Clinical Image
An Intracardiac Mass Derived from Coronary Sinus
Irem Karauzum and Tayfun Sahin*
Department of Cardiology, Medical Faculty of Kocaeli University, Turkey
*Corresponding author: Irem Karauzum, Department of Cardiology, Medical Faculty of Kocaeli University, Umuttepe Yerleskesi, Eski Istanbul Yolu 10. Km, 41380 Kocaeli, Turkey
Published: 22 Jan, 2018
Cite this article as: Karauzum I, Sahin T. An Intracardiac
Mass Derived from Coronary Sinus.
Clin Surg. 2018; 3: 1878.
Keywords
Coronary sinus; Intracardiac mass; Pericardial tamponade; Echocardiography; Cardiac tomography
Clinical Image
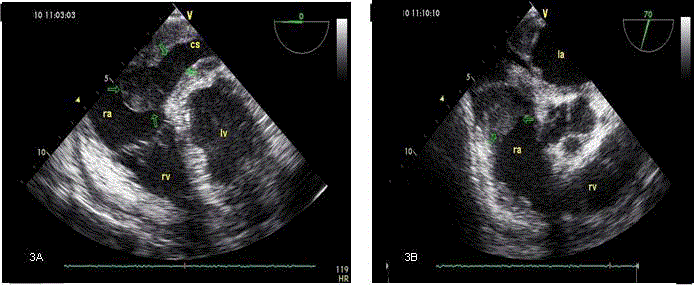
An eighty-year old male patient admitted to our cardiology department with complaints of cough and progressive dispnea continuing for three months. A review of his medical history was showed subtotal gastrectomy and cholecystectomy. He had smoked for 60 years and he has quited smoking 10 years-ago. On the physical examination, his vital signs showed a pulse of 131 bpm, blood pressure of 100/70 mmHg. He had regular but distant heart sounds, with no murmurs or rubs. Respiratory system examination revealed a prolonged expirium and there were no rales or rhonchi. The rest of the physical examination was unremarkable. On electrocardiogram, there was sinus tachicardia with rate of 138 bpm and low voltage QRS in all derivations. Chest X-ray showed increased cardio-thoracic index and blunted cardiophrenic angle. An emergent Tran thoracic Echocardiogram (TTE) revealed a large pericardial effusion with tamponade physiology compressing the right heart chambers at diastole and presenting significant respiratory variations in right and left ventricular transvalvular flow velocities. Pericardiocentesis was done, and 1500 mL hemorrhagic fluid was aspirated. His basic laboratory findings were unremarkable. His hormone levels, serologic tests, rheumatologic markers, tumor markers and fluid PCR were examined for pericardial effusion etiology and the results were also unremarkable. Fluid cytology revealed no malignant cells. Because of the patient has been a heavy smoker, thoracic (Figure 1A) and abdominal Computed Tomography (CT) scan was performed to detect any neoplasm. The CT findings were normal. The control echocardiogram was normal except minimal pericardial effusion near the left ventricular posterior wall and the diastolic dysfunction. Any pathologic finding which can cause pericardial effusion could not been found, so the patient was discharged and follow-up with transtorasic echocardiography was planned. The first and third month echocardiograms did not determine any pericardial effusions. Because of the sixth month TTE revealed a suspicious mass in the right atrium, the patient was hospitalized in the cardiology department and the investigation has been continued. A transesophageal echocardiogram was performed and an incomplete membrane in the right atrium, an excessive thickening of interatrial septum and a round-shaped mass which derived from the coronary sinus and filled the coronary sinus completely, and extended from the coronary sinus to the right atrium and the interatrial septum was detected. Right ventricular wall thickness and echogenicity were increased (Figures 2A, 3A and 3B). Cardiac Magnetic Resonance Imaging (CMRI) revealed a mass derived from coronary sinus and protruded to the right and left atrium (Figure 1B), localized mass lesions in the left and right ventricular apex and bilateral pleural effusion particularly significant on the left side. Thoracic CT demonstrated bilateral pleural effusion, compressive atelectasis in the adjacent parenchyma, a soft-tissue mass derived from coronary sinus and protruded to the right atrium and interatrial septum (Figure 2B), slight thickening of the pericardium, thickening with locally lipomatous component in the left ventricular and atrial wall and obstructed left lower lobe pulmonary vein. Any non-cardiac tumour was not found in the patient after the examinations. Intracardiac malign neoplasm arising from coronary sinus was considered primarily and a biopsy was recommended. However, the patient refused any invasive intervention and was discharged from the hospital voluntarily. It was learned that the patient had died one month after being discharged.
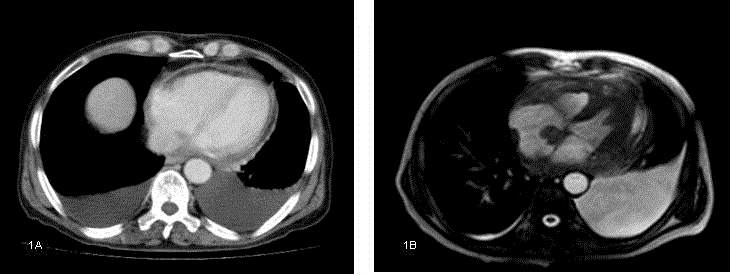
Figure 1
Figure 1A
Thoracic computed tomography which was performed after pericardiocentesis was normal.
Figure 1B: A mass in the right atrium was seen on the sixth month cardiac magnetic resonance imaging as a
filling defect.
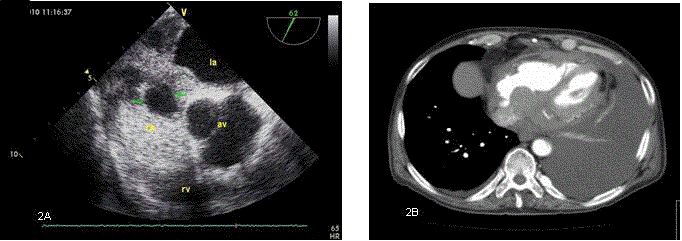
Figure 2
Figure 2A
In the Transesophageal Echocardiogram (TEE), at 620, aortic valve level, the mass was seen as a
filling defect in the right atrium when the contrast agent was administered.
Figure 2B: A mass derived from coronary sinüs and protruded to the right atrium was seen on the sixth month
thoracic computed tomography as a filling defect.