Mini Reviewt
Ultrasound Assisted Mini Abdominoplasty – Mini Review
Alfredo Hoyos1* and David E Guarin2
1Department of Plastic, Aesthetic, Maxillofacial, and Hand Surgery, University of San Martin in Bogota, Colombia
2Department of Plastic Surgery, Universidad del Valle, Hospital Universitario del Valle, Colombia
*Corresponding author: Alfredo Hoyos, Department of Plastic, Aesthetic, Maxillofacial, and Hand Surgery, University of San Martin in Bogota, Carrera 15# 83–33, Suite 304, Bogotá, Colombia
Published: 23 Nov, 2017
Cite this article as: Hoyos A, Guarin DE. Ultrasound
Assisted Mini Abdominoplasty – Mini
Review. Clin Surg. 2017; 2: 1759.
Abstract
High definition techniques added to the limited abdominoplasty technique allows achieving natural fit and aesthetically pleasant outcomes to the post-delivery woman with a reduced morbidity and faster recovery. The muscular diastasis, skin laxity and extra fat deposits and accurately be managed. Keywords: Vaser; UAL; High definition; Abdominoplasty
Key Points
1. The traditional mini or limited abdominoplasty approaches cannot achieve the best aesthetic outcomes. 2. The ultrasound assisted liposuction is a useful tool to improve the limited Abdominoplasty outcomes and recovery time.
Introduction
The post-delivery abdominal wall changes including skin laxity, stretch marks and muscular diastasis have been managed by means of an abdominoplasty. The adding of adjuvant procedures like liposuction has help to enhance the outcomes as well as the patient satisfaction [1]. However, there are patients with not enough skin laxity to consider an abdominoplasty. To approach this issue Greminger (1987) and Wilkinson (1988) introduce a “limited” or “mini” abdominoplasty to manage the skin laxity and excess of the lower mid-region of the abdomen [2,3]. Notwithstanding the technique refinements, current approaches are still far from optimal. Adjuvant tools such as ultrasound technologies assists the surgeon work by breaking down the adipocytes facilitating the extraction and enhancing the results in a secure and effective way [4]. With the help of this technology, a natural athletic contour of the female abdominal wall can be achieved by means of multi-layer liposculpture to define the contour and the superficial anatomy of the rectus abdominis and oblique muscles. This paper discusses the use of the ultrasound technologies and the hidefinition techniques in conjunction of the mini Lipectomy approach to achieve a natural athletic abdomen in post-delivery patients.
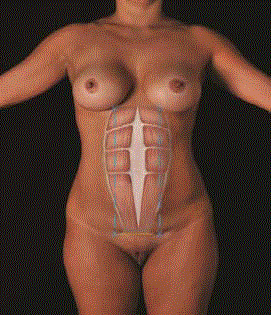
Figure 1
Figure 1
Abdominal marking.
Diastasis of the rectus abdomen is muscles: Mark the origin and insertion of
the muscles and draw a line between them (blue line).
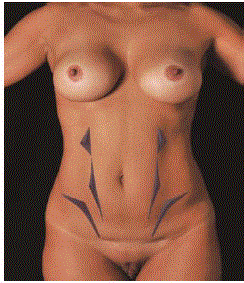
Figure 2
Figure 2
Negative Areas.
Mark the negative areas below the costal margin, the midline and lateral to
the rectus abdominis lower insertion to recreate the lights and shadows of
the superficial anatomy.
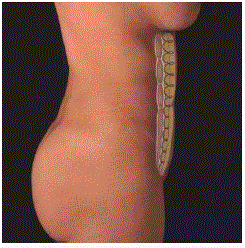
Figure 3
Figure 3
Abdominal flap suture.
The progressive tension sutures the abdominal flap to the midline. From the
xyphoid down to the umbilicus use deep from to enhance the midline. Down
the umbilicus use only superficial continuous stitches.
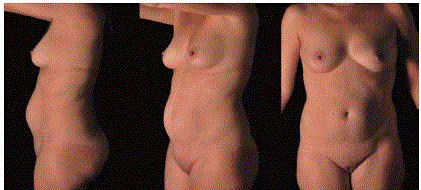
Figure 4a
Figure 4a
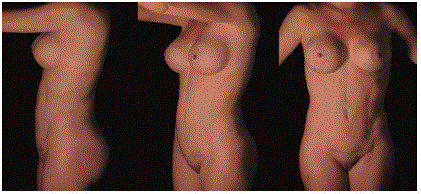
A 30-year-old female. She had a delivery 6 years before the
procedure. Note the central bulge in the mid and lower abdomen due rectus
abdominis muscle diastasis.
Figure 4b
Figure 4b
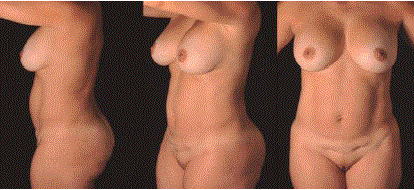
Ultrasound assisted mini abdominoplasty. 14 months after
surgery. The diastasis was corrected and muscular definition was achieved.
Periareolar breast augmentation as well as 400 ml gluteal fat grafting was
also done.
Figure 5a
Figure 5a
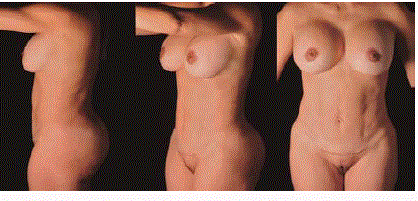
A 44-year-old female with a previous C- section 10 years before.
Note the supra umbilical bulge due to the diastasis.
Figure 5b
Figure 5b
Ultrasound assisted mini abdominoplasty. 7 months after surgery.
The Diastasis was corrected and a natural abdomen with an athletic contour
was achieved. 350 ml gluteal fat grafting and breast implant exchange was
also done.
Patient Selection and Classification
The candidates for this procedure are woman with: minimum of 6 months after childbirth, a Matarasso abdominal skin laxity type I or II [5], a Body Mass Index below 30 kg/m2 with or without muscular diastasis and general good health. Patients with severe skin laxity and post bariatric patients are not good candidates for this procedure. The procedure must be done 6 months after the delivery to allow breast-feeding and the regression of the size of the uterus and skin elasticity regression to normal [1]. Previous procedures on the abdominal wall do not contraindicate the procedure but must be taking in to account for the surgical planning
Preparation
Patient counseling including adequate venous thromboembolism risk assessment [6,7], a carefully review of the expectations, information about the procedure, the risks, the complications and the recovery must be written in the consent. The preoperative set of standard photographic record is also critical.
Patient Marking
With the patient in standing position begin with the deep liposuction marks in the trunk, abdomen, buttocks, thighs and arms. Then mark the abdominal midline. Locate the superior and inferior insertions of the rectus abdominis in contraction and connect the points to guide the lateral borders place after the muscle placation (Figure 1). Mark the areas below the costal margin, the midline and lateral to the rectus abdominis lower insertion for extra liposuction to recreate the superficial anatomy (Figure 2) [1]. A horizontal line in the superior border of the pubic hair insertion, following a convex curved line, from 10 cm to 12 cm long is marked. The cesarean section scar can also be used for access the abdominal wall for plication of the rectus muscles.
Operative Technique
The Procedure is done in 2 phases: First liposuction and then the
mini-abdominoplasty.
Liposuction
Begin with the patient in prone position; infiltrate the tumescent
solution (1000 ml of saline plus 10 ml of 1% lidocaine and 1 ml of
epinephrine) with a volume enough to achieve an infiltration/
extraction ratio of 2:1 to 1.5:1. Apply the third generation ultrasound
(VASER® - Valeant Pharmaceuticals North America LLC) with a 3.7
mm 2-ring probes in 80% continuous mode in the deep layer and
pulse mode blended between the superficial, intermediate layers. The
fat extraction is facilitated by using powered-assisted liposuction
(POWER X Lipo® - Valeant Pharmaceuticals North America LLC).
Begin with the deep fat layer using 4.6 mm and 3.7 mm cannulas until
reaching the desired flap thickness. Use small diameter, low trauma
whole pattern to reduce the flap vascular injury.
Follow the markings of the supra umbilical midline and the
negative areas to perform superficial liposuction using 3.0 mm
cannulas and achieve the desired etching.
Mini-abdominoplasty
Make a transverse incision over the supra pubic marking or use
the previous Pfannestiel scar of the Cesarean surgery [8]. Raise the
anterior abdominal flap from the pubic incision up to the xiphoid
process in a supra fascial layer creating a central tunnel. Release
the umbilicus from its base to access the upper abdominal flap. The
rectus abdominis muscle diastasis is plicated by two-layer stitching
using a double x stitches, with 0 Nurolon suture (NUROLON® -
Ethicon, Inc, Somerville, New Jersey), and later a running Vicryl 0
suture (VICRYL® - Ethicon, Inc, Somerville, New Jersey). Suture
the abdominal flap to the midline by using a progressive tension technique starting with a profound continuous stitches from the
xyphoid down to the umbilicus (enhance the midline in the upper
abdomen) and then superficial below the umbilicus (Figure 3). Fix
the umbilicus to the muscle fascia with 4.0 Vicryl. Remove the excess
of skin and fat tissues. Use a close negative pressured drain and
suture the flap in layers. Extra liposuction can be done to enhance the
athletic depressions and contour.
After Care
Closely follow the antithrombotic measures according to the
risk score [6]. The early mobilization is mandatory for every patient.
Compression garment and a foam vest are indicated for up to 2
months as well as daily drainage.
The drain is left for 3 up to 10 days when the drainage is less
than 50 ml in 24 hours. In the postoperative office checkup include
standard set of photographs (Figure 4 and 5).
Discussion
The abdominal skin laxity and contour changes after delivery are common concerns that not always have the criteria to consider a conventional abdominoplasty technique. The “limited” or “mini” abdominoplasty proposed by Greminger [2] and Wilkinson [3] to deal with patients with limit to borderline laxity cannot achieve all the desired aesthetic outcomes of a natural and athletic abdomen. By adding the high definition lipoplasty techniques [4,9] to the mini abdominoplasty approach the aesthetic outcomes are improved and the natural, athletic and aesthetically desired abdomen can be recreated. This approach uses a minimal scar, resolve the rectus abdominis diastasis, enhance the overall contour and recreate the natural lights and shadows of a healthy fit abdomen. This minor invasive approach is associated with less bleeding, shorter surgical time and a faster postoperative recovery. The technique require the adequate knowledge and training in the use of energy based liposuction technologies, however is easily reproducible and have a low morbidity with a high satisfaction index among patients [1].
References
- Hoyos AE, Perez ME, Castillo L. Dynamic definition mini-lipoabdominoplasty combining multilayer liposculpture, fat grafting, and muscular plication. Aesthet Surg J. 2013;33(4):545-60.
- Greminger RF. The mini-abdominoplasty. Plast Reconstr Surg. 1987;79(3):356-65.
- Wilkinson TS. Mini-abdominoplasty. Plast Reconstr Surg. 1988;82(5):917-8.
- Hoyos AE, Millard JA. VASER-assisted high-definition liposculpture. Aesthet Surg J. 2007;27(6):594-604.
- Matarasso A, Matarasso DM, Matarasso EJ. Abdominoplasty: classic principles and technique. Clin Plast Surg. 2014;41(4):655-72.
- Iorio ML, Venturi ML, Davison SP. Practical guidelines for venous thromboembolism chemoprophylaxis in elective plastic surgery. Plast Reconstr Surg. 2015;135(2):413-23.
- Pannucci CJ. Evidence-Based Recipes for Venous Thromboembolism Prophylaxis: A Practical Safety Guide. Plast Reconstr Surg. 2017;139(2):520e-32e.
- Decarle DW, Durfee RB. The Pfannenstiel incision for cesarean section. West J Surg Obstet Gynecol. 1948;56(6):360-64.
- Hoyos AE, Prendergast PM. High Definition Body Sculpting: Art and Advanced Lipoplasty Techniques. Springer Berlin Heidelberg. 2014.