Mini Review
Bertolotti’s Syndrome and Its Management; Pain Physician Perspective -A Brief Review
Ashok Jadon*
Department of Anaesthesia & Pain Relief Services, Tata Motors Hospital, Jamshedpur-831004, India
*Corresponding author: Ashok Jadon, Department of Anaesthesia & Pain Relief Services, Tata Motors Hospital, Jamshedpur-831004, India
Published: 16 Nov, 2017
Cite this article as: Jadon A. Bertolotti’s Syndrome and
Its Management; Pain Physician
Perspective -A Brief Review. Clin Surg.
2017; 2: 1737.
Abstract
Low Back Pain (LBP) is multifactorial and often challenging for definitive diagnosis and successful
treatment. Transitional vertebra (sacralization of lumbar vertebra or lumbarization of sacral vertebra)
also known as Bertolotti’s syndrome is an important etiological factor in LBP. The symptoms are not
uniform and therefore the treatment is mostly symptomatic. The surgical treatment is the last resort
where all other treatments have failed to provide relief.
Keywords: Low back pain; Bertolotti’s syndrome; Transitional vertebra; Lumbarization;
Sacralization; Radiofrequency ablation
Introduction
Low back pain in the presence of Lumbosacral Transitional Vertebra (LSTV) originally noted by Mario Bertolotti in 1917 and termed as “Bertolotti’s Syndrome”. The prevalence of LSTV in patients seeking treatment for low back pain ranges from 4.6% to 35.6% [1,2]. The etiopthogenesis of LSTV is still elusive however; HOX genes, which regulate the segmentation of the vertebral column into individual vertebral segments and functional requirements of load transmission at the SI junction, have been postulated as causes of LSTV.
Pathogenesis of Back Pain
Causes of Formation of LSTV or Sacralization leads to changes in dynamics of load transmission resulting in significant morphological changes in various parts of spine. Changes in width of lamina and cancellous bone content, reduced height of pars interarticularis and alteration in facet morphology are few of the examples which are possibly related to low back pain [3]. Other causes of back pain in LSTV includes thinner and weaker iliolumbar ligaments result in vertebral segment instability and could subsequently lead to early disc degeneration. It is not known that, the weak iliolumbar ligaments is a result of LSTV or, represent an adaptive mechanism to preserve stability (to compensate for a weak iliolumbar ligament) [4]. In Type II LSTV, the pseudo-articulation between the transverse process and the sacrum creates a pseudo-articulation or “false joint”. This localized stress at the articulation contributes to low back pain [5] . LSTV may produce low back pain due to arthritic changes occurring at the site of pseudoarthrosis [6] or due to disc herniation or degeneration, facet joint arthrosis, or spinal canal or foraminal stenosis [7]. Disc protrusion or extrusion above the transitional vertebra could lead to radiating pain as a result of nerve root compression and chemical irritation [8]. Hypermobility and abnormal torque moments at the level immediately above the transitional vertebra and restricted movement between the L5 and S1 vertebra result in degenerative changes at the level above the anomalous articulation. The presence of an LSTV can result in pinching of a lumbar spinal nerve between the transverse process of the 5th lumbar vertebra and the sacral ala, a condition known as "Far-Out Syndrome" [9]. Extra-foraminal entrapment of the spinal nerve leading to radiculopathy may occur from the “micro motion” at dysplastic facet joints (at the level below the transitional vertebra) due to resultant Osteoporosis.
Prevalence of Back Pain with Type of LSTV
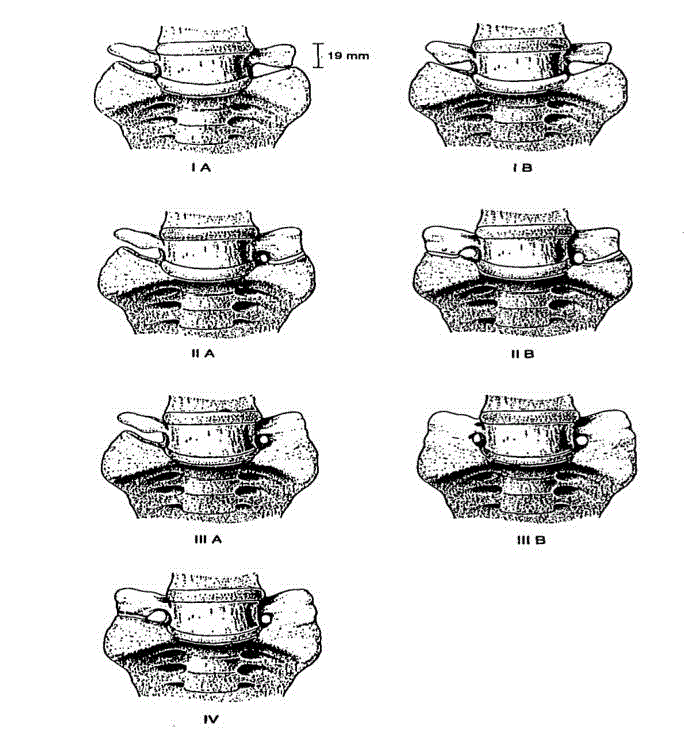
There are four variations (Type IA IB, IIA, IIB, IIIA, IIIB and IV) of LSTV depending on the presence of elongated transverse process and its fusion with sacrum (Figure 1). Of all, 46% patients with a Type I and 40% of patients with a Type III, 73% of patients with Type II and 66% of patients with Type IV reported low back pain. Type II and Type IV LSTV positively correlate with increased prevalence and greater severity of low back and buttock pain. Severity of back pain increases with the presence of LSTV.
Figure 1
Figure 1
Types of LSTV depending upon the presence of elongated
transverse process of transitional vertebra and articulation with sacrum.
Figure 2
Figure 2
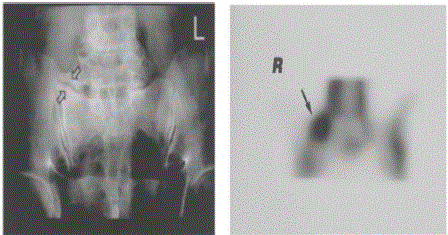
Broad arrows showing Pseudoarthrosis on right side; solid arrow
showing increased uptake of radio-isotope due to increased metabolic
activity/ inflammation.
Figure 3
Figure 3(B)
Concerns for Interventional Pain Management
It is important to remember that the functional L5 nerve root always originates from the “last mobile” segment of the spine. The last mobile segment of the spine is defined as the lowest level with a fully formed disc space, bilateral facet joints and two free transverse processes, which do not articulate with the ala of the sacrum or the pelvis. Therefore, in the case of a sacralized L5, the functional L5 nerve root corresponds to the anatomical L4 nerve root. In patients with a lumbardized S1, the last fully mobile level is usually L6-S2, and the functional L5 nerve root corresponds with the L6 nerve root [10]. In clinical presentation, the neurologic symptoms caused by the L6 nerve root compression resemble those of the L5 rather than the S1 nerve root compression in the normal configuration [11]. The alteration in nerve root innervation caused by a transitional vertebra may make it difficult to find the pain generator. Therefore, in patients receiving selective nerve root blocks, one should be aware of a transitional segment before initiating the injection [12]. The presence of an LSTV is associated with a higher incidence of a concomitant Thoracolumbar TV (TLTV) and vice versa.
Diagnosis of Pain Generators
It is often difficult to differentiate symptomatic and asymptomatic extra-foraminal stenosis secondary to osteophyte formation on conventional MRI alone. Either 3D MR lumbosacral radiculography or Selective radiculography in combination with CT is the most reliable modality to diagnose far-out entrapment of the L5 nerve root. This radiculography clearly demonstrates not only the degree of L5 nerve root impingement, but also the etiology of the L5 nerve root compression. Discography may be useful if the disc above the transitional vertebra is suspected for the source of the pain [13]. Bone scintigraphy may show increase uptake on bone scintigraphy secondary to degeneration and metabolic activity of the anomalous articulation (Figure 2). When increased uptake is seen on the upper1/2 to 1/3 part of the sacroiliac joint, this should not be mistaken for sacroiliac joint disease and degenerative LSTV articulations should especially be considered in the differential diagnosis. Diagnostic block of pseudo articulation can be given with small amount of local anaesthetic with or without steroid. If anesthetic block of the anomalous articulation does not provide pain relief, other associated causes of low back pain may be considered [14].
Treatment
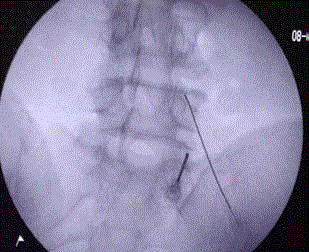
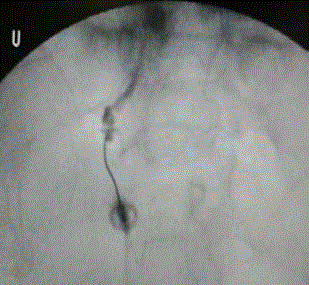
Injections of steroids or local anesthetics into the transverse process and sacral articulation (pseudo arthrosis) site can be both diagnostic and therapeutic. Long-term relief can be achieved by radiofrequency ablation by creating strip lesion at pseudoarthrosis area once local anaesthetic block has resulted in significant relief [15]. Other symptoms may need specific treatment depending on pathogenesis of the pain and radicular symptoms (Figure 3A and B). An algorithm (Figure 4) has been proposed to help in decision making in patients of back pain associated with LSTV. Surgical resection of Mega-apophysis is an option in selected patients however, results of surgical treatment are only slightly better than conservative treatment [16].
References
- Apazidis A, Ricart PA, Diefenbach CM, Spivak JM. The prevalence of transitional vertebrae in the lumbar spine. Spine J. 2011;11(9):858-62.
- Quinlan JF, Duke D, Eustace S. Bertolotti's syndrome. A cause of back pain in young people. J Bone Joint Surg Br. 2006;88(9):1183-6.
- Mahato NK. Facet dimensions, orientation, and symmetry at L5-S1 junction in lumbosacral transitional States. Spine (Phila Pa 1976). 2011;36(9):E569-73.
- Aihara T, Takahashi K, Ogasawara A, Itadera E, Ono Y, Moriya H. Intervertebral disc degeneration associated with lumbosacral transitional vertebrae: a clinical and anatomical study. J Bone Joint Surg Br. 2005;87(5):687-91.
- Connolly LP, d'Hemecourt PA, Connolly SA, Drubach LA, Micheli LJ, Treves ST. Skeletal scintigraphy of young patients with low-back pain and a lumbosacral transitional vertebra. J Nucl Med. 2003;44(6):909-14.
- Bertolotti M. Contributo alla conoscenza dei vizi di differenziazione regionale del rachide con special riguardo all assimilazione sacrale della v. lombare. Radiologiqu Medica. 1917(4):113-44.
- Paik NC, Lim CS, Jang HS. Numeric and morphological verification of lumbosacral segments in 8280 consecutive patients. Spine (Phila Pa 1976). 2013;38(10):E573-8.
- Luoma K, Vehmas T, Raininko R, Luukkonen R, Riihimäki H. Lumbosacral transitional vertebra: relation to disc degeneration and low back pain. Spine (Phila Pa 1976). 2004;29(2):200-5.
- Weber J, Ernestus RI. Transitional lumbosacral segment with unilateral transverse process anomaly (Castellvi type 2A) resulting in extraforaminal impingement of the spinal nerve: a pathoanatomical study of four specimens and report of two clinical cases. Neurosurg Rev. 2010;34(2):143-50.
- McCulloch JA, Waddell G. Variation of the lumbosacral myotomes with bony segmental anomalies. J Bone Joint Surg Br. 1980;62-B(4):475-80.
- Chang HS, Nakagawa H. Altered function of lumbar nerve roots in patients with transitional lumbosacral vertebrae. Spine. 2004;29(15):1632-5.
- Kim YH, Lee PB, Lee CJ, Lee SC, Kim YC, Huh J. Dermatome variation of lumbosacral nerve roots in patients with transitional lumbosacral vertebrae. Anesth Analg. 2008;106(4):1279-83.
- Ugokwe KT, Chen TL, Klineberg E, Steinmetz MP. Minimally invasive surgical treatment of Bertolotti's Syndrome: case report. Neurosurgery. 2008;62(5 Suppl 2):ONSE454-5.
- Almeida DB, Mattei TA, Sória MG, Prandini MN, Leal AG, Milano JB, et al. Transitional lumbosacral vertebrae and low back pain: diagnostic pitfalls and management of Bertolotti's syndrome. Arq Neuropsiquiatr. 2009;67(2A):268-72.
- Burnham R. Radiofrequency sensory ablation as a treatment for symptomatic unilateral lumbosacral junction pseudarticulation (Bertolotti's syndrome): a case report. Pain Med. 2010;11(6):853-5.
- Li Y, Lubelski D, Abdullah KG, Mroz TE, Steinmetz MP. Minimally invasive tubular resection of the anomalous transverse process in patients with Bertolotti's syndrome: presented at the 2013 Joint Spine Section Meeting: clinical article. J Neurosurg Spine. 2014;20(3):283-90.