Case Report
Fibroepithelial Polyp Presenting as a Large Vulvar Mass
Usha Verma* and Lydia A. Fein
Department of Obstetrics and Gynecology, University of Miami/Miller School of Medicine, USA
*Corresponding author: Usha Verma, Department of Obstetrics and Gynecology, University of Miami/ Miller School of Medicine, USA
Published: 29 Aug, 2017
Cite this article as: Verma U, Fein LA. Fibroepithelial Polyp
Presenting as a Large Vulvar Mass.
Clin Surg. 2017; 2: 1605.
Clinical Image
A 51-year-old P3043 woman presented to the emergency room with complaint of large mass
hanging from her right labia. Patient reported to be homeless and was a poor historian. She reported
that the mass was painless, but causing her constant discomfort and that it interfered with sitting
and walking. She was not able to recollect the duration of the mass but did note that it had been
steadily growing and was now associated with afoul smelling discharge. She also reported subjective
fevers, decreased appetite and weight loss. Her past medical history was significant for Hepatitis
C and a motor vehicle accident that required hospitalization in remote past. Surgical history was
significant for two cesareans sections and right leg abscess incision and drainage. She reported
illegal use of drugs.
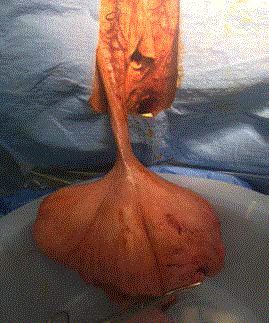
Her vitals were stable on presentation. On exam a pedunculated mass was noted arising from
the right labia majora. The stalk measured 5 cm × 2 cm and a large venous plexus was noted in the
stalk. The mass measured 20 cm × 11 cm × 8 cm (Figure 1). The inferior aspect of the mass was
ulcerated and foul smelling discharge tinged with blood was noted coming from the ulcerated area.
Her white blood cell count was 15.7/mm3 and Hemoglobin 12.3 G/dl. Sexually transmitted infection
screening was positive only for Hepatitis C, which she endorsed on admission.
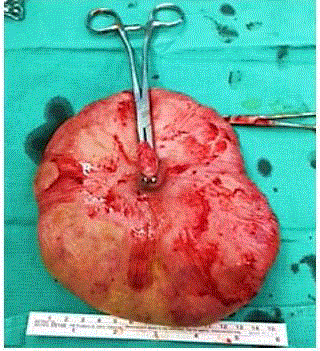
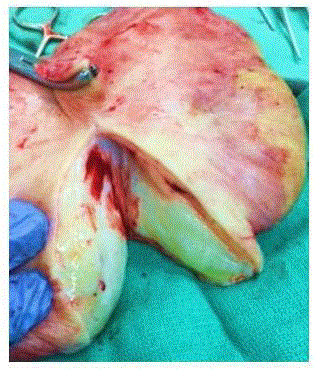
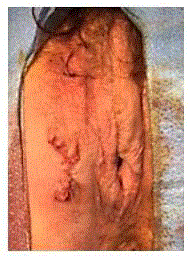
Surgical resection of the vulvar mass was performed under general anesthesia without
complication (Figures 2-4). Surgical pathology revealed fibroepithelial stromal polyp (FEP) without
a typical features. Resection margins were negative for neoplastic cells. Overall histologic findings
were consistent with fibroepithelial polyp with marked edema. However due to unusual size and
some histological resemblance to a neoplastic lesion (angiomyxoma), close clinical monitoring was
recommended by pathology.
Comments
Here we describe a rare case of FEP arising from the vulva. Moreover the size of this FEP in
our case is impressive. Fibroepithelial polyps commonly occur in the vagina. Typically, FEPs are
less than five centimeters [1]. To our knowledge, only one other case of a FEP measuring this large
has been reported (20 cm) [2]. Others have reported FEPs over 15-18 cm [3,4]. The pathogenesis
of FEPs is not clear. The presence of estrogen and progesterone receptor-positive FEP stromal cells
and their more common occurrence in reproductive-aged women and in pregnancy-followed by
regression after delivery-suggest that these growths are hormonally driven [1].
FEPs arise from mesenchymal tissue and must be distinguished from other vulvovaginal
mesenchymal lesions to achieve an accurate diagnosis by clinical presentation and histopathologic
features. The lesion described in this report is consistent with the typical presentation of FEPS, polypoid
and exophytic with large, thick-walled vessels located at the core of the lesion. On immunohistologic
staining, they are typically Desminpositive, as was reported here [5]. Histologically, stellate and
multinucleate stromal cells are present with varying degrees of cellularity, nuclear pleomorphism,
and mitotic activity. For this reason, it can be difficult to exclude malignancy [1,6]. FEPs bear
most resemblance to angiomyxomas, which are also most likely to appear in reproductive-aged
women. Aggressive (deep) angiomyxomas tend to be deeper, poorly circumscribed, and have
minimal cellularity on histology. Like FEPs, they can grow quite large and are also Desmin positive.
However, a distinguishing feature may be HGMA2 positivity on IHC. HGMA2 protein is expressed
in aggressive angiomyxomas but not in FEPs [7]. Superficial angiomyxomas may also be on the
differential for FEPs. They tend to be polypoid, well-demarcated, with spindle and stellate-shaped
stromal cells, but they differ from FEPs in that they stain negative for Desmin on IHC and have
smaller, thin-walled vessels. Acute inflammatory cells throughout the tumor can also be identified
in these tumors. Unlike deep angiomyxomas, they do not involve deeper tissues and do not stain
positive for HGMA2.
Figure 1
Figure 2
Figure3
Figure 4
References
- Nucci MR. Vulvar Neoplasia. Gynecologic Pathology: A Volume in the Series: Foundations in Diagnostic Pathology, Amsterdam: El Sevier. 2009:31-75.
- Chan MF, Yong TT, Sittampalam K. Giant labial fibroepithelial stromal polyp. Malaysian J Pathol. 2013;35(1):91-4.
- Madueke-Laveau OS, Gogoi R, Stoner G. Giant fibroepithelial stromal polyp of the vulva: largest case reported. Annals SurgInnov Res. 2013;7:8.
- Colak E, Kucuk GO, Kesmer S, Yildirim K. Giant fibroepithelial polyp of the perineum: Giant fibroepithelial polyp. Int J Surg Case Rep. 2015;17:126-7.
- Crum CP, Nucci MR, Lee KR. Soft Tissue Lesions of the Vulva and Vagina. In Diagnostic Gynecology and Obstetrics Pathology. Philadelphia: Elsevier. 2011:165–7.
- Nucci MR,Young RH, Fletcher CD. Cellular pseudosarcomatous fibroepithelial stromal polyps of the lower female genital tract: an underrecognized lesion often misdiagnosed as sarcoma. Am J Surg Pathol. 2000;24(2):231-40.
- McCluggage WG, Connolly L, McBridge HA. HMGA2 is a sensitive but not specific immunohistochemical marker of vulvovaginal angiomyxoma. Am J Surg Pathol. 2010;34(7):1037-42.
- Ostor AG, Fortune DW, Riley CB. Fibroepithelial polyps with atypical stromal cells (pseudosarcoma botryoides) of vulva and vagina. A report of 13 cases. Int J Gynecol Pathol. 1988;7(4):351-60.