Case Report
The Paradoxical Cerebral Herniation and Pseudohipoxic Brain Swelling: Two Lethal Forms of Severe Intracranial Hypotension
Ricardo Díaz-Romero*
Department of Neurosurgery, Hospital Insular of Las Palmas, Spain
*Corresponding author: Ricardo Díaz-Romero, Department of Neurosurgery, Hospital Insular of Las Palmas, Plaza Doctor Pasteur, s/n., 35016, Las Palmas de Gran Canaria, Spain
Published: 23 Nov, 2017
Cite this article as: Díaz-Romero R. The Paradoxical
Cerebral Herniation and Pseudohipoxic
Brain Swelling: Two Lethal Forms of
Severe Intracranial Hypotension. Clin
Surg. 2017; 2: 1760.
Abstract
Paradoxical Cerebral Herniation (PCH) is a life-threatening condition in patients with large
craniectomies precipitated by a gradient between the atmospheric and intracranial pressure
resulting in brain compression.
Keywords: Paradoxical cerebral herniation; Pseudohipoxic brain swelling; Severe intracranial
hypotension
Introduction
There are several reports of sudden neurological impairment after uneventful surgeries with imaging resemble those of hypoxic encephalopathy, and are caused by a sudden intracranial hypotension by the effect of negative pressure drainage this entity is known as Pseudohipoxic brain swelling (PBS) [1-3].
Case Presentation
This is a case report of a 17-year-old male that suffered a severe TBI with bifrontal craniectomy.
After uneventful cranioplasty repair with autologous graft a sudden neurological deterioration up
to coma was verified, concomitant with a high output of the aspiration subgaleal drainage; head CT
showed diffuse cerebral swelling with hypodensity predominantly on the basal ganglia. Soon after
the patient developed signs of brain death and dies (Figure 1).
Case 2
A 46-year-old male underwent hemicraniectomy after a severe TBI with satisfactory recovery
with a GCS of 14. Two and half month’s later patient suffered rapid neurologic deterioration,
accompanied by prominently depressed skin flap. No evident CFS leak was found. An emergency
cranioplasty repair was performed followed within a few hours by dramatic clinical and radiological
improvement. The patient returned to his previous condition and remained asymptomatic at the
one-year follow-up (Figure 2).
Conclusion
We report two infrequent but lethal caused by severe intracranial hypotension. For PBS epidural aspiration drains should be avoided and is advisable to perform cranioplasty before 3 months for preventing PCH.
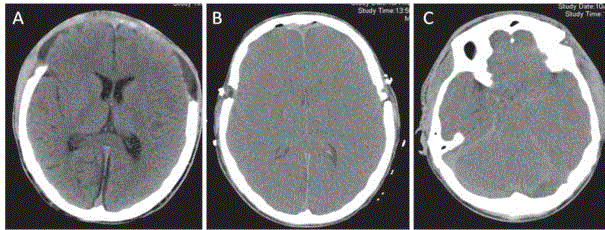
Figure 1
Figure 1
(A) Axial cranial CT showing a bifrontal craniectomy, (B) Severe diffuse brain swelling, mild hypodensity
basal ganglia, (C) Effacement of cranial base cisterns.
Figure 2
Figure 2
Axial CT scans. (A, B) Marked concavity at the craniectomy
site, displacement and compression of the brain with 17 mm midline shift,
effaced sulci, basal cistern obliteration and uncal herniation with brainstem
compression immediately prior to the emergency cranioplasty. (C, D) Five
hours after this cranioplasty significant decrease of the midline shift is
noted along with reappearance of basal cisterns and resolution of signs of
transtentorial herniation with reduced dilation of left temporal horn.
References
- Paldino M, Mogilner AY, Tenner MS. Intracranial hypotension syndrome: a comprehensive review. Neurosurgical Focus. 2003;15(6):1-8.
- Van Roost D, Thees C, Brenke C, Oppel F, Winkler PA, Schramm J. Pseudohypoxic brain swelling: a newly defined complication after uneventful brain surgery, probably related to suction drainage. Neurosurgery. 2003;53(6):1315-27.
- Díaz-Romero R, Avendaño P, Coloma G. Life-threatening paradoxical brain herniation rapidly reversed by emergency cranioplasty repair: a case report. Acta neurochirurgica. 2015;157(11):2031-2.