D,
Kasai T, Takegami Y, et al. Comparison
of Wear Rate between Ceramic on
Ceramic, Metal on Highly Cross-Linked
Polyethylene and Metal on Metal
Bearings: A 5-10-Year Follow-Up Study.
Clin Surg. 2018; 3: 1915.
Abstract
Currently, there is a lack of evidence on the medium-term follow-up of cementless total hip
arthroplasty (THA) using metal-on highly cross-linked polyethylene bearing (MoP), ceramic on
ceramic bearing (CoC), and metal on metal (MoM) bearings at more than 5 years follow-up. Our
aim was to calculate the 5 to 10-year wear rate and incidence rate of osteolysis for three types of
THAs.
Seventy-seven patients (68 women, 9 men) underwent MoP THAs, 105 (85 women, 20 men)
underwent CoC THAs and 55 (11 women, 44 men) underwent MoM THAs. The average patient
age at the time of surgery was 64.7, 55.9, and 59.9 years in the MoP, CoC, and MoM THA groups,
respectively. Clinical and radiologic measurements at a mean follow-up of 7.6 years (range, 5 to
10 years) were analyzed. The mean postoperative Harris hip scores showed no difference among
the groups. The mean annual liner wear rates were 0.0160, 0.0040 and 0.0054 mm/year in MoP,
CoC and MoM THAs, with that of CoC THAs being significantly lower than the others. Osteolysis
(14.5%) among MoM THAs was significantly more frequently observed compared with MoP and
CoC THAs. Kaplan-Meier survival at 10 years with regard to implant loosening, or revision THA as
the endpoint, was 96.1% (95% CI: 88.4 to 98.7) for MoP, 98.6% (95% CI: 90.3 to 98.6) for CoC, and
98.2% (95% CI: 88.0 to 99.7) for MoM (p=0.360). Excellent clinical and radiological outcomes were
obtained for MoP and CoC of bearings.
Keywords: Ceramic on ceramic bearing; Metal on highly cross-linked polyethylene bearing;
Metal on metal bearings; Total hip arthroplasty; Wear
Introduction
The primary goal of Total Hip Arthroplasty (THA) is to provide the patientwith end-stage
osteoarthritis of the hip with a long-lasting, pain free [1,2]. However, with improved implant
designs and surgical techniques, aseptic loosening and osteolysis due to particulate debris generated
by conventional polyethylenehave become a major limitation to prosthetic long-term survivorship
[3-6]. Osteolysis has been reported in up to 60% of young active patients with conventional
polyethylene [6]. In an attempt to avoid problems caused by wear debris, different bearing surfaces
have been developed, such as metal-on-highly cross-linked polyethylene (MoP) which is intended
to reduce linear and volumetric wear than conventional polyethylene [3,4,6,7]. Similarly, hard
bearing surfaces which produce even less volumetric wear, such as ceramic-on-ceramic (CoC) and
metal-on-metal (MoM), have also been developed to address the problem of osteolysis.
However, they have their own inherent limitations, such as ceramic fracture and squeaking, or
adverse local tissue reaction (ALTR) [1,2,6,8]. In the last two decades, several systematic reviews
and a number of clinical randomized controlled trials, comparing the survivorship of THA implants
with different bearing surfaces, have been published. However, the results of these studies are
inconsistent and continue to be debated [2,6,8-11].
Therefore, the aim of our study was to perform a retrospective evaluation of the clinical and
radiographic outcomes between MoP, CoC and MoM cementless THAs over a 5 to 10-year followup
to compare the wear rate and the incidence of osteolysis.
Figure 1
Figure 1
Cementless components used in this study.
1(A) Metal on highly cross-linked polyethylene bearing.
1(B) Ceramic on Ceramic bearing.
1(C) Metal on Metal bearing.
Figure 2
Figure 2
Digitized AP-view radiographs using the computer-digitizer facilities
of the roman V1.70 software (Institute of Orthopaedics, Oswestry, UK) were
obtained to determine femoral head penetration into the liners.
2(A) Metal on highly cross-linked polyethylene bearing.
2(B) Ceramic on Ceramic bearing.
2(C) Metal on Metal bearing.
Materials and Methods
Patient selection
Between August 2007 and December 2011, we performed
consecutive primary CoC, MoP, or MoM THAs, with the type
selected based on the recommendation of the senior surgeon
performing the procedure. In total, 220 patients (237 THAs), who
completed a minimum follow-up period of 5 years, were eligible for
the study. The exclusion criteria were: death from causes unrelated to
surgery (1 patient; 1 joint), patient inaccessibility (5 patients moved
abroad; 5 joints) and Crowe group III/IV hips (3 patients; 3 joints).
No significant differences were noted between the groups with regard
to sex, body mass index, or diagnosis. (Table1) However, patient age
at surgery for the group who received CoC THAs was significantly
lower than that for the other groups. Informed consent was obtained
from all patients, and the study was approved by the ethics committee
of our hospital.
A posterolateral approach was used for all procedures, with
patients in the lateral decubitus position. The socket was fixed in
the acetabulum using an acetabular alignment guide, with a target
acetabular position of 20° of anteversion and 45° of inclination [12].
Acetabular and femoral components
Acetabular and femoral components used for MoP and CoC
THAs were manufactured by Stryker Orthopaedics (Mahwah, NJ),
while those for MoM were from Depuy Orthopaedics (Warsaw,
IN; Figure 1; Table 1). The Crossfire Polyethylene Insert (Stryker
Orthopaedics) wasused for all cases in which a highly cross-linked
polyethylene liner was implanted, with the BIOLOX® forte (Ceramtec,
Plochingen, Germany) used as a ceramic liner and head. The diameter
of the cobalt chrome head and of the ceramic head used is provided
in Table 1.
Data collection
Patients’ clinical data, including the Harris hip score (HHS), were
prospectively recorded by a senior surgeon at 1 month prior to THA,
at 6 months and 1 year post-THA, and then annually, up to the endpoint
of follow-up. These data were then retrospectively extracted
from patients’ medical records for analysis.
Radiographs of the hips were obtained in the standard
anteroposterior (AP) view, with both hips in neutral rotation and
0° abduction, and in the Lauenstein (frog position) view, with the
patient in the supine position and the hips in 45° abduction [7,13].
Radiographs were obtained at 3 months postoperatively and then
annually to the last follow-up.
Definite loosening of the femoral component was defined as a
progressive axial subsidence of more than 3 mm or a varus or valgus
shift [14]. Definite loosening of the acetabular component was
defined as a change in the vertical and/or medial position of >2 mm
or presence of a continuous radiolucent line >2 mm in width on both
AP and Lauenstein-view radiographs [15]. Osteolysis was defined
as areas of endosteal, intracortical or cancellous bone destruction of
>2 mm, that were non-linear and were progressive [16]. Acetabular
inclination was measured using the trans-ischial line as a reference,
and anteversion was measured from digitized AP radiographs,
using the method of Lewinnek et al. [12,17]. Using the methods of
Dorr et al. [6,11,18], penetration of the femoral head into the liner
was measured from digitized AP and Lauenstein-view radiographs
(Figure 2), by two surgeons using the Roman software (V1.70,
Institute of Orthopaedics, Oswestry, UK).
Femoral head penetration was measured at annual intervals
to calculate the rate of wear, true wear and creep. The true wear
represented the steady-state linear wear rate and creep represented
a measure of the early head penetration that can be attributed to
“running-in” wear as well as polyethylene creep and deformation [5].
Wear rate was calculated by dividing total femoral head penetration
at the end-point of observation by the number of years of follow-up.
Linear regression models of femoral head penetration over time were
constructed, with the y-intercept providing the creep rate and the slope
of the line the true wear rate [11,19]. Intraclass correlation coefficients
(ICCs) were calculated and used to determine inter-observer
reliability regarding the measurement of femoral head penetration.
In the MoM group, patients underwent magnetic resonance imaging
(MRI) when indicated, based on clinical symptoms, including hip
pain or discomfort of the hip and concern for ALTR.
Statistical analysis
Statistical analyses were performed using SPSS version 21 (IBM
Corp., Armonk, NY) and EZR (Saitama Medical Center, Jichi Medical
University). Between-group differences were evaluated using an
analysis of variance (ANOVA), Tukey’s test, Pearson’s chi-squared
test, Holm-Bonferroni methods and log-rank test as appropriate. A
p-value < 0.05 was considered statistically significant.
Table 1
*: CoC THAs vs. MoM THAs P< 0.001
†: CoC THAs vs. MoP THAs P< 0.001
BMI: Body mass index
NA: Not available
All values given as the mean and standard deviation
Figure 3
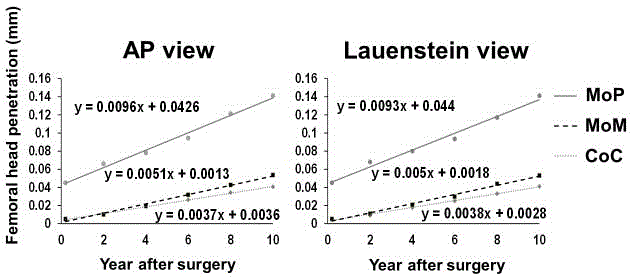
Figure 3
Linear regression for mean femoral head penetration over time in the CoC THA and MoM and MoP THA groups. The slope and intercept are considered
to represent true wear and creep, respectively.
CoC: ceramic on ceramic; MoP: metal on highly cross-linked polyethylene
MoM: metal on metal; AP: anteroposterior
Table 2
HHS: Harris hip score
*: CoC THAs vs. MoM THAs: P< 0.001
†: MoM THAs vs. MoP THAs: P< 0.05
‡: CoC THAs vs. MoM THAs: P< 0.05
All values given as the mean and standard deviation
Results
Clinical results
The mean postoperative HHS was 85.3, 89.9 and 90.3 among
MoP, CoC and MoM THAs, respectively (p=0.063; Table 2). Neither
the incidence of dislocation nor heterotopic bone formation differed
between three groups (Table 3). All 5 dislocations were successfully
treated conservatively by using single closed reduction, with no
recurrence noted. All joints were classified as Brooker class 1; the
patients showed no symptoms, and were treated conservatively [20].
There was no ceramic fracture among CoC THAs (Table 3).
One joint among MoP THAs (1.3%) required revision THA due
to aseptic loosening of the cup. One joint (0.9%) among CoC THAs
required revision THA due to progressive femoral osteolysis caused
by femoral neck impingement on the elevated acetabular metal liner.
There was no revision THA among MoM THAs.
One joint (0.9%) among CoC THAs exhibited audible squeaking;
because it was painless, revision THA was not required. No incidence
of deep infection or pulmonary embolism was identified in either
group. One incidence of deep vein thrombosis (DVT) was identified
among MoP THAs was found deep vein thrombosis (DVT); however,
there was no DVT in CoC and MoM THA groups.
The Kaplan-Meier survival curve at 10 years, using implant
loosening or revision THA as the endpoint of analysis, was 96.1%
(95% CI, 90.0 to 99.3) for the MoP group, and 98.6% (95% CI, 90.3 to
98.6) for the CoC group and 98.2% (95% CI: 88.0 to 99.7) for MoM
THAs, which was not significantly different between the groups
(p=0.360).
Radiographic results
Neither the anteversion nor inclination of the acetabular
component position differed between the three THA groups (Table
2).The incidence rate of osteolysis was greater for MoM THAs than
either MoP (p < 0.05) or CoC (p < 0.001) THAs (Table 3). Although
no joints among CoC THAs showed aseptic loosening, 2 joints (2.6%)
among MoP THAs showed loosening, with one of these cases (1.3%)
requiring revisionbecause of progression of loosening. In contrast,
one joint (1.8%) among MoM THAs showed aseptic cup loosening
(Table 3). MRI was performed on a total of 10 hips (18.2%). A
pseudocystic tumor was identified in four hips; as symptoms were
minimal, revision THA was not required.
The wear rate
Femoral head penetration could not be measured in 8 joints
among patients with a CoC THA and 2 joints among patients with
a MoM THA because the margin of the femoral head could not be
identified clearly in these joints. Thus, measures of femoral head
penetration were obtained for 97 and 53 joints among patients with
a CoC and MoM THA, respectively. The ICC of measurement was
0.737 (95% CI: 0.16 to 0.982, p=0.0043) for CoC, 0.876 (95% CI:
0.490 to 0.977, p=0.002) for MoP and 0.761 (95% CI: 0.203 to 0.958,
p=0.001) for MoM THAs.
The wear rate was significantly lower for CoC and MoM THAs
compared to MoP THAs, irrespective of the radiographic view (AP
and Lauenstein, p < 0.0001). In addition, the wear rate was significantly
lower for CoC than MoM THAs on AP-view radiographs, while the
wear rate in the Lauenstein-view showed no difference between CoC
and MoM THAs (Table 4).
The creep rate for CoC THAs was 0.0036 mm/year on AP-view
radiographs and 0.0028 mm/year on Lauenstein-view radiographs.
Conversely, the creep rate for MoP THAs was 0.0426 mm on AP-view
radiographs and 0.0440 mm on Lauenstein-view radiographs (Figure
3). The creep rate for MoM THAs was 0.0013 mm/year on AP-view
radiographs and 0.0018 mm/year on Lauenstein-view radiographs.
The true wear rate for MoP THAs was 0.0096 mm/year on
AP-view radiographs and 0.0093 mm/year on Lauenstein-view
radiographs, while the rate for CoC was 0.0037 mm/year on AP-view
radiographs and 0.0038 mm/year on Lauenstein-view radiographs.
Conversely, the true wear rate for MoM THAs was 0.0051 mm/year
on AP-view radiographs and 0.0050 mm/year on Lauenstein-view
radiographs.
Table 3
THA: Total hip arthroplasty
DVT: Deep vein thrombosis
PE: Pulmonary embolism
Table 4
‡: CoC THAs vs. MoM THAs: P< 0.05
§: CoC THAs vs. MoP THAs: P< 0.001
¶: MoM THAs vs. MoP THAs: P< 0.001
All values given as mean and Standard Deviation (SD).
Discussion
The main reason for failure of THA with conventional
polyethylene is bearing surface wear and the resultant wear-induced
osteolysis, which can result in implant loosening and failure [8,9,21].
Therefore, modern materials with improved wear characteristics,
such as metal, ceramics, and highly cross-linked polyethylene, have
been implanted worldwide for use in THA [9,21-23].
Previous studies have shown that survival with aseptic loosening
at the midterm follow-up do not differ significantly between CoC and
MoP THAs [6,10]; however, few studies have compared midterm
outcomes between MoP, CoC, and MoM THA, without a metaanalysis
being available [24]. In our study, we found that the survival
rates at the 10years with regard to implant loosening or revision
THA did not differ significantly between the three types of THAs.
However, MoM significantly increased the risk of osteolysis than CoC
and MoP THAs.
Previous studies reported a mean liner wear rate of 0.01 to 0.059
mm/year for MoP THAs, measured from AP-view radiographs
[5,6,25,26]. In contrast, the mean liner wear rate for CoC THAs was
0.00183 to 0.0067 mm/year on AP-view radiographs [6,27].The in
vitro wear of CoC and MoM components was below 0.1 mm3/million
cycles and 1.0 mm3/million cycles, respectively [28]. Thus, our results
are fairly consistent with those of previous reports, in that the wear
rate for CoC THAs was roughly 25% of the rate for MoP THAs. The
wear rate for MoM THAs was around one-third of that for MoP
THAs.
The true wear rate for MoP THAs was previously reported to be
0.006 mm/year [19]. However, to the best of our knowledge, the true
wear rate for MoM THAs has not been reported thus far. The true
wear rate of CoC THAs in our previous study was around 50% of
that of MoP THAs. Since the creep represents ‘bedding in’, the true
wear rate differed less than the wear rate between the three types of
THAs [11].
The overall THA survivorship was high for both groups, with no
significant between-group difference. The wear rates of MoM and
CoC THAs were significantly lower than that of MoP THAs. However,
MoM THAs exhibited more frequent osteolysis and demonstrated a
significantly higher risk of revision than CoC and MoP THAs [24].
Thus, excellent clinical and radiological outcomes were obtained for
CoC and MoP THAs. Longer-term studies are needed to determine
the effect of the wear rate and true wear rate on implant longevity.
This study has some limitations. First, our study is retrospective
in nature, with a relatively small number of patients. As well, the
analysis was based on consecutive cases, with no randomization and
no power analysis performed to determine if sufficient patients were
included to detect clinically meaningful differences between groups.
Patients who received CoC THAs were significantly younger than
patient in the other groups. This might have been caused by selection
bias and might have affected the clinical and radiographic results.
Second, we measured femoral head penetration using the technique
described by Dorr along with the computer-digitizer facilities of the
Roman V1.70 software. The validity of this method for measuring
femoral head penetration following CoC THA has been previously
reported [6,11,19]. However, validation of MoM THA has never been
reported. This method, which is typically used to examine femoral
head penetration following MoP THA, is not easily applicable for
CoC and MoM THA. Third, we could not analyze the metal artifact
reduction sequence MRI and serum metal ion levels for all patients
with MoM THAs and could not identify an objective causative factor
of osteolysis. Further studies are needed to clarify the association
between bearing type and osteolysis.
Conclusion
Although CoC and MoM THA had a lower wear rate than MoP THAs, three types of THAs provided good implant survivorship. However, osteolysis among MoM THAs was more frequently observed compared to MoP and CoC THAs. Studies that span a longer follow up period are needed to better understand the effects of wear rate and material bioactivity on implant longevity.
References
- D'Antonio JA, Capello WN, Naughton M. Ceramic bearings for total hip arthroplasty have high survivorship at 10 years. Clin Orthop Relat Res. 2012;470(2):373-81.
- Shetty V, Shitole B, Shetty G, Thakur H, Bhandari M. Optimal bearing surfaces for total hip replacement in the young patient: a meta-analysis. Int Orthop. 2011;35(9):1281-7.
- Callary SA, Solomon LB, Holubowycz OT, Campbell DG, Munn Z, Howie DW. Wear of highly crosslinked polyethylene acetabular components. Acta Orthop. 2015;86(2):159-68.
- D'Antonio J, Capello W, Manley M, Bierbaum B. New experience with alumina-on-alumina ceramic bearings for total hip arthroplasty. J Arthroplasty. 2002;17(4):390-7.
- Engh CA, Stepniewski AS, Ginn SD, Beykirch SE, Sychterz-Terefenko CJ, Hopper RH, et al. A randomized prospective evaluation of outcomes after total hip arthroplasty using cross-linked marathon and non-cross-linked enduron polyethylene liners. J Arthroplasty. 2006;21(6):17-25.
- Nikolaou VS, Edwards MR, Bogoch E, Schemitsch EH, Waddell JP. A prospective randomised controlled trial comparing three alternative bearing surfaces in primary total hip replacement. J Bone Joint Surg Br. 2012;94(4):459-65.
- Takao M, Ohzono K, Nishii T, Miki H, Nakamura N, Sugano N. Cementless modular total hip arthroplasty with subtrochanteric shortening osteotomy for hips with developmental dysplasia. J Bone Joint Surg Am. 2011;93(6):548-55.
- Milošev I, Kovač S, Trebše R, Levašič V, Pišot V. Comparison of ten-year survivorship of hip prostheses with use of conventional polyethylene, metal-on-metal, or ceramic-on-ceramic bearings. J Bone Joint Surg Am. 2012;94(19):1756-63.
- Wyles CC, Jimenez-Almonte JH, Murad MH, Norambuena-Morales GA, Cabanela ME, Sierra RJ, et al. There are no differences in short- to mid-term survivorship among total hip-bearing surface options: a network meta-analysis. Clin Orthop Relat Res. 2015;473(6):2031-41.
- Bascarevic Z, Vukasinovic Z, Slavkovic N, Dulic B, Trajkovic G, Bascarevic V, et al. Alumina-on-alumina ceramic versus metal-on-highly cross-linked polyethylene bearings in total hip arthroplasty: a comparative study. Int Orthop. 2010;34(8):1129-35.
- Higuchi Y, Hasegawa Y, Seki T, Komatsu D, Ishiguro N. Significantly lower wear of ceramic-on-ceramic bearings than metal-on-highly cross-linked polyethylene bearings: a 10- to 14-year follow-up study. J Arthroplasty. 2016;31(6):1246-50.
- Kanoh T, Hasegawa Y, Masui T, Yamaguchi J, Kawabe K, Ishiguro N. Accurate acetabular component orientation after total hip arthroplasty using an acetabular alignment guide. J Arthroplasty. 2010;25(1):81-6.
- Mestriner MB, Verquietini CMA, Waisberg G, Akkari M, Fukunaga ET, Santili C. Radiographic evaluation in epiphysiolysis: possible predictors of bilaterality? Acta Ortop Bras. 2012;20(4):203-6.
- Kim YH, Kim J-S, Oh SH, Kim JM. Comparison of porous-coated titanium femoral stems with and without hydroxyapatite coating. J Bone Joint Surg Am. 2003;85(9):1682-8.
- Sutherland CJ, Wilde AH, Borden LS, Marks KE. A ten-year follow-up of one hundred consecutive Müller curved-stem total hip-replacement arthroplasties. J Bone Joint Surg Am. 1982;64(7):970-82.
- Lee JH, Lee BW, Kim SY. Midterm results of primary total hip arthroplasty using highly cross-linked polyethylene minimum 7-year follow-up study. J Arthroplasty. 2011;26(7):1014-9.
- Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR. Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am. 1987;60(2):217-20.
- Barrack RL, Lavernia C, Szuszczewicz ES, Sawhney J. Radiographic wear measurements in a cementless metal-backed modular cobalt-chromium acetabular component. J Arthroplasty. 2001;16(7):820-8.
- García-Rey E, García-Cimbrelo E, Cruz-Pardos A, Ortega-Chamarro J. New polyethylenes in total hip replacement: a prospective, comparative clinical study of two types of liner. J Bone Joint Surg Br. 2008;90(2):149-53.
- Brooker AF, Bowerman JW, Robinson RA, Riley LH. Ectopic ossification following total hip replacement. Incidence and a method of classification. J Bone Joint Surg Am. 1973;55(8):1629-32.
- Cai P, Hu Y, Xie J. Large-diameter delta ceramic-on-ceramic versus common-sized ceramic-on-polyethylene bearings in THA. Orthopedics. 2012;35(9):e1307-13.
- Gallo J, Goodman SB, Lostak J, Janout M. Advantages and disadvantages of ceramic on ceramic total hip arthroplasty: a review. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2012;156(3):204-12.
- Lombardi AV, Mallory TH, Cuckler JM, Williams J, Berend KR, Smith TM. Mid-term results of a polyethylene-free metal-on-metal articulation. J Arthroplasty. 2004;19(7):42-7.
- Yin S, Zhang D, Du H, Du H, Yin Z, Qiu Y. Is there any difference in survivorship of total hip arthroplasty with different bearing surfaces? A systematic review and network meta-analysis. Int J Clin Exp Med. 2015;8(11):21871-85.
- Capello WN, D'Antonio JA, Ramakrishnan R, Naughton M. Continued improved wear with an annealed highly cross-linked polyethylene. Clin Orthop Relat Res. 2011;469(3):825-30.
- Reynolds SE, Malkani AL, Ramakrishnan R, Yakkanti MR. Wear analysis of first-generation highly cross-linked polyethylene in primary total hip arthroplasty: an average 9-year follow-up. J Arthroplasty. 2012;27(6):1064-8.
- Epinette JA, Manley MT. No differences found in bearing related hip survivorship at 10-12 years follow-up between patients with ceramic on highly cross-linked polyethylene bearings compared to patients with ceramic on ceramic bearings. J Arthroplasty. 2014;29(7):1369-72.
- Al-Hajjar M, Fisher J, Tipper JL, Williams S, Jennings LM. Wear of 36-mm BIOLOX (R delta ceramic-on-ceramic bearing in total hip replacements under edge loading conditions. Proc Inst Mech Eng Part H. 2013;227(5):535-42.