Case Report
Keloid on the Penis after Circumcision: A Rare Complication
Murat Sanal* and Bettina Haerter
Department of Pediatric Surgery, Innsbruck Medical University, VTT Clinic, Austria
*Corresponding author: Murat Sanal, Department of Pediatric Surgery, Innsbruck Medical University, VTT Clinic, Anichstr. 35, 6020 Innsbruck, Austria
Published: 02 Nov, 2017
Cite this article as: Sanal M, Haerter B. Keloid on the
Penis after Circumcision: A Rare
Complication. Clin Surg. 2017; 2: 1705.
Abstract
Keloids are defined as scars that extend beyond the borders of the original wound, do not regress spontaneously and tend to recur following excision. We report a 13-year-old boy presenting with a huge keloid formation on the penis after circumcision as a rare location for keloid formation and as a rare complication after circumcision. Therapeutic strategy consisted of surgical excision followed by intralesional corticosteroid injection and silicone gel sheet application. Keywords: Keloid; Circumcision; Penis
Introduction
Keloids are elevated fibrous scars that from following dermal injury. They are characterized
by fibroblastic proliferation and excessive collagen deposition. Many factors such as skin tension,
darker pigmented ethnicity and genetic predisposition are parameters which play a major role in
keloid development [1,2]. Patients typically present with aesthetic concerns, although keloids can
also cause pruritis, pain, pressure and functional complications [2].
Most commonly keloids arise on the sternum, shoulders and upper arms, earlobes and cheeks
[1,2] Keloid formation on the penis is a rare occurrence [3]. We describe the case of a 13 year/old
boy presenting with a huge keloid formation on the penis after circumcision and discuss the diverse
management strategies for keloids.
Case Presentation
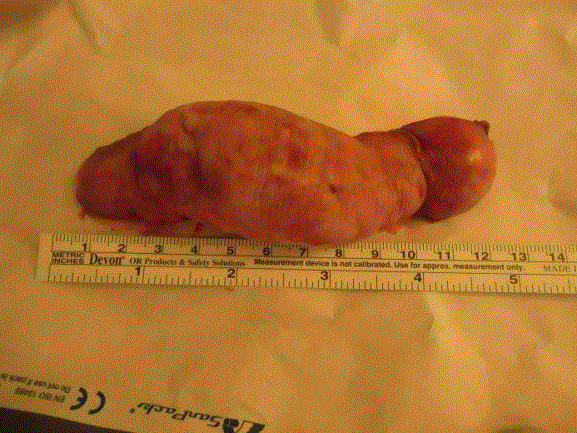
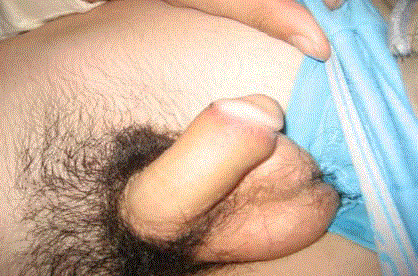
A 13-year-old boy presented with a huge keloid formation on the coronal sulcus of the penis,
measuring 2.5 cm breadthways and 3 cm thickness (Figure 1 and 2). He did not complain about
pain, burning or miction disorders, but about itching. The patient had undergone a circumcision
at the age of 11 years and since developed the swelling on the coronal sulcus. Anamnestic there was
no wound infection, no prolongated wound healing or skin tension. Neither the patient nor other
family members ever had a keloid formation before.
In an out-patient intervention a circular incision was carried out to the level of superficial fascia
intramarginally cranial and caudal in the keloid tissue. Before skin closure a corticosteroid (1 ml
triamcinolone acetonide 5 mg/ml) was injected with a 27 gauge needle into the upper dermis of
the wound edges. Skin closure was done by monofile caprosyn 5/0 interrupted sutures. Dressing
consisted of a dexpanthenol ointment and compresses. There was no intra- or postoperative
complications. Wound healing was uneventful and a silicone gel sheet was applied for 2 weeks. Two
years following excision there was no recurrences (Figure 3).
Figure 1
Figure 2
Figure3
Discussion
Circumcision is one of the oldest and most used surgical procedures. It is a relatively safe and
simple procedure, however even under ideal circumstances, does carry the risk of complications.
Often mentioned early complications are bleeding, inadequate skin removal and wound infection.
They tend to be minor and quite treatable. Other serious complications include iatrogenic
hypopadias, glanular necrosis and amputation [3,4]. Late complications include epidermal inclusion
cysts, suture sinus tracts, chordee, redundant foreskin, urethrocutaneous fistulae, meatitis and
meatus stenosis. Keloid development after circumcision is a very rare complication [3].
Keloid scarring is one of the most frustrating clinical problems in wound healing. Keloids
are scars that extend beyond the borders of the original wound, do not regress spontaneously
and tend to be notoriously recurrent following excision. They develop as a result of an abnormal excise the keloid tissue intramarginally in order not to stimulate additional collagen synthesis and surgical therapy should be
combined with adjuvant treatment such as pressure, topical silicone
gel sheeting, corticosteroids and radiotherapy. Radiation therapy is
contraindicated in children and not desirable for penile keloids due
to the close proximity of germ cells [1,2,6].
Intralesional corticosteroid injection decreases fibroblast
proliferation, collagen synthesis and suppresses pro-inflammatory
mediators. The most commonly used drug for steroid injection is
triamcinolone acetonide suspension at a dosis of 5 mg/ml to 10 mg/
ml, which is injected intralesionally [6].
Topical silicone gel sheeting is a noninvasive and extensively
studied approach to the prevention and treatment of keloids. The
mechanism of action is unknown, but it has been suggested that
silicone sheeting increasing the temperature, hydration and perhaps
the oxygen tension of the occluded scar, causing it to soften and
flatten as it affects local keratinocytes to alter growth factor secretion
and secondarily influences fibroblast regulation [2,6].
Compression therapy is not practicable on the penis. Hence for
our patient remained corticosteroid application and topical silicone
gel sheeting as adjunct to surgical excision.
Knowing that keloidal scarring is one of the most frustrating
clinical problems in wound healing as success rates in the management
of keloids are poor despite new approaches for the treatment we are
lucky that our patient is recurrence free 2 years after excision.
References
- Leventhal D, Furr M, Reiter D. Treatment of keloids and hypertrophic scars; a metaanalysis and review of the literature. Arch Facial Plast Surg. 2006; 8:362-8.
- Shehzad A Khan. Keloid-An Update. Physicians Academy. 2008;2(6):25-9.
- Erdemir F, Gokce O, Sanli O, Kadioglu A, Parlaktas BS, Uluocak N, et.al. A rare complication after circumcision: keloid of the penis. Int Urol Nephrol 2006;38(3-4):609-11.
- Brown D. Hypospadias. Postgrad Med J 1949;25:367-75.
- Krill AJ, Palmer LS, Palmer JS. Complications of circumcision. ScientificWourldJournal. 2011;11:2458-68.
- Shaffer JJ, Taylor SC, Cook Bolden F. Keloidal scars:a review with a critical look at therapeutic options. J Am Acad Dermatol. 2002;46:63-97.