Case Report
Free Radial Forearm Flap Failure due to Un- Autonomization in a 105-Year Old Patient
Yusuf Kenan Coban1*, Kaan Bekircan1, Ozcan Ocuk1, Orhan Gazi Dinc1 and Nese Karadag2
1Department of Plastic Reconstructive and Aesthetic Surgery, Inonu University Medical Faculty Malatya, Turkey
2Department of Pathology, Inonu University Medical Faculty Malatya, Turkey
*Corresponding author: Yusuf Kenan Coban, Department of Plastic Reconstructive and Aesthetic Surgery, Inonu University Medical Faculty Malatya, Turkey
Published: 05 Sep, 2017
Cite this article as: Coban YK, Bekircan K, Ocuk O, Dinc
OG, Karadag N. Free Radial Forearm
Flap Failure due to Un-Autonomization
in a 105-Year Old Patient. Clin Surg.
2017; 2: 1608.
Abstract
Age itself should not be considered a contraindication to serve as the technique of choice to treat complex reconstructive challengers in older patients. Octogenarian is defined being older than 80 years or more. General surgery practice shows a mortality rate of 5 percent for octogenarians. This is more for those older than 90 years. Older patients are less capable of handling longer water electrolyte imbalances. Renal blood flow drops 50 percent from young adulthood to the age of 80 years.
Introduction
In search for related medical literature, there are several case series of elderly patients who had free flap surgery [1-3]. In those series, age range varies between 70 and 95 years. Upper age that withstands with the difficulties of microsurgical tissue transfer is important for showing the capabilities of human body. This report briefly aims to show an experience of free flap transfer in a 105 year-old female patient.
Case Presentation
The patient was diagnosed as squamous cell ca of the lower lip 5 years earlier and had 5
operations which included wedge lip excision and repairs with local tissues. The end result was
wound dehiscence with exposing bare mandibular symphysis with granulation tissue. Xerosis of
the tongue, poor nutritional status and lack of competence oral functions were noted. As local flap
options had already been used, a free radial forearm flap repair was planned taking the risk of ASA
IV (older age, diminished organ functions, poor nutrition etc).
Under general anesthesia, a radial forearm flap harvested from the right upper extremity
was transferred to the mandibular defect by anastomosing radial artery to right facial artery
with concomitant vein to facial vein. She was administered heparin IV treatment for three weeks
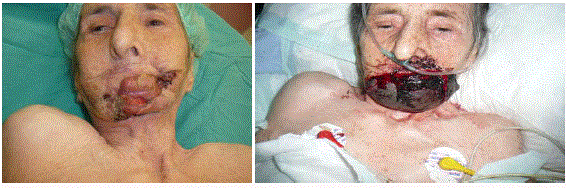
postoperatively. The flap was good in place until the 10th post-op day. A sudden enlarging cyanosis
covered the whole flap with bleeding every side of it (Figure 1). A hand Doppler examination showed
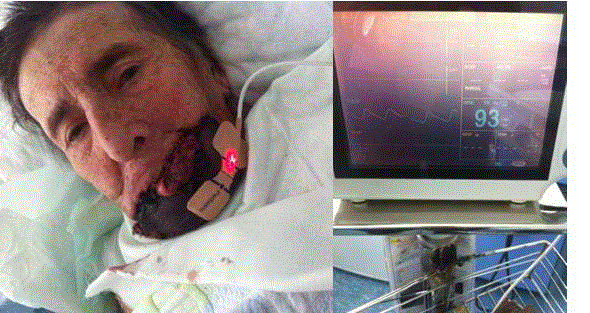
the radial artery was patent beneath the flap. A further examination with pulse -oxymeter was made
at post-op 18th day. It proved that there was 93% of oxygen saturation on the screen (Figure 2). At
that time, a skin biopsy was taken from the flap for histopathologic examination. Hematoxylin eosin
staining with x40 and x100 magnification showed an ischemic necrosis without any inflammation
of dermis and sub-dermal fat layer. Clinically the prominent abnormally with the biochemical data
were low albumin, low fibrinogen and low total protein (Figure 3). Human albumin infusion was
given at the second postoperative week in order to correct low albumin level. Peripheral parenteral
solutions were also administered during the whole postoperative period. D-dimer level was also
elevated, as a result of anticoagulant therapy presence (D-dimer; 418 mg/dl). This was a reflection
of fragmentation of fibrin network consisting D-dimers by plasmin in the blood. A fibrin layer
forms within the first 2 days and this would be one of the most important steps for gaining a good
revascularisation process.
Figure 1
Figure 2
Figure3
Figure 3
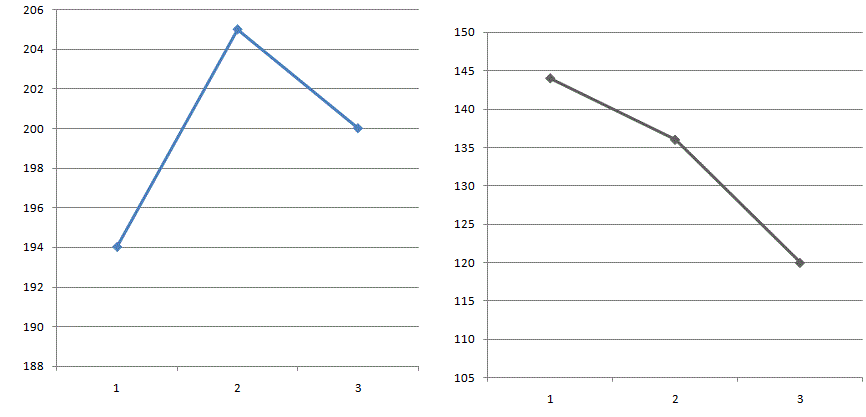
The graphics show the course of the levels of total rpotein, albümin, fibrinogen and platelet counts during the follow-up period. A) albümin and total
protein as g/dl B) fibrinogen as mg/dl and platelet counts (1st, 2nd, and 3rd blood samplings were done at 1st, 10th and 18th postop days).
Discussion
A general consensus that flap survival is possible, when thrombosis or pedicle ligation occurred
after postoperative day 12 is present. This minimal critical period of time may even be as low as 6
days for arterial and 9 days for pedicle and 4 days for venous compromise [5]. According to a recent
review, most of thromboses occur within the first two postoperative days. Some of them are related to heparin induced thrombocytopenia and thrombosis (HITT) and
it is associated with drop in platelet count seen 4-10 days following
heparin treatment [6]. We exclude this option, as the platelet count
had not dropped below any critical level during the follow-up period.
Establishment of functional revascularization is essential for the
successful healing of cutaneous wounds. Angiogenesis, the formation
of new blood vessels from an existing vascular bed, is a normal
physiological process. It is an integral factor in determining the
success or failure in Plastic and Reconstructive Surgery [7]. Critical
time period required for independent neovascularsation to allow flap
survival is not known. Most authors conclude that salvage surgical
intervention for flaps presenting with delayed vascular compromise
after fourth postoperative day are unsuccessful.
Free flap autonomisation can be defined as a certain time after
which neovascularisation or angiogenesis from recipient bed of free
flap transfer has become sufficient enough to allow its survival without
revision [8]. In ischemic flaps after resuming reperfusion, it was
shown that inflammatory cells infiltrate the reperfusion tissue which
can be detected within flap by biopsies taken at 7th day experimentally
[9]. It can be said that a free tissue transfer to a non-vascularised
environment carry a risk of flap failure due to major pedicle loss,
even in the long term. Histologic neovascularisation evidence has
been demonstrated in animal studies [10]. In surviving flaps, the
reduced blood flow gradually increases in a favorable recipient
site. Early neovascularisation starts at 4 days in the pig and rabbit
models [11]. Even the presence of ischemic cells within flap, there
must be inflammatory cells scattered around the necrotic areas on
histopathologic examination. We have found very low inflammatory
cell in the skin biopsy. We speculate that there was a reduced skin
perfusion during the early post-surgery days and this discrete skin
perfusion should be clinically present in the dermal layer of the flap,
while there was active bleeding beneath the flap. A hypothesis would
be that atrophic skin of a very elderly person did not permitted a
clear skin perfusion via skin perforators of radial forearm flap. In
other words, the perfusion was limited only deep fascial layer of the fasciocutaneous flap. A second hit by low fibrinogen level may have
not propagated a physiologic angiogenesis from the poor recipient
bed. All these events sequence ended up with total flap failure.
Conclusion
Free flap failure in the very old patient was resulted from the
following factors;
• Poor recent bed and vascularisation
• Low fibrinogen level
• Reduced skin perfusion
• Reduced inflammatory response
References
- Ozkan O, Ozgentas HE, Islamoglu K, Boztug N, Bigat Z, Dikici MB. Experiences with microsurgical tissue transfers in elderly patients. Microsurgery. 2005;25(5):390-5.
- Perrot P, Le Floch R, Bellier-Waast F, Bourdais L, Pannier M, Duteille F. [Free-flap reconstruction in the elderly patient]. Ann Chir Plast Esthet. 2008;53(5):420-3.
- Furnas H, Canales F, Lineaweaver W, Buncke GM, Alpert BS, Buncke HJ. Microsurgical tissue transfer in patients more than 70 years of age. Ann Plast Surg. 1991;26(2):133-9.
- Carmeliet P. Angiogenesis in health and disease. Nat Med. 2003;9(6):653-60.
- Granzow J, Li AI, Caton A, Boyd JB. Free Flap Survival Following Failure of the Vascular Pedicle. Ann Plast Surg. 2015;75(1):44-8.
- Tessler O, Vorstenbosch J, Jones D, Lalonde S, Zadeh T. Heparin-induced thrombocytopenia and thrombosis as an under-diagnosed cause of flap failure in heparin-naive patients: a case report and systematic review of the literature. Microsurgery. 2014;34(2):157-63.
- Akhavani MA, Sivakumar B, Paleolog EM, Kang N. Angiogenesis and Plastic Surgery. J Plast Recontr and Aesth Surg. 2008:61(12);1425-37.
- Yoon AP, Jones NF. Critical time for neovascularisation/angiogenesis to allow free flap survival after delayed postoperative anastomotic compromise without surgical intervention: A review of the literature. Microsurgery. 2016;36(7):604-12.
- Coban YK, Ciralik H. The effects of increased ischemic times on adipose tissue: a histopathologic study using the epigastric flap model in rats. Aesthetic Plast Surg. 2007;31(5):570-3.
- Mücke T, Borgmann A, Wagenpfeil S, Günzinger R, Nöbauer C, Lange R, et al. Autonomization of epigastric flaps in rats. Microsurgery. 2011;31(6):472-8.
- Tsur H, Daniller A, Strauch B. Neovascularization of skin flaps: route and timing. Plast Reconstr Surg. 1980;66(1):85-90.