Case Report
Two Very Rare Complications of Pancreatic Pseudocysts in one Patient: What are the Odds?
Palmela C1*, Barjas E1, Grenho J2, Ferreira R1, Santos AA1, Maio R2 and Cravo M1
1Department of Gastroenterology Service, Hospital Beatriz Ângelo, Loures, Portugal
2Department of General Surgery Service, Hospital Beatriz Ângelo, Loures, Portugal
*Corresponding author: Carolina Maria Simões Palmela, Department of Gastroenterology Service, Hospital Beatriz Ângelo, Avenida Carlos Teixeira, 3, 2674-514 Loures, Portugal
Published: 03 Aug, 2017
Cite this article as: Palmela C, Barjas E, Grenho J, Ferreira
R, Santos AA, Maio R, et al. Two Very
Rare Complications of Pancreatic
Pseudocysts in one Patient: What are
the Odds?. Clin Surg. 2017; 2: 1595.
Abstract
Herein we describe two consecutive and rare complications in a patient with known chronic alcoholic pancreatitis and pancreatic pseudocysts. The patient was first admitted to the emergency department with a spontaneous splenic rupture with active hemorrhage needing an emergent splenectomy. Eight months later spontaneous drainage from an orifice in the laparotomy scar occurred, which corresponded to cutaneous fistulization of the pancreatic pseudocyst. Keywords: Pancreatic disorders; Chronic pancreatitis; Pancreatic pseudocyst
Case Presentation
A 58-year-old male was admitted to the emergency department (ED) with severe abdominal pain, nausea and vomiting lasting for 12 hours. The pain was very intense, localized to the epigastrium, sudden in onset and had appeared after a meal. His past medical history was remarkable for chronic alcohol consumption (100 grams of alcohol per day in the last 10 years), a chronic alcoholic pancreatitis diagnosed 18 months before, with two episodes of mild acute pancreatitis in the last 12 months associated with active alcohol consumption. He was being followed in our outpatient clinic and had recently performed an abdominal CT scan that showed a pancreatic pseudocyst measuring 11 cm × 8 cm (Figure 1) located near the pancreatic tail. On admission, physical examination revealed a distressed and alert patient, with hypotension and tachycardia (97/60 mmHg, 105 bpm) and left upper quadrant severe tenderness, abdominal rigidity and diminished bowel sounds. Further examination was normal. Laboratory tests showed a hemoglobin (Hb) value of 9.2 g/dL, which corresponded to a 4 g drop from previous levels (13.1 g/dL; reference range (RR) 13.5 to 17.5 g/dL) and no leukocytosis or thrombocytosis. Serum amylase was 153 U/L (RR 28 to 100 U/L), lipase 232 U/L (RR 13 to 60 U/L), and C-reactive protein 8.63 mg/dL (RR< 0.50 mg/dL). Emergent abdominal CT scan showed a large subcapsular splenic hematoma with parenchymal laceration and superior capsular rupture (Figure 2). There was no history of previous trauma. The patient underwent emergent laparotomy, confirming a large splenic hematoma with almost total capsular detachment and active hemorrhage with a hemoperitoneum of 2,000 mL. A splenectomy was performed without complications and the patient was discharged 6 days later. The patient was observed one month later in a gastroenterology outpatient visit. He had no abdominal pain, anorexia or vomiting. Despite previous recommendations, the patient maintained active alcohol consumption. A control CT scan performed 3 months after surgery showed three pseudocysts, one posterior to the pancreatic tail with 102 mm × 73 mm, another anterior to the pancreatic tail with 64 mm × 35 mm and the other near the anterior abdominal wall with 68 mm × 55 mm (Figure 3A). Since the patient was totally asymptomatic and gaining weight, a watchful attitude was maintained. Three months later, the patient presented again in the ED complaining of acute abdominal pain, nausea, sweating and spontaneous fluid drainage from the laparotomy scar. He reported the spontaneous appearance of a cutaneous orifice two days earlier. On examination, his blood pressure was 63/38 mmHg, heart rate was 100 bpm and he had no fever (36.7°C). The abdomen was mildly tender in the upper abdomen and it was possible to identify an orifice in the middle of the laparotomy scar (Figure 3C). His hemoglobin level was 8.2 g/dl, white cell count was 28.880 × 109/L (RR 4.000 to 10.000) with 83% neutrophils; his CRP was 24 mg/dL (RR< 0.50), creatinine 2.2 mg/dL (RR 0.70 to 1.20), amylase 25 U/L, lactate 20 mg/dL (RR< 11). An urgent abdominal CT scan showed the disappearance of the pseudocysts previously described, with a small residual fluid collection containing air connected to a fistulous cutaneous tract, small quantities of free fluid and peritoneal mesenteric and omental thickening, suggesting spontaneous drainage of the pseudocysts (Figure3B). The patient responded well to fluid challenge, vasopressors and antibiotics, and was admitted to the intermediate care unit. The fistula drained a total of 100 mL of a hemato-purulent fluid, with an amylase level of 15 U/L and Escherichia coli was isolated. The patient remained stable and was discharged 10 days later. The fistula closed spontaneously two weeks later (Figure 3D). An outpatient magnetic resonance cholangiopancreatography revealed a dilated Wirsung’s duct with multiple intra-ductal calcifications and a residual pseudocyst measuring 2.9 cm × 1 cm near the pancreatic tail without evident direct communication with the pancreatic main duct.
Discussion
Pancreatic pseudocysts are a common complication of acute and chronic pancreatitis, complicating the course of the later in 30% to 40% of patients [1]. Alcohol-related pancreatitis is the major cause of pseudocyst formation, being responsible for 59% to 78% of all pseudocysts in countries with high alcohol consumption [1]. In the present case, pseudocyst formation was probably related to acute exacerbations of chronic pancreatitis associated with active alcohol consumption. The clinical course of pancreatic pseudocyst can range from spontaneous regression, persistence with or without symptoms or to result in complications [1,2]. Acute complications include rupture, pleural or bronchial fistula, infection and bleeding (usually from splenic artery pseudoaneurysm). Chronic complications include biliary obstruction, gastric outlet obstruction and thrombosis of the splenic or portal vein [1,2]. Herein we describe two exceedingly rare complications in the same patient: atraumatic splenic rupture followed by a spontaneous pseudocyst fistulization to the skin. The splenic complications associated with chronic pancreatitis and pancreatic pseudocysts are rare, with the exception of splenic vein thrombosis [3]. The reported incidence of splenic necrosis, intrasplenic pseudocysts and spontaneous splenic rupture is 2.2% [3]. Generally, splenic rupture is traumatic and associated with traffic accidents [4]. Atraumatic or spontaneous splenic rupture may occur in hematological and other malignancies, infectious diseases (mononucleosis and malaria), and acute or chronic pancreatitis [5]. There are several mechanisms that can explain spontaneous splenic rupture in the setting of chronic pancreatitis. In the presence of a pancreatic pseudocyst the most likely mechanism is enzymatic, with erosion of the splenic capsule. Another possible source of bleeding is a splenic artery pseudoaneurysm eroded by the contents of the pseudocyst [5]. In the present case, the formation of a splenic artery pseudoaneurysm and capsular erosion were the most probable causes of the hemorrhage because of the proximity between the pseudocyst and splenic hilum. Because of its rarity, spontaneous splenic rupture is frequently missed. The delay of emergent surgery is responsible for the high morbidity and mortality rate associated with this condition [5]. Another rare complication of pancreatic pseudocysts is spontaneous rupture and/or fistulization, occurring in less than 3% of cases [6]. The clinical course and patient outcome depends on the site of rupture. Rupture into the gastrointestinal tract, more frequently into the colon, may present with no symptoms or lead to melena or hematemesis [1,7]. Rupture into the abdominal cavity results in peritonitis and occasionally hemorrhagic shock, requiring emergent surgical exploration. Occasionally, pseudocysts rupture into the vascular system or the thoracic cavity [1,8]. Pancreatic collections rupture into the abdominal wall is exceedingly rare. To date, we found four cases of abdominal wall pancreatic pseudocysts reported in the literature, none of them with cutaneous fistulization. Subhas et al. [9] reported three cases of abdominal wall collections associated with peripancreatic pseudocysts, submitted to percutaneous drainage. Davey et al. [10] reported an uncomplicated pseudocyst presenting in the anterior abdominal wall following acute pancreatitis. Molina Infante et al. [11] reported cutaneous fistulization of acute fluid collections associated with acute necrotizing pancreatitis. To the best of our knowledge, this is the first case described in the literature of a pancreatic pseudocyst rupture to the abdominal wall and spontaneous cutaneous fistulization. The presence of a large infected pseudocyst in the proximity of the anterior abdominal wall combined with abdominal wall fragility associated with previous laparotomy was probably the mechanism that predisposed the patient to spontaneous cutaneous fistulization. Uncomplicated rupture of pseudocyst is a rare occurrence. In our case, we successfully managed our patient conservatively.
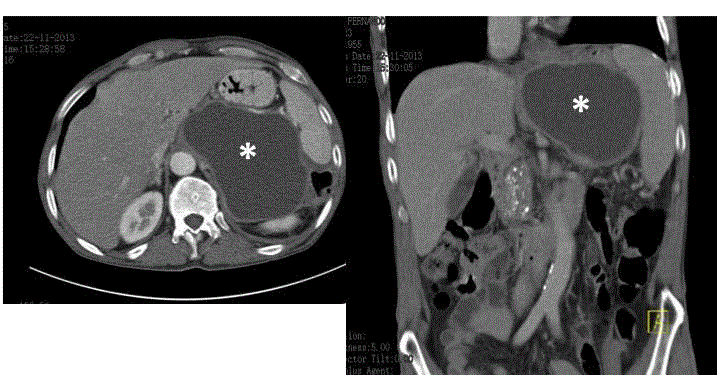
Figure 1
Figure 1
Abdominal CT scan showing a pancreatic pseudocyst of 11 cm
× 8 cm (asterisk) and pancreatic calcifications in a 58-year-old patient with
chronic pancreatitis.
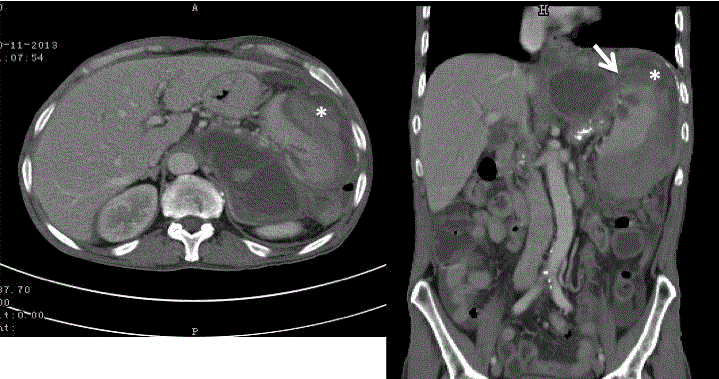
Figure 2
Figure 2
Abdominal CT scan showing a pancreatic pseudocyst and a large
subcapsular splenic hematoma (asterisk) with parenchymal laceration and
superior capsular rupture (arrow).
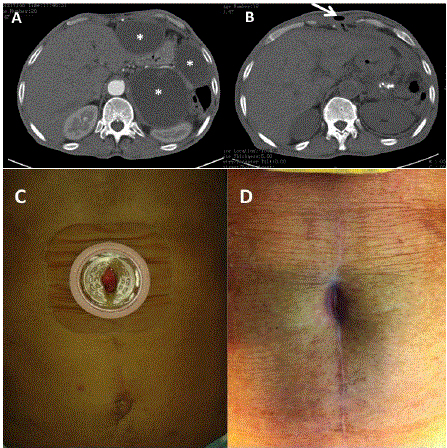
Figure 3
Figure 3
Abdominal CT scan showing three pseudocysts (asterisks).
B) CT three months later showing disappearance of the pseudocysts and
a fistulous anterior abdominal wall path (arrow). C) External orifice of the
cutaneous fistula in the middle of the laparotomy scar. D) Spontaneous
closure of the cutaneous orifice.
Conclusion
The present case illustrates two exceedingly rare complications associated with pancreatic pseudocysts. Because of their rarity, the diagnosis might be missed. It is important to be aware of such possibilities because of their need of prompt identification and management. To the best of our knowledge, we describe the first case of pancreatic pseudocyst rupture to the abdominal wall and cutaneous fistulization.
References
- Habashi S, Draganov PV. Pancreatic pseudocyst. World J Gastroenterol. 2009;15(1):38-47.
- Gouyon B, Levy P, Ruszniewski P, Zins M, Hammel P, Vilgrain V, et al. Predictive factors in the outcome of pseudocysts complicating alcoholic chronic pancreatitis. Gut. 1997;41(6):821-5.
- Steer ML, Waxman I, Freedman S. Chronic pancreatitis. N Engl J Med. 1995;332(22):1482-90.
- Renzulli P, Hostettler A, Schoepfer AM, Gloor B, Candinas D. Systematic review of atraumatic splenic rupture. Br J Surg. 2009;96(10):1114-21.
- Kurzbaum A, Qarawany LL, Nasrallah N, Safori GS. Spontaneous splenic rupture: A rare complication of chronic pancreatitis. Israeli J Emerg Med. 2008;8:35-8.
- Lillemoe KD, Yeo CJ. Management of complications of pancreatitis. Curr Probl Surg. 1998;35(1):1-98.
- Somani PO, Jain SS, Shah DK, Khot AA, Rathi PM. Uncomplicated spontaneous rupture of pancreatic pseudocyst into stomach: A case report. World J Gastrointest Endosc. 2013;5(9):461-4.
- Pitchumoni CS, Agarwal N. Pancreatic pseudocysts: when and how should drainage be performed? Gastroenterol Clin North Am. 1999;28(3):615-39.
- Subhas G, Bakston D, Ferguson L, Silapaswan S, Mittal VK. Abdominal wall pseudocyst fluid collection: a complication of pancreatic pseudocyst. Am Surg. 2010;76(12):1428-9.
- Davey PT, McKevitt G, Novak J. A pancreatic pseudocyst presenting in the anterior abdominal wall. Pancreas. 2011;40(3):484-6.
- Infante MJ, Martínez NO, Rincón NO, Díaz PA, Rodríguez BGM. Acute necrotizing pancreatitis with complicated fluid collections with cutaneous fistulas. An Med Interna. 2003;20(8):413-5.