Case Report
A Case of Ectopic Liver Tissue Adherent to the Gallbladder
Eoghan B, Ilona A and Gerrard O'Donoghue*
Department of Surgery, University Hospital Waterford, Ireland
*Corresponding author: Gerrard O'Donoghue, Department of Surgery, University Hospital Waterford, Waterford, Ireland
Published: 29 Nov, 2017
Cite this article as: Eoghan B, Ilona A, O'Donoghue G. A
Case of Ectopic Liver Tissue Adherent
to the Gallbladder. Clin Surg. 2017; 2:
1770.
Abstract
We report a case of a 30 year old lady who presented to the emergency department with a one day history of severe epigastric pain which radiated to the back. On physical exam she was mildly tender in the epigastrium and right hypochondrium. Labs were notable for an amylase of 1297 U/L. Ultrasound abdomen noted multiple small gallstones in the gallbladder but no wall thickening or intra/extra hepatic bile duct dilatation. She was diagnosed with a gallstone pancreatitis and managed conservatively on initial presentation. She was discharged the following day and underwent elective laparoscopic cholecystectomy as an outpatient. During the laparoscopic surgery, a month later, a small nodule was found loosely adherent to the gallbladder serosa. Histology revealed this to be a portion of anatomically normal liver parenchyma also referred to as Ectopic Liver Tissue (ELT). Ectopic Liver Tissue is a rare developmental abnormality in which normally functioning liver tissue develops at an extra-hepatic site and has no connection to the true liver, in contrast to the accessory lobe of the Liver which has an anatomical connection to the liver proper. ELT has been reported in multiple intra-abdominal and thoracic sites including the kidneys, heart and pleural cavity. The incidence of ELT is debated and widely felt to be underestimated. ELT rarely presents symptomatically, as in our case, and is often diagnosed at autopsy or following surgery for another reason. However because of the increased risk of hepatocellular carcinoma associated with ELT we believe it to be an important congenital abnormality.
Introduction
Ectopic Liver tissue is a rare developmental abnormality in which normally functioning liver tissue develops at an extra-hepatic site and has no connection to the true liver [1], in contrast to the accessory lobe of the Liver which has an anatomical connection to the Liver proper. ELT has been reported in multiple intra-abdominal and thoracic sites including the kidneys, heart and pleural cavity [2-4]. The incidence of ELT is debated and widely felt to be underestimated. ELT rarely presents symptomatically and is often diagnosed at autopsy or following surgery for another reason. However because of the increased risk of hepatocellular carcinoma associated with ELT we believe it to be an important congenital abnormality [5].
Case Presentation
Ms X, a previously well 30 year old lady, presented herself to the emergency department complaining of a one day history of severe epigastric pain. It came on suddenly overnight and woke her from sleep. It radiated through to her back. At its worst she graded it as 10/10. This pain was associated with nausea and two episodes of vomiting. She denied any change in bowel habit, any dark urine or pale stool. Similarly she denied any urinary symptoms and her last menstrual period was three weeks previously. She denied any recent alcohol intake. On physical examination she was mildly tender in the epigastrium and right hypochondium. There was no guarding or rigidity and bowel sounds were present. Vitals were all within normal limits on review in the ED. Bloods (Table 1) were notable for an elevated amylase, Gamma GT and alanaine aminotransferases. C reactive protein was also elevated. Chest X ray was normal and did not indicate any free air under the diaphragm. Ultrasound of the abdomen was performed and identified a gallbladder containing multiple small gallstones. There was no evidence of gallbladder wall thickening or intra/extra hepatic bile duct dilatation (Figure 1). In light of these findings Ms X was admitted as an Imrie o pancreatitis for observation over night. The following day she had clinically improved with resolution of the abdominal pain and tenderness. Bloods had also improved with a fall in amylase and CRP (Table 1). Ms X was discharged and brought back one month later for elective laparoscopic cholecystectomy. She tolerated the procedure well with no immediate complications. Intra operatively there was noted to be a small nodule loosely adherent to the gallbladder serosa (Figure 2). This nodule was removed en bloc with the gallbladder. Histology identified this nodule to be a portion of normal Liver parenchyma without any connection to the Liver proper, i.e Ectopic Liver Tissue (ELT).
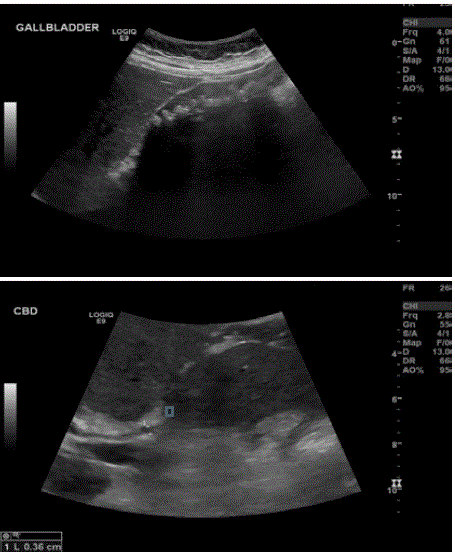
Figure 1
Figure 1
Extensive number of shadowing gallstones in the
gallbladder. Negative for thickening of the anterior gallbladder wall. Negative
for intra or extra hepatic biliary dilatation.
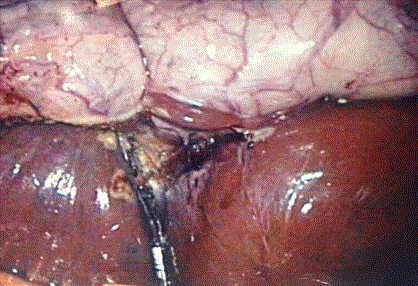
Figure 2
Figure 2
Intraoperative photo displaying gallbladder reflected superiorly,
Liver inferiorly and small nodule of normal liver parenchyma adherent to the
gallbladder.
Discussion
Ectopic Liver Tissue (ELT) is a rare developmental abnormality in which liver tissue develops at an extra-hepatic site with no communication with the liver proper [1]. The true incidence is unknown as it is widely felt to be under-reported. A large study which reviewed over 5500 autopsy cases identified only 13 cases of ELT, another large study which reviewed 1802 laparoscopic cholecystectomy cases identified 12 cases of ELT [6,7]. The precise mechanism behind the development of ectopic liver tissue is poorly understood. The most common site for ELT is the gallbladder although it has been found at various sites including the pancreas, adrenal glands, spleen, falciform ligament, pylorus, retroperitoneally, as well as in the thoracic cavity. An overarching theory has yet to explain its development in such diverse locations [8]. ELT is usually asymptomatic and generally found intraoperatively during surgeries performed for another reason, as in our case, or at autopsy. However ELT is subject to the same pathologies as the liver proper and on occasion has been reported to cause symptoms, predominantly chronic abdominal pain, and secondary to torsion or haemorrhage [1]. Importantly ELT does not contain a complete physiological hepatic lobule architecture often lacking a complete vascular and ductal system. This in turn often leads to the ELT being exposed to carcinogenic material for a prolonged duration which facilitates the carcinogenic process. This is thought to account for the significant observation that ELT seems predisposed to neoplastic transformation independent of the Liver proper [9].
Table 1
Conclusion
ELT is a rare entity. Due to its predominantly asymptomatic nature it is rarely diagnosed pre-operatively. However due to its documented increased risk of neoplastic transformation it seems prudent to remove the ELT when identified serendipitously intraoperatively. Increased awareness of this congenital anomaly may result in increased detection rates among radiologists in the future.
References
- Ioannis Triantafyllidis, Leonidas Papapavlou, Nikolaos Nikoloudis, Athanasios Economou, Efstathios Andreadis, Maria Chrissidou, et al, Ectopic Liver Tissue Attached to the Gallbladder Wall: a case report, Cases J. 2009;2:6786.
- Xu L, Jeudy J, Burke AP. Ectopic hepatic tissue presenting as right atrial mass. Hum. Pathol. 2012;43(6):958-60.
- Iber T, Rintala R. Intrapulmonary ectopic liver. J. Pediatr. Surg. 1999;34(9):1425-6.
- Merve A, Scheimberg I, Ectopic liver tissue in the kidney: case report and literature review, journal of pediatric and developmental pathology. 2014;17(5):382-5.
- Oldani A, Garavoglia M. Hepatocellular Cancer Arising From Ectopic Liver Tissue on Diaphragm in Association with Desmoid Mesenteric Tumor. J Liver. 2013;2:133.
- Eiserth P. BeitragezurKenntnis der Nebenlebern.Virchows Arch A PatholAnatHistopathol. 1941;307:307-13.
- Watanabe M, Matsura T, Takatori Y, Ueki K, Kobatake T, Hidaka M, et al. Five cases of ectopic liver and a case of accessory lobe of the liver. Endoscopy. 1989;21(1):39-42.
- Park WH, Choi SO, Lee SS, Randolph JG. Ectopic umbilical liver in conjunction with biliary atresia: Uncommon association. J Pediatr Surg. 1991;26(2):219-22.
- Arakawa M, Kimura Y, Sakata K, Kubo Y, Fukushima T, Okuda K. Propensity of ectopic liver to hepatocarcinogenesis: case reports and a review of the literature. Hepatology. 1999;29(1):57-61.