Case Report
Antibiotics versus Appendectomy for Acute Appendicitis: A Randomized Trial
Rupsha Nura Laila1, Md Abdul Momen1, Md Anayet Ullah2, Md Habibullah Sarkar1 and M Mizanur
Rahman3*
1Department of Surgery, Rajshahi Medical College Hospital, Rajshahi, Bangladesh
2Department of Community Medicine, Barindo Medical College, Rajshahi, Bangladesh
3Department of Surgical Oncology, National Institute of Cancer Research and Hospital, Mohakhali, Dhaka
*Corresponding author: M Mizanur Rahman, Department of Surgical Oncology, National Institute of Cancer Research and Hospital, Mohakhali, Dhaka, Bangladesh
Published: 03 Aug, 2017
Cite this article as: Laila RN, Md Abdul Momen, Md Anayet
Ullah, Md Habibullah Sarkar, Rahman
MM. Antibiotics versus Appendectomy
for Acute Appendicitis: A Randomized
Trial. Clin Surg. 2017; 2: 1659.
Abstract
Background: Although appendectomy is the standard treatment of Acute Appendicitis (AA), we
tried to determine the role of antibiotics in the management of AA and to justify if appendectomy
still remains the gold standard of care.
Methods: Randomly selected two hundred consecutive suspected AA patients, screened by Modified
Alvarado Score, allocated equally in study group (with antibiotics) and control (appendectomy)
group. All Pre-, per- and post-treatment clinical information’s collected and recorded in a predesigned
data collection sheet and Telephone (or email) follow-ups conducted at 15 days, 1 month,
6 months, and 12 months.
Results: Antibiotics were efficacious in 67% of cases, 9 needed urgent appendectomy and 24 relapse
cases at 12 months follow-up. Early postoperative complications was 25% in appendectomy group
and during follow up 5% present with sub-acute intestinal obstruction.
Conclusion:
Recurrent appendicitis and risk of missing serious pathology is potential drawback,
but good patient selection can help overcome this and Use of antibiotics for the treatment of acute
appendicitis could be a good option for treatment.
Keywords: Acute appendicitis; Antibiotic treatment; Recurrent appendicitis; Follow up;
Appendectomy; Efficacy; Complications
Introduction
Acute appendicitis still ranks as one of the most common acute surgical emergencies, which
was described and systematically studied in the mid-19th century. Appendectomy has been the
mainstay for the treatment for acute appendicitis since it was first reported by McBurney in 1889.
Since then, many studies, articles and even books have been written upon this subject and it seems
that nothing new can be added and still an ongoing debate. The role of antibiotic treatment in
acute uncomplicated appendicitis may have been overlooked mainly on the basis of tradition rather
than evidence, considering that other intra-abdominal inflammatory processes such as colonic
diverticulitis, salphingitis, neonatal enterocolitis etc. are primarily managed non-operatively.
The incidence of acute appendicitis is lowest in societies with a high dietary fiber intake, but in
developing countries that are adopting a more refined western-type diet; the incidence continues
to rise. There has been a dramatic reduction in the incidence of appendicitis in Western countries
over the last three decades. Is there a relationship between falling incidence and increased use of
antibiotics?
Traditionally, appendectomy has been the primary treatment, even in cases of unconfirmed
diagnosis, given the low incidence of major complications. However, in 15% – 30% of cases the
appendix is found to be free of disease upon resection [1,2]. As appendectomy is associated with
surgical wound infection, intestinal obstruction due to adhesions, pneumonia, and tubal infertility
in females, the possibility of using conservative treatment merits investigation. In this study we tried
to find benefit using antibiotic in acute appendicitis and made a comparison with appendectomy
cases.
Material and Methods
Study population
Patients (>14 years old) presented with suspected AA screened
carefully by attending surgeons in Rajshahi Medical College Hospital,
Rajshahi, Bangladesh from January 2013 to December 2014 was
enrolled in this study. Clinical history, physical examination and
laboratory blood tests (blood hemoglobin g/l and leukocyte count
E9/l, Neutrophil count) as well as urine analysis, X-ray K.U.B region
and U.S.G of lower abdomen was undertaken as per need. Finally by
using Modified Alvarado Score total 200 Patients who were eligible
for inclusion in the randomized control study invited to participate
and informed about the protocol. Acute appendicitis patients with
diffuse peritonitis, antibiotic (ciprofloxacin) documented allergy,
Positive pregnancy test and irritable bowel disease IBD were excluded
from study. After signed informed consent obtained, 100 patients
were included in appendectomy group and 100 patients in antibiotic
group. There is no formal ethical committee in the institute we tried
to maintain all ethics of research of international standard.
Registration procedure
After signed informed consent, all patients evaluated for study
enrollment are registered in participating institution using predesigned
data collection sheet.
Randomization
After confirming the diagnosis of uncomplicated AA by Modified
Alvarado Score, patients were randomized by number of patient. 1st
patient was allocated to antibiotics (study group), and 2nd patient to
appendectomy (control group). Thus uneven no. patients remain
under antibiotic therapy and even no. patients got operative treatment.
The randomization was performed in 1:1 equal allocation ratio. To
randomize a patient, an independent surgeon on duty worked.
Interventions
Surgical treatment: After randomization to undergo operative
treatment, open appendectomy was performed by standard technique
using a McBurney right lower quadrant muscle splitting incision.
Prophylactic antibiotic as a single dose of 400 mg i.g ciprofloxacin and
500 mg metronidazole i.v. was administered approximately 30 min
preoperatively. The histopathological examination of the appendix
performed and the histological diagnosis of acute appendicitis
requires involvement of the muscularis of the appendix (transmural
neutophil invasion).
Antibiotic therapy
After randomization to receive antibiotic treatment, intravenous
ciprofloxacin 400 mg 12 hourly with Metronidazole 500 mg 8 hourly
administered for three days. The clinical status of the antibiotic
group patients re-evaluated within 12-24 hours after admission and
monitored during the whole stay. If progressive infection, perforated
appendicitis or peritonitis is clinically suspected, the patient
underwent emergency appendectomy and the histopathological
examination of the appendix performed. The three-day intravenous
antibiotic treatment was followed by seven days of oral antibiotic
therapy with Cipofloxacin 500 mg × 2 combined with metronidatzole
400 mg × 3 resulting in ten-day total duration of the antibiotic
therapy.
Operational analysis
The primary end-point
The primary endpoint of treatment success in this trial is
defined as treatment efficacy in the antibiotic treatment group as
the resolution of AA with antibiotic treatment resulting in discharge
from the hospital without the need for surgical intervention and no
recurrent appendicitis during a minimum follow-up of one-year.
Treatment efficacy in the operative treatment arm is defined as
successful appendectomy evaluated to be 100%.
Secondary end-points
• Post-intervention complications
• Late recurrence of AA after conservative treatment
• Duration of hospital stay
• Sick leave
A recurrent AA will be diagnosed on a clinical basis. A patient
with recurrent AA could receive 2nd time antibiotic therapy or
appendectomy as per need and the recurrent AA diagnosis would
be verified histopathological examination of removed appendix. For
the primary study endpoint, the overall treatment efficacy will favor
surgical treatment. For the secondary end-points, late recurrence
of AA after one-year follow-up is naturally associated only with the
antibiotic treatment arm. The outcome regarding the other secondary
endpoints of overall morbidity, sick leave, treatment costs, pain
scores and pain medication utilization in the antibiotic treatment
arm is evaluated to be superior compared with surgical treatment.
The duration of the hospital stay was most likely be similar in both
treatment arms.
Follow-up
Patients outcome obtained during hospital stay (days 0,1,2) and
then by a phone interview at two week, one month, six month and at
one year after the intervention. During follow up additional need for
sick leave, wound infections and recurrent AA, an incisional hernia
with the McBurney incision for the surgery group was registered.
Potential adhesion related problems such as sub acute intestinal
obstruction evaluated for both groups.
Statistical analysis
Pre study estimates suggested that at least 200 allocated patients
would be necessary to confirm a 10-15 per cent difference in treatment
efficacy and complications between study and control patients at 80
per cent power with a 5 per cent significance level. The χ2 test was
used to check for differences between proportions. Student's t test or
ANOVA was used for comparisons of continuous variables between
groups. P < 0.050 was considered significant in two-tailed tests. SPSS®
version 16.0 software was used for the statistical calculations.
Figure 1
Figure 2
Figure 3
Figure 4
Figure 5
Results
Study population
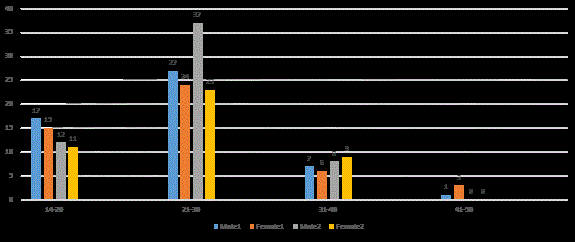
The total study population (200) consisted of 91 female and 109
male with age ranged from 14 to 45 years. A peak incidence of acute
appendicitis was found in patients 14–30 years of age in both age
groups. The mean age in appendectomy group and primarily treated
antibiotic group was respectively 25.06 years and 24.63 years, on the
other hand female: male ratio 1:1.3 and 1: 1.08 respectively (Figure 1).
Per operative finding of resected appendix
In appendectomy group, per operatively 69 appendixes was
inflamed with fibrinous exudates and faecolith was found in only 3
appendixes. 2 perforated appendixes with faecolith in lumen were
found and 4 gangrenous appendixes were found. But 25 appendixes were apparently looking normal. Those patients who underwent
appendectomy after failure of antibiotic therapy, preoperatively 4
appendixes were highly inflamed and 5 was gangrenous appendix.
During follow up period two (2) patients underwent appendectomy
due to recurrent appendicitis.
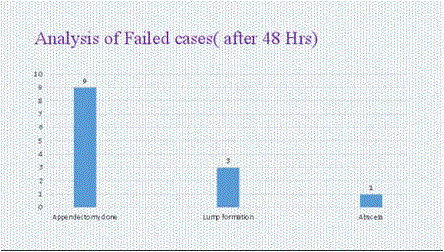
Complications during hospital stay
In Antibiotic group thirteen (13) patients developed complications
nine (9) underwent appendectomy during antibiotic therapy, three
(3) patients develop appendicular lump, one (1) patient suffered from
appendix abscess. Twenty five (25) patients developed complications
after primary appendectomy treatment which is described in Table 2.
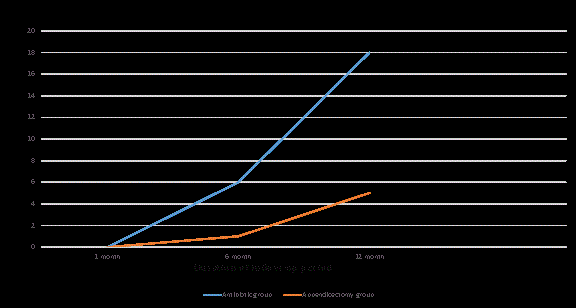
Complications during follow-up period
This study design resulted 100 antibiotic treated patients, with a
primary recovery rate of 91% ( 91 in 100) and a 12 months recurrence
rate of 24% (Figure 2-5). In appendectomy group during follow
up five (5) patients later present with recurrent subacute intestinal
obstruction and improved by conservative treatment. Among these 5
patients 4 were with normal appendix according to histopathological
report.
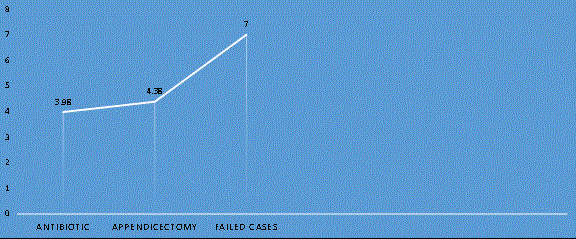
Duration of hospital stay
Mean duration of hospital stay in conservative group was 3.97
days while in operative group was 4.24 days. Those who underwent
appendectomy during antibiotic treatment stay in hospital for a
median of 7 days (Figure 2). So according to t-test and ANOVA test
there is significant difference in duration of hospital stay between
appendectomy group and those who underwent appendectomy due
to development of localized peritonitis after antibiotic therapy (Table
1 and 2) but Post Hoc test shows no significant difference in between
groups.
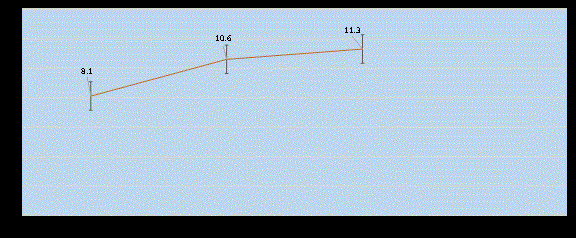
Return to normal activity
Those improve by antibiotic therapy (91 patients) return to
normal activity within mean duration of 8.1648 days. Mean duration
of return to normal activity was respectively 10.8367 and 11.333 in
appendectomy group (100 patients) and appendectomy done after
failure of antibiotic group (9 patients).
Incidence rates of negative appendectomy
There was highest percentage of negative appendectomy was
found in the second and third decade and mostly among female (8).
Discussion
Main findings
In this RCT according to definition of operational analysis
treatment efficacy in antibiotic group was 67% and in appendectomy
group it is 100%. But rate of complication in appendectomy group
(30%) was comparable to failure of antibiotic therapy (33%). Rate of
negative appendectomy in appendectomy group and antibiotic group
was respectively 12% and 1%.
Strengths and limitations
This RCT was under direct supervision of few competent
surgeons, so less chance of diagnostic dilemma and no chance of
delay to take operative decision if antibiotic treatment failed. In the
meantime follow up was ensured by using mobile reminder system.
There are several important limitations. The number of population in
this RCT was small and during subsequent follow up complications
were noted from verbal interview of the patients. Only in few cases,
patients could submit hospital document of their complications.
Comparison with previous study
The first prospective randomized controlled pilot study
comparing antibiotic treatment with appendectomy was published
in 19951 with 40 adult patients and promising results. Only one of
twenty patients (5%) who received antibiotic therapy did not recover
on this treatment (iv cefotaxime 2 g x 2 and tinidazole 800 mg x 1 for
2 days followed by oral ofloxacin 200 mg x 2 and tinidazole 500 mg x
2 for 8 days) and required surgery. Seven patients (37%) experienced
recurrent appendicitis within one year. The authors concluded that
antibiotic therapy was as effective as surgery, but with high recurrence
rate.
A decade later another prospective multicenter randomized
controlled trial was presented by Styrud et al. [2] 252 male patients
between 18-50 years old with clinically assumed appendicitis, CRP
>10mg/l and without suspicion of perforation were included. The
antibiotic recovery rate was 88% and the recurrence rate within
one year was 14%. This was compared with a complication rate of
14% in the surgery group. The antibiotic regimen was the same as in the pilot study from 1995 unpublished data, presented at a surgical
symposium 2007, and showed a recurrence rate of 24% after 5-year
follow-up [3]. During the completion of this study, antibiotic
treatment of acute appendicitis has become in focus [4-7] and several
other studies, meta-analyses and systematic reviews on the subject
have been published. The RCTs have had similar antibiotic recovery
rates around 90% and similar 1-year recurrence rates around 10%-
15% (with some exceptions) [1,2,8,9].The conclusions of the metaanalyses
and systematic reviews have been inconsistent and have
varied from stating that antibiotics may be used only for selected
patients with uncomplicated appendicitis with appendectomy
remaining the gold standard [10-12] to a much more positive
attitude towards antibiotic therapy incurring fewer complications
compared to surgery [13-15]. Acute appendicitis successfully
treated by antibiotics still remains a potential source of recurrent
appendicitis. On the other hand, post-operative wound infections
and post appendectomy bowel obstruction, even after 30 years from
appendectomy, have been described. Any abdominal operation can
result in adhesions, which may cause intestinal obstruction later in
life. But Negative appendectomy appears at least as dangerous as
perforated appendicitis concerning both small bowel obstruction
and mortality [16]. Overall complication rate after appendectomy is
hard to specify because definitions and reporting of complications are
inconsistent, but a complication rate of 10% - 20% in large randomized
trials has been shown [17-19]. In this study during follow up in
control group five (5) patients later present with recurrent subacute
intestinal obstruction and improved by conservative treatment.
Among these 5 patients 4 were with normal appendix according to
histopathological report. Our RCT showed a recurrence rate of 24%
and 22 of those patients ask to be treated conservatively a second time
and two needed appendectomy. The incidence of perforation was not
found among patients with recurrence, and it may be that antibiotic
treatment could have been used second time. First-year recurrence
rate of AA successful treated by antibiotic ranges between 10 and 15%.
So our RCT result is comparable with other RCT. Higher percentages
have been reported in the previous study of Eriksson and in a recent prospective study by Vons et al. [9] (36.8% and 26% respectively). Due
to the rate of recurrence, according to the Ansaloni meta-analysis,
the clinical effectiveness favors surgery. Surgery can treat acute
appendicitis in 100% of cases with the mortality and morbidity rate
already described. Recurrence of appendicitis after appendectomy is
quite impossible. The diagnosis of acute appendicitis is often difficult
to make and remains largely a clinical one. Diagnostic uncertainty
may lead to a delay in treatment or negative surgical exploration, both
adding to the morbidity associated with this condition. The exact
mechanisms leading to AA are still obscure but enteric bacteria (both
aerobic and anaerobic bacteria) probably play a more important role.
Whereas obstruction plays of minor importance, although it could be
one of the contributing factors for perforation. If infection were the
prevailing etiology of acute appendicitis, it would be logical to treat it
with antibiotics rather than appendectomy. Thus, antibiotics offer the
opportunity to treat AA even when surgical resources are not easily
available such as in developing countries. There are several different
types of antibiotics, and combinations of antibiotics, that can be used
in the treatment of appendicitis. Considering the treatment cost and
efficacy metronidazole and ciprofloxacin may be the best option
given the coverage of aerobic gram-positive and gram-negative
bacteria. So we have chosen this regimen of antibiotic in our study.
We did not analyse the hospital costs in between two groups but
significant difference in hospital costs was reported by Hansson et al.
[20] with a reduction in expenses of 25-50% in the antibiotic group
compared to surgery. The antibiotic approach offers the opportunity
to avoid aboard Soviet ships treated at sea. In the latter Gurin et
al. [21] by reviewing the conservative treatment outcomes in 252
patients with AA on vessels of the Kalingrad fishing industry from
1975 to 1987, reported a recovery rate of 84.1% with the only use of
antibiotics. Thus, antibiotics offer the opportunity to treat AA even
when surgical resources are not easily available such as in developing
countries. Now question arise what is the best option? Probably there
is no right answer to this dilemma.. Eight meta-analyses and reviews,
including a Cochrane report, of the RCTs comparing antibiotics
with surgery have been published during recent years [15,22,23],
but the conclusions in these summaries have not been unanimous.
Some authors stated that antibiotics might be safely used in selected
patients with uncomplicated appendicitis leading to overall reduced
complication rate, but the reports emphasized that appendectomy
should remain the gold standard treatment. Others pointed out that
antibiotic treatment incur fewer and less severe complications than
surgery and could be regarded an alternative treatment in a majority
of patients when such patients are willing to accept a risk of either
initial treatment failure or later recurrence. The American College
of Surgeons, [24] the Society for Surgery of the Alimentary Tract,
[25] and the World Society of Emergency Surgery [26] all describe appendectomy (either laparoscopic or open) as the treatment of
choice for appendicitis. Regarding an antibiotics-first strategy, the
American College of Surgeons patient information guide indicates
that it “may be effective, but there is a higher chance of re occurrence
[26]; the Society for Surgery of the Alimentary Tract patient care
guidelines suggest that it is “not a widely accepted treatment” [27]; and
the World Society of Emergency Surgery states that “this conservative
approach features high rates of recurrence and is therefore inferior
to the traditional appendectomy. Non-operative antibiotic treatment
may be used as an alternative treatment for specific patients for whom
surgery is contraindicated”.
However, experience in Europe suggests that an antibiotics-first
strategy is an alternative that warrants consideration, particularly
in a patient who has had prior surgical complications and has a
strong preference for avoiding appendectomy. European have also
shown that as many as half the patients so treated will have early
treatment failures, and all have a risk of recurrent appendicitis that
may ultimately require appendectomy [27]. It is recommended that
although appendectomy remains the recommended treatment for
appendicitis, clinicians should inform appropriate patients about
the evidence related to an antibiotics-first strategy, as well as the
uncertainties.
However, the question whether primary antibiotic treatment of
acute appendicitis is inferior, equal or superior to appendectomy
is highly debated, although we believe they should be regarded
complementary.
Table 1
Table 2
Conclusion
Appendectomy can be universally considered a “mile stone” in modern medicine. The comparison of surgery and antibiotic therapy is still an ongoing debate. Should we compare the rate of early failure in the antibiotic therapy with the rate of white appendicitis? Or should we compare the recurrence rate of antibiotic treated appendicitis within 30-days and long-time morbidity of surgery? In order to reduce the rate of “white appendicitis” and misdiagnosis there is the need to improve the diagnostic power. Therefore, we suggest adopting at least a single institutional clinical diagnostic tool and algorithm. The comparison of antibiotic and surgery needs a homogenous and more objective patient selection and guidelines. Some advantages and some disadvantages are intrinsic in both the treatment choice and cannot be compared. On the other hand, outpatient antibiotic treatment cannot be proposed as a clinical standard practice. High risk patients should be treated by antibiotics whilst surgery is to be considered mandatory after conservative treatment failure.
References
- Eriksson S, Granström L. Randomized controlled trial of appendicectomy versus antibiotic therapy for acute appendicitis. Br J Surg. 1995;82(2):166-1669.
- Styrud J, Eriksson S, Nilsson I, Ahlberg G, Haapaniemi S, Neovius G, et al. Appendectomy versus antibiotic treatment in acute appendicitis. A prospective multicenter randomized controlled trial. World J Surg. 2006;30(6):1033-7.
- Styrud J, Eriksson S, Nilsson I, Haapaniemi S, Neovius G, Rex L, et al. Femårs uppföljning av randomiserad kontrollerad studie mellan appendektomi contra antibiotikabehandling vid icke perforerad appendicit. Kirurgveckan Stockholm. 2007.
- Liu K, Ahanchi S, Pisaneschi M, Lin I, Walter R. Can acute appendicitis be treated by antibiotics alone? Am Surg. 2007;73(11):1161-5.
- Mason RJ. Surgery for appendicitis: is it necessary? Surg Infect (Larchmt). 2008;9(4):481-8.
- Vons C. Can acute appendicitis be treated by antibiotics and in what conditions? J Chir (Paris). 2009;146(1):17-21.
- Gronroos JM. Clinical suspicion of acute appendicitis - is the time ripe for more conservative treatment? Minim Invasive Ther Allied Technol. 2011;20(1):42-5.
- Malik AA, Bari SU. Conservative management of acute appendicitis. J Gastrointest Surg. 2009;13:966-70.
- Vons C, Barry C, Maitre S, Pautrat K, Leconte M, Costaglioli B, et al. Amoxicillin plus clavulanic acid versus appendicectomy for treatment of acute uncomplicated appendicitis: an open-label, non-inferiority, randomised controlled trial. Lancet. 2011;377(9777):1573-9.
- Fitzmaurice GJ, McWilliams B, Hurreiz H, Epanomeritakis E. Antibiotics versus appendectomy in the management of acute appendicitis: a review of the current evidence. Can J Surg. 2011;54(5):307-14.
- Varadhan KK, Humes DJ, Neal KR, Lobo DN. Antibiotic therapy versus appendectomy for acute appendicitis: a meta-analysis. World J Surg. 2009;34(2):199-209.
- Ansaloni L, Catena F, Coccolini F, Ercolani G, Gazzotti F, Pasqualini E, et al. Surgery versus conservative antibiotic treatment in acute appendicitis: a systematic review and meta-analysis of randomized controlled trials. Dig Surg. 2011;28:210-21.
- Liu K, Fogg L. Use of antibiotics alone for treatment of uncomplicated acute appendicitis: A systematic review and meta-analysis. Surgery 2011;150(4):673-83.
- Sakorafas G, Mastoraki A, Lappas C, Sampanis D, Danias N, Smyrniotis V. Conservative treatment of acute appendicitis: heresy or an effective and acceptable alternative to surgery? Eur J Gastroenterol Hepatol. 2011;23(2):121-7.
- Varadhan K, Neal K, Lobo D. Safety and efficacy of antibiotics compared with appendicectomy for treatment of uncomplicated acute appendicitis: meta-analysis of randomised controlled trials. BMJ. 2012;344:e2156.
- Tingstedt B, Johansson J, Nehez L, Andersson R. Late abdominal complaints after appendectomy--readmissions during long-term follow-up. Dig Surg. 2004;21(1):23-7.
- Ortega AE, Hunter JG, Peters JH, Swanstrom LL, Schirmer B. A prospective, randomized comparison of laparoscopic appendectomy with open appendectomy. Laparoscopic Appendectomy Study Group. Am J Surg. 1995;169(2):208-12.
- Hansen JB, Smithers BM, Schache D, Wall DR, Miller BJ, Menzies BL. Laparoscopic versus open appendectomy: prospective randomized trial. World J Surg. 1996;20(1):17-20.
- Moberg AC, Berndsen F, Palmquist I, Petersson U, Resch T, Montgomery A. Randomized clinical trial of laparoscopic versus open appendicectomy for confirmed appendicitis. Br J Surg. 2005;92(3):298-304.
- Hansson J, Korner U, Khorram-Manesh A, Solberg A, Lundholm K. Randomized clinical trial of antibiotic therapy versus appendicectomy as primary treatment of acute appendicitis in unselected patients. Br J Surg. 2009;96(6):473-81.
- Gurin NN, Slobodchuk Iu S, Gavrilov Iu F. The efficacy of the conservative treatment of patients with acute appendicitis on board ships at sea. Vestn Khir Im I I Grek. 1992;148(5):144-50.
- Wilms IM, de Hoog DE, de Visser DC, Janzing HM. Appendectomy versus antibiotic treatment for acute appendicitis. Cochrane Database Syst Rev. 2011;11:CD008359.
- Mason R, Moazzez A, Sohn H, Katkhouda N. Meta-Analysis of Randomized Trials Comparing Antibiotic Therapy with Appendectomy for Acute Uncomplicated (No Abscess or Phlegmon) Appendicitis. Surg Inf. 2012;13(2):74-84.
- American College of Surgeons. Operation Brochures for Patients. 2014.
- Society for Surgery of the Alimentary Tract. SSAT patient care guidelines: appendicitis.
- Sartelli M, Viale P, Catena F, Luca A, Moore E, Mark M, et al. 2013 WSES guidelines for management of intra-abdominal infections. World J Emerg Surg. 2013;8:3.
- Flum DR. Acute Appendicitis Appendectomy or the “Antibiotics First” Strategy. N Engl J Med. 2015;372:1937-43.