Case Report
A New Treatment for Primitive Neuroectodermal Tumor (PNET) of Prostate: Total Pelvic Exenteration (TPE) and Double Diversion
Lichen Teng, Wei Liangjun, Yongpeng Xu and Changfu Li*
Department of Urology, Harbin Medical University Cancer Hospital, Harbin city, China
*Corresponding author: Changfu Li, Department of Urology, Harbin Medical University Cancer Hospital, Harbin city, Postal code: 150080, China
Published: 23 Nov, 2017
Cite this article as: Teng L, Liangjun W, Xu Y, Li C.
A New Treatment for Primitive
Neuroectodermal Tumor (PNET) of
Prostate: Total Pelvic Exenteration
(TPE) and Double Diversion. Clin Surg.
2017; 2: 1758.
Abstract
Introduction: To report a rare case of Primitive Neuroectodermal Tumor (PNET) of prostate and
to present a new surgical method for PNET of prostate.
Materials and Methods: A 27-year-old male was admitted to Harbin Medical University Cancer
Hospital (Harbin, China) for dysuria and dyschezia, magnetic resonance imaging (MRI) reveal a
large mass that may involve bladder and rectum in the prostate region. Histopathological analysis
of biopsy of prostate indicated mesenchymal origin tumor, and immunohistochemistric confirmed
diagnosis of PNET of prostate. En bloc Total Pelvic Exenteration (TPE) and double barrel
sigmoidostomy were performed. Double stomas in the skin incision are used for fecal and urinary
diversion, respectively.
Results: Related complications, such as urinary tract infection and ileus do not occur. Short-term
outcome in the case is satisfactory, normal diet can be taken. However long-term efficacy remains
to be evaluated.
Conclusion: Clinical features of PNET of prostate should be paid much more attention and radical
surgery is recommended.
Keywords: Prostate; Primitive neuroectodermal tumor; Total pelvic exenteration; Double
barrel sigmoidostomy
Introduction
According to the tissue of origin, Primitive Neuroectodermal Tumor (PNTE) is divided into central PNTE and peripheral PNTE. A large size of infiltrative soft mass is a common feature of them[1]. Incidence of PNET occurring in urological organs is very low, previous reports about PNET mainly originated from kidney, bladder, and adrenal glands and so on. Compared with these organs, PNET of prostate is rarer, until to 2003, Peyromaure M documented first case in the world. Up to date, only less than twenty cases of PNET of prostate. The disease appears clinical features of tumors of mesenchymal tissue, such as poor prognosis and lack of optimal model of treatment. Combined therapies are considered now, including surgery, chemotherapy, radiotherapy and so on. How to choice optimal therapy is difficult for urologic oncologists. At December of 2016, we treated a case of PNET of prostate using total pelvic exenteration and double barrel sigmoidostomy, the patient obtains satisfactory efficacy following surgery.
Case Presentation
A 27-year-old male patient presented to Outpatient of Harbin Medical University Cancer
Hospital (Harbin, China), who complained symptoms of dysuria and dyschezia for two weeks.
Moreover, he has indwelled catheter for two days in the local hospital. After the patient was
hospitalized, the result of digital rectal examination indicated that a large smooth mass significantly
swelled to the rectal cavity. Laboratory examination showed that value of serum Prostate Special
Antigen (PSA) was 1.52 ng/mL and white blood cells (WBC) were 13 × 109/L, and the magnetic
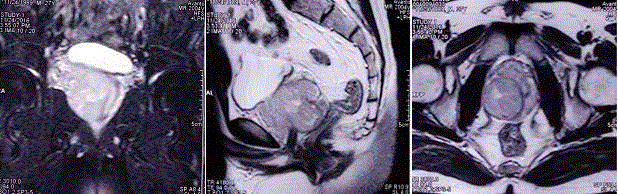
resonance imaging (MRI) revealed a mass of 84 mm × 78 mm × 72 mm replaced the prostate gland,
which may involve posterior wall of bladder and anterior wall of rectum (Figure 1). Transrectal
biopsy of the prostate gland was performed. Pathological analysis demonstrated malignant tumor
of prostate gland mesenchymal origin and untypical morphology. The tumor cells were positive
for Desmin and Vim and negative for CD34, CD117 and SMA. The patient was diagnosed as large prostate tumor and urinary tract infection. After antibiotic treatment of couple days, we carefully communicate with the patient and his
dependants about plan for treatment. Finally, we performed total
pelvic exenteration and double barrel sigmoidostomy.
During operation, we found a large firm mass companied with
surrounding tissue edema, which filled and fixed in pelvic cavity. After
en bloc resection of total pelvic organs, 15-cm distal sigmoid colon
of stoma was closed. Bilateral ureters were anastomosed end-to-side
with sigmoid colon respectively, in which stents were indwelled. The
anastomotic site was placed in retroperitoneal space. While faeces are
evacuated through upper stoma, urine is discharged via lower one
(Figure 2). At 48 h after operation, the patient started to drink, and
the patient was allowed to eat at day 4 post-operation. At day 5 postoperation,
the patient can freely ambulate, and he was discharged
from hospital at week 2 post-operation. The histopathological study
revealed that area of tumor filled with small round cells (Figure 3 A),
indicating a PNET, moreover, bladder and rectum were involved, and
pelvic lymph nodes has not found metastasis. The cells were positive
for Vim, CD56 and CD99 (Figure 3B-D), and negative for CK and
CD34 (Figure 3E and 3F).
Figure 1
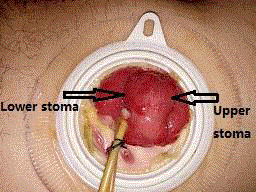
Figure 2
Figure 2
Double barrel sigmoidostomy: upper stoma is used for fecal
diversion, and lower one is used for urinary diversion.
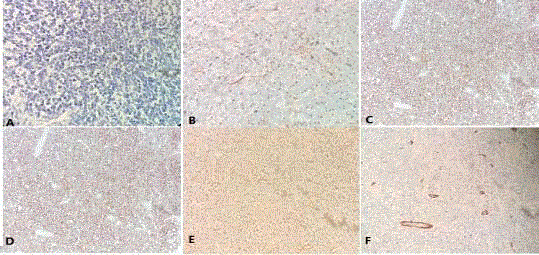
Figure 3
Figure 3
Representive images with E staining and immunohistochemistric
staining (× 200).
A.E. Staining revealed a lot of small round cells distributed in tumor region.
B.Immunohistochemistric staining demonstrating small round cells positive
for CD99; C and D reveal small round cells is positive for CD56 and Vim,
respectively. E and F show small round cells negative for CK and CD34,
respectively.
Discussion
PNET is kind of extremely rare malignant tumor with high
aggressiveness. Early diagnosis and timely radical surgery would
contribute to prolong survival. Therefore, to improve the rate of
early diagnosis and obtain satisfactory outcome, it is very important
to deeply understand its clinical features, and to reasonably choose
treatment regimen.
Clinical features
Peripheral PNET can originate from different organs or tissues,
such as lung, liver and vertebra and so on, however, PNET of urologic
organs-origin is rare, among them, kidney is a mainly organ of origin,
compared with which, incidence of PNET of prostate gland is much
less. Additionally, the disease commonly occurs in range in age of 20
to 30-year-old. To our best knowledge, from 2003 to now total sixteen
cases along with our case have been reported [2-13], median age is
27 years. Due to insidious onset, there is commonly asymptomatic
for the patients at early stage, thereafter, with increasing of tumor
size, significant dysuria and dyschezia would seriously affect life of
the patients, hematuria and chronic anal pains are also complained
by some patients, in addition, a lot of residual urine and frequent
indwelling catheter also result in refractory urinary tract infections.
All of cases exhibited large diameter of primary tumor (>5 cm) at
diagnosis. Digital rectal exam should be performed. Similarly to our
case, the value of PSA maintain in the normal range in most cases
except for two cases. 7,8 Primary tumor appear rapid progress,
in the present case, the diameter of tumor increase by about 1 cm
duration one month, incidence of multiple distal metastases for
PNET of prostate gland is low, two cases of pulmonary and lymph
node metastasis were reported [9-11]. Imaging examinations,
such as Computed Tomography (CT) and MRI can show a large
occupying lesion replaced prostate gland in the pelvic cavity,
which may involve and shift surrounding organs, such as bladder,
rectum or seminal vesicles. Except for some necessary imaging
examinations, establishment of PNET of prostate gland mainly rely
on immunohistochemistric staining, which can confirm PNET by
positive for CD99 and/or other neuronal markers in a lot of small
round cells, at the same time, lymphoma and myogenic tumor need
to be excluded.
Treatment
Due to low incidence of PNET of the prostate and cohort study
of large number of cases, currently, the standard treatment regimen
has not yet been established. In the previous studies, combined
therapy with surgery, neoadjuvant or adjuvant chemotherapy and
radiation therapy were effective, and most of cases underwent radical
prostatectomy [2,3,9,11]. Because peripheral PNET prong to develop
distant metastases and local recurrence within 2-3 year after surgery,
to decrease this possibility, as for localized PNET of prostate [14],
we performed aggressively an en bloc total pelvic exenteration in the
present case, and double barrel sigmoidostomy is used for with both
the urinary and fecal diversions [15]. Compared with ureterostomy
or urinary conduit diversion, we take advantage of reflected part of sigmoid colon with end in subtle ways as urinary diversion. It is helpful
to nurse stoma and improve quality of life, more importantly, the
operation has not increase incidence of related complications, such as
gut leakage and urinary tract infection; moreover, surgical complexity
is not increased furthermore. The long-term outcome remains to be
evaluated in the future. Except for radical surgery, chemotherapy is
a potentially effective treatment for localized PNET of the prostate
[16]. Chemotherapeutic agents include incristine (V), driamycin/
Doxorubicin (A), cyclophosphamide (C) and Actinomycin-D,
which are commonly used in combination with each other [17].
In conclusion, although PNET of prostate is extremely rare, but
urologic oncologists should pay much more attention to the young
male patients with above mentioned clinical features. To minimize
the harm of the disease, radical surgery should be performed as early
as possible in localized PNET of prostate, combined therapy is help to
improve efficacy of treatment.
Compliance with Ethical Standard
The study was supported by Heilongjiang postdoctoral scientific research developmental fund (LBH-Q15104) and by a grant from Heilongjiang Provincial Department of Public Health (670). All procedures performed in studies were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration, and informed consent was obtained from patient in the study.
References
- Virani MJ, Jain S. Primary intraspinal primitive neuroectodermal tumor (PNET): a rare occurrence. Neurology India. 2002;50(1):75-80.
- Peyromaure M, Vieillefond A, Boucher E, De Pinieux G, Beuzeboc P, Debré B, et al. Primitive neuroectodermal tumor of the prostate. J Urol. 2003;170(1):182-3.
- Colecchia M, Dagrada G, Poliani PL, Messina A, Pilotti S. Primary primitive peripheral neuroectodermal tumor of the prostate. Immunophenotypic and molecular study of a case. Arch Pathol Lab Med. 2003;127(4):el90-3.
- Thete N, Rastogi D, Arya S, Singh A, Rao P, Chandge A, et al. Primitive neuroectodermal tumour of the prostate gland: ultrasound and MRI findings. Br J Radiol. 2007;80(956):e180-3.
- Al Haddabi I, Al Bahri M, Burney I. Cytokeratin-positive primitive neuroectodermal tumor of the prostate: case report and review of literature. Indian J Pathol Microbiol. 2012;55(4):569-71.
- Kumar V, Khurana N, Rathi AK, Malhotra A, Sharma K, Abhishek A, et al. Primitive neuroectodermal tumor of prostate. Indian J Pathol Microbiol. 2008;51(3):386-8.
- Zhao SM, He CH, Ren JK. Primitive neuroectodemal tumour of the prostate and lung metastasis: a case report. Chin J Urol. 2013;34:737.
- Liu Z, Pu JX. Primitive neuroeetodermal tumour of the prostate: two case report and literature review. Literature of No.15 Chinese Urology Academic Conference. 2008.
- Funahashi Y, Yoshino Y, Hattori R. Ewing's sarcoma/primitive neuroectodermal tumor of the prostate. Int J Urol. 2009;16(9):769.
- Mohsin R, Hashmi A, Mubarak M, Sultan G, Shehzad A, Qayum A. Primitive neuroectodermal tumor/Ewing's sarcoma in adult uro-oncology: A case series from a developing country. Urol Ann. 2011;3(2):103-7.
- Wu T, Jin T, Luo D, Lin Chen, Xiang Li. Ewing's sarcoma/primitive neuroectodermal tumor of the prostate: A case report and literature review. Can Urol Assoc J. 2013;7(5-6): E458-E9.
- Li X, Bu R. One case report of prostate primitive neuroectodermal tumor performed hematuresis and literature review. Modern Oncol. 2015;23:2031-4.
- Liao C, Wu X, Wang X, Li H. Primitive neuroectodermal tumor of the prostate: Case report from China. J Cancer Res Ther. 2015;11(3):668.
- Song HC, Sun N, Zhang WP, Huang CR. Primary Ewing’s sarcoma/primitive neuroectodermal tumor of the urogenital tract in children. Chin Med J (Engl). 2012;125(5):932-6.
- Mao Q, Li H, Xiao L. Retrospective analysis of surgical treatment for adult prostate sarcoma. Chin J Urol. 2016;37:30-3.
- Balamuth NJ, Womer RB. Ewing's sarcoma. Lancet Oncol. 2010;11(2):184-92.
- Tan Y, Zhang H, Ma GL, En-hua Xiao, Xiao-chun Wang. Peripheral primitive neuroectodermal tumor: dynamic CT, MRI and clinicopathological characteristics--analysis of 36 cases and review of the literature. Oncotarget. 2014;5(24):12968-77.