Case Report
Salvage Arthrodesis of the Knee with a Vascularized Fibular Graft
Stefanie C.M. van den Heuvel1*, Fientje J.C. van der Veen1, Timothy U. Jiya2 and Henri A.H.
Winters1
1Department of Plastic, Reconstructive and Hand Surgery, VU University Medical Center, Netherlands
2Department of Orthopedics Surgery, VU University Medical Center, Netherlands
*Corresponding author: Stefanie C.M. van den Heuvel, Department of Plastic, Reconstructive and Hand Surgery
Published: 18 Sep, 2017
Cite this article as: van den Heuvel SCM, van der Veen
FJC, Jiya TU, Winters HAH. Salvage
Arthrodesis of the Knee with a
Vascularized Fibular Graft. Clin Surg.
2017; 2: 1610.
Abstract
van den Heuvel SCM, van der Veen FJC, Jiya TU, Winters HAH. Salvage Arthrodesis of the Knee with a Vascularized Fibular Graft. Clin Surg. 2017; 2: 1610.
Introduction
Large skeletal defects around the knee joint may be caused by a traumatic compound fracture,
a tumor resection, or osteomyelitis, failed arthroplasty or failed arthrodesis. Various reconstructive
techniques, including endoprosthesis, allograft, vascularized or non-vascularized autograft, or a
combination of these techniques, have been described as treatment of large skeletal defects around
the knee [1,2,3].
Previously, the fibula has been used specifically for knee arthrodesis as an ipsilateral pedicled
graft [4-6,2], or as a free transplant from either extremity in a single [2,5,7-9] or a double-strut
fashion [10,3]. The use of a vascularized fibular graft that is rotated on its peroneal artery pedicle is
technically demanding.
We present four illustrative case histories of patients with a pedicled fibular graft for a salvage
arthrodesis of the knee. Refinements of the surgical technique that expand graft size and graft
mobility are described.
Methods
Surgical technique
Pre-operative assessment: Vascular imaging is required to determine if the peroneal artery is
expendable. In our patients, we used duplex imaging, as it is simple, efficient and does not expose
the patient to radiation.
Approach: A lateral approach is used, with the dissection carried between the posterior and
lateral compartments of the leg. The fibula is exposed by extraperiosteal dissection. First the peroneal
muscle is separated from the anterior aspect of the fibula down to the anterior intramuscular septum,
which is also dissected off the fibula. Further elevation of the anterior compartment muscles,
including the anterior tibial artery and the deep peroneal nerve, reveals the interosseous membrane.
Proximal and distal osteotomy: The distal osteotomy is placed 8 cm to 10 cm proximal to the
ankle to preserve the ankle stability. Normally, the fibular head is preserved to maintain the lateral
stability of the knee. In these cases, this is no longer needed because an arthrodesis is performed. So,
to obtain the maximal length of the graft, the fibula head is taken with the graft after dissecting and
protecting the peroneal nerve.
After ligation of the peroneal artery and vein at the distal osteotomy site, the posterior tibial
muscle is separated from the fibula, leaving the flexor hallucis longus muscle and the peroneal artery
and vein attached to the bone.
Transfer of the free fibular graft: The flexor halluces longus muscle is transsected at the distal osteotomy site and the fibula is passed deep to the peroneal muscle and anterior muscle compartment, along the interosseous membrane
and is rotated upward lateral to the tibia. The fibula is inserted into
the medullary canal of both the distal femur and proximal tibia. The
space between the distal femur and proximal tibia is supplemented
with cancelleous bone.
A uniplanar orthofix dynamic axial fixator was used to stabilize
the arthrodesis. This was found suitable as it permits early cyclic
movement and subsequent progressive loading thus enhancing union
of the opposing ends of de distal femur and proximal tibia as well as
incorporation of the vascularized fibula. Fixation was achieved with
6 bi-cortical screws (3 proximal and 3 distal, inserted on each side
and when feasible, well away from the endpoints of the fibula graft)
upon which the body of the dynamic axial fixator was assembled and
mounted under adequate compression. Subsequent dynamization at
3-6 weeks enhanced healing. However, it is important to note that
rotational stability may be an important drawback of the uniplanar
orthofix dynamic axial fixator and as such the authors recommend
that the use of a multiplanar fixator, particularly in the early healing
phase, be considered.
Postoperative care: Partial weight bearing is allowed after 3 to 6
weeks, thereafter healing is checked by radiographs.
Figure 1
Figure 2
Figure 3
Figure 4
Case Presentation
Case 1
A 24-year-old male sustained multiple trauma including an intra
articular fracture of the left knee following a road traffic accident. The
most feasible option was an arthrodesis of his left knee. Eighteen years
later a re-arthrodesis was performed because of malalignment. Nine
years later a total knee arthroplasty (MRH Stryker®) was performed
with reconstruction of the extensor mechanism complicated by skin
necrosis and a prosthetic joint infection (PJI). A debridement with
antibiotics, irrigation and retention (DAIR) of the knee prosthesis
was performed whilst a medial and lateral gastrocnemius flap was
used to facilitate wound closure. Due to persistent PJI, the prosthesis
was extracted and an arthrodesis was performed with the aid of an
external fixator. At that time it was quite clear that fusion is highly
unlikely due to severe bone loss. A staged pseudoarthrosis repair
was planned upon adequate antbiotic treatment of the underlying
infection. After four months a pseudarthrosis repair was performed
with a pedicled ipsilateral fibular graft. The flexor hallucis longus
muscle and a skin paddle were taken with the graft to cover the large
soft tissue defect. The reconstruction was stabilized by an external
fixator. Partial weight bearing started 6 weeks after surgery.
Six weeks after the operation a superficial pin tract infection
occurred, which resolved after 4 months when the external fixator
was removed. The fibular graft fractured two weeks after removing
the external fixator and the leg was stabilized with an above-the-knee
cast. After one year a second pseudoarthrosis repair was performed
using a fusion nail. Five months after the operation radiographs
showed complete fusion of the fracture and full weight bearing was allowed.
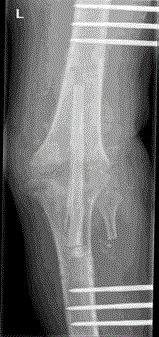
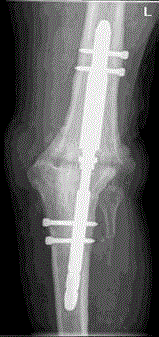
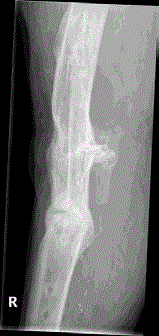
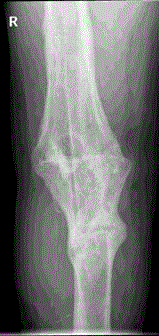
Picture 1-2. Directly post-operative.
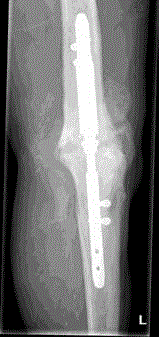
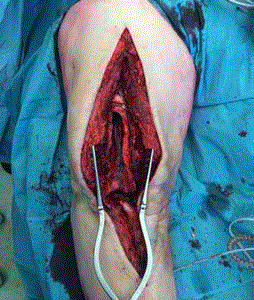
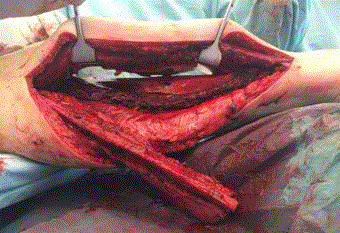
Picture 3-4. Four years post-operative.
Case 2
A 60-year-old patient with a prosthetic joint infection of his right
knee underwent a two-stage revision after a failed DAIR procedure.
Six years later a VY quadriceps-plasty and an osteotomy of the tibial
tuberosity was performed because of limited range of motion. This
was complicated by another infection. A second two-stage revision
was performed but failed due to recurrent infection. Due to massive
bone loss, an arthrodesis of the knee with an ipsilateral vascularized
fibular graft was performed. The reconstruction was stabilized by
an external fixator. Partial weight bearing started after 6 weeks and
full weight bearing was allowed after 12 weeks. Five months later
the patient fell and sustained a traumatic fracture at the junction
of the fibular graft with the tibia. This resulted in a pseudarthrosis,
which united after external fixation and application of autogeneous
cancelleous bone graft from the illiac crest.
Picture 5-6. Directly post-operative
Picture 7-8. Two years post-operative.
Case 3
A 73-year-old man with osteoarthritis of the right knee underwent
a total knee arthroplasty. He had previously suffered several episodes
of erysipelas infections of both legs and also a septic arthritis of the
right knee. Fourteen months after surgery a hematogenic infection of
the prosthesis occurred and the prosthesis was extracted followed by
appropriate antibiotic treatment. Because of the recurrent episodes
of erysipelas infections a revision arthroplasty was not performed.
Instead an arthrodesis was performed using a vascularized fibular
bone graft. The reconstruction was stabilized by an external fixator.
Partial weight bearing started three weeks after surgery and full weight bearing at 3 months.
Three months after the operation a superficial pin tract infection
occurred that resolved after removal of the external fixator and oral
antibiotics. The leg was stabilized with an above- the- knee cast for an
additional 6 weeks.
Five months after the operation radiographs showed complete
fusion.
Case 4
A 49-year-old man received a total knee arthroplasty due to
symptomatic osteoarthristis of the right knee. Two years later, after
several recurrent infections, the prosthesis was extracted. Because
of the recurrent infections revision arthroplasty was not performed
directly. After one year patient received a re-implantation of his
prosthesis. Due to infections the prosthesis was removed and in a
single session, patient received a hinged prosthesis. One year later,
this hinged prosthesis was removed due to another infection, and
replaced by an external fixator in order to stabilize the joint for healing.
We attempted an arthrodesis of the knee using an arthrodesis rod;
however, the patient developed a pseudoarthrosis. In a last attempt
to salvage the function of the leg, we perfromed a re-arthrodesis of
the right knee using an ipsilateral vascularized fibular graft. This was
eleven years after initial operation. Partial weight bearing started
6 weeks after surgery and full weight bearing at 6 months. Last
outpatient clinic visit two years later, radiographs showed complete
fusion and full weight bearing is possible.
Figure 5
Figure 6
Figure 7
Figure 8
Figure 9
Figure 10
Discussion
Large bone defects involving the knee joint can be reconstructed
by prosthetic replacement, allograft with joint cartilage, rotation
plasty or arthrodesis by allograft or autogenous bone graft.
Reconstruction with a tumour or hinged knee prosthesis, or
an articulating allograft provides a painless and stable knee with
an adequate range of motion. However the extensor mechanism
needs to be intact and there is an increased risk of infection and/or
implant loosening. Arthrodesis aided with allografts are susceptible
to infection, non-union and stress fractures, which may not unite
[11,12].
The vascularized fibular graft has many advantages such as high
union rate, early union, possibility of graft hypertrophy, early healing
after fracture, higher resistance against infection when compared
with other types of reconstruction, and possibility of simultaneously
reconstruction of bone and skin defect (osteocutaneous composite
graft) [13-17]. Also the number of further revision procedures
required after use of a vascularized fibula as a salvage procedure is
much less than with other modalities of reconstruction.
The case histories of these patients do illustrate that a pedicled
vascularized fibula is a good option in knee arthrodesis and sometimes
the only alternative to amputation.
Several studies have reported modifications of this technique
[8,6,2,18]. These studies reported mostly very satisfactory results with
this technique, when an ipsilateral pedicled fibula is used according
to our technique, dissection of recipient vessels and performance of
microvascular anastomoses is not needed. Despite the satisfactory
results obtained with this technique, most authors also describe
Figure 9: Case 4 Intra Post Operative.
Figure 10: Case 4 Intra Post Operative.
some shortcomings of this technique. The most common problem
is the limited range, due to the typical short peroneal vascular
pedicle. Raising the fibula flap/graft extended as distal as possible
will lengthen the pedicle and optimize the reach. In some cases a free
fibula graft will allow more flexibility to the orthopaedic surgeon who
can position the fibula exactly as desired. If, for instance, the femoral
defect is too large, the pedicled fibula will not reach high enough, and
a free fibula graft is called for.
On the basis of our case studies, we recommend some technical
modifications when using a pedicled fibular graft for knee arthodesis.
A modification we use to lengthen the graft is to include the
fibular head with the graft. Usually the proximal 4-6 cm of the
fibula (including the fibular head) should be retained to preserve
knee stability. In arthrodesis there is no need for co-lateral ligament
stability, so the fibular head can be included in the graft, aiding
adequate length in larger defects, especially on the tibial side.
The second and most important modification is the routing of
the flap/graft transfer. Instead of going around the outside of the
knee, we use the plane of the interosseous membrane to transfer the
fibula to its new position. This means we have to dissect the anterior
compartment from both the tibia and fibula. The fibula is then rotated
180 degrees upward in the plane of the interosseous membrane.
Obviously, the proximal origin of the anterolateral muscles is left
intact. This includes the anterior tibial artery and the peroneal nerve.
In this way, function of the anterolateral muscles is preserved. The
pedicle of the fibula flap now follows an almost straight line from its
origin to its destination, allowing for maximal reach.
When the fibula, including the fibular head is no longer in its
original position, the reach of the lateral gastrocnemius muscle is
greatly enhanced, aiding it’s mobilization for the treatment of possible
anterior defects in the knee region. This is an additional advantage.
Stabilization of the arthrodesis is of paramount importance.
As mentioned earlier, the authors recommend that the use of a
multiplanar fixator, particularly in the early healing phase, be
considered. Although aided by adequate trauma, suboptimal
rotational stability may have contributed to the fracture sustained in
case II of our series. Furthermore, no rotational failure was seen in
any of our case series, however the number of patients is far too small
to draw any conclusions in this regard.
Conclusion
We believe that an ipsilateral pedicled fibula flap/graft is a good solution for salvage arthrodesis of the knee. The suggested modifications contribute to better use of this technique.
References
- Saika KC, Bhuyan SK, Saikia SP, Rongphar R, Jitesh. Resection and arthrodesis of the knee joint for giant cell tumours of bone. J Orthop Surg (Hong Kong). 2010;18(2):208-14.
- Geoffrey GH. The role of pedicled or free fibular grafts in knee arthrodesis. Ann Plast Surg. 1997;39(1):60-3.
- Amr SM, El-Mofty AO, Amin SN, Morsy AM, El-Malt OM, Abdel-Aal HA. Reconstruction after resection of tumours around the knee: role of the free vascularized fibular graft. Microsurgery 2000;20(5):233-51.
- Malizos KN, Zalavras CG, Soucacos PN, Beris AE, Urbaniak JR. Free vascularized fibular grafts for reconstruction of skeletal defects. J Am Acad Orthop Surg. 2004;12(5):360-9.
- San-Julian M, Canadell J. Fractures of allografts used in limb preserving operations. Int Orthop. 1998;22(1):32-6.
- Serafin D. The fibula flap. In: Serafin D, editor. Atlas of microsurgical composite tissue transplantation. Philadelphia: WB Saunders. 1996;547-66.
- Wada T, Naito T, Usui M, Tsuchida Y, Kanaya K, Tsuji H. Free vascularized fibular grafts for reconstruction of large femoral defects involving the knee joint: report of two cases. J Reconstr Microsurg. 1998;14(3):205-29.
- Masamichi Usui, Ishii S, Naito T, Wada T, Nagoya A, Takahashi T, et al. Arthrodesis of knee joint by vascularized fibular graft. Microsurgery. 1996;17(1):2-8.
- Han CS, Wood MB, Bishop AT, Cooney WP. Vascularized bone transfer. J Bone Joint Surg. 1992;74(10):1441-9.
- Hsu RWW, Wood MB, Sim FH, Chao EYS. Free vascularized fibular grafting for reconstruction after tumour resection. J Bone Joint Surg. 1997;79-B:36-42.
- O’Brien BM, Gumley GJ, Dooley BJ, Pribaz JJ. Plast Reconstruc Surg. 1988; 82(2):311-8.
- Ortiz-Cruz E, Gebhardt MC, Jennings LC, Springfield DS, Mankin HJ. The results of transplantation of intercalary allografts after resection of tumours. A long-term follow-up study. J Bone Joint Surg Am.1997;79(1):97-106.
- Ellingsen DE, Rand JA. Intramedullary arthrodesis of the knee after failed total knee arthroplasty. J Bone Joint Surg Am. 1994;76(6):870-7.
- Enneking WF, Shirley PD. Resection-arthrodesis for malignant and potentially malignant lesions about the knee using an intramedullary rod and local bone grafts. J Bone Joint Surg Am. 1977;59(2):223-36.
- Rasmussen RM, Bishop AT, Wood MB. Arthrodesis of the knee with a vascularized fibular rotatory graft. J Bone Joint Surg Am. 1995;77(5):751-59.
- Wada T, Usui M, Nagoya S, Isu K, Yamawaki S, Ishii S. Resection arthrodesis of the knee with a vascularised fibular graft. J Bone Joint Surg Br. 2000;82(4):489-93.
- Nouri H, Meherzi MH, Jenzeri M, Daghfous M, Hdidane R, Zehi K, et al. Knee arthrodesis using a vascularised fibular rotatory graft after tumor resection. Orthop Traumatol Surg Res. 2010; 96(1):57-63.