Case Report
Hypoglossia with Severe Mandibular Transversal Discrepancy: A Case Report
Afia Sultana1, Lena Björnstrom2 and Mats Sjöström1*
1Department of Odontology, Oral and Maxillofacial Surgery, Umeå University hospital, Umeå, Sweden
2Department of Odontology, Umeå University Hospital, Umeå, Sweden
*Corresponding author: Mats Sjöström, Department of Odontology, Section for Oral and Maxillofacial Surgery, Umeå University Hospital, S-901 87 Umeå, Sweden
Published: 23 Nov, 2017
Cite this article as: Sultana A, Björnstrom L, Sjöström M.
Hypoglossia with Severe Mandibular
Transversal Discrepancy: A Case
Report. Clin Surg. 2017; 2: 1762.
Abstract
Objective: To describe the etiology of hypoglossia, the consequences for oral function and our
experience from treating a young boy with severe mandibular transversal discrepancy.
Materials and Methods: We present a 15 year old boy with hypoglossia and severe mandibular
transversal discrepancy, treated with mandibular midline distraction and orthodontic treatment.
Results: Total treatmenttime is sixyears and the result shows improvement of dental occlusion
relationship as well as enlargement of the tongue resulting in an improved occlusal function.
Conclusion: From this case report it is suggested that a multidisciplinary approach of several
different specialists as pediatric, orthodontists, speech therapists, maxillofacial surgeons and
radiologists are should be involved in examination and treatment planning for this rare diagnosis
in order to improve the patient's quality of life. Early surgical interventions are positive for occlusal
function.
Keywords: Hypoglossia; Mandibular midline distraction; Transversal discrepancy
Introduction
Hypoglossia is a rare congenital malformation, associated with micrognathia of the mandible
and varying degree of limb anomalies [1]. Since the first description by de Jussieu in 1719 less
than 75 cases have been reported with or without anomalies of the extremities [2]. Though the
isolated hypoglossia is not so common but in both cases of isolated hypoglossia and hypoglossia
with syndrome, the common clinical features includes micrognathia, severe transverse deficiency
of mandible, hypodontia, anterior crowding, unilateral or bilateral cross-bite or maxillomandibular
discrepancies, marked enlargement of the sublingual muscular ridge, hypertrophy of sublingual and
submandibular glands narrow basal arch and dentoalveolar bone [3-6].
A child born with hypoglossia together with micrognathia can suffer from apnea and asphyxia
requiring tracheostomy and artificial nasal tube feeding. During early linguistic development, speech
therapy for the improvement of phonetics may be needed. For the micrognathia and malocclusion
correction of transverse deficiency of mandible is recommended in early teens [7-9]. Mandibular
Midline Distraction (MMD) is the surgical procedure done in case of transverse deficiency of
mandible [7,10]. The purpose of this article is to report our experiences from treating a male patient
born with severe transverse deficiency of mandible together with hypoglossia.
Case Presentation
A young patient, born 2001, was referred to the regional cleft team 2010. Medical charts from
a neighboring university hospital reported that the patient was born in pregnancy week 34 with
underweight. Several malformations were diagnosed; duodenal stenosis, missing one kidney,
retrognathic mandible, hypoglossia, uncomplicated heart failure, impaired hearing, choanal
atresia and malformation of costae. No heredity or environmental etiological factors explaining
the malformations could be found. Surgical correction of the duodenal stenosis and the choanal
atresia was performed in early age. Until the age of two, the patient had tracheostomy and feeding
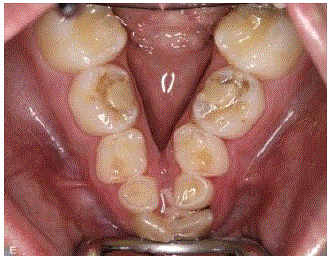
tube due to the retrognathic mandible. The patient’s actual problems 2010 were related with a severe
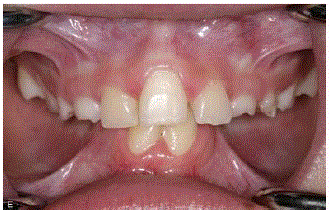
transversal discrepancy in the mandible (Figure 1) resulting in a bilateral scissors bite between the
dental arches (Figure 2). This malocclusion resulted in a diet based only on soft food. Dental analysis
revealed a Class I molar relationship, a severe transversal discrepancy in the mandible with bilateral scissors bite, deep bite with traumatic occlusion to the palatal gingiva.
The mandibular dental arch showed a severe crowding. The dentition
in the mandible was 36, 75-73, 31, 41, 83-85, 46. The dentition in the
maxilla was 16, 55-53, 12, 11, 22, 63-65, 26. Despite the malocclusion,
the patient had a normal range of jaw movement without any muscle
or temporomandibular tenderness. Radiographic examination stated
that the patient was missing two central incisors in the mandible and
one central incisor in the maxilla. The treatment objectives were to
establish harmonious functional occlusion with help of extraction
of 73 and 83, midline distraction in the mandible with bone borne
distractor and fixed appliance for aligning of mandibular teeth.
After the extraction of 73 and 83, there was a two-year delay in
the therapy and during that period, a central mandibular incisor had
to be extracted due to caries. Pre-operative the midline distraction, a
Cone Beam Computer Tomography (CBCT) was performed in order
to prepare a 3D anatomic model. With the model, a bone borne intraoral
Bologna midline distractor (KLS Martin) with a distraction range
of 15 millimeter (mm) could be adjusted. The CBCT examination
visualized a severe crowding of two impacted mandibular cuspids.
In September 2013, the surgery was performed with a vertical
osteotomy in the midline between the cuspids with help of piezo
surgery under general anesthesia. The boy was discharged the first
postoperative day. The active distraction started seven days postop
with a rate of one mm/day (0.5 mm two times a day). The active
distraction period (15 days) was uneventful. From the day of the
surgery and through the active distraction period the patient had a
removable splint in the maxilla for elimination of the deep bite. At the
end of the distraction period a significant change in the mandibular
dental arch was observed.
One week into the consolidation period there was a fracture of
the distractor device resulting in a relapse of approximately half the
distracted length. The device was removed under general anesthesia
and after a healing period of six months the surgical procedure was
repeated. The new Bologna midline distractor (KLS Martin) was
an individually designed hybrid distractor and planned for 15 mm
distraction. The fixation was both in mandibular bone and on the dental
arch through a fixation to a metal splint cemented on the occlusal
plane. The active distraction period started five days postop with a rate
of one mm per day (0.5 mm two times a day). At the end of the active
distraction period, the patient had a nearly normal transversal relation
between maxilla and the mandible. The device was removed after six
months consolidation but the consolidation period was prolonged for
ten more months. During that period the patient had a cemented bar
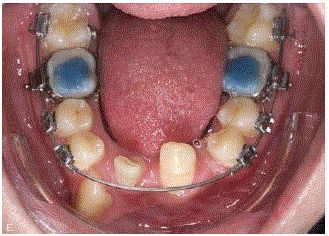
construction in the mandible. The bar construction was then replaced
with fixed appliance in the mandible (Figure 3) in combination with
a removable splint in the upper jaw, used in the night, to prevent
from attrition. At the start of the orthodontic treatment, the patient
had a normal sagittal occlusion, a slightly increased overjet, normal
overbite, and a nearly normal transversal relation between the dental
arches. The orthodontic treatment plan was to transversally expand
the lower dental arch to normal transversal relation and to level both
dental arches. We decided to keep the only upper central incisor in
the midline and, if necessary, replace missing incisors in the lower jaw
with implants after completed growth. Due to transversal instability,
a lifelong retention is essential. We plan for a cemented retainer in
the lower jaw and a removable retainer in the upper jaw. Throughout
the treatment, the patient has shown normal range of jaw movement
without any muscle or temporomandibular tenderness. Radiographic
examination visualizes normal bone support for the teeth in the
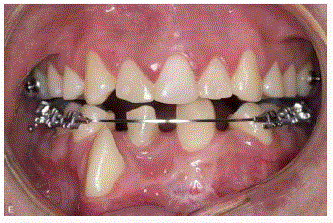
anterior mandible. The actual dental occlusion (Figure 4) allows the
patient to chew food with normal consistence without symptoms
from the temporomandibular joint. Speech therapy is planned for
improvement of phonetics. The patient’s father has given a written
acceptance for publication of the patients’ medical history.
Figure 1
Figure 2
Figure3
Figure 4
Discussion
Hypoglossia is a rare developmental anomaly with unknown pathogenesis, manifested by a very small or rudimentary tongue. Although the etiology of this syndrome is unknown both genetic and environmental factors have been proposed to be responsible for the occurrence [11]. The genetic cause has not been clearly established yet. According to Tan et al. [12] the explanation of hypoglossia is unlikely because of chromosomal aberrations. An autosomal dominant or multifactorial mode of inheritance was proposed by Mishima et al. [13]. On the other hand an autosomal recessive mode of inheritance was proposed by Tuncbilek et al. [14]. Mutation of Msx 2, a homeobox gene may also be responsible for the orofacial and limb anomaly [15]. In contrast, according to, Alexander et al. [16], Pindborg and Gorlin excluded the possibility of genetic abnormality for the syndrome and considered intra uterine environmental factor as the source. Environmental factors include ingestion of teratogenic drugs like Mecilazine, Marjuana, Benzamine hydrochloride, Tigan, Benedictine, Imipramine or Diazepam [17-20]. Radiation exposures during first trimester, intrauterine trauma, chorionic villous sampling procedure, presence of organized thrombi, stapedial artery injury or premature involution are also considered as causative factors [18,21]. Several theories also proposed that the membranous strands, produced by rupturing of amnion during early pregnancy, causes oral anomalies [22]. The medical history could not identify any etiologic factor in the actual case. Stress is necessary for any bony growth and the lack of stimulus from the tongue results in failure of transverse and anterio-posterior growth of the alveolar arches, resulting in formation of severe dentoalveolar malocclusion [22]. These patients require later treatment for the improvement of function (mastication, swallowing and speech) and aesthetics. Mandibular distraction osteogenesis can improve skeletal and soft tissue situation. It also produces regenerated basal bone reducing the risk of relapse [4,23]. The mandibular midline distraction (MMD) in the actual case has resulted in new attached gingiva in the marginal bone, which is positive from a periodontal situation for teeth close to the osteotomy. The start of post distraction orthodontic treatment differs widely ranging from immediately after the active distraction period to 4 months after the end of the distraction period [24-27]. Our patient had a consolidation period for 16 months resulting in normal bone support for the teeth in the anterior mandible. Which distractor is best one for MMD is not defined yet. Alkan A et al. [9] suggested that a lingually placed tooth borne hyrax appliance should be the first choice whether Gijt JP et al. [28] proposed that Rotterdam mandibular distractor (RMD) which is a slim, rigid bone-borne distractor could be used for MMD. Due to the severe transversal discrepancy we could not place the distractor lingually. We used an individually designed reinforced distractor with the goal to reduce the risk for fracture of the device. The most common reported complication associated with MMD includes breakage of distractor in situations with a toothborne distractor [28,29]. The risk of breakage can eventually be due to a vertical osteotomy and occlusal loading. The vertical loading and that our first distractor only had bone fixation could be one reason for the fracture. A step osteotomy could reduce the vertical movement but was not possible to perform in our case. MMD can have effect on temporomandibular joint (TMJ). Kita et al. [7] suggested that early occlusal stability after skeletal expansion is important in the management of TMJ disorders. MMD also improves the bite force and occlusal contact area than preoperative values [8]. With the widening of jaw the tongue size increased in volume in our patient. One can speculate if treatment of hypoglossic patients with MMD at growing age can help to regain the tongue size spontaneously. The MMD can improve the occlusal function for patients with hypoglossia. A lifelong retention in the anterior mandible is necessary to reduce the risk for transversal relapse, probably must depending on the reduced volume of the tongue. Speech therapy is planned for the improvement of phonetics.
Conclusion
In conclusion, it is suggested that a multidisciplinary approach of several different specialists as pediatric, orthodontists, speech therapists, maxillofacial surgeons and oral and maxillofacial radiologists should be involved in examination and treatment planning for this rare diagnosis for improvement of patient's quality of life in situations with hypoglossia with transversal discrepancies in the occlusion. Early surgical intervention is positive for occlusal function.
References
- Hennekem RCM, Krantz ID, Allanson JE. Gorlin’s Syndrome of the Head and Neck. 5th edn. New York: Oxford University Press. 2010;913-22.
- Sharma G, Vengal M, Pai KM, Nagpal A. Hypoglossia Type 1A: report of a case and review of literature with focus on clinical investigations. Indian J Dent Res. 2012;23(2):264-70.
- Guerrero CA, Bell WH, Contasti GI, Rodriguez AM. Mandibular widening by intraoral distraction osteogenesis. Br J Oral Maxillofac Surg. 1997;35(6):383-92.
- Del Santo Jr M, Guerrero CA, Buschang PH, English JD, Samchukov ML, Bell WH. Long-term skeletal and dental effects of mandibular symphyseal distraction osteogenesis. Am J Orthod Dentofacial Orthop. 2000;118(5):485-93.
- Proffit WR, White RP, Sarver DM. Contemporary treatment of dentofacial deformity. St. Louis: Mosby. 2003.
- King JW, Wallace JC. Unilateral Brodie bite treated with distraction osteogenesis. Am J Orthod Dentofacial Orthop. 2004;125(4):500-9.
- Kita H, Kochi S, Yamada A, Imai Y, Konno N, Saitou C, et al. Mandibular widening by distraction osteogenesis in the treatment of a constricted mandible and tele- scopic bite. Cleft Palate Craniofac J. 2004;41(6):664-73.
- Alkan A, Arici S, Sato S. Bite force and occlusal contact area changes following mandibular widening using distraction osteogenesis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(4):432-36.
- de Gijt JP, Vervoorn K, Wolvius EB, Van der Wal KG, Koudstaal MJ. Mandibular midline distraction: a systematic review. J Craniomaxillofac Surg. 2012;40(3):248-60.
- Kessler P, Wiltfang J, Merten HA, Neukam FW. Distraction osteogenesis of the mandible in craniofacial abnormalities. Mund Kiefer Gesichtschir. 2000;4(3):178-82.
- Gorlin RJ, Cohen MM Jr, Hennekam RCM. Syndromes of the Head and Neck, Oxford University Press, New York, NY, USA. 4th edn. 2001.
- Tan HK, Smith JD, Goh DY. Unfused hypoplastic tongue in a newborn. Int J Pediatr Otorhinolaryngol. 1999;49(1):53-61.
- Mishima K, Sugahara T, Mori Y, Sakuda M. Case report: hypoglossia-hypodactylia syndrome. J Cranio Maxillofac Surgery. 1996;24(1):36-9.
- Tuncbilek E, Yalcin C, Atasu M. Aglossia-adactylia syndrome (special emphasis on the inheritance pattern). Clin Genet. 1977;11(6):421-3.
- Grippaudo FR, Kennedy DC. Oromandibular-limb hypogenesis syndromes: a case of aglossia with an intraoral band. Br J Plast Surg. 1998;51(6):480-3.
- Alexander R, Friedman JS, Eichen MM, Buchbinder D. Oromandibular-limb hypogenesis syndrome: type II A, hypoglossia-hypodactylia--report of a case. Br J Oral Maxillofac Surg. 1992;30(6):404-6.
- Nevin NC, Burrows D, Allen G, Kernohan DC. Aglossia-adactylia syndrome. J Med Genet. 1975;12(1):89-93.
- Lustmann J, Lurie R, Struthers P, Garwood A. The hypoglossia--hypodactylia syndrome. Report of 2 cases. Oral Surg Oral Med Oral Pathol. 1981;51(4):403-8.
- Bökesoy I, Aksüyek C, Deniz E. Oromandibular limb hypogenesis/Hanhart's syndrome: possible drug influence on the malformation. Clin Genet. 1983;24(1):47-9.
- Weingarten RT, Walner DL, Holinger LD. Tongue hypoplasia in a newborn. Int J Pediatr Otorhinolaryngol. 1993;25(1-3):235-41.
- Oulis CJ, Thornton JB. Severe congenital hypoglossia and micrognathia with other multiple birth defects. J Oral Pathol. 1982;11(4):27682.
- Nepram SS, Jain P, Huidrom RD. Isolated microglossia: A case report. J Med Soc. 2015;29(3):180-1.
- Conley R, Legan H. Mandibular symphyseal distraction osteogenesis: diagnosis andtreatment planning considerations. Angle Orthod. 2003;73(1):3-11.
- Iseri H, Malkoç S. Long-term skeletal effects of mandibular symphyseal distraction osteogenesis. An implant study. Eur J Orthod. 2005;27(5):512-7.
- Duran I, Malkoc S, Iseri H, Tunali M, Tosun M, Kucukkolbasi H. Microscopic evaluation of mandibular symphyseal distraction osteogenesis. Angle Orthod. 2006;76(3):369-74.
- Seeberger R, Kater W, Davids R, Thiele OC, Edelmann B, Edelmann B, et al. Changes in the mandibular and dento-alveolar structures by the use of tooth borne mandibular symphyseal distraction devices. J Craniomaxillofac Surg. 2011;39(3):177-81.
- Malkoc S, Iseri H, Karaman AI, Mutlu N, Kucukkolbasi H. Effects of mandibular symphyseal distraction osteogenesis on mandibular structures. Am J Orthod Dentofacial Orthop. 2006;130(5):603-11.
- Alkan A, Ozer M, Bas B, Bayram M, Celebi N, Inal S, et al. Mandibular symphyseal distraction osteogenesis: review of three techniques. Int J Oral Maxillofac Surg. 2007;36(2):111-17.
- Weil TS, Van Sickels JE, Payne CJ. Distraction osteogenesis for correction of trans-verse mandibular deficiency: a preliminary report. J Oral Maxillofac Surg. 1997;55(9):953-60.
- Bell WH, Gonzalez M, Samchukov ML, Guerrero CA. Intraoral widening and lengthening of the mandible in baboons by distraction osteogenesis. J Oral Maxillofac Surg. 1999;57(5):548-62.