Case Report
Pathological Fractures of the Mandible: A Report of 27 Cases
Yi Zhao1,2, Rui-Fang Li1,3, Yan-Fang Sun1,3, Bing Liu1,3 and Jun Jia1,3*
1State Key Laboratory Breeding Base of Basic Science of Stomatology (Hubei-MOST) and Key Laboratory of Oral
Biomedicine Ministry of Education, School and Hospital of Stomatology, Wuhan University, China
2Department of Prosthodontics, School and Hospital of Stomatology, Wuhan University, China
3Department of Oral and Maxillofacial Surgery, School and Hospital of Stomatology, Wuhan University, China
*Corresponding author: Jun Jia, Department of Oral and Maxillofacial Surgery, School and Hospital of Stomatology, Wuhan University, Wuhan 430079, China
Published: 03 Aug, 2017
Cite this article as: Zhao Y, Li R-F, Sun Y-F, Liu B, Jia J.
Pathological Fractures of the Mandible:
A Report of 27 Cases. Clin Surg. 2017;
2: 1839.
Abstract
Purpose: To review 27 cases of pathological fractures of the mandible.
Methods: A retrospective study was undertaken to analyze the etiology, site, treatment methods,
and prognosis of pathological mandibular fractures (from 1993 to 2015) at Hospital of Stomatology,
Wuhan University.
Results: Pathological mandibular fractures were most associated with iatrogenic factor (11
cases), such as rim mandibulectomy, cyst enucleation or third molar extraction, followed by
osteoradionecrosis of mandibles (7 cases), bone destruction resulting from benign or malignant
tumors (5 cases) and osteomyelitis (4 cases). The predominant site was the mandibular body (23
fractures, 82.14%), followed by the angle/posterior molar region (4 fractures, 14.29%), and one
condyle (3.57%). Several methods were used to treat the fractured mandibles. Fourteen cases
(51.85%) of pathological fractures were treated by resection, in which seven cases were reconstructed
by autogenous bone or composite tissue flap, two with reconstruction plate, and five without
reconstruction; six cases of fractures (22.22%) underwent close reduction with intermaxillary
fixation or chin cap immobilization; four cases (14.82%) underwent open reduction and internal
fixation (wire or miniplate) with/without intermaxillary fixation; and the remaining three cases
(11.11% ) treated by sequestrectomy or condylectomy.
Conclusion: Pathological mandibular fractures have diverse etiologies. Many patients required
resection of primary lesions, while conservative management without rigid fixation can obtain bony
union in some patients.
Keywords: Pathological fracture; Mandible; Osteomyelitis; Osteoradionecrosis
Introduction
Pathological fracture of the mandible (PFM) is a fracture which occurs through a preexisting
lesion or in a diseased part of the bone, comprising < 1% of all fractures [1]. Most data are documented
in independent case reports. Common causal factors include surgical procedures, osteonecrosis of
the jaw, infection and tumors [2,3].
It has been shown that the frequence of the etiology of PFMs has changed during the past several
decades. Iatrogenic fracture of the mandible still remains the main cause of PFMs. The incidence
of osteomyelitis decreases in recent years possibly because of improved oral health, early treatment
of carious teeth and efficient antibiotic application. However, the osteoradionecrosis and late PFMs
significantly increase because of the wide use of adjuvant radiation therapy for patients suffering
from head and neck cancer [4].
Compared with traumatic fracture, PFMs frequently involve a much more complex clinical
situation such as preexistence of pathology of the bone, lack of buttressing, and generally a
compromised nutritional status. In addition, PFM frequently involves the patients who are
systemically immunocompromised individuals, with grossly infected bone with non-viable or
normal bone dramatically destroyed by the disease [5,6]. Therefore, PFMs are often difficult to treat.
In this report, 27 cases of pathological mandibular fractures treated in a teaching hospital of
stomatology in China were reviewed and analyzed. The aim of this study was to determine the etiology of pathological fractures, the site, and the treatment offered.
Table 1
Methods and Methods
The hospital records and the radiographs of 27 patients who suffered from pathological fracture of the mandible were retrospectively analyzed. All the patients were treated at the Department of Oral and Maxillofacial Surgery, Hospital of Stomatology, Wuhan University from January 1, 1993 to November 31, 2015. The etiology of these mandibular fractures was identified as osteoradionecrosis (ORN), benign/malignant tumors, infections, or iatrogenic factors. Data collected included age, gender, etiology, site, management methods and outcome. A panoramic radiograph was often used to identify pathological mandibular fractures and CT scan was only used to clarify some uncertain cases. This study was performed according to the principles of the Declaration of Helsinki and approved by the review board of the Ethics Committee of Hospital of Stomatology, Wuhan University.
Results
Twenty-seven patients with 28 pathologic fractures were collected
with an average length of follow up of 12 months. Nineteen patients
were male and 8 were female. The average age was 51 years with a
range of 4-71 years. There was only one child with follicular cyst (aged
4) and all other patients were 30 or older.
Etiologically, seven patients were diagnosed as osteoradionecrosis
(ORN), one of which developed fractures of both the left angle and
right body of the mandible, four as osteomyelitis. Two fractures
were caused by direct invasion of the mandible by squamous cell
carcinoma and ameloblastoma, respectively, and a condyle fracture
by metastatic malignant tumor from breast adenocarcinoma. Eight
cases of fracture were related with enucleation of odontogenic
keratocyst (OKC), resection of calcifying cystic odontogenic tumor
(CCOT) or arteriovenous malformation and rim mandibulectomy
of oral squamous cell carcinoma (OSCC) (Table 1). Two patients
had fractures following third molar extractions and one case was
associated with a follicular cyst of the mandible. A total of 11 (40.74%)
pathological fractures were caused by iatrogenic factors.
The symptom of a cracking noise was frequently noted by patients
with pathological fractures. Malocclusion, incapability of mouth
closing or limitation of motion of the mandible was sometimes
complained (Figure 1). Intraoral or submandibular sinus tract or fistula was found in 4 cases of osteomyelitis, 3 osteoradionecrosis,
an odontogenic keratocyst and an arteriovenous malformation. The
predominant site of pathological fractures was the mandibular body
(23 fractures, 82.14%), followed by the angle/posterior molar region
(4 fractures, 14.29%), and one condyle (3.57%).
Among 27 cases under management, fourteen cases (51.85%)
of pathological fractures were treated by resection, in which seven
cases were reconstructed by autogenous bone or composite tissue
flap (Figure 2 and 3), two with reconstruction plate and five without
reconstruction. Six cases of fractures (22.22%) underwent close
reduction with intermaxillary fixation or chin cap combined with
extraoral traction for mandible immobilization (Figure 4). Four
cases underwent open reduction and internal fixation (wire or
miniplate) (Figure 5). Two patients with osteomyelitis were treated
with local sequestrectomy with intermaxillary fixation (IMF) and
another underwent IMF combined with antibiotics. Lastly, the
condyle fracture by metastatic breast adenocarcinoma was treated by
condylectomy.
Overall, most cases were satisfactory with the treatments.
However, there were several cases with some sequelae. One case
of mandibular reconstruction failed, in which the fibular free flap
was used for the fracture of ORN caused by radiation therapy of nasopharyngeal carcinoma. In addition, significant malocclusion was
observed in four patients who received segmental mandibulectomy
without reconstruction, and minor degree of malocclusion
demonstrated in two other patients treated with a sequestrectomy.
No nonunion of the mandible or other complications were observed.
Figure 1
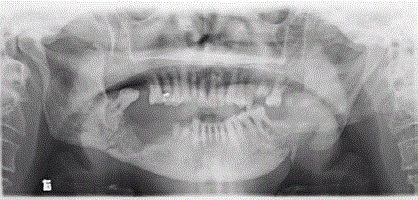
Figure 1
Left angle fracture and right mandibular body fracture in one patient of nasopharyngeal carcinoma after radiation therapy. Open bite could be seen in
the panoramic radiograph.
Figure 2
Figure 2
Pathological fracture of the right mandible caused by unicystic ameloblastoma. A. Preoperative panoramic radiograph showing cystic radiolucency of
the ramus and posterior part of the right mandible with fracture of the angle (arrow). B. Curettage of the lesion and partial resection of the involved bone, and
reconstruction with nonvascularized iliac bone graft. C. Significant bone formation 28 months after operation.
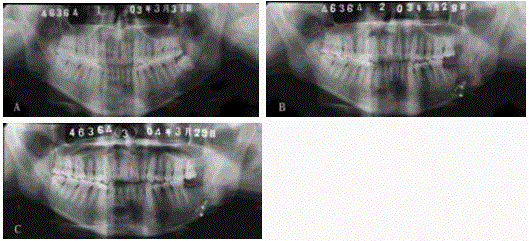
Figure 3
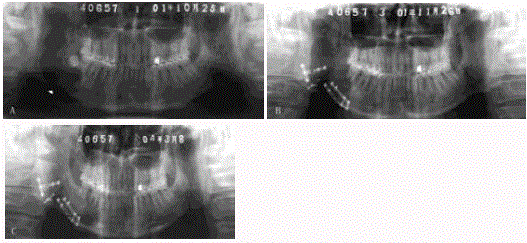
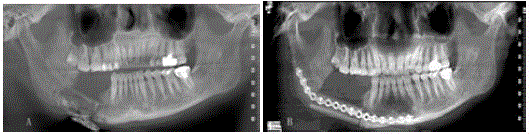
Figure 3
Pathological fracture of the right mandible after embolization and resection of arteriovenous malformation. A. Panoramic radiograph showing fracture
of the body of the right mandible and iodoform strip in the right submandibular region for drainage. B. Segmental mandibulectomy and reconstruction with
vascularized fibular bone graft.
Figure 4
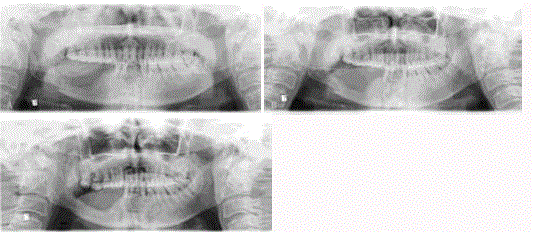
Figure 4
Pathological fracture of the right mandible after rim mandibulectomy for OSCC. A. Panoramic radiograph showing minimal displacement of the fragments
3 weeks after rim mandibulectomy. B. Blurring of the fracture line and callus formation after conservative management by chin cap mandibular immobilization for
50 days. C. Mandibular continuity recovered with bone remodeling after 12 months.
Figure 5
Figure 5
Pathological fracture of the left mandible from enucleation of odontogenic keratocyst. A. Preoperative panoramic radiograph showing unilocular radiolucency of the left posterior mandible. B. Transossous wire fixation of the fracture after enucleation of cyst. C. Significant bone regeneration of the operated area one year postoperation.
Discussion
In the present study, iatrogenic factors including third molar
extraction, rim mandibulectomy or cyst enucleations were common
aetiologies for PFMs. A systemic meta-analysis [7] revealed a higher
rate of PFMs associated with exodontia was in the fifth decade of life
with male prevalence. Seventy-five percent PFMs following tooth
removal were due to third molar removal. The commonly risk factors
more commonly identified were removal of the third molar, fully
dentate patient, associated pathology, impacted tooth, angle region,
and time interval of 3 weeks. In regard to PFMs associated with
marginal (rim) mandibulectomy, a 15% incidence of fracture has
been noted to occur at the osteotomy site [8]. The curvilinear shape of
the osteotomy is biomechanically more favorable than the orthogonal
osteotomy and is more resistant to fracture formation [9]. At least 1
cm vertical height of the lower border of the residual mandible should
be preserved to withstand masticatory loading forces and to prevent
pathological fracture [10-12]. Identifying and addressing the risk
factors will enable the surgeon to avoid the complication of iatrogenic
mandibular fractures. Considerable controversy exists regarding the
treatment strategy for PFMs with iatrogenic factors. Although some
surgeons advocate open reduction and fixation with miniplates
and monocortical screws for iatrogenic mandibular fractures, most
published documents reported the choice of closed reduction for
these fractures [7,13]. Of our 11 cases of iatrogenic mandibular
fractures, 6 cases were conservatively treated by intermaxillary
fixation or chin cap combined with extraoral traction for mandible
immbolization, 3 cases by open reduction and fixation, and 2 cases
by surgical resection with bone graft. Of particular interest was that
a pathologic fracture only treated with a chin cap combined with
extraoral traction eventually healed in the patient who underwent
rim mandibulectomy and irradiated, although bone healing and
remodeling was significantly delayed.
In recent years, the rate of pathological mandibular fractures
associated with ORN significantly increases due to the wide use of
adjuvant radiation therapy for head and neck cancer. One review
of 1000 patients receiving head and neck radiation found 2.6%
developed ORN and 23% of these progressed to pathologic fractures
[14]. In a case study of 44 patients with PFM, Coletti and Ord [5]
noted that the most common cause of PFM was osteoradionecrosis, which implicated in 49 percent of their cases. In our study, the
proportion of ORN was 25.92%, much less than those reported
above. Although the optimum management for osteoradionecrosis
is currently not standardized, surgical resection and vascularized
bone reconstruction has been recommended as the first choice of
treatment for these patients with pathological mandibular fractures
[15-18]. However, advanced stage ORN-related reconstructions are
uniquely challenging [17] since the soft tissues are scarred with poor
healing potential due to their decreased blood supply and absence of
cervical vessels may compromise microvascular flap reconstruction.
Furthermore, treatment planning should be directed towards the
patient’s general health, nutritional status and ruling out recurrent
cancer [13]. Contrary to the increasing rate of ORN, the incidence of
osteomyelitis decreases in recent years possibly because of improved
oral health, early treatment of carious teeth and efficient antibiotic
application. Ideal treatment of PFM associated with osteomyelitis is
considered to be not open reduction with rigid plate fixation but rather
closed reduction with intermaxillary fixation [2] or intermaxillary
elastic traction [19], because open reduction might cause further
ischemic necrosis through periosteal reflection [2]. Spontaneous
bone healing may take place if there is long-term immobilization
of the mandible after complete elimination of the infection with or
without surgical eradication. In our series, three cases of bone healing
occurred when intermaxillary fixation combined with sequestrectomy
or antibiotic therapy was used.
Bony lesions (cysts or tumors) may alter the adjacent bone
and weaken the mandible, thus predisposing it to fracture. PFMs
associated with benign cystic lesions are very rarely reported with
10 cases in the recent literature review [6]. In our series, 2 PFMs
associated with ameloblastomas were identified, and the patients
were treated by segmental mandibulectomy with iliac bone graft.
PFMs are frequently associated with metastatic tumor or primary
oral squamous cell carcinoma [6]. The most frequently involved site
is mandibular angle, followed by the body and condyle. Treatment of
pathological fractures caused by primary or secondary malignancies is
often limited by the patient’s general health, as a pathological fracture
may represent an advanced stage of neoplastic disease. Therefore,
the aim of the treatment is the preservation of oral function and
pain control to maintain quality of life [20]. Secondary metastases
to the mandible are usually from breast, lung, kidney and prostate.
Treatment will depend on the tumor type and patient’s general
condition. Although surgery is an option in selected cases, frequently
radiation therapy or chemotherapy will be given as palliative
treatment. Our case of secondary metastasis of the condyle from
breast adenocarcinoma underwent condylectomy and postoperative radiotherapy due to pain and limited mouth opening associated
with pathological condylar fracture [20]. Two cases of pathological
mandibular fracture associated with OSCC invasion were treated
by segmental mandibulectomy with pedicle myocutaneous flap and
postoperative radiotherapy.
References
- Ezsias A, Sugar AW. Pathological fractures of the mandible: a diagnostic and treatment dilemma. Brit J Oral Maxillofac Surg. 1994;32:303-6.
- Gerhards F, Kuffner HD, Wagner W. Pathological fractures of the mandible. A review of the etiology and treatment. Int J Oral Maxillofac Surg. 1998;27:186-90.
- Grau-Manclús V, Gargallo-Albiol J, Almendros-Marqués N, Gay-Escoda C. Mandibular fractures related to the surgical extraction of impacted lower third molars: a report of 11 cases. J Oral Maxillofac Surg. 2011;69:1286-90.
- Bourhis J, Overgaard J, Audry H, Ang KK, Saunders M, Bernier J, et al. Hyper-fractionated or accelerated radiotherapy in head and neck cancer: A meta-analysis. Lancet. 2006;368:843-54.
- Coletti D, Ord RA. Treatment rationale for pathological fractures of the mandible: A series of 44 fractures. Int J Oral Maxillofac Surg. 2008;37:215-22.
- Boffano P, Roccia F, Gallesio C, Berrone S. Pathological mandibular fractures: a review of the literature of the last two decades. Dental Traumatology. 2013;29:185-96.
- Joshi A, Manu Goel M, Thorat A. Identifying the risk factors causing iatrogenic mandibular fractures associated with exodontia: a systemic meta-analysis of 200 cases from 1953 to 2015. Oral Maxillofac Surg. 2016;20:391-96.
- Barttelbort SW, Bahn SL, Ariyan SA. Rim mandibulectomy for cancer of the oral cavity. Am J Surg. 1987;154:423-28.
- Barttelbort SW, Ariyan S. Mandibule preservation with oral cavity carcinoma: rim mandibulectomy versus sagittal mandibulectomy. Am J Surg. 1993;166:411-15.
- Chen YL, Kuo SW, Fang KH, Hao SP. Prognostic impact of marginal mandibulectomy in the presence of superficial bone invasion and the nononcologic outcome. Head Neck. 2011;33:708-13.
- Werning JW, Byers RM, Novas MA. Preoperative assessment for and outcomes of mandibular conservation surgery. Head Neck. 2001;23:1024-30.
- Ariyan S, Abrahams JJ, Brattelbort SW, Mutalik P. Tomographic studies of humun jaws to assess potentials for preserving the blood supply in rim mandibulectomies. Plast Reconstr Surg. 1995;96:816-22.
- Carlsen A, Marcussen M. Spontaneous fractures of the mandible concept and treatment strategy. Med Oral Patol Oral Cir Bucal. 2016;21:e88-94.
- Epstein JB, Wong FLW, Stevensom-Moore P. Osteoradionecrosis: clinical experience and a proposal for classification. J Oral Maxillofac Surg. 1987;45:104-10.
- Chang DW, Oh HK, Robb GL, Miller MJ. Management of advanced mandibular osteoradionecrosis with free flap reconstruction. Head Neck. 2001;23:830-35.
- Alam DS, Nuara M, Christian J. Analysis of outcomes of vascularized flap reconstruction in patients with advanced mandibular osteoradionecrosis. Otolaryngol Head Neck Surg. 2009;141:196-201.
- Buchbinder D, St Hilaire H. The use of free tissue transfer in advanced osteoradionecrosis of the mandible. J Oral Maxillofac Surg. 2006;64:961-64.
- Sawhney R, Ducic Y. Management of Pathologic fractures of the mandible secondary to osteoradionecrosis. Otolaryngol Head Neck Surg. 2013;148:54-8.
- Ogasawara T, Sano K, Hatsusegawa C, Miyauchi K, Nakamura M, Matsuura H. Pathological fracture of the mandible resulting from osteomyelitis successfully treated with only intermaxillary elastic guiding. Int J Oral Maxillofac Surg. 2007;37:581-3.
- Jia J, Zhang WF, Liu B, Zhao YF. Pathological fracture of condyle from metastatic breast adenocarcinoma. Oral Oncol Extra. 2006;42:98-9.