Case Report
Laparoscopic Mesh Technique as Surgical Treatment for an Abdomino-Perineal Amputation Postoperative Perineal Hernia, To Flap or Not?
Torres Villachica J, Guevara Martínez J and Cantero Cid R*
Department of General Surgery, La Paz University Hospital, Spain
*Corresponding author: Ramon Cantero, Department of General Surgery, La Paz University Hospital, Madrid, Spain
Published: 09 Jan, 2018
Cite this article as: Torres Villachica J, Guevara Martínez
J, Cantero Cid R. Laparoscopic Mesh
Technique as Surgical Treatment for
an Abdomino-Perineal Amputation
Postoperative Perineal Hernia, To Flap
or Not?. Clin Surg. 2018; 3: 1902.
Abstract
Perineal hernia is a rare but well-known complication after major pelvic surgery such as abdominoperineal amputation. There are several surgical approaches for the repair of this defect, such as transabdominal (laparoscopic or open), transperineal or combined. We present a case in which we expose some important aspects to consider whether or not we should perform a peritoneal flap in the laparoscopic approach with nonabsorbable visceral contact mesh placement as a surgical treatment of the perineal incisional hernia in a patient operated previously of an abdomino-perineal laparoscopic amputation due to adenocarcinoma of the rectum. We believe that this technique offers good results and is an effective alternative approach to the transabdominal and transperineal open approaches.
Introduction
Postoperative perineal hernia can be defined as the protrusion of the intraabdominal viscera through a defect in the pelvic floor to the perineal region [1-3]. It can occur spontaneously, following a perineal trauma or after an abdominoperineal resection, sacrectomy or pelvic exenteration [4]. Very little is known about spontaneous perineal hernia. These are infrequent complications of abdominoperineal operations with a prevalence of 0.34% [5] and an incidence of up to 7% [6]. Several approaches have been described for the repair of perineal hernias that include open, transperineal or combined transabdominal abdominoperineal repairs. The most common symptoms are pain and a feeling of stretch or discomfort when standing up, but urinary symptoms, bowel obstruction or deterioration of the skin of the perineum may also occur. Several approaches have been described for the repair of perineal hernias that include transabdominal, transperineal or open combined abdominoperineal repairs [2,4-8]. The laparoscopic transabdominal techniques of perineal hernias are not well described in the medical literature to date [4]. Concerns about the insertion of intra-abdominal meshes to close peritoneal defects are mainly based on the risk of adhesions, mesh bacteria colonization, and the potential for fistula formation [2]. This, however, is attenuated by the development of new synthetic meshes used in the increasingly popular repair technique of laparoscopic incisional hernias [2]. There are studies in which there is evidence of a reduction in the incidence of morbidity related to the mesh and facilitate a minimally invasive approach to reconstructive surgery for large defects of the abdominal wall with the recognized benefits of laparoscopy. The use of laparoscopic transabdominal repair of perineal hernias is not well described [2]. We present a case report demonstrating the benefits of laparoscopic perineal hernia repair after a previous open Abdominoperineal Resection (APR) using a non-resorbable mesh to repair the defect. We have demonstrated that the use of laparoscopy repairing the pelvic floor defect using a non-resorbable synthetic mesh offers excellent results with many potential advantages over open and transperineal transabdominal repairs.
Materials and Methods
A 66-year-old woman who as background had a breast cancer surgery in 2006 without recurrence and in 2015 an abdominoperineal laparoscopic amputation due to rectal adenocarcinoma (T4N1M0), receiving neoadjuvant and adjuvant radiotherapy and chemiotherapy cycles. She described mass sensation in the perineal area, some constipation and discomfort when sitting. In CT controls, two and one year prior to surgery for perineal hernia, occupation of the presacral space of fibrosis and relaxation of the pelvic floor with cystocele, peritoneocele and enterocele were described. Without other relevant background she was scheduled for laparoscopic transabdominal perineal eventroplasty.
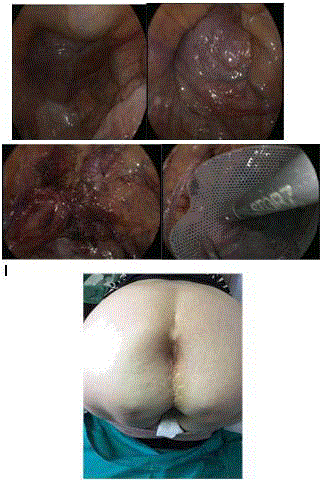
Figure 1
Results
Laparoscopic intervention was developed. During the procedure, an adhesional small bowel compound and an intense fibrosis of the lower pelvis with venous dilatation of peritoneal vessels were founded. The peritoneum of the Douglas pouch was unwoven and towards the pelvic peritoneum of the laterals with incidental opening of the bladder which was repaired with continuous synthetic suture that was covered with all the peritoneum detached before (Douglas and lateral pelvic peritoneum) which at the same time covers the entire defect placing an Omyra (visceral contact mesh) mesh over the minor pelvis. Patient was discharged without problems and after two months from surgery there wasn’t any sign of recurrence and an improvement of life quality since it was developed was experienced.
Discussion
Secondary perineal hernias are infrequent complications of major pelvic surgery with a higher prevalence in cancer surgeries that present as asymptomatic symptoms associated with risk factors such as smoking, women, chemotherapy, among others [2,4,7,8]. The approximate time interval between the Surgery and the appearance of the perineal incision is 6 months to 5 years. In this case, the patient presented as risks female sex, a rectal tumor also treated with chemotherapy and radiotherapy [2,4,6-8]. Usually the surgery is left for those symptomatic patients (pain, obstructive symptoms, cutaneous erosion before the rose of the hernia when sitting, etc) and this entails the reduction of the hernia by mobilizing the handles of the sac, closing the defect with or without a prosthetic mesh. These techniques range goes from the repair with synthetic mesh (which are mostly used in wide defects providing a new pelvic floor), flaps of skin muscle rotation and fascia lata, omentoplasties [2,4,6]. The type of mesh is also important because in the cases of hydrophilic meshes, these reduce the risk of adhesions with the viscera and the synthetic non-resorbable polyester provides a prolonged sustenance of the pelvic floor. Being a post-surgical complication that is not very prevalent, there is no consensus regarding the most appropriate therapeutic approach [4]. We believe that in those patients who have received treatment with radiotherapy and that significant fibrosis of the pelvic structures is associated, it is better to place the mesh with visceral contact without performing peritoneal detachment since the destructuration of this pelvic space implies an increased risk of injury to adjacent organs (bladder, seminal vesicles, prostate, vagina, etc.) leaving the peritoneal flap as an alternative to those with a more favorable anatomy. We have had good results with the use of this mesh but a longer follow-up is necessary.
Conclusion
Abdominal-perineal amputation is a widely spread surgery in all healthcare insurance systems worldwide and an unusual but important complication is the incisional hernia. Since in some cases surgical approach is the only effective treatment to the symptoms (abdominal pain, intestinal obstruction, skin erosions, etc.) we demonstrated with this case that laparoscopic repair is a safe surgical procedure with good results in which depending on the characteristics of the pelvis we can choose to perform or not a peritoneal flap, prioritizing the safety of the patient.
References
- Steele SR, Hull TL, Read TE, Saclarides TJ, Senagore AJ, Whitlow CB, Editors. The ASCRS Textbook of Colon and Rectal Surgery. Third Edition. 2016.
- Rayhanabad J, Sassani P, Abbas MA. Laparoscopic repair of perineal hernia. JSLS. 2009;13(2):237-41.
- Ewan LC, Charleston PJ, Pettit SH. Two case reports of perineal hernia after laparoscopic abdominoperineal resection with a proposed modification to the operative technique. Ann R Coll Surg Engl. 2014;96(2):e9-10.
- Allen SK, Schwab K, Day A, Singh-Ranger D, Rockall TA. Laparoscopic repair of postoperative perineal hernia using a two-mesh technique. Colorectal Dis. 2015;17(3):O70-3.
- Ryan S, Kavanagh DO, Neary PC. Laparoscopic repair of postoperative perineal hernia. Case Rep Med. 2010;2010.
- Aboian E, Winter DC, Metcalf DR, Wolff BG. Perineal hernia after proctectomy: prevalence, risks, and management. Diseases of the Colon and Rectum. 2006;49(10):1564-8.
- Mjoli M, Sloothaak DA, Buskens CJ, Bemelman WA, Tanis PJ. Perineal hernia repair after abdominoperineal resection: a pooled analysis. Colorectal Dis. 2012;14(7): e400-6.
- Akatsu T, Murai S, Kamiya S, Kojima K, Mizuhashi Y, Hasegawa H, et al. Perineal hernia as a rare complication after laparoscopic abdominoperineal resection: report of a case. Surg Today. 2009;39(4):340-3.