Case Report
Randomized Prospective Single-Blinded Study of TEP Inguinal Hernia Repair: Tacking Mesh versus Self-Fixating Mesh
Yazan Al Jamal*, Eee LN Buckarma, Becca Gas and David Farley
Department of General Surgery, Mayo Clinic, Rochester, Minnesota, USA
*Corresponding author: Yazan Al Jamal, Department of General Surgery, Mayo Clinic, 200 First S SW, Rochester, MN 55905, USA
Published: 16 Jan 2018
Cite this article as: Al Jamal Y, Buckarma ELN, Gas B,
Farley D. Randomized Prospective
Single-Blinded Study of TEP Inguinal
Hernia Repair: Tacking Mesh versus
Self-Fixating Mesh. Clin Surg. 2018; 3:
1856.
Abstract
Background: Totally extraperitoneal inguinal hernia repair (TEP-IHR) offers advantages over
conventional open IHR. ProGrip™ self-fixating mesh delivers a tack-free fixation repair. Using
ProGrip™ during TEP-IHR may lead to decreased postoperative pain and/or complications
compared to fixating mesh with titanium clips.
Methods: A randomized, prospective, single-blinded study compared ProGrip™ mesh versus
regular Prolene mesh with titanium tack fixation. A total of 38 patients underwent 65 TEP-IHR at
our institution. All repairs were completed with either Prolene mesh (Group TT = 19 patients) with
tack fixation or ProGrip™ self-fixating mesh (Group PG = 19 patients). Blinded patients were asked
to rate their level of pain according to a Likert scale (0=no pain, 5=severe pain) preoperatively, and
at 1 and 4 weeks postoperatively.
Results: Thirty eight men underwent 65 TEP-IHR with a mean age of 55 years (SD±11), mean BMI
of 30 kg/m2 (SD±9) and mean ASA of 1.9 (SD±0.5). Most repairs were bilateral (TT=16, PG=11).
Operative times (TT=65 min±18; PG=77 min±31, p=0.1), hospital length of stay (15.7 vs 14.4
hours, p=0.63), and urinary retention (TT=1, PG=1, p=NS) were similar. No significant differences
occurred in the level of pain or limitation of movement pre-op and 4 weeks postop. The patients in
TT group reported more pain and limitation of movement than the patients in PG group at 1 week
postop (p=0.02).
Conclusions: ProGrip™ self-fixating mesh for TEP-IH repair appears safe and effective; it has similar
performance to Prolene mesh using titanium tack fixation.
Introduction
Hernia repairs represent one of the most common surgical operations performed worldwide [1]. While there are multiple methods to fix inguinal herniae, a tension-free repair is the procedure of choice [2]. Endoscopic inguinal herniorrhaphy has become an established approach to repair groin herniae. Totally extraperitoneal inguinal hernia repair (TEP-IHR) offers advantages over conventional open IHR: preperitoneal approach with potentially less discomfort, less morbidity, and the easy option for bilateral repairs [3]. Different types of mesh and fixation methods have been described to avoid inguinodynia with limited success [4,5]. Recently, a self-fixating mesh has been introduced and used successfully in open and MIS inguinal hernia repairs [6-8]. It is made of monofilament polyester with resorbable grips on one side to allow positioning and fixation of the mesh to the surrounding tissue and collagen film on the other side to facilitate mesh handling and deployment [9,10]. We questioned whether using self-fixating mesh during TEP-IHR would lead to decreased postoperative pain and complications compared to fixating mesh with titanium tacks.
Methods
With approval of our Institutional Review Board, a randomized, prospective, single-blinded study of 38 patients was used to compare self-fixating mesh versus regular Prolene mesh with titanium tacks performed by one surgeon and his surgical team at the Mayo Clinic, Rochester MN from December 2013 to November 2015. All males between the ages of 18 and 100 years of age undergoing TEP-IHR were eligible. Baseline demographics and perioperative data were extracted from the medical records, including: age, gender, body mass index (BMI in kg/m2), previous inguinal hernia operations, laterality and type of hernia, length of operation, total amount of hours spent in the hospital, amount of pain medication administered (converted to morphine equivalents), conversion rates, intra-operative complications, postoperative surgical complications (e.g., wound infection, hematoma), and general postoperative complications (e.g., pneumonia, urinary tract infection, pulmonary embolism). Follow-up data were obtained through review of the medical record (e.g., postoperative return visits), including long term issues and hernia recurrence. Blinded patients were asked to rate their level of pain on a Likert scale (0 through 5; 0 = no pain, 5 = severe pain) preoperatively, and at 1 and 4 weeks, postoperatively. In follow-up, we used a standardized telephone script consisting of 12 questions, and asked for symptoms such as pain and limitation of movement while lying down, bending over, sitting up, coughing, taking a deep breath, walking upstairs and performing activities of daily living. TEP-IHR was performed under general anesthesia, using a 3-port, midline technique (one infraumbilical 10-mm Hasson trocar, two 6-mm trocars). A balloon dissector and blunt dissection expose the preperitoneal space of Bogros. Placement of Prolene mesh (10 cm × 15 cm) fixed with titanium tacks or ProGripTM self-fixating mesh (10 cm × 15 cm) was utilized to widely cover hernia defects. Because of data distribution, comparisons between groups were performed with nonparametric tests as appropriate. All statistical tests were twosided, and a p value of 0.05 was considered statistically significant. Continuous data are presented as means with standard deviation (SD) or median (range), and categorical data are presented as counts and percentages. All statistical analyses were performed using JMP software (version 9.0.1; SAS, Cary, NC).
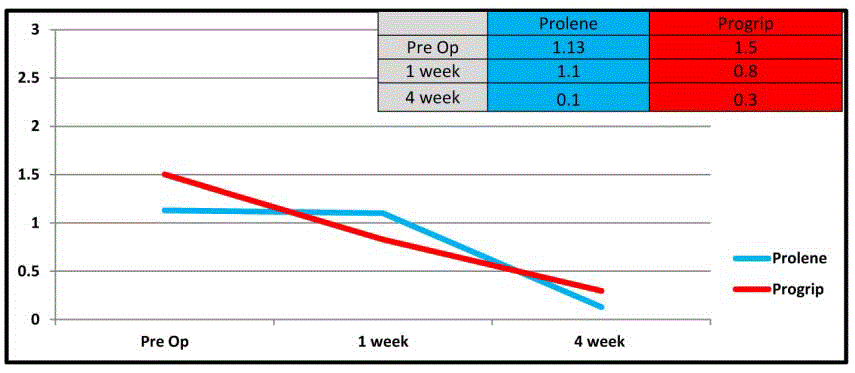
Figure 1
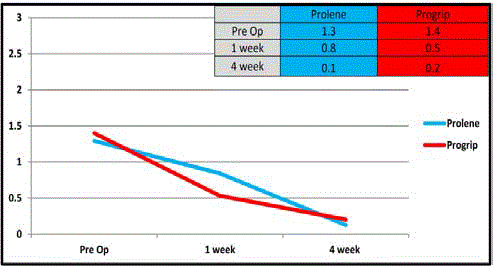
Figure 2
Results
Thirty eight male patients underwent 65 TEP-IHR. The selffixating
ProGripTM mesh (PG) group (n=19) and regular Prolene
mesh with titanium tacks (TT) group (n=19) were similar: mean
(SD) age was 55 years (±11) in PG and 58 years (±11) in TT (p=NS);
mean (SD) BMI was 30 Kg/m2 (±4) in PG and 30 Kg/m2 (±10) in TT,
(p=NS). Mean (SD) ASA was 1.7 (±0.5) in both groups. Most repairs
were bilateral (TT= 16, PG = 11, p=NS, Table 1).
No significant intra operative complications were encountered;
the median (range) starting time of operation was 8:59 am (8:08,
14:24) for TT and 8:57 am (8:04, 12:48) for PG. The mean (SD)
operative time for bilateral repairs was 69 (±6.5) minutes for TT and
84 (±7.8) minutes for PG (p= 0.17).The mean (SD) operative time for
unilateral repairs was 40 (±12) minutes for TT and 66 (±7) minutes
for PG (p=0.09). During their hospitalization, PG patients required
more pain medication (morphine equivalents) than TT patients (63
mg (±5.3) vs. 21 mg (±4.4), respectively; p = 0.01).Mean (SD) hospital
length of stay was 15.7 (±1.5) hours for TT and 14.4 (±1.5) hours for
PG. Three patients stayed overnight (TT=2 for bladder catheterization
due to urinary retention and pain management; PG=1 for bladder
catheterization due to urinary retention) (Table 2). One TT patient
required antibiotics for a minor superficial skin infection at the
umbilical port site, and one recurrence was identified in the PG group
over the median time of observation of 12 months. No recurrence was
seen in TT patients (p=NS).
All patients (100%) responded to our pre-operative, 1 week and 4 week postoperative surveys. Hernia repair improved the pain and
the movement limitation in patients in both groups. Overall, Twentyseven
patients (74%) reported some type of pain preoperatively
compared to 10 patients (25%) who reported some type of pain at 4
weeks postoperatively, p < 0.05.Moreover, 26 (68%) patients reported
some limitation of movement preoperatively compared to only 4 (10%)
patients at 4 weeks postoperatively; p< 0.05. There was no difference
in the level of pain preoperatively between the two groups (TT=1.3/5,
PG=1.6/5; p=0.2).TT patients reported a higher pain score than PG
patients at 1 week postoperatively (TT=1.1/5, PG=0.8/5; p=0.02).No
difference in the level of pain 4 weeks postoperatively was reported
between groups (TT=0.1/5, PG=0.3/5; p=0.1) (Table 3 and Figure 1).
There was no difference between groups preoperatively in movement
limitation (TT=1.3/5, PG=1.4/5; p=0.6). TT patients reported more
movement limitationat1 week postoperatively compared to PG
patients (TT=0.84/5, PG=0.53/5; p=0.01). There was no difference
in movement limitations between groups at 4 weeks postoperatively
(TT=0.12/5, PG=0.2/5; p=0.5) (Table 4 and Figure 2).
Table 1
Table 2
Discussion
This randomized prospective, single blinded study of 38 patients
undergoing TEP IH repairs suggests: 1) ProGrip™ self-fixating mesh
for TEP-IHR is safe and effective, 2) it has similar operative times
and outcomes to Prolene mesh using titanium tacks, 3) ProGrip™
patients ingested more narcotic medication postoperatively than
Prolene patients, and 4) the pain and limitation movement scores
at one week postoperatively were higher for the TT patients, but
there was no difference in pain and limitation movement scores at
4 weeks. ProGrip™ self-fixating mesh is a tack-free fixation mesh
for use in open & laparoscopic hernia repairs. It is composed of
absorbable Monofilament Polylactic Acid micro-grips on one
surface integrated with a lightweight Monofilament Polyethylene
Terephthalate. The micro grips act as a kind of “Velcro” to the soft
tissue surfaces resulting in self-fixation. Initial studies have shown
that this mesh is safe for use in both TEP and open inguinal hernia
repair [11]. While slightly more expensive than plain Prolene mesh,
ProGrip™ mesh does not require the expense of titanium tackers [12].
In our study, using tacks was faster than placing ProGrip™, but not
significantly so. The challenging aspect of using ProGrip™ is moving
the mesh within the confined preperitoneal space. It is not always
easy to move the fixating mesh over the cord structures, the hernia
sac and surrounding fat. However with repetition, handling the mesh
becomes easier and takes less time. Developing wide exposure and
maximizing the preperitoneal space facilitates easier placement.
One recurrence was encountered in our study: a ProGrip™ patient
presented 6 months later with a left sided recurrent inguinal hernia
after undergoing TEP IHR for large, incarcerated, bilateral indirect
herniae. The dissection and hernia reduction were difficult in this
patient, but the mesh panels were placed in satisfactory positions.
Re-exploration has not yet been performed, and we remain unclear
why recurrence occurred on the patient’s left side. In a meta-analysis,
Lau and Patil recommended fixation of mesh routinely, especially in
large hernias (>3 cm) [13,14]. However, fixating mesh using tacks
for smaller defects has been controversial due to the concerns of
an increasing incidence of pain and concerns of recurrence with no
fixation [15,16]. Our group published a prospective study in 2006 that
showed a significant reduction in the use of postoperative narcotic
analgesia, hospital length of stay, the development of postoperative
urinary retention, as well as no increase in recurrence rate by
eliminating tack fixation of mesh during laparoscopic TEP-IHR [4].
Another study compared the use of Fibrin sealant with tack fixation
in laparoscopic TEP inguinal hernia repair and found there was no
advantage in using one technique over the other4.Moreover, in the
most recent meta-analysis by Cristaudo and his group, there were no
differences in (Carolina Comfort Scale) scores when comparing types
of mesh, configuration of the mesh or fixation methods [17].
Others have found most patients undergoing laparoscopic IH
repairs [3,18] recover quickly and have less pain with activity than they
did preoperatively. We are encouraged that this small study similarly
confirms superb outcomes in short follow up for both ProGrip and
tacking options. Surgeons should feel confident that both options
offer effective repair for their patients. This prospective study has
several limitations. The small size of patients in both groups limits the
power to reflect statistical differences. This study had a large number
of bilateral repairs reflecting the inherent referral bias of our practice.
Furthermore, we recognize that survey scores were consistently very
low preoperatively, at 1 week and at 4 weeks postoperatively for both
groups; statistical differences may have been identified, but clinical
relevance may be negligible. In summary, this small prospective,
randomized study, confirms several known findings about patients
undergoing TEP-IHR: 1) most had less pain and greater freedom
of movement following the procedure (with use of either tacks or
ProGrip) and 2) ProGrip™ self-fixating mesh is a reasonable option
to Prolene mesh tacked with Titanium clips. It will take much larger
randomized trials with longer follow-up to confirm our findings.
References
- Awad SS, Fagan SP. Current approaches to inguinal hernia repair. Am J Surg. 2004;188(6):9S-16S.
- Eklund AS, Montgomery AK, Rasmussen IC, Sandbue RP, Bergkvist LA, Rudberg CR. Low recurrence rate after laparoscopic (TEP) and open (Lichtenstein) inguinal hernia repair: a randomized, multicenter trial with 5-year follow-up. Ann Surg. 2009;249(1):33-8.
- McCormack K, Scott NW, Go PM, Ross S, Grant AM, Collaboration EUHT. Laparoscopic techniques versus open techniques for inguinal hernia repair. Cochrane Database Syst Rev. 2003(1):CD001785.
- Koch CA, Greenlee SM, Larson DR, Harrington JR, Farley DR. Randomized prospective study of totally extraperitoneal inguinal hernia repair: fixation versus no fixation of mesh. JSLS. 2006;10(4):457-60.
- Tam KW, Liang HH, Chai CY. Outcomes of staple fixation of mesh versus nonfixation in laparoscopic total extraperitoneal inguinal repair: a meta-analysis of randomized controlled trials. World J Surg. 2010;34(12):3065-74.
- Chastan P. Tension-free open hernia repair using an innovative self-gripping semi-resorbable mesh. Hernia. 2009;13(2):137-42.
- Kapischke M, Schulze H, Caliebe A. Self-fixating mesh for the Lichtenstein procedure--a prestudy. Langenbecks Arch Surg. 2010;395(4):317-22.
- Messaris E, Nicastri G, Dudrick SJ. Total extraperitoneal laparoscopic inguinal hernia repair without mesh fixation: prospective study with 1-year follow-up results. Arch Surg. 2010;145(4):334-8.
- Kolbe T, Hollinsky C, Walter I, Joachim A, Rulicke T. Influence of a new self-gripping hernia mesh on male fertility in a rat model. Surg Endosc. 2010;24(2):455-61.
- Hollinsky C, Kolbe T, Walter I, Joachim A, Sandberg S, Koch T, et al. Comparison of a new self-gripping mesh with other fixation methods for laparoscopic hernia repair in a rat model. J Am Coll Surg. 2009;208(6):1107-14.
- HInformations derived from ProGrip Laparoscopic Self- Fixating Mesh Information sheet. 2009(© 2012 Covidien 11.12 M120886).
- Estimate derived from Mayo Clinic Hospital Supply service. Based on typical prices of anatomical mesh and absorbable fixation in the US.
- Teng YJ, Pan SM, Liu YL, Yang KH, Zhang YC, Tian JH, et al. A meta-analysis of randomized controlled trials of fixation versus nonfixation of mesh in laparoscopic total extraperitoneal inguinal hernia repair. Surg Endosc. 2011;25(9):2849-58.
- Sajid MS, Ladwa N, Kalra L, Hutson K, Sains P, Baig MK. A meta-analysis examining the use of tacker fixation versus no-fixation of mesh in laparoscopic inguinal hernia repair. Int J Surg. 2012;10(5):224-31.
- Lantis JC, 2nd, Schwaitzberg SD. Tack entrapment of the ilioinguinal nerve during laparoscopic hernia repair. J Laparoendosc Adv Surg Tech A. 1999;9(3):285-9.
- Taylor C, Layani L, Liew V, Ghusn M, Crampton N, White S. Laparoscopic inguinal hernia repair without mesh fixation, early results of a large randomised clinical trial. Surg Endosc. 2008;22(3):757-62.
- Cristaudo A, Nayak A, Martin S, Adib R, Martin I. A prospective randomised trial comparing mesh types and fixation in totally extraperitoneal inguinal hernia repairs. Int J Surg. 2015;17:79-82.
- Ali SM, Zendejas B, Yadav S, Hernandez-Irizarry RC, Lohse CM, Farley DR. Predictors of chronic groin discomfort after laparoscopic totally extraperitoneal inguinal hernia repair. J Am Coll Surg. 2013;217(1):72-8.