Short Communication
Long Term Survival after Surgery for Ampullary Carcinoma: Case Report and Short Review of Literature
Maddibande Ramachar Sreevathsa*
Department of Surgery, M.S.Ramaiah Medical College Hospital, Bangalore 560054, India
*Corresponding author: Maddibande Ramachar Sreevathsa, Department of Surgery, M.S.Ramaiah Medical College Hospital, Bangalore 560054, India
Published: 09 Nov 2017
Cite this article as: Sreevathsa MR. Long Term Survival
after Surgery for Ampullary Carcinoma:
Case Report and Short Review of
Literature. Clin Surg. 2017; 2: 1723.
Abstract
Ampullary Carcinoma is a distinct type amongst the four subsites of Periampullary Carcinoma due
to its good biological behaviour. Ampullary Carcinoma arises within the Ampullary Complex and
is recognized sooner due to earlier presentation with obstructive jaundice. It contributes to 0.2%
of all gastro-intestinal malignancies. They have a better resection and survival rate compared to
pancreatic variety of Periampullary Carcinoma. Long term survival beyond 10 years, after curative
resection, has not been well described in the literature. We report a case of Ampullary Carcinoma
presenting initially with obstructive jaundice and surviving for 14 years despite recurrence of the
tumor. A short review of the literature is presented.
Keywords: Ampulla of vater; Ampullary carcinoma; Non pancreatic periampullary carcinoma;
Pancreatoduodenectomy
Abbreviations
FAC: 5 Fluorouracil, Adriamycin, Cyclophosphamide; CECT: Contrast Enhanced Computer Tomography; FNAC: Fine Needle Aspiration Cytology; TNM: Tumor, Node, Metastasis for Staging; ER: Estrogen Receptor; PR: Progesterone Receptor; HER 2 Neu: Herceptin 2 Neu; IHC: Immunohistochemistry
Material and Methods
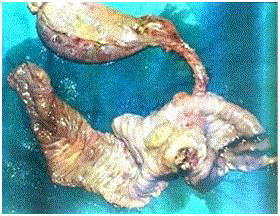
A 44 year old woman underwent pancreatoduodenectomy for obstructive jaundice due to Ampullary Carcinoma of Stage T2 N0 M0 in March 1995 (Figure 1). 8 Years Later (September 2003), the patient presented with pain in the right lumbar region when a hard, mobile, irregular parietal mass of size 7 cm × 5 cm was identified in the right lumbar region, near the old drainage tube scar. FNAC confirmed the nodule to be malignant. A CECT Abdomen was done which showed a big peritoneal nodule in the same area, infiltrating the oblique muscles, and indenting the right lobe of liver. One additional nodule was found in Morrison’s Pouch (Figure 2 and 3). On explorative laparotomy there were 3 peritoneal nodules. Of the two nodules described on CECT, one was infiltrating the parietes; adherent to inferior margin of Segment VI of the Liver, the other was located in Morrison’s Pouch. A third nodule was found in the Appendices Epiploicae of the right half of transverse colon and was adherent to the parietal mass. These 3 nodules were found along the track of the old drainage tube. Metastatectomy of the 3 nodules was done; the parietal nodule was excised with part of Segment VI of the Liver to yield a tumor free margin (Figure 4 and 5). Histopathological Examination of these nodules confirmed them to be a recurrence of Ampullary Adenocarcinoma. The specimen was not subjected to immuno-histochemistry. One year later, in October 2004, on a routine CT scan of the abdomen, recurrence of the tumor was found in the Segment VII of the Liver infiltrating the upper pole of the right kidney. The patient then underwent en block resection of Segment VII of the Liver and Right Kidney (Figure 6). Patient was well until 2009, when she presented with a lump in the right breast (Stage T2N0M0). A tru-cut needle biopsy confirmed the lump to be Infiltrating Duct Carcinoma which was ER-ve, PR-ve, HER2 neu -ve on IHC. Patient underwent Modified Radical Mastectomy (Figure 7). She succumbed to neutropenic fever after receiving a 3rd cycle of FAC regime of post operative chemotherapy.
Figure 1
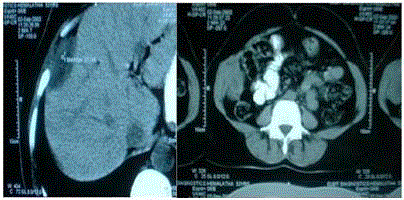
Figure 2
Figure 2
CECT showing peritoneal lesion indenting the right lobe of liver and
infiltrating oblique muscles.
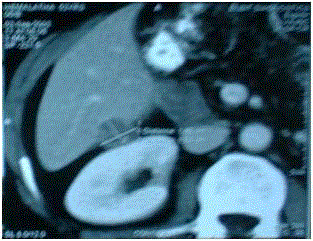
Figure 3
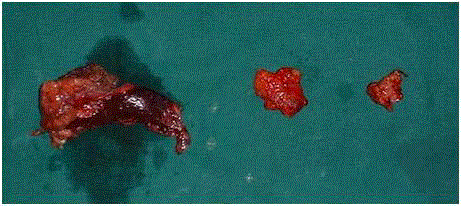
Figure 4
Figure 4
Specimens of Metastatectomy. The first specimen is the parietal
nodule with margin of liver.
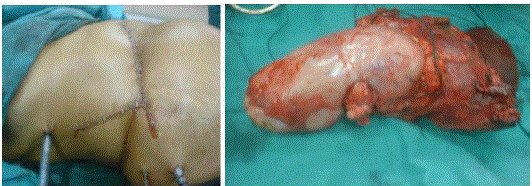
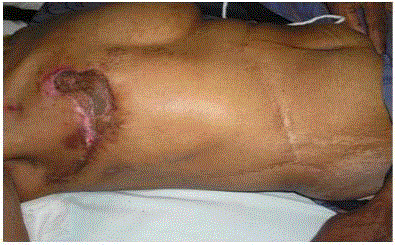
Figure 5
Figure 5 and 6
Showing incision and specimen for right en bloc resection of
Segment VI of Liver and Right Kidney.
Figure 7
Discussion
Peri-Ampullary Carcinoma can arise from 4 subsites within a 2 cm radius of the Ampulla of Vater. These subsites are the distal portion of Common Bile Duct, Duodenum, Ampullary Complex and the adjacent portion of Pancreas. Ampullary Carcinoma arises within the Ampullary Complex distal to the confluence of Distal Common Bile Duct and Pancreatic Duct [1]. Peri-Ampullary Carcinoma and Ampullary Carcinoma account for 5% and 0.2% of all gastrointestinal cancers, respectively. Two distinct varieties of Ampullary Cancer have been described histologically- Intestinal and Pancreatico- Biliary. Following curative resection, the Intestinal variety has a cure rate similar to the Duodenal type and Pancreatico- Biliary type, rather than to Pancreatic Cancer [2]. Ampullary Carcinoma has a higher resectability rate compared to the other subsites of Peri-Ampullary Carcinoma and Pancreatic Carcinoma. Its five year survival rate varies from 30% to 68% [1,2]. Similarly, there is increasing evidence that Non Pancreatic Peri-Ampullary Cancers have different, yet more favourable biological behaviour than their pancreatic counterparts. They are also more likely to be resected for cure [3]. A surgical outcome study showed a five year survival of 59.9% for the resected group of 78 patients having Ampullary Carcinoma. In this group, among those undergoing pancreatoduodenectomy, the presence of lymph node metastasis did not affect their overall survival. However, metastasis to 2 or more lymph nodes did influence the disease free survival [4]. Swh-Chin Chen, et al. [5] has reported the effect of lymph node metastasis on the prognosis of Ampullary Carcinoma undergoing curative resection. In 194 evaluable patients, they found that both the lymph node negative group and the patients with more than 14 lymph nodes harvested during pancreatoduodenectomy had 84.4% five year survival. On univariate analysis, the stage of the disease, nodal status, presence of perineural invasion, and grade of the tumor had a significant influence on survival. A multi-institutional retrospective study from Germany evaluated 143 Ampullary Carcinoma patients for prognostic factors influencing long term survival. They concluded that the long term survival of more than 10 years relied strongly on factors such as lymphatic tissue invasion, major vessel invasion, and lymph node status. They have reported a 10 year and 15 year survival of 24% and 10%, respectively. Ampullary Cancers behaved better than others arising in peri- ampullary subsites [6]. Shinkawa H, et al. [7] have reported on a retrospective review of 23 patients that 10 out of 11 patients with recurrent Ampullary Cancer died within 5 years after surgery. The risk factors for long term survival were pancreatic invasion and nodal metastasis. The 10 and 5 year survival was 48% and 43%, respectively. In conclusion, review of the literature suggests that the Non Pancreatic subtype of Ampullary Carcinoma has better chances of survival beyond 10 years.
References
- David P Ryan, Harvey Mamon, Carlos Fernandez- del Castillo. Ampullary Carcinoma: Treatment and Prognosis. 2017.
- Romiti A, Barucca V, Zullo A, Sarcina I, Di Rocco R, D'Antonio C, et al .Tumors of ampulla of vater:A case series and review of chemotherapy options. World J Gastrointest Oncol. 2012;4(3):60-7.
- Erdmann JI, Morak MJ, Duivenvoorden HJ, van Dekken H, Kazemier G, Kok NF, et al. Long term survival after resection for non pancreatic peri-ampullary carcinoma followed by adjuant intra-arterial chemotherapy and concomitant radiotherapy. HPB (Oxford). 2015;17(7):573-9.
- Choi SB, Kim WB, Song TJ, Suh SO, Kim YC, Choi SY. Surgical Outcomes and Prognostic factors for Ampulla of Vater Cancer. Scand J Surg. 2011;100(2):92-8.
- Swh-Chin Chen, Yi- Ming Shyr, Shu – Cheng Chou, Shin E- Wang. The role of lymph nodes in predicting the prognosis of ampullary carcinoma after curative resection. World J Surgical Oncology. 2015;13:224.
- Klein F, Jacob D, Bahra M, Pelzer U, Puhl G, Krannich A, et al. Prognostic factors for long term survival in patients with ampullary carcinoma. The results of 15 year observation period after pancreaticoduodenectomy. HPB Surg. 2014;2014:970234.
- Shin Kawa H, Takemura S, Kiyota S, Uenishi T, Kaneda K, Sakae M, et al. Long term outcome of surgical treatment for Ampullary Carcinoma. Hepatogastroenterology 2012;59(116):1010-2.