Case Report
Primitive Squamous-Cell Carcinoma of the Pleura in a Patient Exposed to Asbestos
Andrea Campione1*, Fabrizio Giordano1, Andrea Bianchi2, Alberto Gorla3 and Alberto Terzi4
1Department of Pathology, Azienda Ospedaliera S.Croce e Carle, Cuneo, Italy
2Department of Nuclear Medicine, Azienda Ospedaliera S.Croce e Carle, Cuneo, Italy
3Department of Thoracic Surgery, Azienda Ospedaliera S.Croce e Carle, Cuneo, Italy
4Department of Thoracic Surgery, Ospedale Sacro Cuore Don Calabria, Verona, Italy
*Corresponding author: Andrea Campione, Department of Pathology, Azienda Ospedaliera S.Croce e Carle Cuneo Italy Via Coppino 26 12100 Cuneo, Italy
Published: 02 Nov, 2017
Cite this article as: Campione A, Giordano F, Bianchi A,
Gorla A, Terzi A. Primitive Squamous-
Cell Carcinoma of the Pleura in a
Patient Exposed to Asbestos. Clin Surg.
2017; 2: 1704.
Abstract
This report describes an unusual case of primary carcinoma of the pleura in a patient occupationally
exposed to asbestos. Clinical and radiological findings strongly supported a diagnosis of malignant
mesothelioma but incisional biopsy and definitive surgical excision showed the uncommon finding
of a primitive squamous-cell carcinoma of the pleura.
Keywords: Pleura; Carcinoma; Asbestos
Introduction
In medical literature there are few reports on primary pleural malignancy other than mesothelioma. In the present study an unusual case of cancer is described.
Case Presentation
A 65-year-old man was referred to our Hospital for recurrent pleural effusions. He had been
smoker and paper mill worker and his past medical or oncological history was negative.
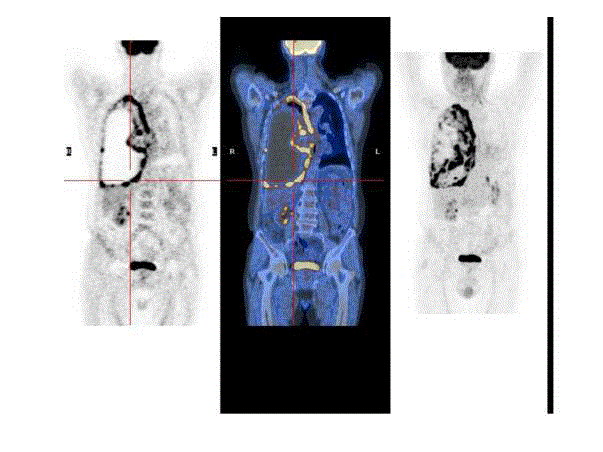
After admission he underwent total body computed tomography/positron emission tomography
scan (TC/PET) which showed radiographic features and uptake values consistent with pleural
involvement by malignant mesothelioma (Figure 1).
During thoracoscopy a serious effusion and pleural nodules were seen.M
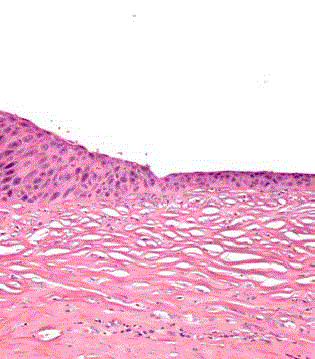
Histological examination of the pleural samples showed a large amount of squamous metaplasia
with verrucous appearance, and large amount of keratin with hyper and paracheratotic horns,
associated with area of dysplasia and areas of squamous keratinizing carcinoma (Figure 2).
Complete immunohistochemical panel of reaction was performed showing positive epithelial
markers (p63, CK7, CK CAM 5.2) and negative mesothelial marker (calretinin, WT1, vimentine).
A thorough work-up failed to detect any primary epidermoidal carcinoma and therefore a
diagnosis of primitive squamous-cell carcinoma of the pleura was made.
Grossly, after performing an extended pleuro-pneumonectomy with curative intent, parietal
pleura showed coalescence of white nodules to form plaques. Dense white tumour encased the
lung, involving visceral pleura and spreading into peripheral pulmonary parenchyma ab extrinseco
(Figure 3).
The remaining lung and bronchial tree was widely examined and failed to show any pathological
finding suggesting primitive pulmonary cancer, thus confirming our previous conclusion.
Three months after an eventless discharge the patient suffered from a late bronchopleural fistula
which finally led to progressive sepsis and decease.
Figure 1
Figure 2
Figure3
Discussion
Microscopically, the tumour consisted of diffuse infiltration of the sub-serous tissue by
squamous keratinizing carcinoma at first suggesting pleural involvement by distant metastasis.
Only the definitive clinical work-up and the absence of other primitive malignancy supported
our diagnosis of squamous-cell carcinoma of the pleura.
Related reports illustrate pleural carcinoma arising in patient
with chronic empyema [3], bronchopleural fistula [4] or following
pneumonectomy for tuberculosis [5], hydatid disease [6] or lung
carcinoma [7].
In these cases authors [6] also hypothesized that chronic
inflammation led to neoplastic transformation through metaplastic
pleura [8].
As far as we know this could be one of the very rare cases of
primitive squamous carcinoma of the pleura unrelated to known
chronic inflammation or previous surgery, unless long-lasting
asbestos exposure could be the only etiopathogenetic factor leading
to asymptomatic persistent inflammation.
References
- Bruce T, Dahlstrom G, Uggla LG. Squamous epithelial cancer of the pleura following extrapleural pneumothorax for pulmonary tuberculosis. Acta Tuberc Scand. 1960;38:261-6.
- Sapino A, Cavallo A, Donna A, Bussolati G. Pleural epidermoid carcinoma from displaced skin following extrapleural pneumothorax in a patient exposed to asbestos. Virchows Arch. 1996;429(2-3):173-6.
- Rüttner JR, Heinzl S. Squamous-cell carcinoma of the pleura. Thorax. 1977;32(4):497-500.
- Prabhakar G, Mitchell IM, Guha T, Norton R. Squamous cell carcinoma of the pleura following bronchopleural fistula. Thorax 1989;44(12):1053-4.
- Rena O, Casadio C, Maggi G. Primitive squamous-cell carcinoma after extrapleural pneumothorax for active tuberculosis. Eur J Cardiothorac Surg. 2001;19(1):92-5.
- Zapatero Gaviria J, Garcia Franco CE, Jimenez Hiscock L, Peñalver Pascual R, Fogué Calvo L, Muguruza Trueba I, et al. Carcinoma arising in the pleural cavity following pneumonectomy for hydatid disease. Respiration. 2004;71(3):285-8.
- Franke M, Chung HD, Johnson FE. Squamous cell carcinoma arising from the pleura after pneumonectomy for squamous cell carcinoma of the lung. Am J Surg. 2010;199(4):e34-5.
- Willén R, Bruce T, Dahlström G, Dubiel WT. squamous epithelial cancer in metaplastic pleura following extrapleural pneumothorax for pulmonary tuberculosis. Virchows Arch A Pathol Anat Histol. 1976;370(3):225-31.