Short Communication
Pneumopathy during Pregnancy
Hugo Esteva1*, Alberto Marchevsky2 and Juan Antonio Mazzei1
1Department of Surgery, Universidad de Buenos Aires, Argentina
2Director Pulmonary and Mediastinal Pathology Cedars Sinai Medical Center University of California, USA
*Corresponding author: Hugo Esteva, Department of Surgery, Universidad de Buenos Aires, Argentina,
Published: 06 Nov, 2017
Cite this article as: Esteva H, Marchevsky A, Mazzei JA.
Pneumopathy during Pregnancy. Clin
Surg. 2017; 2: 1718.
Short Communication
A 31-years old female, with thrombogenic Leyden Factor V, who smoked 5 cigarettes/day from
15 to 25 years.
She started with right chest pain during the last three months of her first pregnancy delivering
a normal baby in December 2013.
Two weeks after, she began with cough and mucous sputum.
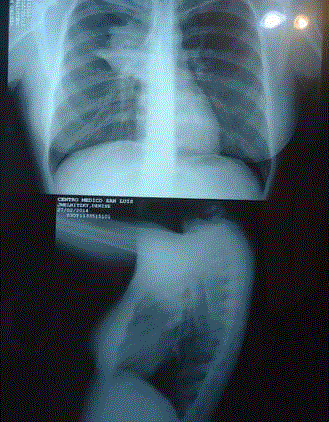
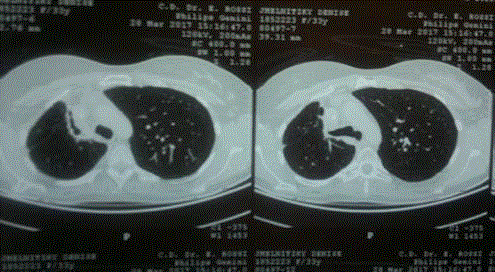
Chest X-rays and PET-CT showed a tumor like lesion with a cavity in the anterior segment of
Right Upper Lobe (Figure 1,2) and low metabolic activity in hilar adenopathies.
Bronchofiberscopy: No endobronchial lesions.
CT Fine Needle Biopsy: No neoplastic cells.
Chorionic Gonadotrophin and Alpha Fetoprotein were negative.
In June 2014 surgical exploration showed hard RUL tumor strongly attached to superior cava
vein. Atypical segmentectomy of Anterior Segment with good margins and sampling of group 4
adenopathy was performed. Intraoperative and delayed Pathology showed chronic inflammation
with acute suppurative areas.
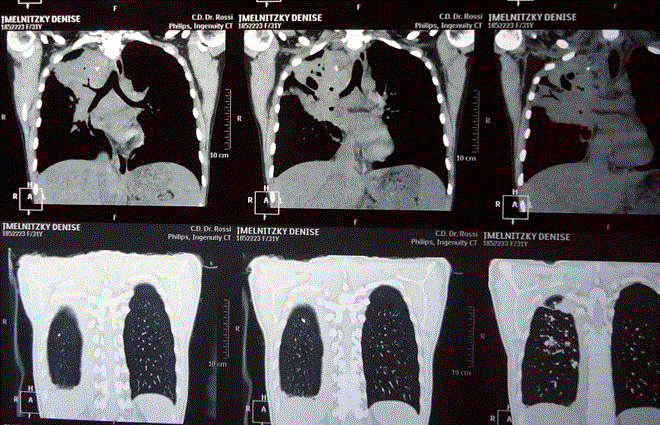
Prolonged antibiotic treatment depending on cultures was indicated without good result (Figure
3).
New bronchoscopy with transbronchial biopsies (TBB) showed non-specific inflammation.
Local and general evolution went torpidly worse, even though different antibiotic schemes were
instituted.
March 2015: Surgical re-exploration. Biopsies of small nodules in RLL and mediastinal pleura.
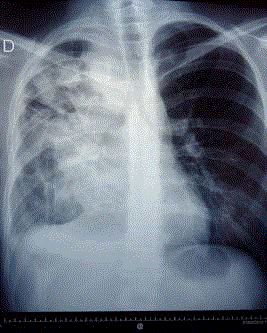
The wedge biopsy of a strongly consolidated Middle Lobe got into a suppurative cavity that was
drained through pneumonostomy (Figure 4).
The patient did better while the cavity slowly got closed and
drainage was thrown out.
Initially the pathological diagnosis didn’t change and an
international consultation was proposed. Material obtained through
both surgical operations and bronchoscopies was sent to the Pathology
Laboratory of the Cedars Sinai Medical Center in California.
No specific lesions were detected in all the previous samples, but
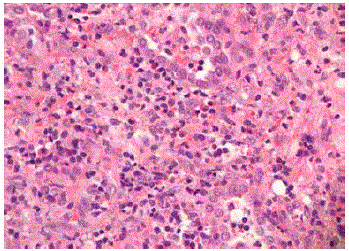
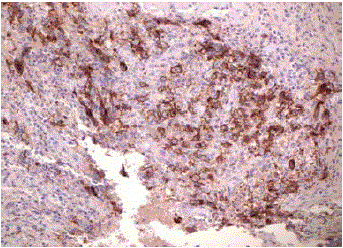
Right Middle Lobe wedge resection was described as: “Lung with
necrotizing pneumonia admixed with atypical lymphoid infiltrates
consistent with Hodgkin lymphoma classical type” (Figure 5, and 6).
The Comment by the Pathologist was as follows: “The case is very
difficult to classify as it shows extensive area of severe necrotizing
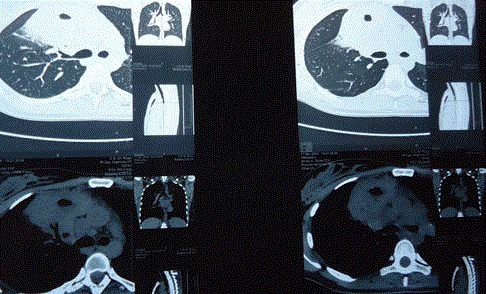
Figure 2: Initial CT scan shows a small cavity inside RUL lesion.
pneumonia. However, the right middle lobe wedge resection specimen
shows nodular areas with a relatively small number of large atypical
cells that exhibit an immunophenotype consistent with Hodgkin
lymphoma (CD30+, MUM+, CD20+, TARC +, PAX5 weakly +,
CD45 -). The case was evaluated by our hematopathologist”.
The patient started specific treatment with good tolerance.
She remains free from the illness more than two years after. Small
asymptomatic bronchiectasis remaining in RULobe (Figure 7).
Figure 1
Figure 2
Figure 3
Figure 4
Figure 5
Figure 6
Figure 7
Conclusion
Persistence and detailed work of surgeons and pathologists lead to life saving diagnosis and treatment in an unusually confusing case.