Research Article
Multivisceral Pancreatic Resections: Worth the Risk?
Arida Siripong1,2*, Mathew Chung1,2,3 and Shayna E Rich4
1Department of General Surgery, Michigan State University General Surgery Residency Program, USA
2Department of Surgery, Grand Rapids Medical Educational Partners, USA
3Department of Surgery, Spectrum Health Medical Group, USA
4Department of Surgery, University of Florida Radiation Oncology Residency Program, USA
*Corresponding author: Arida Siripong, Department of General Surgery, 200 Michigan St. NE Suite 200A, Grand Rapids, MI 49503, USA
Published: 18 Jan, 2018
Cite this article as: Siripong A, Chung M, Rich SE.
Multivisceral Pancreatic Resections:
Worth the Risk?. Clin Surg. 2018; 3:
1869.
Abstract
Introduction: As mortality associated with pancreatic surgery decreases, there has been an
increasing drive towards extended resections for locally advanced pancreatic cancer. However, the
overall impact of multivisceral resections on morbidity and mortality remains unclear.
Methods: An IRB-approved retrospective chart review was conducted amongst patients who
underwent pancreatic resection by a surgical oncologist at a single institution between July 2005
and July 2010. Patients were grouped into four categories based on extent of resection: Standard
Whipple (SW), Multivisceral Whipple (MVW), Distal Pancreatectomy (DP) and Multivisceral
Distal Pancreatectomy (MVDP). Measured variables included demographics, Length of Stay
(LOS), operating room time, margin status, postoperative morbidity, 30-day mortality, and median
survival.
Results: 192 patients were identified, with 145 who underwent standard and 47 multivisceral (MV)
resections. Demographics were similar between the two groups. Multivisceral procedures were
associated with a higher incidence of positive margins (40.5% vs. 22.9%, p=0.01), longer operating
times (4.9 vs. 3.8 hours, p< 0.001), and increased surgical complications (55.3% vs. 34.7%, p=0.012).
30-day mortality was comparable between all groups, but survival was significantly shorter in
patients who underwent multivisceral compared to standard resections (22 months vs. 11 months,
p=0.002).
Conclusion: Although multivisceral pancreatic resections may be performed with acceptable
morbidity and mortality in the appropriate patient population, there does not appear to be a survival
benefit.
Introduction
Pancreatic cancer is a lethal condition, with most patients presenting with unresectable disease
and overall survival at 5% [1]. Although chemotherapy and radiation play a critical role in the
treatment of this disease, only surgery offers the potential for long-term survival. Despite this, 5-year
survival remains at 15% to 20% after surgical resection [1-5]. Traditional approaches for resectable
tumors include a Standard Whipple procedure (SW) and distal pancreatectomy with or without
splenectomy (DP), with mortality rates as low as 5% at high volume centers [6-7].
Given these improvements in surgical outcomes, many have advocated for a more aggressive
operative approach to locally advanced pancreatic disease [7,8]. In 1977, Fortner and colleagues first
introduced a multivisceral pancreatectomy procedure. Despite the high morbidity and mortality at
83% and 9% reported from this study [9], multiple authors have since published updated results after
such procedures. The definitions of “multivisceral” or “extended” pancreatectomy procedures have
varied, including standard pancreatic resections with [1] Extended Lymphadenectomy (ELND),
[2] total pancreatectomy, [3] additional organ(s), and/or [4] arterial or venous resections [10-13].
While it has been established that extended lymphadenectomy in this setting results in higher
morbidity with no survival benefit, concomitant venous resection at the time of pancreatectomy has
demonstrated comparable morbidity and mortality to their standard counterparts [14-22]. When
defined based on additional organ resection, however, the benefit of Multivisceral Resections (MVR)
have been controversial [14,20,22]. Proponents of the more aggressive multivisceral approach have
suggested that local involvement of pancreatic disease may represent tumor location more than
tumor biology [19]. Enbloc resections therefore increase the likelihood of negative margins and
may improve survival rates. Arguments against this approach, however, highlight the increased morbidity and mortality accompanying these complex procedures,
particularly in a population with a median survival of less than
two years. At our institution, MVR was performed for local organ
or vessel involvement diagnosed at the time of surgery for locally
advanced pancreatic disease. Given the lack of consensus regarding
this topic, we conducted the current study to compare the outcomes
of multivisceral vs. standard pancreatic resections at a universityaffiliated
community hospital.
Table 1
Table 1
Patient, Tumor, and Resection Characteristics for Patients who Underwent Pancreatic Resections, by Type and Extent of Surgery.
Patients and Methods
IRB-approved retrospective chart review was used to identify all
patients who underwent pancreatic resection at a university-affiliated community hospital between July 2005 and July 2010. All procedures
were performed by a single fellowship-trained surgical oncologist.
Patients were categorized based on type of resection and anatomic
extent of resection: Standard Whipple (SW), Multivisceral Whipple
(MVW), and standard distal pancreatectomy with or without
Splenectomy (DP), or Multivisceral DP (MVDP). MVR was defined
as any standard pancreatectomy plus removal of an additional organ
or vascular structure. Additional organs included stomach (when
greater than fifty percent was removed), liver, kidney, small bowel,
and colon. Resected vascular structures included portal vein, superior
mesenteric vein, and left renal vein. Whipple procedures with total
pancreatectomy or splenectomy were categorized as MVW.
Data collection
Collected variables included demographics, Body Mass Index
(BMI), ASA classification, pathology, margin status, time in the
operating room, length of hospital stay, postoperative 30-day
morbidity and mortality, and survival. Morbidity was classified into
surgical and nonsurgical groups. Surgical morbidity included Delayed
Gastric Emptying (DGE), DGE requiring Percutaneous Endoscopy
Gastrostomy (PEG), intra abdominal abscess, pancreatic fistula, fluid
collection without bacterial growth, wound infection, and reoperation.
Nonsurgical morbidity included need for thoracentesis, pulmonary
embolus or deep vein thrombosis, superior mesenteric vein or portal
vein thrombosis, and cardiopulmonary failure. Pancreatic fistulas
were defined based on the International Study Group of Pancreatic
Surgery (ISGPS) definition [23] as peripancreatic fluid with amylase
levels greater than three times the serum level after postoperative
day three, or radiographic demonstration of a connection between
the drain fluid and pancreaticojejunostomy anastomosis. Survival
was measured based on the patient’s last date of follow-up or date
of death in multidisciplinary records. Survival was considered the
primary study endpoint, and all patients were censored at the time
of last contact.
Preoperative and operative details
Standard preoperative evaluation included history and physical
examination, standard laboratory testing, and imaging including CT
or MRI of the abdomen and pelvis. For malignancy, imaging was
used to rule out metastatic disease and determine local invasion to
surrounding structures. Patients with clear radiographic evidence
of direct invasion to the portal vein, superior mesenteric vein, or
superior mesenteric artery were excluded. For borderline radiographic
involvement, gross inspection at laparotomy was used to determine
resectability. No patients in the study received neoadjuvant therapy.
For each case, the abdomen was entered using an upper midline
incision or bilateral subcostal incisions. The abdomen was explored
for metastatic foci including palpation of the cavity, and intra
operative ultrasound was used to evaluate for liver metastases.
Patients with evidence of metastatic disease or involvement of
the celiac, superior mesenteric, or common hepatic arteries were
excluded. A pylorus-preserving technique was utilized for Whipple
procedures when deemed appropriate. SW consisted of removal of
the head of the pancreas, duodenum, gallbladder, and distal stomach.
MVR included enbloc removal of surrounding organs and vascular
structures including portal, superior mesenteric and renal veins in cases of local involvement. If venous resection was necessary due to
tumor infiltration, a separate vascular team completed this portion of
the procedure, with venous grafts in all cases. Total pancreatectomy
was performed for pancreatic head tumors with a positive pancreatic
margin on frozen section or intra operative findings concerning for
disease extending into the body or tail of the pancreas. In all cases,
en bloc resections were completed due to clinical suspicion or gross
evidence of macroscopic disease involvement of adjacent structures.
Statistical analysis
SAS 9.2 was used for statistical analysis. To describe the study
population, patient and tumor characteristics were compared
between standard and MVR groups, using Chi-square tests for
categorical variables and Mann-Whitney U-tests for continuous
variables. Analysis was performed in the full sample and within
strata for type of resection (SW vs. MVW and DP vs. MVDP), with
significance set at p-value < 0.05. Similarly, the perioperative course
and postoperative morbidity and mortality were compared using
a matched pair’s analysis. To examine long-term survival, Kaplan-
Meier survival curves were estimated for subgroups defined by
extent and type of surgery. The proportional hazards assumption did
not hold for strata defined by type and extent of resection, so Cox
proportional hazards models were not run. To evaluate endpoints
of 30-day hospital readmission and surgical complications, logistic
regression models were run to evaluate the Odds Ratios (OR) and
95% Confidence Intervals (CI). For each outcome, an unadjusted
analysis was run with main effects for type and extent of surgery and
their interaction, and an adjusted analysis that added all covariates
except histology. A secondary analysis was performed to determine
if pathology impacted outcomes. It was hypothesized that patients
with malignant pathology and a positive margin would demonstrate
shorter median survival compared to their benign counterparts.
Pathology was stratified as benign or malignant. Malignant pathology
included pancreatic adenocarcinoma, liposarcoma, gastrointestinal
stromal tumors, gastric adenocarcinoma, colon cancer, gallbladder
adenocarcinoma, and renal cell carcinoma. Benign conditions
included chronic pancreatitis, pseudo cysts, intraductal papillary
mucinous neoplasms, mucinous and serous cyst adenoma, and
benign neuroendocrine tumors. Kaplan-Meier survival curves were
estimated with methods similar to the main analysis.
Figure 1
Figure 1
Months of Survival for Patients Who Underwent Pancreatic Resections, by Extent and Type of Surgery.
Figure 2
Figure 2
Months of Survival for Patients Who Underwent Pancreatic Resections for Malignant Pathology.
Table 2
Table 3
Table 3
Complications and Outcomes of Whipple and Distal Pancreatectomy (DP) Resections, by Extent of Surgery.
Results
Patient characteristics
Overall, 192 patients underwent pancreatic resections at our
institution during the study period, with 145 (74.9%) undergoing
standard resection and 47 (25.1%) MVR. There were no statistical
differences in baseline demographics between these groups,
overall and in strata based on type of surgery (Whipple or distal
pancreatectomy; Table 1). Indications for pancreatic resection
included periampullary or pancreatic adenocarcinoma (n=103,
54%), chronic pancreatitis or pseudo cyst (n=16, 8%), intraductal
papillary neoplasm or cystic neoplasm (n=26, 14%), duodenal
adenoma or benign tumor (n=11, 6%), benign neuroendocrine
tumor (n=25, 13%), distant metastatic disease (n=6, 3.1%), and extra pancreatic malignancy with local pancreatic invasion (n=5,
3%). Amongst the 47 MVR patients, 12(26%) underwent venous
resection alone, including portal vein, superior mesenteric vein, or
left renal vein resection. Five patients had both venous resection and
organ removal. Seventeen patients (60%) had one additional organ
removed, seven (32%) had two removed, and four (6%) had three
removed. The most commonly resected organs were colon (n=13,
28%) and stomach when greater than 50% was removed (n=13, 28%).
In one case, a patient had a neuroendocrine tumor and idiopathic
thrombocytopenia, so splenectomy was performed in conjunction
with a Whipple procedure. Perioperative and postoperative variables
were compared between standard and MVR, overall and by anatomic
type of surgery (Table 2 and 3). The most frequent complications
included DGE (n=66, 34%), intra abdominal abscesses (n=47, 24%),
and pancreatic fistulas (n=21, 11%). Although MVW were associated
with longer operating times compared to SW, there was no significant
difference in rates of overall surgical morbidity. Those in the MVW
group, however, were more likely to have non surgical complications,
with thoracentesis required in 19% vs. 5% of MVW and SW patients,
respectively. MVDP had a higher incidence of nearly all complications
compared to DP, including surgical and nonsurgical complications.
Reoperation included intra abdominal exploration, with six patients
in this category. Three patients developed significant abdominal pain
between postoperative days three and six with imaging suggesting
pneumatosis. At re-exploration, findings included [1] diffuse
colonic ischemia, with cecostomy performed; [2] SMA thrombosis,
with necrosis of the majority of the small bowel and right colon,
with palliative measures; and [3] diffuse purulent fluid without
signs of perforation or leak, with washout performed. One patient
experienced hemodynamic instability and abdominal compartment
syndrome due to hemorrhage within the first 24 hr after MVW with
portal vein resection. At relaparotomy, diffuse oozing was noted,
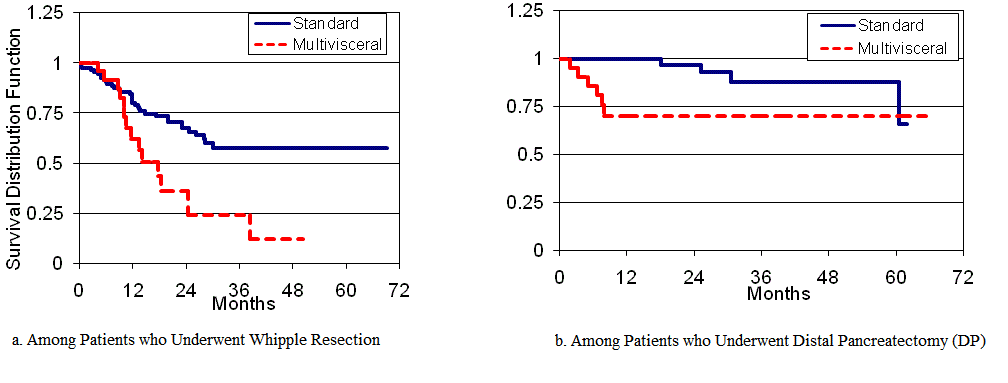
Figure 1: Months of Survival for Patients Who Underwent Pancreatic Resections, by Extent and Type of Surgery.
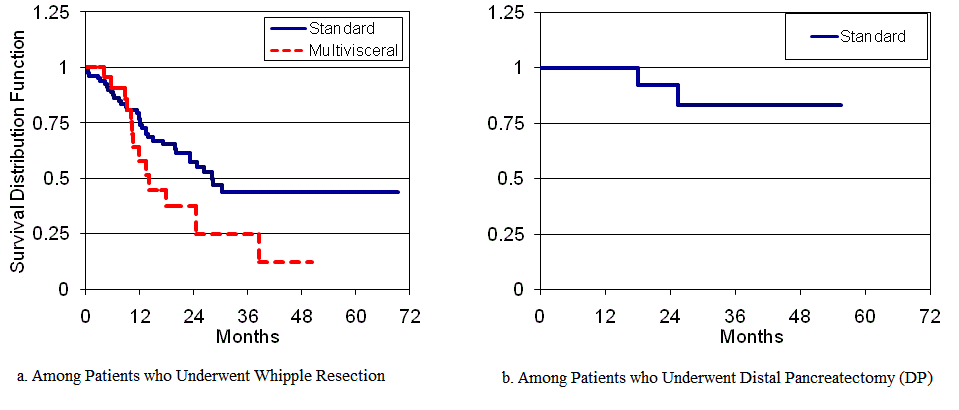
Figure 2: Months of Survival for Patients Who Underwent Pancreatic Resections for Malignant Pathology.
but no distinct source of bleeding was isolated. Another patient who
underwent MVW including superior mesenteric vein resection had
significant anemia and hemodynamic instability on postoperative day
four. Intra operatively, necrosis of the small bowel segment involved
in each of the anastomoses was identified, requiring reconstruction
of the gastrojejunostomy and hepaticojejunostomy with ligation of
the pancreatic duct. Reoperation was necessary in only one individual
in the distal pancreatectomy group- a patient who underwent
MVDP including transverse colectomy for chronic pancreatitis,
pseudo cysts, and a splenic artery aneurysm and presented to the
hospital on postoperative day 20 with significant hematemesis. After
unsuccessful endoscopic interventions, the patient was re-explored
and gastric bleeding was isolated to two small vessels requiring suture
ligation. One patient required reoperation for epidural hematoma
evacuation after epidural placement and neurologic compromise
with imaging confirming a large epidural hematoma. This patient did
not experience any permanent neurologic dysfunction.
In-hospital mortality
In-hospital and 30-day mortality rates were similar between
standard and MVR groups, with only three in-hospital deaths during
the study. One decedent was a 73-year-old male with cirrhosis and
cholestatic liver disease who underwent SW for an obstructing
periampullary tumor with a postoperative course complicated
by liver failure, hepatorenal syndrome, and eventual death. The
second decedent was a 68-year-old female who underwent SW for
cholangiocarcinoma. Postoperatively, she developed a trial fibrillation
with rapid ventricular response and ultimately cardiopulmonary
failure. Although there were plans for reoperation to investigate for
intra abdominal sepsis, the patient experienced a cardiopulmonary
arrest prior to re-exploration. A third patient in the DP group died
intra operatively after sustaining a cardiac arrest.
Survival
Overall, patients in the standard resection groups had a longer
median survival compared to those in the MVR groups (22 vs.
11 months, p=0.002). Even when stratified by type of operation,
multivisceral operations consistently demonstrated inferior survival
(Figure 1). A secondary analysis of survival for patients with malignant
pathology showed similar results (17 vs. 11 for SW vs. MVW; 26vs. 11
for DP vs. MVDP; Figure 2). Few patients had surgical resection for
benign disease.
Discussion
As pancreatic resections have become safer, boundaries regarding the definition of resectability have been challenged [14,15,17,19,20]. In particular, the role and safety of a multivisceral pancreatectomy defined by additional organ removal remains controversial. [14-17,20-29]. Certainly, these technically challenging invasive procedures should be performed at high-volume tertiary care centers where intensive perioperative care is available, but it is unclear if they are accompanied by acceptable morbidity and mortality. Arguments against MVR highlight the increased morbidity and mortality associated with these operations [22], with one study reporting a 3.2 times higher likelihood of postoperative complications after multivisceral compared to standard Whipple procedures [22]. In the largest published series of multivisceral pancreatic resections, Hartwig, et al. [14] compared 101 MVR to 202 standard resections, reporting higher morbidity and mortality when additional organ resection was performed [14]. 55% and 42.8% of patients in the MVR and standard resections groups, respectively, experienced morbidity with 37.6% and 25.3% attributed to surgical complications [14]. Specifically, the authors found an increased incidence of re-exploration in the MVR group, at 22% compared to 9%. Most recently, Burdelski, et al. [22] found that 55 patients with multivisceral pancreatic resections had increased morbidity and mortality compared to 303 patients with standard resections, but significantly lower than the 154 patients who underwent palliative bypass. In contrast, other studies have shown acceptable results for both morbidity and mortality when comparing the two groups. In the present study, surgical complications were more common in the multivisceral group, occurring in 47% vs. 66% of standard and MVR groups, respectively. In subgroup analysis, MVDP demonstrated increased morbidity compared to DP for nearly all types of complications, while MVW and SW had similar surgical morbidity. Therefore, multivisceral resections in the setting of a distal pancreatectomy, but not Whipple, were specifically associated with increased surgical morbidity in the current study. This study was limited in part due to the small sample size, particularly for patients with long-term follow-up. However, these numbers are comparable to similar studies in the literature, and long-term follow-up is primarily limited by the poor survival in this patient population. Another limitation is based on the inclusion of patients with a variety of histology types, including conditions with widely varying prognoses. To evaluate the impact of malignant disease processes on survival, a secondary analysis was performed with patients stratified by type of pathology, with results consistent with the main analysis. Finally, as a retrospective chart review, this study is limited in its ability to establish causality, although a randomized controlled trial would not be ethical in this setting. Our study demonstrated acceptable morbidity and short-term mortality after multivisceral pancreatic resections, particularly in the setting of a Whipple procedure. Unlike previous studies, however, our results highlighted unfavorable longterm survival in these cases and suggest that the long-term benefit and specific indications for multivisceral operations should be carefully evaluated prior to resection. In response to these study findings, at our institution neoadjuvant therapy is now utilized more routinely in the multimodal treatment of pancreatic cancer.
References
- Wagner M, Redaelli C, Lietz M, Seiler C, Friess H, Buchler MW. Curative resection is the single most important factor determining outcome in patients with pancreatic adenocarcinoma. Br J Surg. 2004;91:586-94.
- Butturini G, Stocken DD, Wente MN, Jeekel H, Klinkenbijl JH, Bakkevold KE, et al. Influence of resection margins and treatment on survival in patients with pancreatic cancer: meta-analysis of randomized controlled trials. Arch Surg. 2008;143(1):75-83.
- Neoptolemos JP, Stocken DD, Friess H, Bassi C, Dunn JA, Hickey H, et al. A randomized trial of chemoradiotherapy and chemotherapy after resection of pancreatic cancer. N Engl J Med. 2004;350(12):1200-10.
- Cameron JL, Riall TS, Coleman J, Belcher KA. One thousand consecutive pancreaticoduodenectomies. Ann Surg. 2006;244(1):10-15.
- Birkmeyer JD, Stukel TA, Siewers AE, Goodney PP, Wennberg DE, Lucas FL. Surgeon volume and operative mortality in the United States. N Engl J Med. 2003;349:2117-27.
- Fernandez-Del CC, Rattner DW, Warshaw AL. Standards for pancreatic resection in the 1990s. Arch Surg. 1995;130:295-99.
- DeCastro SM, Busch OR, van Gulik TM, Obertop H, Gouma DJ. Incidence and management of pancreatic leakage after pancreatoduodenectomy. Br J Surg. 2005;92(9):1117-23.
- Buchler MW, Wagner M, schmied BM, Uhl W, Friess H, Z’graggen K. Changes in morbidity after pancreatic resection: toward the end of completion pancreatectomy. Arch Surg. 2003;138(12):1310-4.
- Fortner JG, Kim DK, Cubilla A, Turnbull A, Pahnke LD, Shils ME. Regional pancreatectomy: en bloc pancreatic, portal vein and lymph node resection. Ann Surg. 1977;186(1):42-50.
- Tseng JF, Raut CP, Lee JE, Pisters PW, Vauthey JN, Abdalla EK, et al. Pancreaticoduodenectomy with vascular resection: margin status and survival duration. J Gastrointest Surg. 2004;8:935-49.
- Leach SD, Lee JE, Charnsangavej C, Cleary KR, Lowy AM, Fenoglio CJ, et al. Survival following pancreaticoduodenectomy with resection of the superior mesenteric-portal vein confluence for adenocarcinoma of the pancreatic head. Br J Surg. 1998;85:611-617.
- Al-Haddad M, Martin JK, Nguyen J, Pungpapong S, Raimondo M, Woodward T, et al. Vascular resection and reconstruction for pancreatic malignancy: a single center survival study. J Gastrointest Surg. 2007;11(9):1168-74.
- Siriwardana HP, Siriwardena AK. Systematic review of outcome of synchronous portal-superior mesenteric vein resection during pancreatectomy for cancer. Br J Surg. 2006;93:662-673.
- Hartwig W, Hackert T, Hinz U, Hassenpflug M, Strobel O, Büchler MW, et al. Multivisceral resection for pancreatic malignancies: risk-analysis and long-term outcome. Ann Surg. 2009;250(1):81-7.
- Klempnauer J, Ridder GJ, Bektas H, Pichlmayr R. Extended resections of ductal pancreatic cancer--impact on operative risk and prognosis. Oncology. 1996;53(1):47-53.
- Nikfarjam M, Sehmbey M, Kimchi ET, Gusani NJ, Shereef S, Avella DM, et al. Additional organ resection combined with pancreaticoduodenectomy does not increase postoperative morbidity and mortality. J Gastrointest Surg. 2009;13(5):915-21.
- Suzuki Y, Fujino Y, Tanioka Y, Sakai T, Ajiki T, Ueda T, et al. Resection of the colon simultaneously with pancreaticoduodenectomy for tumors of the pancreas and periampullary region: short-term and long-term results. World J Surg. 2004;28:1007-10.
- Reddy SK, Tyler DS, Pappas TN, Clary BM. Extended resection for pancreatic adenocarcinoma. Oncologist. 2007;12(6):654-63.
- Fuhrman GM, Leach SD, Staley CA, Cusack JC, Charnsangavej C, Cleary KR, et al. Rationale for en bloc vein resection in the treatment of pancreatic adenocarcinoma adherent to the superior mesenteric-portal vein confluence. Ann Surg. 1996;233:154-62.
- Sasson AR, Hoffman JP, Ross EA, Kagan SA, Pingpank JF, Eisenberg BL. En bloc resection for locally advanced cancer of the pancreas: is it worthwhile? J Gastrointest Surg. 2002;6:147-57.
- Mckay A, Sutherland F. Morbidity and Mortality following Multivisceral Resections in Complex Hepatic and Pancreatic Surgery. J Gastrointest Surg. 2008;12:86-90.
- Burdelski C, Reeh M, Bogoevski D, Gebauer F, Tachezy M, Vashist YK, et al. “Multivisceral Resections in Pancreatic Cancer: Identification of Risk Factors.” World J Surg. 2011;35:2756-63.
- Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, et al. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005;138:8-13.
- Nakafusa Y, Tanaka T, Tanaka M, Kitajima Y, Sato S, Miyazaki K. “Comparison of Multivisceral Resection and Standard peration for Locally Advanced Colorectal Cancer: Analysis of Prognostic Factors for Short-Term and Long-Tem Outcome. Diseases of the Colon & Rectum. 2004;47(12):2055-63.
- Hernandez J, Mullinax J, Clark W, Toomey P, Villadolid D, Morton C, et al. “Survival After Pancreaticodudoenectomy is not Improved by Extending Resections to Achieve Negative Margins.” Ann Surg. 2009;250:76-80.
- Raut CP, Tseng JF, Sun CC, Wang H, Wolff RA, Crane CH, et al. Impact of resection status on pattern of failure and survival after pancreaticoduodenectomy for pancreatic adenocarcinoma. Ann Surg. 2007;246(1):52-60.
- Breslin TM, Hess KR, Harbison DB, Jean ME, Cleary KR, Dackiw AP, et al. Neoadjuvant chemoradiotherapy for adenocarcinoma of the pancreas: treatment variables and survival duration. Ann Surg Oncol. 2001;8(2):123-32.
- Luttges J, Vogel I, Nenke M, Henne-Bruns D, Kremer B, Kloppel G. The retroperitoneal resection margin and vessel involvement are important factors determining survival after pancreaticoduodenectomy for ductal adenocarcinoma of the head of the pancreas. Virchows Arch. 1998;433(3):237-42.
- Irani JL, Ashley SW, Brooks DC, Osteen RT, Raut CP, Russell S, et al. Distal pancreatectomy is not associated with increased perioperative morbidity when performed as part of a multivisceral resection. J Gastrointest Surg. 2008;12(12):2177-82.